Abstract
A new method of assessing neurological function and pathology in the newborn infant is being developed based on the transmission of near-infrared light across the brain. Absorption by blood over a range of wavelengths reveals a strong dependency on oxygenation status, and measurements of transmitted light enable the spatial variation in the concentrations of the oxygenated and de-oxygenated forms of hemoglobin to be derived. Optical tomography has so far provided static three-dimensional maps of blood volume and oxygenation as well as dynamic images revealing the brain’s response to sensory stimulation and global hemodynamic changes. The imaging modality is being developed as a safe and non-invasive tool that can be utilized at the cotside in intensive care. Optical tomography of the healthy infant brain is also providing a means of studying neurophysiological processes during early development and the potential consequences of prematurity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Over the past 25 years there has been a dramatic increase in the survival of infants born prematurely. However, despite the advances in neonatal intensive care, brain injury in the perinatal period remains a significant cause of death or permanent and severe impairment [1]. A major development in the care of these vulnerable infants was the ability to image the brain using ultrasound, first described by Pape et al. [2]. This is now a routine clinical tool and provides good anatomical information, particularly in infants with periventricular hemorrhage and post-hemorrhagic hydrocephalus. However, the correlation between brain structure and function is not straightforward. The ability to assess functional integrity of the brain would represent a major advance in the brain-orientated care of critically ill neonates.
Alterations in cerebral perfusion and oxygenation have been described and implicated in the pathophysiology of brain injury in both preterm and term infants [3]. Regional variations in cerebral oxygenation are also known to exist, so that while global oxygenation may appear adequate, regional variations leave areas of the brain at risk of permanent neurological damage. Currently, there is no clinical technique that can provide repeated quantitative regional information on cerebral oxygenation at the cotside.
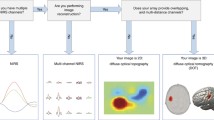
The potential of near-infrared radiation for monitoring cerebral oxygenation and hemodynamics has been widely known since Jöbsis [4] first demonstrated that transmittance measurements could be used to monitor the degree of oxygenation of hemoglobin and cytochrome aa3. While hemoglobin, only present in red blood cells, provides an indicator of blood oxygenation, cytochrome aa3 is an enzyme in the oxidative metabolic pathway, and provides an indicator of tissue oxygenation. This led to the development and increasingly widespread use of clinical near-infrared spectroscopy (NIRS), which offers a safe, non-invasive means of monitoring cerebral function at the bedside [5]. Typically, NIRS monitors the intensity of light passing through brain tissue at two or more wavelengths and converts the observed changes in attenuation into changes in the cerebral concentrations of oxyhemoglobin [HbO2] and deoxyhemoglobin [Hb], which then yield the mean cerebral oxygen saturation. Although NIRS has become an effective research tool for studying infant cerebral hemodynamics, metabolism and neural activation [6–11], researchers have explored the possibility of extending NIRS into an imaging modality. The principle challenge underlying imaging with light is to minimize the blurring effects of scatter. Whereas measurable amounts of near-infrared light can be detected after propagating across several centimeters of brain tissue, widespread scatter ensures that any initial directionality of an incident beam is entirely lost after traveling only a few millimeters.
Two closely related imaging approaches have been developed, known as optical tomography and optical topography [12]. For optical topography, measurements of diffusely reflected light are acquired at small (<3 cm) source-detector separations over an area of the scalp. By keeping the separation low, measured signals are relatively high and therefore may be acquired quickly, enabling brain activity with characteristic responses as fast as 100 ms or so to be studied and images to be displayed in real-time. Optical topography has been widely used to study the evoked response of the infant brain to a broad variety of sensory stimuli [13–16]. However, the small separations restrict the sensitivity to surface (cortical) tissues.
By comparison, three-dimensional (3D) optical tomography is a significantly more challenging task, requiring sophisticated reconstruction algorithms and more sensitive and expensive technology. While much of the development has been (and continues to be) focused on breast imaging [17–20], the methodology and instrumentation are generally the same for brain imaging. In the following sections we review the principles behind optical tomography and its uses so far for acquiring images of the newborn infant brain.
