Abstract
Purpose
Diagnosis of tuberculous uveitis (TBU) is often challenging and is usually made after excluding other causes of uveitis. We analysed the characteristics of TBU and variables associated with visual outcome.
Methods
A retrospective, observational analysis was performed in patients with presumptive TBU who were started on specific TB treatment between January 2006 and June 2016. Demographic, clinical, radiological, analytical and ophthalmic examination variables were studied. After completing TB treatment, a follow-up of at least 9 months was performed. A univariate and logistic regression analysis was applied to identify the variables associated with visual acuity and recurrences of uveitis.
Results
Forty affected eyes of 24 individuals were identified; 79% of patients were diagnosed during the last 3 years of the study period. Median delay from onset of symptoms to diagnosis was 12 weeks. Loss of visual acuity was the most frequent symptom (87.5%). Posterior uveitis was the most frequent localization (72.9%); 19 patients (79.2%) presented at least one of the Gupta signs predictive of TBU, but there were no confirmed diagnoses.
Outcome
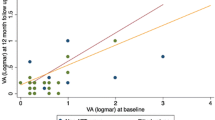
There was improvement in visual acuity in 74.4% of the eyes, but a complete response was achieved only in 56.4%. There was recurrence in two patients. The initiation of treatment ≥ 24 weeks after onset of symptoms was significantly associated with no improvement (p = 0.026).
Conclusion
TBU can cause permanent damage to visual acuity, particularly in patients with delayed diagnosis. A prompt initiation of systemic TB treatment is essential to improve visual prognosis.


Similar content being viewed by others
References
Cordero-Coma M, Salazar R, Costales F. Tuberculous uveitis: an update. Expert Rev Ophthalmol. 2014;9:125–37. https://doi.org/10.1586/17469899.2014.897228.
Lee C, Agrawal R, Pavesio C. Ocular tuberculosis. A clinical conundrum. Ocul Immunol Inflamm. 2016;24:237–42. https://doi.org/10.3109/09273948.2014.985387.
Lou SM, Larkin KL, Winthrop K, Rosenbaum JT, Group USS. Lack of consensus in the diagnosis and treatment for ocular tuberculosis among uveitis specialists. Ocul Immunol Inflamm. 2015;23:25–31. https://doi.org/10.3109/09273948.2014.926936.
Alvarez GG, Roth VR, Hodge W. Ocular tuberculosis: diagnostic and treatment challenges. Int J Infect Dis. 2009;13:432–5. https://doi.org/10.1016/j.ijid.2008.09.018.
Ang M, Chee SP. Controversies in ocular tuberculosis. Br J Ophthalmol. 2017;101:6–9. https://doi.org/10.1136/bjophthalmol-2016-309531.
Levenson JH, Kozarsky K. Visual Acuity. In: Walker HK, Hall WD, Hurst JW, editors. Clinical methods: the history, physical, and laboratory examinations. 3rd ed. Boston: Butterworths; 1990, pp. 563–4.
Jabs DA, Nussenblatt RB, Rosenbaum JT, Group SoUNSW. Standardization of uveitis nomenclature for reporting clinical data. Results of the First International Workshop. Am J Ophthalmol. 2005;140:509–16.
Gupta A, Sharma A, Bansal R, Sharma K. Classification of intraocular tuberculosis. Ocul Immunol Inflamm. 2015;23:7–13. https://doi.org/10.3109/09273948.2014.967358.
Ang L, Kee A, Yeo TH, Dinesh VG, Ho SL, Teoh SC, et al. Treatment outcome in patients with presumed tubercular uveitis at a tertiary referral eye care centre in Singapore. Int Ophthalmol. 2016. https://doi.org/10.1007/s10792-016-0401-6.
Gupta A, Bansal R, Gupta V, Sharma A, Bambery P. Ocular signs predictive of tubercular uveitis. Am J Ophthalmol. 2010;149:562–70. https://doi.org/10.1016/j.ajo.2009.11.020.
Agrawal R, Gupta B, Gonzalez-Lopez JJ, Rahman F, Phatak S, Triantafyllopoulou I, et al. The role of anti-tubercular therapy in patients with presumed ocular tuberculosis. Ocul Immunol Inflamm. 2015;23:40–6. https://doi.org/10.3109/09273948.2014.986584.
Bajema KL, Pakzad-Vaezi K, Hawn T, Pepple KL. Tuberculous uveitis: association between anti-tuberculous therapy and clinical response in a non-endemic country. J Ophthalmic Inflamm Infect. 2017;7:19. https://doi.org/10.1186/s12348-017-0137-0.
Mora P, Ghirardini S, Héron E, Sedira N, Olcelli F, Gandolfi S, et al. Ocular tuberculosis: experience of an Italian and French cohort. Acta Ophthalmol. 2015;93:e403-4. https://doi.org/10.1111/aos.12602.
Agrawal R, Gunasekeran DV, Grant R, Agarwal A, Kon OM, Nguyen QD, et al. Clinical features and outcomes of patients with tubercular uveitis treated with antitubercular therapy in the collaborative ocular tuberculosis study (COTS)-1. JAMA Ophthalmol. 2017;135:1318–27. https://doi.org/10.1001/jamaophthalmol.2017.4485.
