Abstract
Introduction and hypothesis
This study evaluated factors and their prevalence associated with urinary (UI) and fecal (FI) incontinence during and after a woman’s first pregnancy.
Methods
Nulliparous Chinese women with no UI or FI before pregnancy were studied with a standardized questionnaire for UI and FI from early pregnancy until 12 months after childbirth. Maternal characteristics and obstetric data were analyzed using descriptive analysis, independent sample t test, chi-square test, and logistic regression.
Results
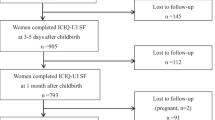
Three hundred and twenty-eight (74.2 %) women completed the study. The prevalence of antenatal UI increased with gestation. Overall, 192 (58.5 %), 60 (18.3 %), and 76 (23.1 %) had normal vaginal delivery, instrumental delivery, and cesarean section, respectively. Twelve months after delivery, prevalence of stress urinary incontinence (SUI) and urge urinary incontinence (UUI) was 25.9 % [95 % confidence interval (CI) 21.5–30.6] and 8.2 % (95 % CI 5.2–11.2), respectively. In those who delivered vaginally, the prevalence was 29.7 % and 9.1 %, respectively. Prevalence of FI was 4.0 % (95 % CI 1.9–6.1). On logistic regression, vaginal delivery [odds ratio (OR) 3.6], antenatal SUI (OR 2.8), and UUI (OR 2.4) were associated with SUI. Antenatal UUI (OR 6.4) and increasing maternal body mass index (BMI) at the first trimester (OR 1.2) were associated with UUI. Antenatal FI was associated with FI (OR 6.1).
Conclusions
The prevalence of SUI, UUI, and FI were 25.9 %, 8.2 %, and 4.0 %, respectively, 12 months after delivery. Vaginal delivery, antenatal SUI, and UUI were associated with SUI; antenatal UUI and increasing maternal BMI at the first trimester were associated with UUI. Antenatal FI was associated with FI. Pregnancy, regardless of route of delivery and obstetric practice, had an effect on UI and FI.
Similar content being viewed by others
References
Thom DH, Rortveit G (2010) Prevalence of postpartum urinary incontinence: a systematic review. Acta Obstet et Gynecol 89:1511–1522
Burgio KL, Zyczynski H, Locher JL, Richter HE, Redden DT, Wright KC (2003) Urinary incontinence in the 12-month postpartum period. Obstet Gynecol 102:1291–1298
Brown SJ, Donath S, MacArthur C, McDonald EA, Krastev AH (2010) Urinary incontinence in nulliparous women before and during pregnancy: prevalence, incidence, and associated risk factors. Int Urogynecol J 21:193–202
Zhu L, Li L, Lang J, Xu T (2012) Prevalence and risk factors for peri- and postpartum urinary incontinence in primiparous women in China: a prospective longitudinal study. Int Urogynecol J 23:563–572
Schraffordt ES, Vervest HAM, Oostvolgel HJM (2003) Anorectal symptoms after various modes of vaginal delivery. Int Urogynecol J Pelvic Floor Dysfunct 14:244–249
Yang X, Zhang HX, Yu HY, Gao XL, Yang HX, Dong Y (2010) The prevalence of fecal incontinence and urinary incontinence in primiparous postpartum Chinese women. Eur J Obstet Gynecol Reprod Biol 152:214–217
Solans-Domenech M, Sanchez E, Espuna-Pons M, Pelvic Floor Research Group (2010) Urinary and anal incontinence during pregnancy and postpartum. Obstet Gynecol 115:618–628
Burgio KL, Matthews KA, Engel BT (1991) Prevalence, incidence and correlates of urinary incontinence in healthy middle-aged women. J Urol 146:1225–1229
Borello-France D, Burgio KL, Richter H, Zyczynski H, Fitzgerald MP, Whitehead W et al (2006) Fecal and urinary incontinence in primiparous women. Obstet Gynecol 108:863–872
Zacharin RF (1977) “A Chinese anatomy” – the pelvic supporting tissues of the Chinese and Occidental female compared and contrasted. Aust NZJ Obstet Gynaec 17:1–11
Howard D, DeLancey JO, Tunn R, Ashton Miller JA (2000) Racial differences in the structure and function of the stress urinary continence mechanism. Obstet Gynecol 95:713–717
Dietz HP (2003) Do Asian women have less pelvic organ mobility than Caucasians? Int Urogynecol J Pelvic Floor Dysfunct 14:250–253
Shek K, Dietz H (2010) Intrapartum risk factors for levator trauma. BJOG 117:1485–1492
Hong Kong College of Obstetricians & Gynaecologists (2004) Territory-wide Obstetrics and Gynaecology Audit. Hong Kong College of Obstetricians and Gynaecologists Web. http://hkcog.obg.cuhk.edu.hk/public/docs/audit/audit_og_2004.asp. Accessed 22 October 2012.