Optical tomography
Optical tomography is based on the general principle that a finite set of measurements of transmitted light between pairs of points on the surface is sufficient to reconstruct the 3D distribution of internal scattering and absorbing properties [21]. The instrumentation consists of an array of optical sources and detectors arranged over the infant scalp (Fig. 1a). A measurement with each source-detector pair is sensitive to the absorbing and scattering properties of tissues within a “banana-shaped” volume known as the photon measurement density function (PMDF) as illustrated in Fig. 1b [22]. In principle, images can be reconstructed by “back-projecting” along each PMDF in a manner analogous to X-ray computed tomography (CT). First, it is necessary to estimate the shapes of the PMDFs using a mathematical model of light transport within the tissue. Since the internal optical properties are initially unknown, a homogenous model based on the estimated average properties of tissues is often employed for this purpose. However, the form of each PMDF is strongly influenced by heterogeneity in the optical properties, and differences between the true and modeled distributions of properties can lead to significant errors in the image. Therefore, using a so-called “non-linear” approach, some investigators employ an iterative scheme to derive refined estimates of the PMDFs. Iterations normally start with a first guess for the optical properties consisting of homogenous distributions of absorption and scatter. The images obtained after each iteration are then used to generate new PMDFs, and this process is repeated until no further improvements in the absorption and scatter images are observed. Unfortunately, unlike X-ray CT, optical tomography image reconstruction is both ill-posed (the solution may not be unique or cannot be achieved through stable convergence) and highly underdetermined (the number of unknowns, i.e., pixels in the image, far exceeds the amount of data) [21]. To make the problem more tractable, optical tomography has so far depended on models of light propagation in tissue based on various simplified assumptions, which can lead to inaccuracies in the images. However, advances in theory and computing technology is enabling the development of increasingly more sophisticated reconstruction techniques. The underlying theory and state-of-the-art reconstruction methods are described in detail in recent topical reviews by Arridge [21] and by Gibson et al. [23].
The ultimate goal of optical tomography is to generate 3D images that represent the absolute absorbing and scattering properties of the investigated tissue, with the highest possible spatial resolution and quantitative accuracy. While absorption properties measured at two or more wavelengths can provide information on blood volume and oxygenation within the brain, scatter may be a valuable indicator of variation in myelination [23]. To acquire such images from a single set of measurements on an infant head requires a very precise knowledge of the head geometry and of the locations of the sources and detectors. So far, at least, it has proven difficult to achieve the required degree of precision for optical tomography of the infant brain due to the irregularity of head shapes and due to technical constraints resulting from the comfort and safety requirements of the head/instrument interface [24]. This imaging approach also demands a mathematical model that can mimic all possible distributions of optical properties within the infant head (including non-scattering regions) and an accurate estimate of the noise characteristics of the instrumentation [23]. Reconstruction of the absolute optical properties is significantly aided by acquiring a second set of measurements on a so-called reference object with known (and typically homogenous) optical properties using identical source and detector locations. In principal, differences between the two sets of measurements enables the tissue properties to be derived, while errors due to geometrical uncertainties largely cancel, as do some systematic sources of error in the measurements [25]. This technique is widely employed for optical tomography of the breast [20, 26, 27]. Previous attempts to reconstruct 3D maps of absolute optical properties of the infant brain are summarized in “Static imaging of the infant brain” section.
