Abstract
Purpose
Helicobacter pylori infection is considered to have a positive association with colorectal neoplasms. In this study, we evaluated the association between H. pylori infection and colorectal adenomas, based on the characteristics of these adenomas in Korea, where the prevalence of H. pylori infection is high and the incidence of colorectal cancer continues to increase.
Methods
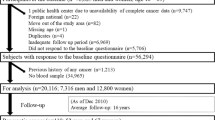
The study cohort consisted of 4,466 subjects who underwent colonoscopy and esophagogastroduodenoscopy during screening (1,245 colorectal adenomas vs. 3,221 polyp-free controls). We compared the rate of H. pylori infection between patients with adenoma and polyp-free control cases, using multivariable logistic regression analysis.
Results
The overall rate of positive H. pylori infection was higher in adenoma cases than in polyp-free control cases (55.0 vs. 48.5%, p < 0.001). The odds ratio (OR) of positive H. pylori infection in patients with adenoma compared to polyp-free controls was 1.28 (95% CI 1.11–1.47). The positive association of H. pylori infection with colorectal adenomas was more prominent in advanced adenomas (OR 1.84, 95% CI 1.25–2.70) and multiple adenomas (OR 1.72, 95% CI 1.26–2.35). Based on the location of these adenomas, the OR was significant only in patients with colonic adenomas (OR 1.31, 95% CI 1.13–1.52) and not in those with rectal adenoma (OR 0.85, 95% CI 0.58–1.24).
Conclusion
Helicobacter pylori infection is an independent risk factor for colonic adenomas, especially in cases of advanced or multiple adenomas, but not for rectal adenomas.

Similar content being viewed by others
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61:69–90
Center MM, Jemal A, Ward E (2009) International trends in colorectal cancer incidence rates. Cancer Epidemiol Biomarkers Prev 18:1688–1694
Jung KW, Won YJ, Kong HJ, Oh CM, Lee DH, Lee JS (2014) Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2011. Cancer Res Treat 46:109–123
Shin A, Hong CW, Sohn DK, Kim BC, Han KS, Chang HJ, Kim J, Oh JH (2011) Associations of cigarette smoking and alcohol consumption with advanced or multiple colorectal adenoma risks: a colonoscopy-based case–control study in Korea. Am J Epidemiol 174:552–562
Kim BC, Shin A, Hong CW, Sohn DK, Han KS, Ryu KH, Park BJ, Nam JH, Park JW, Chang HJ, Choi HS, Kim J, Oh JH (2012) Association of colorectal adenoma with components of metabolic syndrome. Cancer Causes Control 23:727–735
Fu Z, Shrubsole MJ, