Abstract
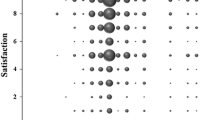
Thyroidectomy has few complications, as a result, many patients are concerned about the prominence of their scar. Performing thyroid surgery through excessively small incisions in order to maximise cosmesis may increase the likelihood of complications. This study investigates the relationship between conventional approach thyroidectomy scar length and patient satisfaction. A validation of self-measurement of neck circumference and thyroidectomy scar was carried out with the measurements taken by patients compared with those taken by an investigator. One hundred consecutive patients who had undergone conventional thyroidectomy and total thyroidectomy within 24 months were invited to measure their scars and neck circumference, and to score their satisfaction on a Likert scale of 1–10. Spearman’s correlation was calculated for the relationship between absolute and relative scar length, and patient satisfaction. Thirty-four patients entered the preliminary study and 80 patients entered the main study (80% response rate). Measurements by patients and investigators were closely associated: Spearman’s Rank correlation coefficient for neck circumference and for scar length were ρ = 0.9, p < 0.0001 and ρ = 0.93, p < 0.0001 respectively. No significant correlation was evident between scar length and patient satisfaction (ρ = 0.068, p = 0.55), or between relative scar length ratio and patient satisfaction (ρ = −0.045, p = 0.69). Mean scar length was 6.96 cm [standard deviation (SD) 2.70], and mean satisfaction score 8.62 (SD 2.04). Thyroidectomy scar length appears to have no association with patient satisfaction. Thyroid surgery should, therefore, not be performed through unnecessarily small incisions for purely aesthetic reasons.


Similar content being viewed by others
References
Miccoli P, Berti P, Raffaelli M, Materazzi G, Baldacci S, Rossi G (2001) Comparison between minimally invasive video-assisted thyroidectomy and conventional thyroidectomy: a prospective randomized study. Surgery 130(6):1039–1043
O’Connell DA, Diamond C, Seikaly H, Harris JR (2008) Objective and subjective scar aesthetics in minimal access vs conventional access parathyroidectomy and thyroidectomy surgical procedures: a paired cohort study. Arch otolaryngol–Head Neck surg 134(1):85–93
Sgourakis G, Sotiropoulos GC, Neuhauser M, Musholt TJ, Karaliotas C, Lang H (2008) Comparison between minimally invasive video-assisted thyroidectomy and conventional thyroidectomy: is there any evidence-based information? Thyroid 18(7):721–727
Rob C, Smith R (1976) Head and neck part II. Operative surgery, 3rd edn. Butterworths, London
El-Labban GM (2009) Minimally invasive video-assisted thyroidectomy versus conventional thyroidectomy: A single-blinded, randomized controlled clinical trial. J minim access surg 5(4):97–102
Perigli G, Cortesini C, Qirici E, Boni D, Cianchi F (2008) Clinical benefits of minimally invasive techniques in thyroid surgery. World J Surg 32(1):45–50
Miccoli P, Minuto MN, Ugolini C, Pisano R, Fosso A, Berti P (2008) Minimally invasive video-assisted thyroidectomy for benign thyroid disease: an evidence-based review. World J Surg 32(7):1333–1340
Seybt MW, Terris DJ (2010) Minimally invasive thyroid cancer surgery. Minerva chir 65(1):39–43
Ruggieri M, Zullino A, Straniero A, Maiuolo A, Fumarola A, Vietri F, D’Armiento M (2010) Is minimally invasive surgery appropriate for small differentiated thyroid carcinomas? Surg today 40(5):418–422
Miccoli P, Materazzi G, Berti P (2010) Minimally invasive thyroidectomy in the treatment of well differentiated thyroid cancers: indications and limits. Curr opin otolaryngol head neck surg 18(2):114–118
Miyano G, Lobe TE, Wright SK (2008) Bilateral transaxillary endoscopic total thyroidectomy. J Pediatr Surg 43(2):299–303
Simple Interactive Statistical Analysis: Correlations procedures (1999) SISA. http://www.quantitativeskills.com/sisa/statistics/correl.htm. Accessed March 2011
Ware J, Snow K, Kosinski M (1993) SF-36 Health survey: manual and interpretation guide. Quality-Metric Incorporated, Lincoln, Rhode Island
Development of the World Health Organization WHOQOL-BREF quality of life assessment. The WHOQOL Group (1998) Psychol Med 28(3):551–558
Conflict of interest
The authors declare they have no conflict of interest. The authors received no funding for this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Toll, E.C., Loizou, P., Davis, C.R. et al. Scars and satisfaction: do smaller scars improve patient-reported outcome?. Eur Arch Otorhinolaryngol 269, 309–313 (2012). https://doi.org/10.1007/s00405-011-1613-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-011-1613-z