Meanwhile, an alternative approach to optical tomography is to generate images of changes in optical properties that occur due to a natural or induced alteration in blood volume and/or oxygenation. This requires obtaining two sets of data, before and after the change, which can normally be achieved in rapid succession without movement of the interface or adjustments to the instrument. So-called “difference imaging” has been shown to be highly robust when uncertainties in tissue geometry are significant or when very simple tissue models are employed [25]. In most situations it is appropriate to assume that scattering properties have remained unchanged, which further simplifies the image reconstruction problem. However, quantitative accuracy of the derived changes is inevitably compromised if the reconstruction algorithm includes no prior knowledge of the absolute distributions of scatter and absorption. The difference imaging approach is commonly applied to optical topography of evoked response to sensory stimuli by acquiring baseline data prior to activation [14–16], although averaging over several repeated stimuli is often necessary due to the weakness of the signal. Optical imaging of the natural variation in vascular response has been pioneered by the group of Dr. Randall Barbour at the State University of New York, who synchronize data acquisition with the cardiac cycle [28]. Optical tomography of sensory stimulation and global hemodynamic changes in the newborn infant brain is reviewed in “3D imaging of hemodynamic activity” section.
Static imaging of the infant brain
Optical tomography of the neonatal brain was first demonstrated by the group of Dr. David Benaron at Stanford University [29, 30]. Their imaging system measures the flight times of photons that scatter across the brain between points on the head circumference using a flexible headband that holds up to 34 pairs of source and detector fibers in contact with the head (Fig. 2). The head is illuminated using pulses of near-infrared light at each source location, and the distribution of photon flight times (commonly known as the temporal point spread function, or TPSF) at each detector fiber location is recorded. Compared to simple intensity measurements, time-of-flight data contain significantly greater information about the internal optical properties, enable the effects of scatter and absorption to be distinguished and are comparatively insensitive to the coupling of light into and out of the surface [31, 32].
Optical tomography of the infant brain using a flexible headband developed by researchers at Stanford University [30]
Images representing a transverse slice across the brain were reconstructed by the Stanford group using a simple method that involves deriving absorption and scattering parameters from each TPSF using an analytical model, and then back-projecting along anticipated statistically averaged paths of photons between each source-detector pair [33]. Scans performed on infants at a variety of gestational ages successfully identified intracranial hemorrhage [30, 34] and focal regions of low oxygenation after acute stroke [29]. Figure 3 shows an image obtained on an infant with large bilateral intraventricular hemorrhages (confirmed by ultrasound), which clearly indicates the lesions. The grayscale is proportional to the total optical absorbance at 785 nm [34]. A major drawback is the prolonged scan times (up to several hours), which is a consequence of the low source power (100 μW average) and the use of a single electronic detector. The source power also limits the maximum source-detector separation to about 5 cm, and therefore information about optical properties near the center of the infant brain is inevitably compromised. A further limitation of the method is the acknowledged simplicity of the image reconstruction algorithm, which ignores the inherent 3D nature of photon migration in tissues and the highly heterogeneous structure of the infant head.
An optical absorption image of an infant brain revealing large bilateral hemorrhages (indicated by arrows), generated using the Stanford University optical tomography system [34]
These technical limitations have been largely overcome by our group at University College London (UCL) using a 32-channel time-resolved system [35]. The instrument illuminates the infant head at up to 32 points sequentially while detecting transmitted light at 32 other locations simultaneously, resulting in a maximum of 1,024 separate TPSFs with an overall temporal resolution of about 100 ps. A fiber laser source is used that provides mean powers of up to 55 mW at each of two wavelengths (780 nm and 815 nm), enabling signals to be measured across the entire thickness of an infant head, and a full scan to be performed in about 5–10 min. Initial studies on premature infants used custom-made foam-lined, plastic helmets whose dimensions were based on a series of measurements acquired from digital photographs of each infant prior to the study. However, more recent studies have been performed using an adaptable helmet that provides sufficient adjustment to accommodate head sizes of infants from about 24 weeks gestational age to term (Fig. 4).