Kee AR, Gonzalez-Lopez JJ, Al-Hity A, Gupta B, Lee CS, Gunasekeran DV, et al. Anti-tubercular therapy for intraocular tuberculosis: a systematic review and meta-analysis. Surv Ophthalmol. 2016;61:628–53. https://doi.org/10.1016/j.survophthal.2016.03.001.
Smit DP, Esterhuizen TM, Meyer D. The prevalence of intraocular tuberculosis in HIV-positive and HIV-negative patients in south africa using a revised classification system. Ocul Immunol Inflamm. 2016;23:1–8. https://doi.org/10.1080/09273948.2016.1263342.
Tognon MS, Fiscon M, Mirabelli P, Graziani G, Peracchi M, Sattin A, et al. Tuberculosis of the eye in Italy: a forgotten extrapulmonary localization. Infection. 2014;42:335–42. https://doi.org/10.1007/s15010-013-0554-4.
Cordero-Coma M, Garzo I, Salazar R, Franco M, Calleja S, Ruiz de Morales JM. Treatment of presumed tuberculous uveitis affecting the posterior segment: diagnostic confirmation and long term outcomes. Arch Soc Esp Oftalmol. 2013;88:339–44. https://doi.org/10.1016/j.oftal.2012.11.011.
Li KK, Chan WM, Tam BS, Ng JS, Lam DS. Needle tap in the diagnosis of inflammation. Ophthalmology. 2004;111:609. https://doi.org/10.1016/j.ophtha.2003.12.036 (author reply—10).
Sharma K, Gupta V, Bansal R, Sharma A, Sharma M, Gupta A. Novel multi-targeted polymerase chain reaction for diagnosis of presumed tubercular uveitis. J Ophthalmic Inflamm Infect. 2013;3:25. https://doi.org/10.1186/1869-5760-3-25.
Bouza E, Merino P, Muñoz P, Sanchez-Carrillo C, Yáñez J, Cortés C. Ocular tuberculosis. A prospective study in a general hospital. Medicine (Baltimore). 1997;76:53–61.
Troutbeck R, Lim LL. Clinical controversy: to treat, or not to treat? That is the tuberculosis question. Clin Exp Ophthalmol. 2012;40:653–4. https://doi.org/10.1111/j.1442-9071.2012.02855.x.
Abrams J, Schlaegel TF. The role of the isoniazid therapeutic test in tuberculous uveitis. Am J Ophthalmol. 1982;94:511–5.
Bansal R, Gupta A, Gupta V, Dogra MR, Bambery P, Arora SK. Role of anti-tubercular therapy in uveitis with latent/manifest tuberculosis. Am J Ophthalmol. 2008;146:772–9. https://doi.org/10.1016/j.ajo.2008.06.011.
Patel SS, Saraiya NV, Tessler HH, Goldstein DA. Mycobacterial ocular inflammation: delay in diagnosis and other factors impacting morbidity. JAMA Ophthalmol. 2013;131:752–8. https://doi.org/10.1001/jamaophthalmol.2013.71.
González-Martín J, García-García J, Anibarro L, Vidal R, Esteban J, Blanquer R, et al. Consensus document on the diagnosis, treatment and prevention of tuberculosis. Enferm Infecc Microbiol Clin. 2010;28:297.e1-20. https://doi.org/10.1016/j.eimc.2010.02.006.
Ang M, Hedayatfar A, Wong W, Chee SP. Duration of anti-tubercular therapy in uveitis associated with latent tuberculosis: a case–control study. Br J Ophthalmol. 2012;96:332–6. https://doi.org/10.1136/bjophthalmol-2011-300209.
Ng KK, Nisbet M, Damato EM, Sims JL. Presumed tuberculous uveitis in non-endemic country for tuberculosis: case series from a New Zealand tertiary uveitis clinic. Clin Exp Ophthalmol. 2017;45:357–65. https://doi.org/10.1111/ceo.12881.
Krassas N, Wells J, Bell C, Woodhead M, Jones N. Presumed tuberculosis-associated uveitis: rising incidence and widening criteria for diagnosis in a non-endemic area. Eye (Lond). 2018;32:87–92. https://doi.org/10.1038/eye.2017.152.
La Distia Nora R, van Velthoven ME, Ten Dam-van Loon NH, Misotten T, Bakker M, van Hagen MP, et al. Clinical manifestations of patients with intraocular inflammation and positive QuantiFERON-TB gold in-tube test in a country nonendemic for tuberculosis. Am J Ophthalmol. 2014;157:754 – 61. https://doi.org/10.1016/j.ajo.2013.11.013.
Trad S, Bodaghi B, Saadoun D. Update on immunological test (Quantiferon-TB Gold) contribution in the management of tuberculosis-related ocular inflammation. Ocul Immunol Inflamm. 2017. https://doi.org/10.1080/09273948.2017.1332232.
Acknowledgements
Fundación Galicia Sur Statistics Foundation for statistical support.
Funding
Without financing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
An institucional Review Board approval was obtained from the Comité Ético de Investigación Galicia Sur (registration code 2017/007.
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Anibarro, L., Cortés, E., Chouza, A. et al. Early treatment of tuberculous uveitis improves visual outcome: a 10-year cohort study. Infection 46, 549–554 (2018). https://doi.org/10.1007/s15010-018-1161-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-018-1161-1