Abstract
Purpose
Infants with epilepsy often have a catastrophic course. There is a reluctance to operate in the very young, due to the perception of an unacceptable risk of morbidity with early operations. The purpose of this investigation was to better characterize the efficacy and safety of epilepsy surgery in infants.
Methods
Epilepsy operations performed on children under 1 year old, between 2002 and 2013, were reviewed for demographic information, epilepsy characteristics, surgical approach, outcomes, and surgical complications.
Results
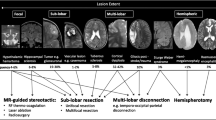
Twenty-five patients, ages 11 days to 11.5 months (mean 4.7) at operation, were identified. All had daily seizures. Twenty-two (88 %) had an abnormal magnetic resonance imaging (MRI). Sixteen (64 %) patients underwent hemispherotomy at initial operation. Seven (28 %) infants had grid placement followed by focal resection. Focal cortical dysplasia was the most common pathology (40 %) followed by hemimegalencephaly (32 %). Complications occurred in 36 % of patients. These included hydrocephalus in five patients (20 %). Two patients had significant intra-operative complications which required unplanned staging of their operations. Both recovered without permanent injury. Mean follow-up was 62.4 months. Twenty patients (80 %) are seizure-free, and 10 (40 %) are off anticonvulsant medication. Two patients are Engel class 2, and the remaining three patients were Engel class 4, one of whom died with status epilepticus from the contralateral hemisphere.
Conclusion
Infants with localization-related catastrophic epilepsy can have excellent outcomes from early epilepsy surgery. Complications are common in this patient group and proper diagnosis can be challenging. Young age should not exclude infants with catastrophic epilepsy from consideration for early surgical intervention.




Similar content being viewed by others
References
Camfield C, Camfield P (2008) Twenty years after childhood-onset symptomatic generalized epilepsy the social outcome is usually dependency or death: a population-based study. Dev Med Child Neurol 50:859–863
Camfield CS, Camfield PR (2007) Long-term social outcomes for children with epilepsy. Epilepsia 48(Suppl 9):3–5
Wirrell E, Wong-Kisiel L, Mandrekar J, Nickels K (2012) Predictors and course of medically intractable epilepsy in young children presenting before 36 months of age: a retrospective, population-based study. Epilepsia 53:1563–1569
Sillanpaa M, Shinnar S (2010) Long-term mortality in childhood-onset epilepsy. N Engl J Med 363:2522–2529
Teutonico F, Mai R, Veggiotti P, Francione S, Tassi L, Borrelli P, Balottin U, LoRusso G (2013) Epilepsy surgery in children: evaluation of seizure outcome and predictive elements. Epilepsia 54(Suppl 7):70–76
Englot DJ, Breshears JD, Sun PP, Chang EF, Auguste KI (2013) Seizure outcomes after resective surgery for extra-temporal lobe epilepsy in pediatric patients. J Neurosurg Pediatr 12:126–133
Steinbok P, Gan PY, Connolly MB, Carmant L, Barry Sinclair D, Rutka J, Griebel R, Aronyk K, Hader W, Ventureyra E, Atkinson J (2009) Epilepsy surgery in the first 3 years of life: a Canadian survey. Epilepsia 50:1442–1449
Dunkley C, Kung J, Scott RC, Nicolaides P, Neville B, Aylett SE, Harkness W, Cross JH (2011) Epilepsy surgery in children under 3 years. Epilepsy Res 93:96–106
Duchowny M, Jayakar P, Resnick T, Harvey AS, Alvarez L, Dean P, Gilman J, Yaylali I, Morrison G, Prats A, Altman N, Birchansky S, Bruce J (1998) Epilepsy surgery in the first three years of life. Epilepsia 39:737–743
Hauptman JS, Pedram K, Sison CA, Sankar R, Salamon N, Vinters HV, Mathern GW (2012) Pediatric epilepsy surgery: long-term 5-year seizure remission and medication use. Neurosurgery 71:985–993
Loddenkemper T, Holland KD, Stanford LD, Kotagal P, Bingaman W, Wyllie E (2007) Developmental outcome after epilepsy surgery in infancy. Pediatrics 119:930–935
Honda R, Kaido T, Sugai K, Takahashi A, Kaneko Y, Nakagwa E, Sasaki M, Otsuki T (2013) Long-term developmental outcome after early hemispherotomy for hemimegalencephaly in infants with epileptic encephalopathy. Epilepsy Behav 29:30–35
Freitag H, Tuxhorn I (2005) Cognitive function in preschool children after epilepsy surgery: rationale for early intervention. Epilepsia 46:561–567
Gowda S, Salazar F, Bingaman WE, Kotagal P, Lachhwani DL, Gupta A, Davis S, Niezgoda J, Wyllie E (2010) Surgery for catastrophic epilepsy in infants 6 months of age and younger. J Neurosurg Pediatr 5:603–607
Engel JJ (ed) (1993) Surgical treatment of the epilepsies. Raven, New York
Schramm J, Behrens E, Entzian W (1995) Hemispherical deafferentation: an alternative to functional hemispherectomy. Neurosurgery 36:509–515, discussion 515–506
Villemure JG, Mascott CR (1995) Peri-insular hemispherotomy: surgical principles and anatomy. Neurosurgery 37:975–981