To date, nearly 40 infants have been scanned using the UCL system, with roughly two thirds of the scans yielding data sufficient for reliable image reconstruction. Failure to obtain images has been due to a variety of factors, such as infant movement, a poorly fitting helmet or instrumental instability. Images representing absolute optical properties have been generated with the aid of measurements on homogeneous reference objects placed into the helmet immediately following the infant scan. Three types of reference object have so far been employed: a fluid-filled balloon [36], a fluid-filled latex shell [24] and a compressible head phantom filled with polyvinyl alcohol slime [37], each with uniform tissue-like optical properties. Images of the absorption and scattering properties of the infant brain have been reconstructed using the iterative non-linear algorithm known as TOAST (temporal optical absorption and scattering tomography) developed at UCL by Prof. Simon Arridge and his colleagues [21, 38]. TOAST compares the measured data with the simulated data derived from a computer model of the infant brain and updates the model iteratively until a satisfactory match is achieved. The absorption images reconstructed at the two wavelengths have been used to generate images of regional cerebral blood volume (rCBV) and regional tissue oxygen saturation (rStO2) [39].
Static brain images are images reconstructed with reference to the homogenous phantom with no change in the state of the infant during data acquisition. Images have been reconstructed from both healthy infants [24] and infants with evidence of intraventricular hemorrhage (IVH) on cranial ultrasound scan [24, 36]. We have found the images of rCBV and rStO2 from the healthy infants to be symmetrical, but to exhibit considerable regional heterogeneity. This is consistent with studies of regional cerebral perfusion using SPECT, demonstrating the vulnerability of the periventricular white matter to hypoxic-ischemic injury [40]. This contrasts with images from infants with evidence of unilateral IVH on cranial ultrasound scans. These images are asymmetrical with a greatly increased amount of light absorption on the side of the hemorrhage, consistent with a resolving blood clot. Figure 5 shows coronal slices from 3D images of rCBV and rStO2 from a 34-week gestational age infant with left-sided intraventricular hemorrhage, and a corresponding cranial ultrasound scan. A distinct area of desaturated hemoglobin on the left side is exhibited (10% compared to 62% on the contralateral side), although more lateral and superficial than the position indicated by the ultrasound scan. An ischemic penumbra surrounding hemorrhagic lesions has been described both in adults and infants [41, 42].
3D imaging of hemodynamic activity
As described above in “Optical tomography” section, imaging changes in optical properties enables a more robust difference imaging approach to be employed without the requirement of reference measurements on a homogeneous object. While effectively used by many groups for optical topography of the cerebral cortex, so far only our group at UCL has attempted whole-brain optical tomography images of hemodynamic changes in infants. The first successful study of global changes resulting from small alterations in ventilator settings was performed on a severely brain-injured 38-week-old female [43]. She had suffered a severe global hypoxic-ischemic insult following uterine rupture, and required mechanical ventilation, sedation and muscle relaxants. After attaching the helmet to the infant, sets of data at two wavelengths (780 nm and 815 nm) were acquired over a period of 3 h for various settings of the respiration rate and fractions of inspired oxygen. This enabled images of changes in optical properties to be reconstructed corresponding to specific changes in the partial pressures of either carbon dioxide (PaCO2) or oxygen (PaO2) or both. For example, Fig. 6 shows (a) coronal and (b) sagittal slices revealing the changes in absorption at 815 nm due to an increase in PaCO2. Vasodilation in response to increased PaCO2 produces an expected global increase CBV. Figure 6 appears to show the two cerebral hemispheres with central regions of lower absorption at the expected position of the ventricles.
Meanwhile, a recent pilot study at UCL on a small cohort of pre-term babies has led to the first 3D optical images of the entire neonatal head during motor-evoked response [44]. Data were acquired during bilateral passive arm movement, repeated for 12 source positions. Figure 7a shows the change in absorption at 780 nm occurring within the brain of a 33-week-old male infant during passive movement of the left arm, and Fig. 7b shows the corresponding change for a 34-week-old female infant during passive movement of the right arm. The dominant feature in both cases is an increase within the contralateral cerebral hemisphere near the expected position of the motor cortex. As shown elsewhere [44], the increased absorption is a result of increases in both [HbO2] and [Hb]. This is consistent with reports on measurements on neonates using NIRS [45], optical topography [46] and BOLD fMRI [47], but is different from the changes observed in adults in whom [Hb] decreases during evoked responses. Unlike functional magnetic resonance imaging (fMRI), these images were obtained in unsedated infants at the cotside, and by obtaining images of [HbO2] and [Hb] independently it is possible to distinguish the increased oxygen extraction due to brain activation from changes in regional blood volume due to vasodilation.
