Abstract
Objective
To evaluate the usefulness of early transcranial Doppler ultrasound (TCD) goal-directed therapy after severe traumatic brain injury initiated before invasive cerebral monitoring is available.
Design
Prospective, observational clinical study.
Setting
Surgical intensive care unit, university hospital.
Patients and participants
Twenty-four severely brain-injured patients.
Interventions
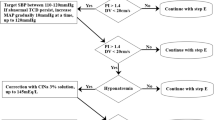
All patients had TCD measurements immediately on admission (T0) and when invasive cerebral monitoring was available (T1). TCD was considered abnormal when two out of three measured values were outside the following limits: Vm < 30 cm/s, Vd < 20 cm/s, PI > 1.4. When admission TCD was abnormal, attending physicians modified treatment to increase cerebral perfusion pressure.
Measurements and results
Admission TCD was performed 18 ± 11 min (T0) after admission, whereas cerebral inasive monitoring was available 242 ± 116 min (T1) after admission. At T0, 11 (46%) patients had abnormal TCD values (group 1) and 13 had normal TCD values (group 2); mean arterial pressure was comparable between groups. All group 1 patients received mannitol and/or norepinephrine. At T1, mean arterial pressure was increased compared to admission in group 1 (105 ± 17 mmHg vs. 89 ± 15 mmHg, p < 0.05) and only two patients had still an abnormal TCD. Although group 1 patients had higher intracranial pressure than those of group 2 (32 ± 13 mmHg vs. 22 ± 10 mmHg, p < 0.01), both cerebral perfusion pressure and jugular venous oxygen saturation were comparable between the groups.
Conclusions
The use of TCD at hospital admission allows identification of severely brain-injured patients with brain hypoperfusion. In such high-risk patients, early TCD goal-directed therapy can restore normal cerebral perfusion and might then potentially help in reducing the extent of secondary brain injury.


Similar content being viewed by others
References
Jones PA, Andrews PJD, Midgley S, Anderson SI, Piper IR, Tocher JL, Housley AM, Corrie JA, Slattery J, Dearden NM, Miller JD (1994) Measuring the burden of secondary insults in head-injured patients during intensive care. J Neurosurg Anesthesiol 6:4–14
Chesnut RM, Marshall LF, Klauber MR, Blunt BA, Baldwin N, Eisenberg HM, Jane JA, Marmarou A, Foulkes MA (1993) The role of secondary brain injury in determining outcome from severe head injury. J Trauma 34:216–222
Stocchetti N, Furlan A, Volta F (1996) Hypoxemia and arterial hypotension at the accident scene in head injury. J Trauma 40:764–767
Rouxel JP, Tazarourte K, Le Moigno S, Ract C, Vigue B (2004) [Medical prehospital rescue in head injury]. Ann Fr Anesth Reanim 23:6–14
DeWitt DS, Jenkins LW, Prough DS (1995) Enhanced vulnerability to secondary ischemic insults after experimental traumatic brain injury. New Horiz 3:376–383
Bouma GJ, Muizelaar JP, Stringer WA, Choi SC, Fatouros P, Young HF (1992) Ultra-early evaluation of regional cerebral blood flow in severely head-injured patients using xenon-enhanced computerized tomography. J Neurosurg 77:360–368
Gopinath SP, Robertson CS, Contant CF, Hayes C, Feldman Z, Narayan RK, Grossman RG (1994) Jugular venous desaturation and outcome after head injury. J Neurol Neurosurg Psychiatry 57:717–723
Coles JP, Fryer TD, Smielewski P, Chatfield DA, Steiner LA, Johnston AJ, Downey SP, Williams GB, Aigbirhio F, Hutchinson PJ, Rice K, Carpenter TA, Clark JC, Pickard JD, Menon DK (2004) Incidence and mechanisms of cerebral ischemia in early clinical head injury. J Cereb Blood Flow Metab 24:202–211
[No authors listed] (1999) [What are the treatment modalities of severe head injuries in the prehospital phase?]. Ann Fr Anesth Reanim 18:36–46
Gabriel EJ, Ghajar J, Jagoda A, Pons PT, Scalea T, Walters BC (2002) Guidelines for prehospital management of traumatic brain injury. J Neurotrauma 19:111–174
Vigué B, Ract C, Benayed B, Zlotine N, Leblanc PE, Samii K, Bissonnette B (1999) Early SjvO2 monitoring in patients with severe brain trauma. Intensive Care Med 25:445–451
Revell M, Porter K, Greaves I (2002) Fluid resuscitation in prehospital trauma care: a consensus view. Emerg Med J 19:494–498
