Abstract
Purpose
Despite the well-known neonatal morbidity risks after elective cesarean deliveries performed before 39 weeks, there are scarce data regarding mortality risks. The objective of this study was to calculate the risk of neonatal mortality after elective repeat cesarean delivery (ERCD) by gestational age.
Methods
The Linked Birth–Infant Death Data Files from the Vital Statistics Data of the Center for Disease Control and Prevention of the U.S. from 2004 to 2008 were analyzed. Only ERCD cases were included. Early death (<7 days), neonatal death (<28 days), and infant death (<1 year) were evaluated. A logistic regression model was used to calculate odds ratios. Cases delivered at 37–41 weeks were studied with 40 weeks as reference.
Results
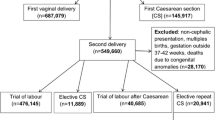
A total of 483,052 cases were included for analysis. The distribution of rates and odds ratios for infant, neonatal and early death was U-shaped with the nadir at 39 weeks. There was a statistically significant increase in early death at 37 compared to 40 weeks’ gestation [OR (95 %) CI = 1.929(1.172–3.176)]. No statistical increase was found in any of the other mortality risks.
Conclusion
There is an increased risk in early death with ERCD performed at 37 weeks. Our study provides evidence of neonatal harm beyond the reported morbidity risks.


Similar content being viewed by others
References
Martin JA, Hamilton BE, Ventura SJ, Osterman MJ, Kirmeyer S, Mathews TJ, Wilson EC (2011) Births: final data for 2009. Natl Vital Stat Rep 60(1):1–70
NIH State-of-the-Science Conference Statement on cesarean delivery on maternal request (2006) NIH Consens State Sci Statements 23(1):1–29
Obstetrics ACoPB (2009) ACOG Practice Bulletin No. 107: Induction of labor. Obstetrics and gynecology 114 (2 Pt 1):386–397. doi:10.1097/AOG.0b013e3181b48ef5
Gynecologists ACoOa (2013) ACOG committee opinion no. 559: Cesarean delivery on maternal request. Obstetrics and gynecology 121(4):904–907. doi:10.1097/01.AOG.0000428647.67925.d3
Gynecologists ACoOa (2013) ACOG committee opinion no. 560: Medically indicated late-preterm and early-term deliveries. Obstetrics and gynecology 121(4):908–910. doi:10.1097/01.AOG.0000428648.75548.00
Gynecologists ACoOa (2013) ACOG committee opinion no. 561: Nonmedically indicated early-term deliveries. Obstetrics and gynecology 121(4):911–915. doi:10.1097/01.AOG.0000428649.57622.a7
Bates E, Rouse D, Tita A (2011) Neonatal outcomes after demonstrated fetal lung maturity before 39 weeks of gestation. Obstet Gynecol 117(5):1229. doi:10.1097/AOG.0b013e3182176296
Tita AT, Landon MB, Spong CY, Lai Y, Leveno KJ, Varner MW, Moawad AH, Caritis SN, Meis PJ, Wapner RJ, Sorokin Y, Miodovnik M, Carpenter M, Peaceman AM, O’Sullivan MJ, Sibai BM, Langer O, Thorp JM, Ramin SM, Mercer BM, Network EKSNM-FMU (2009) Timing of elective repeat cesarean delivery at term and neonatal outcomes. N Engl J Med 360(2):111–120. doi:10.1056/NEJMoa0803267
Tita AT, Lai Y, Landon MB, Spong CY, Leveno KJ, Varner MW, Caritis SN, Meis PJ, Wapner RJ, Sorokin Y, Peaceman AM, O’Sullivan MJ, Sibai BM, Thorp JM, Ramin SM, Mercer BM, (MFMU) EKSNIoCHaHDNM-FMUN (2011) Timing of elective repeat cesarean delivery at term and maternal perioperative outcomes. Obstet Gynecol 117(2 Pt 1):280–286. doi:10.1097/AOG.0b013e3182078115
Ertuğrul S, Gün I, Müngen E, Muhçu M, Kılıç S, Atay V (2013) Evaluation of neonatal outcomes in elective repeat cesarean delivery at term according to weeks of gestation. J Obstet Gynaecol Res 39(1):105–112. doi:10.1111/j.1447-0756.2012.01951.x
Saidu R, Bolaji BO, Olatinwo AW, McIntosh CM, Alio AP, Salihu HM (2011) Repeat caesarean delivery as a risk factor for abnormal blood loss, blood transfusion and perinatal mortality. J Obstet Gynaecol 31(8):728–731. doi:10.3109/01443615.2011.606933
