Abstract
Purpose
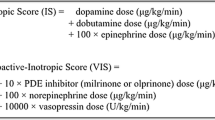
Prospective validation of the vasoactive-inotropic score (VIS) and inotrope score (IS) in infants after cardiovascular surgery.
Methods
Prospective observational study of 70 infants (≤90 days of age) undergoing cardiothoracic surgery. VIS and IS were assessed at 24 (VIS24, IS24), 48 (VIS48, IS48), and 72 (VIS72, IS72) h after surgery. Maximum VIS and IS scores in the first 48 h were also calculated (VIS48max and IS48max). The primary outcome was length of intubation. Additional outcomes included length of intensive care (ICU) stay and hospitalization, cardiac arrest, mortality, time to negative fluid balance, peak lactate, and change in creatinine.
Results
Based on receiver-operating characteristic (ROC) analysis, the area under the curve (AUC) was highest for VIS48 to identify prolonged intubation time. AUC for the primary outcome was higher for VIS than IS at all time points assessed. On multivariate analysis VIS48 was independently associated with prolonged intubation (OR 22.3, p = 0.002), prolonged ICU stay (OR 8.1, p = 0.017), and prolonged hospitalization (OR 11.3, p = 0.011). VIS48max, IS48max, and IS48 were also associated with prolonged intubation, but not prolonged ICU or hospital stay. None of the scores were associated with time to negative fluid balance, peak lactate, or change in creatinine.
Conclusion
In neonates and infants, a higher VIS at 48 h after cardiothoracic surgery is strongly associated with increased length of ventilation, and prolonged ICU and total hospital stay. At all time points assessed, VIS is more predictive of poor short-term outcome than IS. VIS may be useful as an independent predictor of outcomes.
Similar content being viewed by others
References
Parr GV, Blackstone EH, Kirklin JW (1975) Cardiac performance and mortality early after intracardiac surgery in infants and young children. Circulation 51:867–874
Wernovsky G, Wypij D, Jonas RA, Mayer JE Jr, Hanley FL, Hickey PR, Walsh AZ, Chang AC, Castaneda AR, Newburger JW et al (1995) Postoperative course and hemodynamic profile after the arterial switch operation in neonates and infants. A comparison of low-flow cardiopulmonary bypass and circulatory arrest. Circulation 92:2226–2235
Froese NR, Sett SS, Mock T, Krahn GE (2009) Does troponin-I measurement predict low cardiac output syndrome following cardiac surgery in children? Crit Care Resusc 11:116–121
Hoffman TM, Wernovsky G, Atz AM, Kulik TJ, Nelson DP, Chang AC, Bailey JM, Akbary A, Kocsis JF, Kaczmarek R, Spray TL, Wessel DL (2003) Efficacy and safety of milrinone in preventing low cardiac output syndrome in infants and children after corrective surgery for congenital heart disease. Circulation 107:996–1002
Millar KJ, Thiagarajan RR, Laussen PC (2007) Glucocorticoid therapy for hypotension in the cardiac intensive care unit. Pediatr Cardiol 28:176–182
Moffett BS, Mott AR, Nelson DP, Goldstein SL, Jefferies JL (2008) Renal effects of fenoldopam in critically ill pediatric patients: a retrospective review. Pediatr Crit Care Med 9:403–406
Burton GL, Kaufman J, Goot BH, da Cruz EM (2011) The use of arginine vasopressin in neonates following the Norwood procedure. Cardiol Young 21:536–544
Mastropietro CW, Clark JA, Delius RE, Walters HL 3rd, Sarnaik AP (2008) Arginine vasopressin to manage hypoxemic infants after stage I palliation of single ventricle lesions. Pediatr Crit Care Med 9:506–510
Mastropietro CW, Rossi NF, Clark JA, Chen H, Walters H 3rd, Delius R, Lieh-Lai M, Sarnaik AP (2010) Relative deficiency of arginine vasopressin in children after cardiopulmonary bypass. Crit Care Med 38:2052–2058
Gaies MG, Gurney JG, Yen AH, Napoli ML, Gajarski RJ, Ohye RG, Charpie JR, Hirsch JC (2010) Vasoactive-inotropic score as a predictor of morbidity and mortality in infants after cardiopulmonary bypass. Pediatr Crit Care Med 11:234–238
Jacobs ML, Jacobs JP, Jenkins KJ, Gauvreau K, Clarke DR, Lacour-Gayet F (2008) Stratification of complexity: the risk adjustment for congenital heart surgery-1 method and the aristotle complexity score—past, present, and future. Cardiol Young 18(Suppl 2):163–168
Lacour-Gayet F, Clarke D, Jacobs J, Gaynor W, Hamilton L, Jacobs M, Maruszewski B, Pozzi M, Spray T, Tchervenkov C, Mavroudis C (2004) The Aristotle score for congenital heart surgery. Semin Thorac Cardiovasc Surg Pediatr Card Surg Annu 7:185–191
Li J, Zhang G, Holtby H, Cai S, Walsh M, Caldarone CA, Van Arsdell GS (2008) Significant correlation of comprehensive Aristotle score with total cardiac output during the early postoperative period after the Norwood procedure. J Thorac Cardiovasc Surg 136:123–128
Lambert J, Lipkovich I (2008) A macro for getting more out of your ROC curve. SAS Global Forum 2008. SAS, San Antonio
Li J, Zhang G, Holtby H, Humpl T, Caldarone CA, Van Arsdell GS, Redington AN (2006) Adverse effects of dopamine on systemic hemodynamic status and oxygen transport in neonates after the Norwood procedure. J Am Coll Cardiol 48:1859–1864
Acknowledgments
We would like to thank Dr. James Jaggers for his assistance in preparing this manuscript. We would also like to recognize the nurses and staff of the CICU and CTRC at the Children’s Hospital of Colorado for their valuable contributions to our project. This study was supported by grant MO1-RR00069, General Clinical Research Centers Program, NCRR, NIH.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Davidson, J., Tong, S., Hancock, H. et al. Prospective validation of the vasoactive-inotropic score and correlation to short-term outcomes in neonates and infants after cardiothoracic surgery. Intensive Care Med 38, 1184–1190 (2012). https://doi.org/10.1007/s00134-012-2544-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-012-2544-x