Discussion
Currently, the biggest challenges in 3D optical tomography are to improve quantitation and spatial resolution. Phantom experiments and clinical studies suggest that optical tomography is unlikely to yield a spatial resolution of better that 1–2 cm. Although this resolution is inferior to that of established modalities such as MRI, X-ray imaging and ultrasound, it is comparable to positron emission tomography (PET), which, like optical tomography, depends on the facility to distinguish between the functionality of normal and abnormal tissues, rather than the display of precise anatomical information. Improved resolution is possible by incorporating prior anatomical information from generic MRI scans of newborn infants, and this approach is being actively pursued by our group at UCL. Instrumentation remains another significant challenge. The current 3D tomographic system is large, complex and requires highly specialist individuals to perform the measurements, process the data and reconstruct the images. We anticipate that this situation will rapidly improve during the next few years as the associated technology becomes cheaper, smaller and easier to use. Despite the need for further improvements, results achieved so far indicate that optical tomography has the potential to become a powerful tool for understanding the early development and function of the neonatal brain, and in the diagnosis and management of critically ill babies in intensive care.
References
Marlow N, Wolke D, Bracewell MA, Samara M, EPICure Study Group (2005) Neurologic and developmental disability at six years of age after extremely preterm birth. N Engl J Med 352:9–19
Pape KE, Blackwell RJ, Cusick G, Sherwood A, Houang MT, Thornburn RJ, Reynolds EOR (1997) Ultrasound detection of brain damage in preterm infants. Lancet 1:1261–1264
Volpe JJ (2001) Neurology of the Newborn. WB Saunders, Philidelphia 2001:428–493
Jöbsis FF (1977) Noninvasive, infrared monitoring of cerebral and myocardial oxygen sufficiency and circulatory parameters. Science 198:1264–1267
Ferrari M, Mottola L, Quaresima V (2004) Principles, techniques, and limitations of near infrared spectroscopy. Can J Appl Physiol 29:463–487
Brazy JE, Darrell V, Lewis MD, Mitnick MH, Jöbsis FF (1985) Noninvasive monitoring of cerebral oxygenation in preterm infants: Preliminary observations. Pediatrics 75:217–225
Meek JH, Elwell CE, McCormick DC, Edwards AD, Townsend JP, Steward AL, Wyatt JS (1999) Abnormal cerebral hemodynamics in perinatally asphyxiated neonates related to outcome. Arch Dis Child 81:F110–F115
Soul JS, du Plessis AJ (1999) New technologies in pediatric neurology: near-infrared spectroscopy. Semin Pediatr Neurol 6:101–110
Nicklin SE, Hassan IA, Wickramasinghe YA, Spencer SA (2002) The light still shines, but not that brightly? The current status of perinatal near infrared spectroscopy. Arch Dis Child Fetal Neonatal Ed 88:F263–F268
Wolf M, von Siebenthal K, Keel M, Dietz V, Baenziger O, Bucher HU (2002) Comparison of three methods to measure absolute haemoglobin concentration in neonates by near-infrared spectrophotometry. J Biomed Opt 7:221–227
Wilcox T, Bortfeld H, Woods R, Wruck E, Boas DA (2005) Using near-infrared spectroscopy to assess neural activation during object processing in infants. J Biomed Opt 10:011010
Hebden JC (2003) Advances in optical imaging of the newborn infant brain. Psychophysiol 40:501–510
