Abstract
Purpose
Prenatal vitamin D (VitD) deficiency influences children’s health in later life. We aimed to test the associations between maternal VitD status in each of the three trimesters of pregnancy and cord blood 25(OH)D concentrations in newborns.
Methods
Participants were pregnant women recruited from the Shanghai Birth Cohort (SBC) (n = 1100). Of all the participants, 946 completed the collection of venous blood at early (< 16 weeks, T1), mid- (24–28 weeks, T2), and late (32–34 weeks, T3) pregnancy as well as the corresponding cord blood in the newborns. Maternal serum 25(OH)D concentrations were measured by LC–MS/MS, and the information on confounding factors was obtained through a standardized questionnaire.
Results
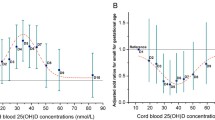
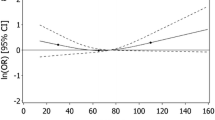
The mean 25(OH)D concentrations at time points T1, T2, T3 in maternal blood and cord blood of the newborns were 26.31 ng/mL, 31.92 ng/mL, 35.62 ng/mL, and 19.77 ng/mL, respectively. Neonatal 25(OH)D level in cord blood was positively correlated with maternal serum 25(OH)D levels at each trimester, and the strongest correlation was found at time point T3.
Conclusion
Maternal 25(OH)D concentrations at each trimester were positively associated with neonatal VitD status in cord blood, and the strongest correlation was found in the late stage of pregnancy, which could be considered as a sensitive time window. Attention should be paid to the nutritional status of VitD during pregnancy to better prevent the VitD deficiency in neonates.




Similar content being viewed by others
References
Chang SW, Lee HC (2019) Vitamin D and health—the missing vitamin in humans. Pediatr Neonatol 60(3):237–244. https://doi.org/10.1016/j.pedneo.2019.04.007
Wheeler BJ, Taylor BJ, de Lange M et al (2018) A longitudinal study of 25-hydroxy vitamin D and parathyroid hormone status throughout pregnancy and exclusive lactation in New Zealand mothers and their infants at 45°S. Nutrients 10(1):E86. https://doi.org/10.3390/nu10010086
Magnus MC, Miliku K, Bauer A et al (2018) Vitamin D and risk of pregnancy related hypertensive disorders: mendelian randomisation study. BMJ 361:k2167. https://doi.org/10.1136/bmj.k2167
Zhao X, Fang R, Yu R et al (2017) Maternal Vitamin D Status in the late second trimester and the risk of severe Preeclampsia in Southeastern China. Nutrients 9(2):138. https://doi.org/10.3390/nu9020138
Xia J, Song Y, Rawal S et al (2019) Vitamin D status during pregnancy and the risk of gestational diabetes mellitus: a longitudinal study in a multiracial cohort. Diabetes Obes Metab 21(8):1895–1905. https://doi.org/10.1111/dom.13748
Pérez-López FR, Pasupuleti V, Mezones-Holguin E et al (2015) Effect of vitamin D supplementation during pregnancy on maternal and neonatal outcomes: a systematic review and meta-analysis of randomized controlled trials. Fertil Steril 103(5):1278–1288. https://doi.org/10.1016/j.fertnstert.2015.02.019
Wang Y, Li H, Zheng M et al (2018) Maternal vitamin D deficiency increases the risk of adverse neonatal outcomes in the Chinese population: a prospective cohort study. PLoS ONE 13(4):e0195700. https://doi.org/10.1371/journal.pone.0195700
Kiely M, O’Donovan SM, Kenny LC et al (2017) Vitamin D metabolite concentrations in umbilical cord blood serum and associations with clinical characteristics in large prospective mother-infant cohort in Ireland. J Steroid Biochem Mol Biol 167:162–168. https://doi.org/10.1016/j.jsbmb.2016.12.006
Hollis BW, Wagner CL (2017) New insights into the vitamin D requirements during pregnancy. Bone Res 5:17030. https://doi.org/10.1038/boneres.2017.30