Tzur T, Weintraub AY, Sheiner E, Wiznitzer A, Mazor M, Holcberg G (2011) Timing of elective repeat caesarean section: maternal and neonatal morbidity and mortality. J Matern Fetal Neonatal Med 24(1):58–64. doi:10.3109/14767051003678267
Clark SL, Miller DD, Belfort MA, Dildy GA, Frye DK, Meyers JA (2009) Neonatal and maternal outcomes associated with elective term delivery. Am J Obstet Gynecol 200(2):156.e151–156.e154. doi:10.1016/j.ajog.2008.08.068
Chiossi G, Lai Y, Landon MB, Spong CY, Rouse DJ, Varner MW, Caritis SN, Sorokin Y, Oʼsullivan MJ, Sibai BM, Thorp JM, Ramin SM, Mercer BM, Network EKSNIoCHaHDNM-FMUM (2013) Timing of delivery and adverse outcomes in term singleton repeat cesarean deliveries. Obstet Gynecol 121(3):561–569. doi:10.1097/AOG.0b013e3182822193
Clark SL, Frye DR, Meyers JA, Belfort MA, Dildy GA, Kofford S, Englebright J, Perlin JA (2010) Reduction in elective delivery at < 39 weeks of gestation: comparative effectiveness of 3 approaches to change and the impact on neonatal intensive care admission and stillbirth. Am J Obstet Gynecol 203(5):449.e441–449.e446. doi:10.1016/j.ajog.2010.05.036
De Luca R, Boulvain M, Irion O, Berner M, Pfister RE (2009) Incidence of early neonatal mortality and morbidity after late-preterm and term cesarean delivery. Pediatrics 123(6):e1064–e1071. doi:10.1542/peds.2008-2407
Ecker J (2013) Elective cesarean delivery on maternal request. JAMA 309(18):1930–1936. doi:10.1001/jama.2013.3982
Hansen AK, Wisborg K, Uldbjerg N, Henriksen TB (2007) Elective caesarean section and respiratory morbidity in the term and near-term neonate. Acta Obstet Gynecol Scand 86(4):389–394. doi:10.1080/00016340601159256
Hourani M, Ziade F, Rajab M (2011) Timing of planned caesarean section and the morbidities of the newborn. N Am J Med Sci 3(10):465–468. doi:10.4297/najms.2011.3465
Robinson CJ, Villers MS, Johnson DD, Simpson KN (2010) Timing of elective repeat cesarean delivery at term and neonatal outcomes: a cost analysis. Am J Obstet Gynecol 202(6):632.e631–632.e636. doi:10.1016/j.ajog.2010.03.045
Salim R, Shalev E (2010) Health implications resulting from the timing of elective cesarean delivery. Reprod Biol Endocrinol 8:68. doi:10.1186/1477-7827-8-68
Paterson CM, Saunders NJ (1991) Mode of delivery after one caesarean section: audit of current practice in a health region. BMJ 303(6806):818–821
Perveen S (2011) Maternal and neonatal adverse outcome at repeat cesarean delivery versus repeat vaginal delivery. J Coll Physicians Surg Pak 21(2):84–87. doi:02.2011/JCPSP.8487
Bujold E, Francoeur D (2005) Neonatal morbidity and decision-delivery interval in patients with uterine rupture. J Obstet Gynaecol Can 27(7):671–673 (author reply 673)
Go MD, Emeis C, Guise JM, Schelonka RL (2011) Fetal and neonatal morbidity and mortality following delivery after previous cesarean. Clin Perinatol 38(2):311–319. doi:10.1016/j.clp.2011.03.001
Lydon-Rochelle MT, Holt VL, Cárdenas V, Nelson JC, Easterling TR, Gardella C, Callaghan WM (2005) The reporting of pre-existing maternal medical conditions and complications of pregnancy on birth certificates and in hospital discharge data. Am J Obstet Gynecol 193(1):125–134. doi:10.1016/j.ajog.2005.02.096
Adams MM, Kirby RS (2007) Measuring the accuracy and completeness of linking certificates for deliveries to the same woman. Paediatr Perinat Epidemiol 21(Suppl 1):58–62. doi:10.1111/j.1365-3016.2007.00838.x
Abouzeid H, Aggarwal D, De Graaf F (2007) Timing of planned repeated caesarean section: an enigma. J Obstet Gynaecol 27(8):798–801. doi:10.1080/01443610701666843
Acknowledgments
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Rights and permissions
About this article
Cite this article
Vilchez, G., Hoyos, L.R., Maldonado, M.C. et al. Risk of neonatal mortality according to gestational age after elective repeat cesarean delivery. Arch Gynecol Obstet 294, 77–81 (2016). https://doi.org/10.1007/s00404-015-3955-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-015-3955-z