Abstract
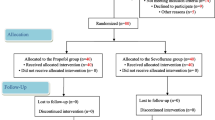
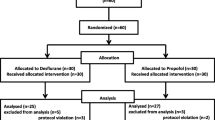
Postoperative cognitive dysfunction (POCD) is diagnosed in up to 30% patients after anaesthesia. The causative role of anaesthetic toxicity remains unclear. Using clinical tests, no clear-cut differences have been observed between anaesthetics so far. The aim of this trial was to compare the incidence of POCD diagnosed by a battery of neuropsychologic tests after propofol and sevoflurane anaesthesia. Secondary goal was to examine possible relationship between POCD positivity and changes in auditory event-related potentials (ERPs). Sixty patients undergoing lumbar discectomy were prospectively randomized to receive depth-controlled sevoflurane (SEVO) or propofol (PROP) based anaesthesia. The neuropsychological examination and auditory event-related potentials (N1, P3a and P3b components) recording was performed preoperatively and on days 1, 6 and 42 after surgery. POCD was defined as a decline of more than one standard deviation in three or more tests. In 43 patients (20 in PROP and 23 in SEVO group) all selected tests were performed and used for the evaluation. POCD was present in 48%/60%, 18%/20% and 17%/11% (SEVO/PROP) of patients on days 1, 6 and 42 after surgery, with no significant intergroup difference. Among neuropsychologic tests, the most significant decline was observed in Semantic Verbal Fluency and Letter-Number Sequencing Test scores, congruently in both groups on days 1 and 6, with full recovery on the last control. Transient deteriorations in other tests were observed as well. No association of POCD positivity and ERPs changes was found, although long-term modifications of P3a and P3b components were observed, mainly in SEVO group. In our study, sevoflurane and propofol anaesthesia was associated with the similar incidence of POCD. Cognitive decline, mainly affecting executive functions, was temporary in most of the patients. Prolonged ERPs alterations after the anaesthesia seem not to have any relationship with the impairment registered by the neuropsychological examination and may represent subclinical changes.



Similar content being viewed by others
References
Moller J, Cluitmans P, Rasmussen L, Houx P, Rasmussen H, Canet J, et al. Long-term postoperative cognitive dysfunction in the elderly: ISPOCD1 study. Lancet 1998;351(9106):857–61.
Monk T, Weldon B, Garvan C, Dede D. Predictors of cognitive dysfunction after major noncardiac surgery. Anesthesiology 2008;108(1):18–30.
Funder KS, Steinmetz J. Post-operative cognitive dysfunction—lessons from the ISPOCD studies. Trends Anaesth Crit Care. 2012;2(3):94–7.
Evered L, Scott DA, Silbert B, Maruff P. Postoperative cognitive dysfunction is independent of type of surgery and anesthetic. Anesth Analg. 2011;112(5):1179–85.
Rasmussen LS, Johnson T, Kuipers HM, Kristensen D, Siersma VD, Vila P, et al. Does anaesthesia cause postoperative cognitive dysfunction? A randomised study of regional versus general anaesthesia in 438 elderly patients. Acta Anaesthesiol Scand. 2003;47(3):260–6.
Royse CF, Andrews DT, Newman SN, Stygall J, Williams Z, Pang J, et al. The influence of propofol or desflurane on postoperative cognitive dysfunction in patients undergoing coronary artery bypass surgery. Anaesthesia 2011;66(6):455–64.
Schoen J, Husemann L, Tiemeyer C, Lueloh A, Sedemund-Adib B, Berger K-U, et al. Cognitive function after sevoflurane- vs propofol-based anaesthesia for on-pump cardiac surgery: a randomized controlled trial. Br J Anaesth. 2011;106(6):840–50.
Cai Y, Hu H, Liu P, Feng G, Dong W, Yu B. Association between the apolipoprotein E4 and postoperative cognitive dysfunction in elderly patients undergoing intravenous anesthesia and inhalation anesthesia. Anesthesiology 2012;116(1):84–93.
Rohan D, Buggy DJ, Crowley S, Ling FKH, Gallagher H, Regan C, et al. Increased incidence of postoperative cognitive dysfunction 24 hr after minor surgery in the elderly. Can J Anesth. 2005;52(2):137–42.
Woodman GF. A brief introduction to the use of event-related potentials (ERPs) in studies of perception and attention. Atten Percept Psychophysiol. 2010;72(8):1–29.