Flack S, Ojemann J, Haberkern C (2008) Cerebral hemispherectomy in infants and young children. Paediatr Anaesth 18:967–973
Lew SM, Matthews AE, Hartman AL, Haranhalli N (2013) Posthemispherectomy hydrocephalus: results of a comprehensive, multiinstitutional review. Epilepsia 54:383–389
Blumcke I, Thom M, Aronica E, Armstrong DD, Vinters HV, Palmini A, Jacques TS, Avanzini G, Barkovich AJ, Battaglia G, Becker A, Cepeda C, Cendes F, Colombo N, Crino P, Cross JH, Delalande O, Dubeau F, Duncan J, Guerrini R, Kahane P, Mathern G, Najm I, Ozkara C, Raybaud C, Represa A, Roper SN, Salamon N, Schulze-Bonhage A, Tassi L, Vezzani A, Spreafico R (2011) The clinicopathologic spectrum of focal cortical dysplasias: a consensus classification proposed by an ad hoc task force of the ILAE diagnostic methods commission. Epilepsia 52:158–174
Bittar RG, Rosenfeld JV, Klug GL, Hopkins IJ, Harvey AS (2002) Resective surgery in infants and young children with intractable epilepsy. J Clin Neurosci 9:142–146
Wyllie E, Comair YG, Kotagal P, Raja S, Ruggieri P (1996) Epilepsy surgery in infants. Epilepsia 37:625–637
Sugimoto T, Otsubo H, Hwang PA, Hoffman HJ, Jay V, Snead OC 3rd (1999) Outcome of epilepsy surgery in the first three years of life. Epilepsia 40:560–565
Taussig D, Dorfmuller G, Fohlen M, Jalin C, Bulteau C, Ferrand-Sorbets S, Chipaux M, Delalande O (2012) Invasive explorations in children younger than 3 years. Seizure 21:631–638
Ramantani G, Kadish NE, Strobl K, Brandt A, Stathi A, Mayer H, Schubert-Bast S, Wiegand G, Korinthenberg R, Stephani U, van Velthoven V, Zentner J, Schulze-Bonhage A, Bast T (2013) Seizure and cognitive outcomes of epilepsy surgery in infancy and early childhood. Eur J Paediatr Neurol 17:498–506
Gonzalez-Martinez JA, Gupta A, Kotagal P, Lachhwani D, Wyllie E, Luders HO, Bingaman WE (2005) Hemispherectomy for catastrophic epilepsy in infants. Epilepsia 46:1518–1525
Glauser TA (2004) Behavioral and psychiatric adverse events associated with antiepileptic drugs commonly used in pediatric patients. J Child Neurol 19(Suppl 1):S25–38
Farwell JR, Lee YJ, Hirtz DG, Sulzbacher SI, Ellenberg JH, Nelson KB (1990) Phenobarbital for febrile seizures–effects on intelligence and on seizure recurrence. N Engl J Med 322:364–369
D’Argenzio L, Colonnelli MC, Harrison S, Jacques TS, Harkness W, Scott RC, Cross JH (2012) Seizure outcome after extratemporal epilepsy surgery in childhood. Dev Med Child Neurol 54:995–1000
Hamer HM, Wyllie E, Luders HO, Kotagal P, Acharya J (1999) Symptomatology of epileptic seizures in the first three years of life. Epilepsia 40:837–844
Vendrame M, Zarowski M, Alexopoulos AV, Wyllie E, Kothare SV, Loddenkemper T (2011) Localization of pediatric seizure semiology. Clin Neurophysiol 122:1924–1928
van der Knaap MS, Valk J (1990) MR imaging of the various stages of normal myelination during the first year of life. Neuroradiology 31:459–470
Duchowny M, Levin B, Jayakar P, Resnick TJ (1994) Neurobiologic considerations in early surgery for epilepsy. J Child Neurol 9(Suppl 2):42–49
Di Rocco C, Iannelli A (2000) Hemimegalencephaly and intractable epilepsy: complications of hemispherectomy and their correlations with the surgical technique. A report on 15 cases. Pediatr Neurosurg 33:198–207
Glass HC, Glidden D, Jeremy RJ, Barkovich AJ, Ferriero DM, Miller SP (2009) Clinical neonatal seizures are independently associated with outcome in infants at risk for hypoxic-ischemic brain injury. J Pediatr 155:318–323
Bourgeois M, Crimmins DW, de Oliveira RS, Arzimanoglou A, Garnett M, Roujeau T, Di Rocco F, Sainte-Rose C (2007) Surgical treatment of epilepsy in Sturge-Weber syndrome in children. J Neurosurg 106:20–28
Kossoff EH, Buck C, Freeman JM (2002) Outcomes of 32 hemispherectomies for Sturge-Weber syndrome worldwide. Neurology 59:1735–1738
Kramer U, Kahana E, Shorer Z, Ben-Zeev B (2000) Outcome of infants with unilateral Sturge-Weber syndrome and early onset seizures. Dev Med Child Neurol 42:756–759
Meador KJ, Loring DW (2013) Risks of in utero exposure to valproate. JAMA 309:1730–1731
Gedzelman ER, Meador KJ (2012) Neurological and psychiatric sequelae of developmental exposure to antiepileptic drugs. Front Neurol 3:182
Conflict of interest
None of the authors has any conflicts of interest to disclose. We confirm that we have read the journal’s position on issues involved in ethical publication and affirm that this report is consistent with those guidelines.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kumar, R.M., Koh, S., Knupp, K. et al. Surgery for infants with catastrophic epilepsy: an analysis of complications and efficacy. Childs Nerv Syst 31, 1479–1491 (2015). https://doi.org/10.1007/s00381-015-2759-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-015-2759-6