Chance B, Anday E, Nioka S, Zhou S, Hong L, Worden K, Li C, Murray T, Ovetsky Y, Pidikiti D, Thomas R (1998) A novel method for fast imaging of brain function, non-invasively, with light. Opt Express 2:411–423
Hintz SR, Benaron DA, Siegal AM, Zourabian A, Stevenson DK, Boas DA (2001) Bedside functional imaging of the premature infant brain during passive motor activation. J Perinat Med 29:335–343
Kotilahti K, Nissilä I, Huotilainen M, Mäkelä R, Gavrielides N, Noponen T, Björkman P, Fellman V, Katila T (2005) Bilateral hemodynamic responses to auditory stimulation in newborn infants. Neuroreport 16:1373–1377
Taga G, Konishi Y, Maki A, Tachibana T, Fujiwara M, Koizumi H (2000) Spontaneous oscillation of oxy- and deoxy-hemoglobin changes with a phase difference throughout the occipital cortex of newborn infants observed using non-invasive optical topography. Neurosci Lett 282:101–104
Pogue BW, Testorf M, McBride T, Osterberg U, Paulsen K (1997) Instrumentation and Design of a frequency-domain diffuse optical tomography imager for breast cancer detection. Opt Express 1:391–403
Culver JP, Choe R, Holboke MJ, Zubkov L, Durduran T, Slemp A, Ntziachristos V, Chance B, Yodh AG (2003) Three-dimensional diffuse optical tomography in the parallel plane transmission geometry: Evaluation of a hybrid frequency domain/continuous wave clinical system for breast imaging. Med Phys 30:235–247
Schmitz CH, Klemer DP, Hardin R, Katz MS, Pei Y, Graber HL, Levin MB, Levina RD, Franco NA, Solomon WB, Barbour RL (2005) Design and implementation of dynamic near-infrared optical tomographic imaging instrumentation for simultaneous dual-breast measurements. Appl Opt 44:2140–2152
Yates TD, Hebden JC, Gibson AP, Everdell NL, Arridge SR, Douek M (2005) Optical tomography of the breast using a multi-channel time-resolved imager. Phys Med Biol 50:2503–2517
Arridge SR (1999) Optical tomography in medical imaging. Inverse Probl 15:R41–R49
Arridge SR (1995) Photon-measurement density functions. Part I: Analytical forms. Appl Opt 34:7395–7409
Gibson AP, Hebden JC, Arridge SR (2005) Recent advances in diffuse optical imaging. Phys Med Biol 50:R1–R43
Austin T, Hebden JC, Gibson AP, Branco G, Yusof R, Arridge SR, Meek JH, Delpy DT, Wyatt JS (2006) Three-dimensional optical imaging of blood volume and oxygenation in the preterm brain. Neuroimage 31:1426–1433
Gibson AP, Yusof RM, Dehghani H, Riley J, Everdell NL, Richards R, Hebden JC, Schweiger M, Arridge SR, Delpy DT (2003) Optical tomography of a realistic neonatal head phantom. Appl Opt 42:3109–3116
Jiang S, Pogue BW, McBride TO, Paulsen KD (2003) Quantitative analysis of near-infrared tomography: sensitivity to the tissue-simulating precalibration phantom. J Biomed Opt 8:308–315
Li A, Miller EL, Kilmer ME, Brukilacchio TJ, Chaves T, Stott J, Zhang Q, Wu T, Chorlton M, Moore RH, Kopans DB, Boas DA (2003) Tomographic optical breast imaging guided by three-dimensional mammography. Appl Opt 42:5181–5190
Bluestone AY, Abdoulaev G, Schmitz CH, Barbour RL, Hielscher AH (2001) Three-dimensional optical tomography of hemodynamics in the human head. Opt Express 9:272–286
Benaron DA, Hintz SR, Villringer A, Boas D, Kleinschmidt A, Frahm J, Hirth C, Obrig H, van Houten JC, Kermit EL, Cheong W-F, Stevenson DK (2000) Noninvasive functional imaging of human brain using light. J Cereb Blood Flow Metab 20:469–477