Shen SY, Xiao WQ, Lu JH et al (2018) Early life vitamin D status and asthma and wheeze: a systematic review and meta-analysis. BMC Pulm Med 18(1):120. https://doi.org/10.1186/s12890-018-0679-4
Miller KM, Hart PH, de Klerk NH et al (2017) Are low sun exposure and/or vitamin D risk factors for type 1 diabetes? Photochem Photobiol Sci 16(3):381–398. https://doi.org/10.1039/c6pp00294c
Larqué E, Morales E, Leis R et al (2018) Maternal and foetal health implications of vitamin D status during pregnancy. Ann Nutr Metab 72(3):179–192. https://doi.org/10.1159/000487370
Courbebaisse M, Souberbielle JC, Baptiste A et al (2019) Vitamin D status during pregnancy and in cord blood in a large prospective French cohort. Clin Nutr 38(5):2136–2144. https://doi.org/10.1016/j.clnu.2018.08.035
Wierzejska R, Jarosz M, Sawicki W et al (2017) Vitamin D concentration in maternal and umbilical cord blood by season. Int J Environ Res Public Health 14(10):E1121. https://doi.org/10.3390/ijerph14101121
Zhang J, Tian Y, Wang W et al (2019) Cohort profile: the Shanghai Birth Cohort. Int J Epidemiol 48(1):21–21g. https://doi.org/10.1093/ije/dyy277
Jiao X, Yuan Y, Wang X et al (2020) Development of a sensitive HPLC-MS/MS method for 25-hydroxyvitamin D(2) and D(3) measurement in capillary blood. J Clin Lab Anal 34(10):e23451. https://doi.org/10.1002/jcla.23451
Institute of Medicine (US) Committee to Review Dietary Reference Intakes for Vitamin D and Calcium; Ross AC, Taylor CL, Yaktine AL, Del Valle HB, editors. Dietary Reference Intakes for Calcium and Vitamin D. Washington (DC): National Academies Press (US) (2011)
Holick MF, Binkley NC, Bischoff-Ferrari HA et al (2011) Evaluation, treatment, and prevention of vitamin D deficiency: An Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 96(7):1911–1930. https://doi.org/10.1210/jc.2011-0385
Baca KM, Simhan HN, Platt RW et al (2016) Low maternal 25-hydroxyvitamin D concentration increases the risk of severe and mild preeclampsia. Ann Epidemiol 26(12):853–857. https://doi.org/10.1016/j.annepidem.2016.09.015
Andersen LB, Jørgensen JS, Jensen TK et al (2015) Vitamin D insufficiency is associated with increased risk of first-trimester miscarriage in the Odense Child Cohort. Am J Clin Nutr 102(3):633–638. https://doi.org/10.3945/ajcn.114.103655
Miliku K, Vinkhuyzen A, Blanken LM et al (2016) Maternal vitamin D concentrations during pregnancy, fetal growth patterns, and risks of adverse birth outcomes. Am J Clin Nutr 103(6):1514–1522. https://doi.org/10.3945/ajcn.115.123752
Zhu P, Tong SL, Hu WB et al (2015) Cord Blood 25-hydroxyvitamin D and Fetal Growth in the China-Anhui Birth Cohort Study. Sci Rep 5:14930. https://doi.org/10.1038/srep14930
Tao RX, Meng DH, Li JJ et al (2018) Current Recommended vitamin D prenatal supplementation and fetal growth: results from the china-anhui birth cohort study. J Clin Endocrinol Metab 103(1):244–252. https://doi.org/10.1210/jc.2017-00850
Tao M, Shao H, Gu J et al (2012) Vitamin D status of pregnant women in Shanghai, China. J Matern Fetal Neonatal Med 25:237–239. https://doi.org/10.3109/14767058.2011.569613
Yun C, Chen J, He Y et al (2017) Vitamin D deficiency prevalence and risk factors among pregnant Chinese women. Public Health Nutr 20(10):1746–1754. https://doi.org/10.1017/S1368980015002980
Bouillon R, Assche FAV, Baelen HV, et al (1981) Influence of the vitamin D-binding protein on the serum concentration of 1,25-dihydroxyvitamin D3. Significance of the free 1,25-dihydroxyvitamin D3 concentration. J Clin Invest 67(3):589–596. https://doi.org/https://doi.org/10.1172/JCI110072.