Tuor UI, Edvinsson L, McCulloch J (1986) Catecholamines and the relationship between cerebral blood flow and glucose use. Am J Physiol 251:H824–H833
Kroppenstedt SN, Kern M, Thomale UW, Schneider GH, Lanksch WR, Unterberg AW (1999) Effect of cerebral perfusion pressure on contusion volume following impact injury. J Neurosurg 90:520–526
Hlatky R, Furuya Y, Valadka AB, Robertson CS (2001) Management of cerebral perfusion pressure. Semin Respir Crit Care Med 22:3–12
Steiner LA, Czosnyka M, Piechnik SK, Smielewski P, Chatfield D, Menon DK, Pickard JD (2002) Continuous monitoring of cerebrovascular pressure reactivity allows determination of optimal cerebral perfusion pressure in patients with traumatic brain injury. Crit Care Med 30:733–738
Kirkpatrick PJ, Chan KH (1997) Transcranial Doppler. In: Reilly P, Bullock MR (eds) Head injury. Chapman & Hall, London, pp 243–259
McQuire JC, Sutcliffe JC, Coats TJ (1998) Early changes in middle cerebral artery blood flow velocity after head injury. J Neurosurg 89:526–532
Aaslid R, Markwalder TM, Nornes H (1982) Noninvasive transcranial Doppler ultrasound recording of flow velocity in basal cerebral arteries. J Neurosurg 57:769–774
Chan KH, Miller JD, Dearden NM (1992) Intracranial blood flow velocity after head injury: relationship to severity of injury, time, neurological status and outcome. J Neurol Neurosurg Psychiatry 55:787–791
van Santbrink H, Schouten JW, Steyerberg EW, Avezaat CJ, Maas AI (2002) Serial transcranial Doppler measurements in traumatic brain injury with special focus on the early posttraumatic period. Acta Neurochir (Wien) 144:1141–1149
Czosnyka M, Matta BF, Smielewski P, Kirkpatrick PJ, Pickard JD (1998) Cerebral perfusion pressure in head-injured patients: a noninvasive assessment using transcranial Doppler ultrasonography. J Neurosurg 88:802–808
Chan KH, Miller JD, Dearden NM, Andrews PJ, Midgley S (1992) The effect of changes in cerebral perfusion pressure upon middle cerebral artery blood flow velocity and jugular bulb venous oxygen saturation after severe brain injury. J Neurosurg 77:55–61
Marshall LF, Marshall SB, Klauber MR, van Berkum Clark M (1991) A new classification of head injury based on computerized tomography. J Neurosurg 75(Suppl):S14–S20
Jennett B (1997) Outcome after severe head injury. In: Reilly P, Bullock MR (eds) Head injury. Chapman & Hall, London, pp 439–461
Bishop CC, Powell S, Rutt D, Browse NL (1986) Transcranial Doppler measurement of middle cerebral artery blood flow velocity: a validation study. Stroke 17:913–915
Czosnyka M, Richards H, Kirkpatrick P, Pickard J (1994) Assessment of cerebral autoregulation with ultrasound and laser doppler wave forms—an experimental study in anesthetized rabbits. Neurosurgery 35:287–293
Ducrocq X, Hassler W, Moritake K, Newell DW, von Reutern GM, Shiogai T, Smith RR (1998) Consensus opinion on diagnosis of cerebral circulatory arrest using Doppler sonography: Task Force Group on cerebral death of the Neurosonology Research Group of the World Federation of Neurology. J Neurol Sci 159:145–150
Trabold F, Meyer PG, Blanot S, Carli PA, Orliaguet GA (2004) The prognostic value of transcranial Doppler studies in children with moderate and severe head injury. Intensive Care Med 30:108–112
Voulgaris SG, Partheni M, Kaliora H, Haftouras N, Pessach IS, Polyzoidis KS (2005) Early cerebral monitoring using the transcranial Doppler pulsatility index in patients with severe brain trauma. Med Sci Monit 11:CR49–52
Jaffres P, Brun J, Declety P, Bosson JL, Fauvage B, Schleiermacher A, Kaddour A, Anglade D, Jacquot C, Payen JF (2005) Transcranial Doppler to detect on admission patients at risk for neurological deterioration following mild and moderate brain trauma. Intensive Care Med 31:785–790
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ract, C., Le Moigno, S., Bruder, N. et al. Transcranial Doppler ultrasound goal-directed therapy for the early management of severe traumatic brain injury. Intensive Care Med 33, 645–651 (2007). https://doi.org/10.1007/s00134-007-0558-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-007-0558-6