Abstract
Objectives
The relationships between shunt infection and predictive factors have not been previously investigated using Artificial Neural Network (ANN) model. The aim of this study was to develop an ANN model to predict shunt infection in a group of children with shunted hydrocephalus.
Materials and methods
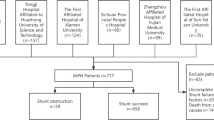
Among more than 800 ventriculoperitoneal shunt procedures which had been performed between April 2000 and April 2011, 68 patients with shunt infection and 80 controls that fulfilled a set of meticulous inclusion/exclusion criteria were consecutively enrolled. Univariate analysis was performed for a long list of risk factors, and those with p value < 0.2 were used to create ANN and logistic regression (LR) models.
Results
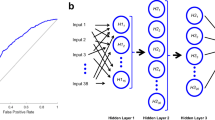
Five variables including birth weight, age at the first shunting, shunt revision, prematurity, and myelomeningocele were significantly associated with shunt infection via univariate analysis, and two other variables (intraventricular hemorrhage and coincided infections) had a p value of less than 0.2. Using these seven input variables, ANN and LR models predicted shunt infection with an accuracy of 83.1 % (AUC; 91.98 %, 95 % CI) and 55.7 % (AUC; 76.5, 95 % CI), respectively. The contribution of the factors in the predictive performance of ANN in descending order was history of shunt revision, low birth weight (under 2000 g), history of prematurity, the age at the first shunt procedure, history of intraventricular hemorrhage, history of myelomeningocele, and coinfection.
Conclusion
The findings show that artificial neural networks can predict shunt infection with a high level of accuracy in children with shunted hydrocephalus. Also, the contribution of different risk factors in the prediction of shunt infection can be determined using the trained network.


Similar content being viewed by others
References
Azimi P, Mohammadi HR (2014) Predicting endoscopic third ventriculostomy success in childhood hydrocephalus: an artificial neural network analysis. J Neurosurg Pediatr 13(4):426–432
Azimi P, Mohammadi HR, Benzel EC, Shahzadi S, Azhari S, Montazeri A (2015) Artificial neural networks in neurosurgery. J Neurol Neurosurg Psychiatry 86(3):251–256
Braga MH, Carvalho GT, Brandão RA, Lima FB, Costa BS (2009) Early shunt complications in 46 children with hydrocephalus. Arq Neuropsiquiatr 67(2 A):273–277
Bruinsma N, Stobberingh EE, Herpers MJ, Vles JS, Weber BJ, Gavilanes DA (2000) Subcutaneous ventricular catheter reservoir and ventriculoperitoneal drain-related infections in preterm infants and young children. Clin Microbiol Infect 6(4):202–206
Caocci G, Baccoli R, Vacca A, Mastronuzzi A, Bertaina A, Piras E, et al. (2010) Comparison between an artificial neural network and logistic regression in predicting acute graft-vs-host disease after unrelated donor hematopoietic stem cell transplantation in thalassemia patients. Exp Hematol 38(5):426–433
Choux M, Genitori L, Lang D, Lena G (1992) Shunt implantation: reducing the incidence of shunt infection. J Neurosurg 77(6):875–880
Dallacasa P, Dappozzo A, Galassi E, Sandri F, Cocchi G, Masi M (1995) Cerebrospinal fluid shunt infections in infants. Childs Nerv Syst 11(11):643–648
Duhaime AC (2006) Evaluation and management of shunt infections in children with hydrocephalus. Clin Pediatr (Phila) 45(8):705–713
Edwards DF, Hollingsworth H, Zazulia AR, Diringer M (1999) Artificial neural networks improve the prediction of mortality in intracerebral hemorrhage. Neurology 53(2):351–357
Gutierrez-Murgas Y, Snowden JN (2014) Ventricular shunt infections: immunopathogenesis and clinical management. J Neuroimmunol 276(1–2):1–8
Kestle JR, Holubkov R, Douglas Cochrane D, Kulkarni AV, Limbrick DD Jr, Luerssen TG, et al. (2016) A new Hydrocephalus Clinical Research Network protocol to reduce cerebrospinal fluid shunt infection. J Neurosurg Pediatr 17(4):391–396
