Abstract
Background
Hypoplastic left heart syndrome (HLHS) is the third most common cause of critical congenital heart disease in newborns, and one of the most challenging forms to treat. Secondary pulmonary lymphangiectasia has been recognized in association with HLHS, an appearance described on fetal MRI as the “nutmeg lung.”
Objective
To investigate the association of fetal nutmeg lung with HLHS survival.
Materials and methods
A retrospective search of the fetal MRI database was performed. The nutmeg lung pattern was defined as T2 heterogeneous signal with tubular structures radiating peripherally from the hila. Postnatal echocardiograms and charts were reviewed.
Results
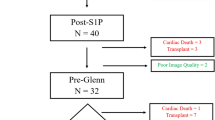
Forty-four fetal MR studies met inclusion criteria, of which 4 patients (9%) had the nutmeg lung pattern and 3 of whom also had restrictive lesions. Mortality in this nutmeg lung group was 100% by 5 months of age. Of the 40 patients without nutmeg lung, mortality/orthotopic heart transplant (OHT) was 35%. Of these 40 patients without nutmeg lung, 5 had restriction on echo, 3 of whom died/had OHT before 5 months of age (60% of patients with restriction and non-nutmeg lung). There was a significantly higher incidence of restrictive lesions (P = 0.02) and mortality/OHT (P = 0.02) in patients with nutmeg lung compared to those without.
Conclusion
The nutmeg lung MR appearance in HLHS fetuses is associated with increased mortality/OHT (100% in the first 5 months of life compared to 35% with HLHS alone). Not all patients with restrictive lesions develop nutmeg lung, and outcome is not as poor when restriction is present in isolation. Dedicated evaluation for nutmeg lung pattern on fetal MR studies may be useful to guide prognostication and aid clinicians in counseling parents of fetuses with HLHS.



Similar content being viewed by others
References
Rychik J (2005) Hypoplastic left heart syndrome: from in-utero diagnosis to school age. Semin Fetal Neonatal Med 10:553–566
Rychik J, Rome JJ, Collins MH et al (1999) The hypoplastic left heart syndrome with intact atrial septum: atrial morphology, pulmonary vascular histopathology and outcome. J Am Coll Cardiol 34:554–560
Marshall AC, van der Velde ME, Tworetzky W et al (2004) Creation of an atrial septal defect in utero for fetuses with hypoplastic left heart syndrome and intact or highly restrictive atrial septum. Circulation 110:253–258
Vida VL, Bacha EA, Larrazabal A et al (2007) Hypoplastic left heart syndrome with intact or highly restrictive atrial septum: surgical experience from a single center. Ann Thorac Surg 84:581–585
Glatz JA, Tabbutt S, Gaynor JW et al (2007) Hypoplastic left heart syndrome with atrial level restriction in the era of prenatal diagnosis. Ann Thorac Surg 84:1633–1638
Rychik J, Szwast A, Natarajan S et al (2010) Perinatal and early surgical outcome for the fetus with hypoplastic left heart syndrome: a 5-year single institutional experience. Ultrasound Obstet Gynecol 36:465–470
Graziano JN, Heidelberger KP, Ensing GJ et al (2002) The influence of a restrictive atrial septal defect on pulmonary vascular morphology in patients with hypoplastic left heart syndrome. Pediatr Cardiol 23:146–151
Moerman PL, Van Dijck H, Lauweryns JM et al (1986) Premature closure of the foramen ovale and congenital pulmonary cystic lymphangiectasis in aortic valve atresia or in severe aortic valve stenosis. Am J Cardiol 57:703–705
Seed M, Bradley T, Bourgeois J et al (2009) Antenatal MR imaging of pulmonary lymphangiectasia secondary to hypoplastic left heart syndrome. Pediatr Radiol 39:747–749
Victoria T, Andronikou S (2014) The fetal MR appearance of ‘nutmeg lung’: findings in 8 cases linked to pulmonary lymphangiectasia. Pediatr Radiol 44:1237–1242
Szwast A, Rychik J (2012) The use of reconstructive surgery to improve quality of life and survival in prenatal hypoplastic left heart syndrome. Futur Cardiol 8:215–225
Feinstein JA, Benson DW, Dubin AM et al (2012) Hypoplastic left heart syndrome: current considerations and expectations. J Am Coll Cardiol 59:S1–S42
Satomi G, Yasukochi S, Shimizu T et al (1999) Has fetal echocardiography improved the prognosis of congenital heart disease? Comparison of patients with hypoplastic left heart syndrome with and without prenatal diagnosis. Pediatr Int 41:728–732
Raman SP, Pipavath SN, Raghu G et al (2009) Imaging of thoracic lymphatic diseases. AJR Am J Roentgenol 193:1504–1513
Eom M, Choi YD, Kim YS et al (2007) Clinico-pathological characteristics of congenital pulmonary lymphangiectasis: report of two cases. J Korean Med Sci 22:740–745
France NE, Brown RJ (1971) Congenital pulmonary lymphangiectasis. Report of 11 examples with special reference to cardiovascular findings. Arch Dis Child 46:528–532
Noonan JA, Walters LR, Reeves JT (1970) Congenital pulmonary lymphangiectasis. Am J Dis Child 120:314–319
Luciani GB, Pessotto R, Mombello A et al (1999) Hypoplastic left heart syndrome with restrictive atrial septal defect and congenital pulmonary lymphangiectasis. Cardiovasc Pathol 8:49–51
Maeda K, Yamaki S, Kado H et al (2004) Hypoplasia of the small pulmonary arteries in hypoplastic left heart syndrome with restrictive atrial septal defect. Circulation 110:II139–II146
Quintero RA, Huhta J, Suh E et al (2005) In utero cardiac fetal surgery: laser atrial septotomy in the treatment of hypoplastic left heart syndrome with intact atrial septum. Am J Obstet Gynecol 193:1424–1428
Vlahos AP, Lock JE, McElhinney DB et al (2004) Hypoplastic left heart syndrome with intact or highly restrictive atrial septum: outcome after neonatal transcatheter atrial septostomy. Circulation 109:2326–2330
McElhinney DB, Tworetzky W, Lock JE (2010) Current status of fetal cardiac intervention. Circulation 121:1256–1263
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Saul, D., Degenhardt, K., Iyoob, S.D. et al. Hypoplastic left heart syndrome and the nutmeg lung pattern in utero: a cause and effect relationship or prognostic indicator?. Pediatr Radiol 46, 483–489 (2016). https://doi.org/10.1007/s00247-015-3514-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-015-3514-6