Abstract
Introduction and hypothesis
The objective of the study was to estimate prevalence of urinary incontinence (UI) health care utilization in women from the population up to specialty care.
Methods
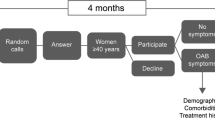
The General Longitudinal Overactive Bladder Evaluation–UI (GLOBE-UI) is a population-based study on the natural history of UI in women ≥ 40 years of age. Prevalence of UI was estimated by using the Bladder Health Survey (BHS). Survey data were linked with electronic health records to build the different steps of the iceberg of disease. Descriptive statistics were used to estimate the prevalence estimates at all levels of the iceberg.
Results
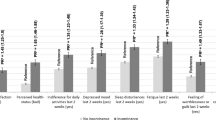
A total sample of 7,059 women received the BHS. Of those, 3,316 (47 %) responded. Prevalence of UI was 1,366 (41 %). Women with or without UI did not differ by age or marital status. However, women with versus without UI were more parous (91 vs 87 %), significantly more overweight or obese (74 vs 61 %), and more likely to have a college education or higher (54 vs 46 %), P < 0.01. Nine hundred fifty-eight (73 %) women with UI reported duration of more than 2 years and 72 % reported moderate to severe UI symptoms. Of all 1,366 women with BHS UI diagnosis, only 339 (25 %) sought care, 313 (23 %) received some care, and 164 (12 %) received subspecialty care.
Conclusions
UI is a highly prevalent disease. Only a minority with UI appears to seek care and a fraction sees a pelvic floor specialist. It is important not only to educate women, but also primary care providers about this highly prevalent yet treatable condition.


Similar content being viewed by others
References
Abrams P, Kelleher CJ, Kerr LA, Rogers RG (2000) Overactive bladder significantly affects quality of life. Am J Manag Care 6:S580–S590
Simeonova Z, Milsom I, Kullendorff AM, Molander U, Bengtsson C (1999) The prevalence of urinary incontinence and its influence on the quality of life in women from an urban Swedish population. Acta Obstet Gynecol Scand 78:546–551
Melville JL, Fan MY, Rau H, Nygaard IE, Katon WJ (2009) Major depression and urinary incontinence in women: temporal associations in an epidemiologic sample. Am J Obstet Gynecol 201:490.e1–490.e7
Hannestad YS, Rortveit G, Sandvik H, Hunskaar S, Norwegian EPINCONT study. Epidemiology of Incontinence in the County of Nord-Trøndelag (2000) A community-based epidemiological survey of female urinary incontinence: the Norwegian EPINCONT study. Epidemiology of Incontinence in the County of Nord-Trøndelag. J Clin Epidemiol 53:1150–1157
Thom D (1998) Variation in estimates of urinary incontinence prevalence in the community: effects of differences in definition, population characteristics, and study type. J Am Geriatr Soc 46:473–480
Milsom I (2000) The prevalence of urinary incontinence. Acta Obstet Gynecol Scand 79:1056–1059
Minassian VA, Drutz HP, Al-Badr A (2003) Urinary incontinence as a worldwide problem. Int J Gynaecol Obstet 82:327–338
Hannestad YS, Rortveit G, Hunskaar S (2002) Help-seeking and associated factors in female urinary incontinence. The Norwegian EPINCONT Study. Epidemiology of Incontinence in the County of Nord-Trøndelag. Scand J Prim Health Care 20:102–107
Kinchen KS, Burgio K, Diokno AC, Fultz NH, Bump R, Obenchain R (2003) Factors associated with women’s decisions to seek treatment for urinary incontinence. J Womens Health (Larchmt) 12:687–698
Shaw C, Brittain K, Tansey R, Williams K (2008) How people decide to seek health care: a qualitative study. Int J Nurs Stud 45:1516–1524
Verbrugge LM, Ascione FJ (1987) Exploring the iceberg. Common symptoms and how people care for them. Med Care 25:539–569