Kestle JR, Riva-Cambrin J, Wellons JC 3rd, Kulkarni AV, Whitehead WE, Walker ML, et al. (2011) A standardized protocol to reduce cerebrospinal fluid shunt infection: the Hydrocephalus Clinical Research Network Quality Improvement Initiative. J Neurosurg Pediatr 8(1):22–29
Konstantelias AA, Vardakas KZ, Polyzos KA, Tansarli GS, Falagas ME (2015) Antimicrobial-impregnated and -coated shunt catheters for prevention of infections in patients with hydrocephalus: a systematic review and meta-analysis. J Neurosurg 122(5):1096–1112
Kulkarni AV, Drake JM, Lamberti-Pasculli M (2001) Cerebrospinal fluid shunt infection: a prospective study of risk factors. J Neurosurg 95-201
Lee JK, Seok JY, Lee JH, Choi EH, Phi JH, Kim SK, et al. (2012) Incidence and risk factors of ventriculoperitoneal shunt infections in children: a study of 333 consecutive shunts in 6 years. J Korean Med Sci 27(12):1563–1568
McCulloch WS, Pitts WH (1943) A logical calculus of the ideas immanent in nervous activity. Bull Math Biophys 5:115–137
McGirt MJ, Zaas A, Fuchs HE, George TM, Kaye K, Sexton DJ (2003) Risk factors for pediatric ventriculoperitoneal shunt infection and predictors of infectious pathogens. Clin Infect Dis 1;36(7):858–862
Moussa WM, Mohamed MA (2016) Efficacy of postoperative antibiotic injection in and around ventriculoperitoneal shunt in reduction of shunt infection: a randomized controlled trial. Clin Neurol Neurosurg 143:144–149
Pirotte BJ, Lubansu A, Bruneau M, Loqa C, Van Cutsem N, Brotchi J (2007) Sterile surgical technique for shunt placement reduces the shunt infection rate in children: preliminary analysis of a prospective protocol in 115 consecutive procedures. Childs Nerv Syst 3(11):1251–1261
Reddy GK, Bollam P, Caldito G (2012) Ventriculoperitoneal shunt surgery and the risk of shunt infection in patients with hydrocephalus: long-term single institution experience. World Neurosurg 78(1–2):155–163
Renier D, Lacombe J, Pierre-Kahn A, Sainte-Rose C, Hirsch JF (1984) Factors causing acute shunt infection. Computer analysis of 1174 operations. J Neurnsurg 61:1072–1078
Rogers EA, Kimia A, Madsen JR, Nigrovic LE, Neuman MI (2012) Predictors of ventricular shunt infection among children presenting to a pediatric emergency department. Pediatr Emerg Care 28(5):405–409
Simon TD, Butler J, Whitlock KB, Browd SR, Holubkov R, Kestle JR (2014) Risk factors for first cerebrospinal fluid shunt infection: findings from a multi-center prospective cohort study. J Pediatr 164(6):1462–1468
Simon TD, Whitlock KB, Riva-Cambrin J, Kestle JR, Rosenfeld M, Dean JM, et al. (2012) Revision surgeries are associated with significant increased risk of subsequent cerebrospinal fluid shunt infection. Pediatr Infect Dis J 31(6):551–556
Spader HS, Hertzler DA, Kestle JR, Riva-Cambrin J (2015) Risk factors for infection and the effect of an institutional shunt protocol on the incidence of ventricular access device infections in preterm infants. J Neurosurg Pediatr 15(2):156–160
Steinbok P, Thompson GB (1976) Complications of ventriculo-vascular shunts: computer analysis of etiological factors. Surg Neurol 5:31–35
Vinchon M, Dhellemmes P (2006) Cerebrospinal fluid shunt infection: risk factors and long-term follow-up. Childs Nerv Syst 22(7):692–697
Vinchon M, Lemaitre MP, Vallée L, Dhellemmes P (2002) Late shunt infection: incidence, pathogenesis, and therapeutic implications. Neuropediatrics 33(4):169–173
Wells DL, Allen JM (2013) Ventriculoperitoneal shunt infections in adult patients. AACN Adv Crit Care 24(1):6–12
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Rights and permissions
About this article
Cite this article
Habibi, Z., Ertiaei, A., Nikdad, M.S. et al. Predicting ventriculoperitoneal shunt infection in children with hydrocephalus using artificial neural network. Childs Nerv Syst 32, 2143–2151 (2016). https://doi.org/10.1007/s00381-016-3248-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-016-3248-2