Halicioglu O, Aksit S, Koc F, et al (2012) Vitamin D deficiency in pregnant women and their neonates in spring time in western Turkey. Paediatr Perinat Epidemiol 26(1):53–60. https://doi.org/10.1111/j.1365-3016.2011.01238.x
Roth DE, Morris SK, Zlotkin S et al (2018) Vitamin D Supplementation in Pregnancy and Lactation and Infant Growth. N Engl J Med 379(6):535–546. https://doi.org/10.1056/NEJMoa1800927
von Websky K, Hasan AA, Reichetzeder C et al (2018) Impact of vitamin D on pregnancy-related disorders and on offspring outcome. J Steroid Biochem Mol Biol 180:51–64. https://doi.org/10.1016/j.jsbmb.2017.11.008
van der Pligt P, Willcox J, Szymlek-Gay EA et al (2018) Associations of maternal vitamin D deficiency with pregnancy and neonatal complications in developing countries: a systematic review. Nutrients 10(5):E640. https://doi.org/10.3390/nu10050640
Park H, Brannon PM, West AA, et al (2016) Vitamin D metabolism varies among women in different reproductive states consuming the same intakes of vitamin D and related nutrients. J Nutr 146: 1537–1545. https://doi.org/https://doi.org/10.3945/jn.116.229971
Karras SN, Wagner CL, Castracane VD (2018) Understanding vitamin D metabolism in pregnancy: from physiology to pathophysiology and clinical outcomes. Metabolism 86:112–123. https://doi.org/10.1016/j.metabol.2017.10.001
Chawla D, Daniels JL, Benjamin-Neelon SE et al (2019) Racial and ethnic differences in predictors of vitamin D among pregnant women in south-eastern USA. J Nutr Sci 8:e8. https://doi.org/10.1017/jns.2019.4
Gould JF, Anderson AJ, Yelland LN et al (2017) Association of cord blood vitamin D with early childhood growth and neurodevelopment. J Paediatr Child Health 53(1):75–83. https://doi.org/10.1111/jpc.13308
Song HB, Xu Y, Yang XW et al (2018) High prevalence of vitamin D deficiency in pregnant women and its relationship with adverse pregnancy outcomes in Guizhou. China J Int Med Res 46(11):4500–4505. https://doi.org/10.1177/0300060518781477
March KM, Chen NN, Karakochuk CD, et al (2015) Maternal vitamin D3 supplementation at 50 mug/d protects against low serum 25- hydroxyvitamin D in infants at 8 wk of age: a randomized controlled trial of 3 doses of vitamin D beginning in gestation and continued in lactation. Am J Clin Nutr 102:402–10. https://doi.org/10.3945/ajcn.114.106385.
O’Callaghan KM, Hennessy A, Hull GLJ et al (2018) Estimation of the maternal vitamin D intake that maintains circulating 25-hydroxyvitamin D in late gestation at a concentration sufficient to keep umbilical cord sera ≥ 25–30 nmol/L: a dose-response, double-blind, randomized placebo-controlled trial in pregnant women at northern latitude. Am J Clin Nutr 108(1):77–91. https://doi.org/10.1093/ajcn/nqy064
Grant CC, Stewart AW, Scragg R, et al (2014) Vitamin D during pregnancy and infancy and infant serum 25-hydroxyvitamin D concentration. Pediatrics 133:e143–53. https://doi.org/10.1542/peds.2013-2602.
Acknowledgements
We are extremely grateful to all the families who took part in this study. And we would like to thank the participating doctors, midwives, and nurses for patient management.
Funding
National Natural Science Foundation of China (Grant No. 81773411), National Key Research and Development Project of China (Grant Nos. 2016YFC1305204, and 2020YFC2008002), Medical and Engineering Cooperation Project of Shanghai Jiao Tong University (Grant No. YG2017ZD15), Shanghai Children's Health Services Capacity Program (grant GDEK201708), the Science and Technology Commission Project of Shanghai Pudong New Area (Grant No. PKJ2017-Y05), the Shanghai Municipal Education Commission— Gaofeng Clinical Medicine Grant Support (Grant No. 20152220), the Shanghai Municipal Commission of Science and Technology Program (Grant No. 13JC1403700), “Eastern Scholar” project supported by Shanghai Municipal Education Commission (Grant No. ZXDF089002), and Shanghai Key Laboratory of Psychotic Disorders (Grant No. 13dz2260500, 14-K06). This study was partly funded by the Shanghai Municipal Health Commission and the Shanghai Jiao Tong University School of Medicine and supported by the National Human Genetic Resources Sharing Service Platform (Grant No.2005DKA21300).
Author information
Authors and Affiliations
Consortia
Contributions
The authors’ contributions were as follows—Xiaodan Yu, Mingqing Xu, Ying Tian, and Jun Zhang conceived of the research idea and designed the study; Xirui Wang, Xianting Jiao, Juan Li, and Fan Yang performed 25(OH)D measurements; Xirui Wang, Xianting Jiao, Mingqing Xu, and Yue Zhang analyzed the data and performed the statistical analysis; Xirui Wang and Xianting Jiao drafted the manuscript; Xiaodan Yu and Mingqing Xu revised the manuscript; Xiaodan Yu and Mingqing Xu supervised or mentored; Xiaodan Yu had primary responsibility for final content. Xiaodan Yu and Mingqing Xu jointly shared the senior authorship. All authors contributed important intellectual content during manuscript drafting or revision and are accountable for the overall work. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Wang, X., Jiao, X., Tian, Y. et al. Associations between maternal vitamin D status during three trimesters and cord blood 25(OH)D concentrations in newborns: a prospective Shanghai birth cohort study. Eur J Nutr 60, 3473–3483 (2021). https://doi.org/10.1007/s00394-021-02528-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-021-02528-w