Abstract
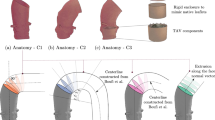
Valve-in-valve transcatheter aortic valve replacement (VIV-TAVR) has proven to be a successful treatment for high risk patients with failing aortic surgical bioprostheses. However, thrombus formation on the leaflets of the valve has emerged as a major issue in such procedures, posing a risk of restenosis, thromboembolism, and reduced durability. In this work we attempted to understand the effect of deployment position of the transcatheter heart valve (THV) on the spatio-temporal flow field within the sinus in VIV-TAVR. Experiments were performed in an in vitro pulsatile left heart simulator using high-speed Particle Image Velocimetry (PIV) to measure the flow field in the sinus region. The time-resolved velocity data was used to understand the qualitative and quantitative flow patterns. In addition, a particle tracking technique was used to evaluate relative thrombosis risk via sinus washout. The velocity data demonstrate that implantation position directly affects sinus flow patterns, leading to increased flow stagnation with increasing deployment height. The particle tracking simulations showed that implantation position directly affected washout time, with the highest implantation resulting in the least washout. These results clearly demonstrate the flow pattern and flow stagnation in the sinus is sensitive to THV position. It is, therefore, important for the interventional cardiologist and cardiac surgeon to consider how deployment position could impact flow stagnation during VIV-TAVR.







Similar content being viewed by others
Abbreviations
- VIV:
-
Valve-in-valve
- TAVR:
-
Transcatheter aortic valve replacement
- THV:
-
Transcatheter heart valve
References
Azadani, A. N., N. Jaussaud, P. B. Matthews, L. Ge, T. A. M. Chuter, and E. E. Tseng. Transcatheter aortic valves inadequately relieve stenosis in small degenerated bioprostheses. Interact. CardioVasc. Thorac. Surg. 11:70–77, 2010.
Brown, J. M., S. M. O’Brien, C. Wu, J. A. H. Sikora, B. P. Griffith, and J. S. Gammie. Isolated aortic valve replacement in North America comprising 108,687 patients in 10 years: changes in risks, valve types, and outcomes in the Society of Thoracic Surgeons National Database. J. Thorac. Cardiovasc. Surg. 137:82–90, 2009.
Cannegieter, S. C., F. R. Rosendaal, and E. Briet. Thromboembolic and bleeding complications in patients with mechanical heart valve prostheses. Circulation 89:635–641, 1994.
Carabello, B. A., and W. J. Paulus. Aortic stenosis. Lancet 373:956–966, 2009.
Clark, M. A., F. G. Duhay, A. K. Thompson, M. J. Keyes, L. G. Svensson, R. O. Bonow, B. T. Stockwell, and D. Cohen. Clinical and economic outcomes after surgical aortic valve replacement in Medicare patients. Risk Manag. Healthc. Policy 5:117, 2012.
De Marchena, E., J. Mesa, S. Pomenti, C. Marin y Kall, X. Marincic, K. Yahagi, E. Ladich, R. Kutz, Y. Aga, M. Ragosta, A. Chawla, M. E. Ring, and R. Virmani. Thrombus formation following transcatheter aortic valve replacement. J. Am. Coll. Cardiol. Interv. 8:728–739, 2015.
Dvir, D., M. Barbanti, J. Tan, and J. G. Webb. Transcatheter aortic valve-in-valve implantation for patients with degenerative surgical bioprosthetic valves. Curr. Probl. Cardiol. 39:7–27, 2014.
Dvir, D., J. G. Webb, N. Piazza, P. Blanke, M. Barbanti, S. Bleiziffer, D. A. Wood, D. Mylotte, A. B. Wilson, J. Tan, D. Stub, C. Tamburino, R. Lange, and J. Leipsic. Multicenter evaluation of transcatheter aortic valve replacement using either SAPIEN XT or CoreValve: Degree of device oversizing by computed-tomography and clinical outcomes. Catheter Cardiovasc. Interv. 86(3):508–515, 2015.
Dvir, D., et al. Transcatheter aortic valve implantation in failed bioprosthetic surgical valves. JAMA 312:162, 2014.
Hansson, N., T. Leetmaa, J. A. Leipsic, K. Jensen, H. R. Andersen, J. M. Jensen, J. Webb, P. Blanke, M. Tang, and B. Nørgaard. TCT-665 early aortic transcatheter heart valve thrombosis: diagnostic value of contrast-enhanced multislice computed tomography. J. Am. Coll. Cardiol. 64:B193–B194, 2014.
