Abstract
Purpose
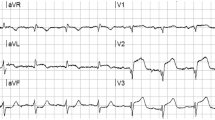
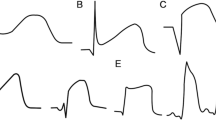
A paucity of information exists to validate the accuracy and reliability of ECG monitoring in the operating room or ICU. The purpose of this study was to determine the accuracy, sensitivity, specificity, and predictive values of the Marquette ECG monitor for detection of perioperative myocardial ischaemia (PMI) as measured by ST segment changes in a high risk population.
Methods
Monitoring for PMI in 28 patients scheduled for aortocoronary bypass surgery was done with the Cardiodata PR® ambulatory continuous electrocardiography (ACECG) monitor lead V5, and compared with lead V5 of the Marquette® Series 7000 ECG/ Surgical operating room monitor, and ECG/Resp ICU monitor. The Marquette lead V5 was evaluated using current criteria for the assessment of diagnostic tests including concordance, sensitivity, specificity, positive and negative predictive values, false positive and false negative rates and compared with the ACECG monitor which served as the reference or “gold standard.” Agreement beyond chance between the two methods was assessed using the Kappa statistic.
Results
Of the 53 observation data points, 27 were defined as ischaemic episodes by ACECG. Concordance between lead V5 in each system was 83% (44/53 episodes). Discordance was 17% (9/53 episodes), predominantly in the postbypass interval (77%, 7/9; P = 0.0184). The incidences of false negatives and false positives for Marquette lead V5 was 26% (7/27) and 7.7% ( 2/26), respectively. The sensitivity and specificity of the Marquette was 0.74 and 0.92. Positive predictive value was 0.91, negative predictive value was 0.77, and Kappa statistic was 66%.
Conclusion
Automated ST segment analysis with the Marquette® Series 7000 monitoring system demonstrates good diagnostic accuracy, moderate sensitivity, and high specificity. However, clinically significant false negative and false positive rates of ischaemia detection are associated with its use, especially in the postoperative period.
Résumé
Objectif
Peu de données nous permettent de valider la précision et la fiabilité du monitorage électrocardiographique en salle d’opération et à l’unité des soins intensifs. Cette étude avait pour but de déterminer dans une population à haut risque, la précision, la sensibilité, la spécificité et la valeur prédictrice du moniteur d’ECG Marquette destiné à la détection de l’ischémie myocardique périopératoire (IMP) telle que mesurée par les altérations du segment ST.
Méthodes
Chez 28 patients programmés pour une chirurgie de revascularisation myocardique, l’IMP était monitorisée par électrocardiographie ambulatoire continue (ECGAC) à l’aide d’un appareil Cardiodata PR® en dérivation V5, pour fin de comparaison à la dérivation V5 d’un moniteur ECG de salle d’opération et d’un moniteur ECG/Resp de soins intensifs Marquette® Series 7000. La dérivation V5 du Marquette était comparée aux critères en vigueur pour l’évaluation des épreuves diagnostiques dont la concordance, la sensibilité, la spécificité, les valeurs prédictrices négatives et positives, le taux de faux positifs et de faux négatifs. L’accord entre les deux méthodes était évaluée par statistique Kappa.
Résultats
Des 53 épisodes observés, 27 ont été décrits par l’ECGAC comme des épisodes ischémiques. La concordance entre la dérivation V5 de chaque système était 83% (44/53 épisodes). La discordance était 17% (9/53 épisodes), avec prédominance pendant l’intervalle post-CEC (77%, 7/9; P =0,0184). Avec le V5 du Marquette, l’incidence de faux négatifs et de faux positifs était respectivement de 26% (7/27) et de 7,7% (2/26). La sensibilité et la spécificité du Marquette étaient de 0,74 et de 0,92. La valeur prédictrice positive était 0,91, et négative, 0,77. La statistique Kappa était calculée à 66%.
Conclusion
L’analyse automatisée du segment ST avec un système de monitorage Marquette Series 7000 est précise, modérément sensible et hautement spécifique. Cependant, un taux cliniquement important de faux négatifs et de faux positifs est associé à son utilisation surtout à la période postopératoire.