Gossett DR, Su RD (2008) Episiotomy practice in a community hospital setting. J Reprod Med 53:803–808
Chan SS, Cheung RY, Yiu AK, Li JC, Lai BP, Choy KW et al (2011) Chinese validation of Pelvic Floor Distress Inventory (PFDI) and Pelvic Floor Impact Questionnaire (PFIQ). Int Urogynecol J 22:1305–1312
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J et al (2010) An International Urogynecologic Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J 21:5–26
Chan SS, Cheung RY, Yiu KW, Lee LL, Pang AW, Choy KW et al (2012) Prevalence of levator ani muscle injury in Chinese women after first delivery. Ultrasound Obst Gynecol 39:704–709
Leung TY, Leung TN, Sahota DS, Chan OK, Chan LW, Fung TY et al (2008) Trends in maternal obesity and associated risks of adverse pregnancy outcomes in a population of Chinese women. BJOG 115:1529–1537
Glazener CMA, Herbison GP, MacArthur C, Lancashire R, McGee MA, Grant AM et al (2006) New postnatal urinary incontinence: obstetric and other risk factors in primiparae. BJOG 113:208–217
Chaliha C, Kalia V, Stanton SL, Monga A, Sultan AH (1999) Antenatal prediction of postpartum urinary and fecal incontinence. Obstet Gynecol 94:689–694
Brown S, Gartland D, Donath S, MacArthur C (2011) Effects of prolonged second stage, method of birth, timing of caesarean section and other obstetric risk factors on postnatal urinary incontinence: an Australian nulliparous cohort study. BJOG 118:991–1000
Arya LA, Jackson ND, Myers DL, Verma A (2001) Risk of new onset urinary incontinence after forceps and vacuum delivery in primiparous women. Am J Obstet Gynecol 185:1318–1323, discussion 1323-1324
Serati M, Salvatore S, Khullar V, Uccella S, Bertelli E, Ghezzi F et al (2008) Prospective study to assess risk factors for pelvic floor dysfunction after delivery. Acta Obstet Gynecol Scand 87:313–318
Ekstrom A, Altman D, Wiklund I, Larsson C, Andolf E (2008) Planned cesarean section versus planned vaginal delivery: comparison of lower urinary tract symptoms. Int Urogynecol J 19:459–465
Groutz A, Helpman L, Gold R, Pauzner D, Lessing JB, Gordon D (2007) First vaginal delivery at an older age: does it carry an extra risk for the development of stress urinary incontinence? Neurourol Urodynam 26:779–782
Rortveit G, Daltveit AK, Hannestad YS, Hunskaar S, Norwegian EPINCONT Study (2003) Urinary incontinence after vaginal delivery or cesarean section. N Engl J Med 348:900–907
Casey BM, Schaffer JK, Bloom SL, Heartwell SF, McIntire DD, Leveno KJ (2005) Obstetric antecedents for postpartum pelvic floor dysfunction. AJOG 192:1655–1662
MacArthur C, Glazener C, Lancashire R, Herbison P, Wilson D, Grant A (2005) Faecal incontinence and mode of first and subsequent delivery: a six-year longitudinal study. BJOG 112:1075–1082
Dahlen H, Homer C (2008) Perineal trauma and postpartum perineal morbidity in Asian and non-Asian primiparous women giving birth in Australia. J Obstet Gynecol Neonatal Nurs 37:455–463
Acknowledgements
This study obtained grants from Health and Health Service Research Fund from Department of Health Bureau of Government of Hong Kong S. A. R.
Details of ethics approval
Ethics approval for the study was granted by the Joint Chinese University of Hong Kong — New Territories East Cluster Clinical Research Ethics Committee (CRE -2009.257) on 17 July 2009.
Funding
This study obtained grants from Health and Health Service Research Fund from Department of Health Bureau of Government of Hong Kong S. A. R.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chan, S.S.C., Cheung, R.Y.K., Yiu, K.W. et al. Prevalence of urinary and fecal incontinence in Chinese women during and after their first pregnancy. Int Urogynecol J 24, 1473–1479 (2013). https://doi.org/10.1007/s00192-012-2004-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-2004-8