Harjai, K. J., J.-M. Paradis, and S. Kodali. Transcatheter aortic valve replacement: game-changing innovation for patients with aortic stenosis. Annu. Rev. Med. 65:367–383, 2014.
Knight, J., V. Kurtcuoglu, K. Muffly, W. Marshall, P. Stolzmann, L. Desbiolles, B. Seifert, D. Poulikakos, and H. Alkadhi. Ex vivo and in vivo coronary ostial locations in humans. Surg. Radiol. Anat. 31:597–604, 2009.
Ku, D. N. Blood flow in arteries. Annu. Rev. Fluid Mech. 29:399–434, 1997.
Makkar, R. R., G. Fontana, H. Jilaihawi, T. Chakravarty, K. F. Kofoed, O. de Backer, F. M. Asch, C. E. Ruiz, N. T. Olsen, A. Trento, J. Friedman, D. Berman, W. Cheng, M. Kashif, V. Jelnin, C. A. Kliger, H. Guo, A. D. Pichard, N. J. Weissman, S. Kapadia, E. Manasse, D. L. Bhatt, M. B. Leon, and L. Søndergaard. Possible subclinical leaflet thrombosis in bioprosthetic aortic valves. N. Engl. J. Med. 2015. doi:10.1056/NEJMoa1509233.
Midha, P. A., V. Raghav, J. F. Condado, S. Arjunon, D. E. Uceda, S. Lerakis, V. H. Thourani, V. Babaliaros, and A. P. Yoganathan. How can we help a patient with a small failing bioprosthesis? JACC Cardiovasc. Interv. 8:2026–2033, 2015.
Moore, B., and L. P. Dasi. Spatiotemporal complexity of the aortic sinus vortex. Exp. Fluids 55:1770, 2014.
Nkomo, V. T., J. M. Gardin, T. N. Skelton, J. S. Gottdiener, C. G. Scott, and M. Enriquez-Sarano. Burden of valvular heart diseases: a population-based study. Lancet 368:1005–1011, 2006.
Petschek, H., D. Adamis, and A. R. Kantrowitz. Stagnation flow thrombus formation. Trans. Am. Soc. Artif. Intern. Organs 14:256–260, 1968.
Prasad, A. K. Particle Image Velocimetry. Berlin: Springer, pp. 51–60, 2007.
Raffel, M., C. E. Willert, S. Wereley, and J. Kompenhans. Particle Image Velocimetry. Berlin: Springer, 2007. doi:10.1007/978-3-540-72308-0
Reul, H., A. Vahlbruch, M. Giersiepen, T. Schmitz-Rode, V. Hirtz, and S. Effert. The geometry of the aortic root in health, at valve disease and after valve replacement. J. Biomech. 23:181–191, 1990.
Saikrishnan, N., S. Gupta, and A. P. Yoganathan. Hemodynamics of the boston scientific lotus™ valve: an in vitro study. Cardiovasc. Eng. Technol. 4:427–439, 2013.
Saikrishnan, N., and A. Yoganathan. Transcatheter valve implantation can alter the fluid flow fields in the aortic sinuses and ascending aorta: an in vitro study. J. Am. Coll. Cardiol. 61:E1957, 2013.
Wootton, D. M., and D. N. Ku. Fluid mechanics of vascular systems, diseases, and thrombosis. Annu. Rev. Biomed. Eng. 1:299–329, 1999.
Yap, C. H., N. Saikrishnan, G. Tamilselvan, and A. P. Yoganathan. Experimental measurement of dynamic fluid shear stress on the aortic surface of the aortic valve leaflet. Biomech. Model Mechanobiol. 11:171–182, 2012.
Acknowledgments
The authors would like to acknowledge the members of the Cardiovascular Fluid Mechanics Laboratory for their assistance and feedback. The authors are grateful to our collaborators at Emory University Hospital—Drs. Vinod Thourani, Vasilis Babaliaros, Stamatios Lerakis, and Jose Condado for providing the valve models and assistance with placing the work in the context of clinical relevance. The glycerin used in this study was generously provided by Procter & Gamble. This study at the CFM lab at the Georgia Institute of Technology was made possible through discretionary funds available to the Principal Investigator including the Wallace H Coulter Endowed Chair.
Conflicts of Interest
The authors have no conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Lakshmi Prasad Dasi oversaw the review of this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Midha, P.A., Raghav, V., Okafor, I. et al. The Effect of Valve-in-Valve Implantation Height on Sinus Flow. Ann Biomed Eng 45, 405–412 (2017). https://doi.org/10.1007/s10439-016-1642-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-016-1642-2