Article PDF
Similar content being viewed by others
References
Smith RC, Leung JM, Mangano DT, SPI Research Croup. Postoperative myocardial ischemia in patients undergoing coronary artery bypass graft surgery. Anesthesiology 1991; 74: 464–73.
Mirvis DM, Berson AS, Goldberger AL, et al. Instrumentation and practice standards for electrocardiographic monitoring in special care units. A report for health professionals by a Task Force of the Council on Clinical Cardiology, American Heart Association. Circulation 1989; 79: 464–71.
Gottleib SO, Weisfeldt ML, Ouyang P, Mellits ED, Gerstenblith G. Silent ischemia as a marker for early unfavorable outcomes in patients with unstable angina. N Engl J Med 1986; 314: 1214–9.
Hollenburg M. Reliability of the continuous ECG after cardiopulmonary bypass and CABG surgery. J Card Surg 1994; 9: 410–2.
Graeber GM, Shawl FA, Head HD, et al. Changes in serum creatine kinase and lactate dehydrogenase caused by acute perioperative myocardial infarction and by transatrial cardiac surgical procedures. J Thorac Cardiovasc Surg 1986; 92: 63–72.
Sheps SB, Schechter MT. The assessment of diagnostic tests. A survey of current medical research. JAMA 1984; 252: 2418–22.
Schechter MT, Sheps SB. Diagnostic testing revisited: pathways through uncertainty. Can Med Assoc J 1985; 132: 755–60.
Department of Clinical Epidemiology and Biostatistics, McMaster University Health Sciences Centre. How to read clinical journals: II. To learn about diagnostic tests. Can Med Assoc J 1981; 124: 703–10.
Knight AA, Hollenberg M, London MJ, et al. Perioperative myocardial ischemia: importance of the preoperative ischémic pattern. Anesthesiology 1988; 68: 681–8.
Hall RI, O’Regan N, Gardner M. Detection of intraoperative myocardial ischaemia —a comparison among electrocardiographic, myocardial metabolic, and haemodynamic measurements in patients with reduced ventricular function. Can J Anaesth 1995; 42: 487–94.
Slogoff S, Keats AS, David Y, Igo SR. Incidence of perioperative myocardial ischemia detected by different electrocardiographic systems. Anesthesiology 1990; 73: 1074–81.
Watanabe S, Buffington CW. Speed and sensitivity of mechanical versus electrographic indicators to mild or moderate myocardial ischemia in the pig. Anesthesiology 1994; 80: 582–94.
Deanfield JE, Shea M, Ribiero P, et al. Transient ST-segment depression as a marker of myocardial ischemia during daily life. Am J Cardiol 1984; 54: 1195–200.
Deanfield JE, Ribiero P, Oakley K, Krikler S, Selwyn AP. Analysis of ST-segment changes in normal subjects: implications for ambulatory monitoring in angina pectoris. Am J Cardiol 1984; 54: 1321–5.
Leung JM, O’Kelly BF, Mangano DT, SPI Research Group. Relationship of regional wall motion abnormalities to hemodynamic indices of myocardial oxygen supply and demand in patients undergoing CABG surgery. Anesthesiology 1990; 73: 802–14.
Brooker S, Lownstein E. Spurious ST segment depression by automated ST segment analysis. J Clin Monit 1995; 11: 186–9.
Marriott HJL. Practical Electrocardiography, 6th ed. Baltimore/London: Williams & Wilkins, 1977: 290–318.
London MJ, Kaplan JA. Advances in electrocardiographic monitoring. In: Kaplan JA (Ed.). Cardiac Anaesthesia, 3rd ed. Philadelphia: WB Saunders & Co., 1993: 299–341.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ansley, D.M., O’Connor, J.P., Merrick, P.M. et al. On line ST-segment analysis for detection of myocardial ischaemia during and after coronary revascularization. Can J Anaesth 43, 995–1000 (1996). https://doi.org/10.1007/BF03011899
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03011899