Hintz SR, Benaron DA, van Houten JP, Duckworth JL, Liu FWH, Spilman SD, Stevenson DK, Cheong W-F (1998) Stationary headband for clinical time-of-flight optical imaging at the bedside. Photochem Photobiol 68:361–369
Schweiger M, Arridge SR (1999) Application of temporal filters to time resolved data in optical tomography. Phys Med Biol 44:1699–1717
Arridge SR, Lionheart WRB (1998) Non-uniqueness in optical tomography. Opt Lett 23:882–884
Benaron DA, Ho DC, Spilman S, van Houten JP, Stevenson DK (1994) Non-recursive linear algorithms for optical imaging in diffusive media. Adv Exp Med Biol 361:215–222
Hintz SR, Cheong W-F, van Houten JP, Stevenson DK, Benaron DA (1999) Bedside imaging of intracranial hemorrhage in the neonate using light: comparison with ultrasound, computed tomography, and magnetic resonance imaging. Pediatr Res 45:54–59
Schmidt FEW, Fry ME, Hillman EMC, Hebden JC, Delpy DT (2000) A 32-channel time-resolved instrument for medical optical tomography. Rev Sci Instrum 71:256–265
Hebden JC, Gibson A, Yusof R, Everdell N, Hillman EMC, Delpy DT, Arridge SR, Austin T, Meek JH, Wyatt JS (2002) Three-dimensional optical tomography of the premature infant brain. Phys Med Biol 47:4155–4166
Hebden JC, Price BD, Gibson AP, Royle G (2006) A soft deformable tissue-equivalent phantom for diffuse optical tomography. Phys Med Biol 51(21):5581–5590
Arridge SR, Schweiger M (1997) Image reconstruction in optical tomography. Phil Trans Royal Soc London Series B-Biol Sci 352:717–726
Hillman EMC (2002) Experimental and theoretical investigations of near-infrared tomographic imaging methods and clinical applications. PhD Thesis University of London. http://www.medphys.ucl.ac.uk/research/borl/theses.htm
Borch K, Greisen G (1998) Blood flow distribution in the normal human preterm brain. Pediatr Res 43:28–33
Powers WJ, Press GA, Grubb RL, Gado M, Raichle ME (1987) The effect of hemodynamically significant carotid artery disease on the hemodynamic status of the cerebral circulation. Ann Intern Med 106:27–34
Volpe JJ, Herscovitch P, Perlman JM, Raichie ME (1983) Positron emission tomography in the newborn: extensive impairment of regional cerebral blood flow with intraventricular haemorrhage and haemorrhagic intracerebral involvement. Pediatrics 72:589–601
Hebden JC, Gibson A, Austin T, Yusof R, Everdell N, Delpy DT, Arridge SR, Meek JH, Wyatt JS (2004) Imaging changes in blood volume and oxygenation in the newborn infant brain using three-dimensional optical tomography. Phys Med Biol 49:1117–1130
Gibson AP, Austin T, Everdell NL, Schweiger M, Arridge SR, Meek JH, Wyatt JS, Delpy DT, Hebden JC (2006) Three-dimensional whole-head optical tomography of passive motor evoked responses in the neonate. Neuroimage 30:521–528
Meek JH, Firbank M, Elwell CE, Atkinson J, Braddick O, Wyatt JS (1998) Regional haemodynamic responses to visual stimulation in awake infants. Pediatr Res 43:840–843
Kusaka T, Kawada K, Okubo K, Nagano K, Namba M, Okada H, Imai T, Isobe K, Itoh S (2004) Noninvasive optical imaging in the visual cortex in young infants. Hum Brain Mapp 22:122–132
Martin E, Joeri P, Loenneker T, Ekatodramis D, Vitacco D, Hennig J, Marcar VL (1999) Visual processing in infants and children using functional MRI. Pediatr Res 46:135–140
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hebden, J.C., Austin, T. Optical tomography of the neonatal brain. Eur Radiol 17, 2926–2933 (2007). https://doi.org/10.1007/s00330-007-0659-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-007-0659-1