Remijn GB, Hasuo E, Fujihira H, Morimoto S. An introduction to the measurement of auditory event-related potentials (ERPs). Acoust Sci Technol. 2014;35(5):229–42.
Pulvermüller F, Lutzenberger W, Müller V, Mohr B, Dichgans J, Birbaumer N. P3 and contingent negative variation in Parkinson’s disease. Electroencephalogr Clin Neurophysiol. 1996;98(6):456–67.
Bonanni L, Franciotti R, Onofrj V, Anzellotti F, Mancino E, Monaco D, et al. Revisiting P300 cognitive studies for dementia diagnosis: early dementia with Lewy bodies (DLB) and Alzheimer disease (AD). Neurophysiol Clin. 2010;40(5–6):255–65.
De Giorgio CM, Rabinowicz AL, Gott PS. Predictive value of P300 event-related potentials compared with EEG and somatosensory evoked potentials in non-traumatic coma. Acta Neurol Scand. 1993;87(5):423–7.
van Hooff JC, de Beer N, Brunia CH, Cluitmans PJ, Korsten HH. Event-related potential measures of information processing during general anesthesia. Electroencephalogr Clin Neurophysiol. 1997;103(2):268–81.
Heinke W, Kenntner R, Gunter TC, Sammler D, Olthoff D, Koelsch S. Sequential effects of increasing propofol sedation on frontal and temporal cortices as indexed by auditory event-related potentials. Anesthesiology 2004;100(3):617–25.
Reinsel R, Veselis R, Wronski M, Marino P. The P300 event-related potential during propofol sedation: a possible marker for amnesia? Br J Anaesth. 1995;74(6):674–80.
Roberts FL, Dixon J, Lewis GTR, Tackley RM, Prys-Roberts C. Induction and maintenance of propofol anaesthesia. Anaesthesia 1988;43(s1):14–7.
Mueller SC, Swainson R, Jackson GM. ERP indices of persisting and current inhibitory control: a study of saccadic task switching. Neuroimage 2009;45(1):191–7.
Tomé D, Barbosa F, Nowak K, Marques-Teixeira J. The development of the N1 and N2 components in auditory oddball paradigms: a systematic review with narrative analysis and suggested normative values. J Neural Transm. 2015;122(3):375–91.
Rasmussen LS, Larsen K, Houx P, Skovgaard LT, Hanning CD, Moller JT. The assessment of postoperative cognitive function. Acta Anaesthesiol Scand. 2001;45(3):275–89.
Powell LM, Molyneux M. Should patients be advised not to drive for 4 days after isoflurane anaesthesia? Anaesthesia 2017;72(6):682–5.
Mracek J, Holeckova I, Chytra I, Mork J, Stepanek D, Vesela P. The impact of general versus local anesthesia on early subclinical cognitive function following carotid endarterectomy evaluated using P3 event-related potentials. Acta Neurochir (Wien). 2012;154(3):433–8.
Papaioannou A, Fraidakis O, Michaloudis D, Balalis C, Askitopoulou H. The impact of the type of anaesthesia on cognitive status and delirium during the first postoperative days in elderly patients. Eur J Anaesthesiol. 2005;22(7):492–9.
Nemeth E, Vig K, Racz K, Koritsanszky KB, Ronkay KI, Hamvas FP, et al. Influence of the postoperative inflammatory response on cognitive decline in elderly patients undergoing on-pump cardiac surgery: a controlled, prospective observational study. BMC Anesthesiol. 2017;17(1):113.
Holečková I, Kletečka J, Štěpánek D, Žídek S, Bludovský D, Pouska J, et al. Cognitive impairment measured by event-related potentials during early and late postoperative period following intravenous or inhalation anaesthesia. Clin Neurophysiol. 2018;129(1):246–53.
Acknowledgements
The authors would like to acknowledge the work performed by independent statistician ing. Kormunda and all staff involved in this study.
Funding
The study was funded by the Charles University research funds PRVOUK P36 and PROGRES Q39.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Kletecka, J., Holeckova, I., Brenkus, P. et al. Propofol versus sevoflurane anaesthesia: effect on cognitive decline and event-related potentials. J Clin Monit Comput 33, 665–673 (2019). https://doi.org/10.1007/s10877-018-0213-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-018-0213-5