Lipton RB, Stewart WF, Celentano DD, Reed ML (1992) Undiagnosed migraine headaches. A comparison of symptom-based and reported physician diagnosis. Arch Intern Med 152:1273–1278
Hu TW, Wagner TH, Bentkover JD, Leblanc K, Zhou SZ, Hunt T (2004) Costs of urinary incontinence and overactive bladder in the United States: a comparative study. Urology 63:461–465
O’Donnell M, Lose G, Sykes D, Voss S, Hunskaar S (2005) Help-seeking behaviour and associated factors among women with urinary incontinence in France, Germany, Spain and the United Kingdom. Eur Urol 47:385–392, discussion 392
Stewart WF, Minassian VA, Hirsch AG, Kolodner K, Fitzgerald M, Burgio K et al (2010) Predictors of variability in urinary incontinence and overactive bladder symptoms. Neurourol Urodyn 29:328–335
Hirsch AG, Minassian VA, Dilley A, Sartorius J, Stewart WF (2010) Parity is not associated with urgency with or without urinary incontinence. Int Urogynecol J 21:1095–1102
Sandvik H, Seim A, Vanvik A, Hunskaar S (2000) A severity index for epidemiological surveys of female urinary incontinence: comparison with 48-hour pad-weighing tests. Neurourol Urodyn 19:137–145
Melville JL, Katon W, Delaney K, Newton K (2005) Urinary incontinence in US women: a population-based study. Arch Intern Med 165:537–542
Minassian VA, Stewart WF, Hirsch AG (2008) Why do stress and urge incontinence co-occur much more often than expected? Int Urogynecol J Pelvic Floor Dysfunct 19:1429–1440
Minassian VA, Stewart WF, Wood CG (2008) Urinary incontinence in women: variation in prevalence estimates and risk factors. Obstet Gynecol 111:324–331
Dooley Y, Lowenstein L, Kenton K, FitzGerald M, Brubaker L (2008) Mixed incontinence is more bothersome than pure incontinence subtypes. Int Urogynecol J Pelvic Floor Dysfunct 19:1359–1362
Frick AC, Huang AJ, Van den Eeden SK, Knight SK, Creasman JM, Yang J et al (2009) Mixed urinary incontinence: greater impact on quality of life. J Urol 182:596–600
Shaw C, Tansey R, Jackson C, Hyde C, Allan R (2001) Barriers to help seeking in people with urinary symptoms. Fam Pract 18:48–52
Frieden TR (2010) A framework for public health action: the health impact pyramid. Am J Public Health 100:590–595
Nygaard IE, Heit M (2004) Stress urinary incontinence. Obstet Gynecol 104:607–620
Shamliyan T, Wyman J, Bliss DZ, Kane RL, Wilt TJ (2007) Prevention of urinary and fecal incontinence in adults. Evid Rep Technol Assess (Full Rep) 161:1–379
Irwin DE, Milsom I, Kopp Z, Abrams P, EPIC Study Group (2008) Symptom bother and health care-seeking behavior among individuals with overactive bladder. Eur Urol 53:1029–1037
Hägglund D, Walker-Engström ML, Larsson G, Leppert J (2003) Reasons why women with long-term urinary incontinence do not seek professional help: a cross-sectional population-based cohort study. Int Urogynecol J Pelvic Floor Dysfunct 14:296–304, discussion 304
Eaker S, Bergström R, Bergström A, Adami HO, Nyren O (1998) Response rate to mailed epidemiologic questionnaires: a population-based randomized trial of variations in design and mailing routines. Am J Epidemiol 147:74–82
Dallosso HM, Matthews RJ, McGrother CW, Clarke M, Perry SI, Shaw C et al (2003) An investigation into nonresponse bias in a postal survey on urinary symptoms. BJU Int 91:631–636
Conflicts of interest
This research was funded by National Institute of Health/National Institute of Diabetes and Digestive and Kidney Diseases, grant # RO1 DK082551. No author on this paper has a conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Minassian, V.A., Yan, X., Lichtenfeld, M.J. et al. The iceberg of health care utilization in women with urinary incontinence. Int Urogynecol J 23, 1087–1093 (2012). https://doi.org/10.1007/s00192-012-1743-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1743-x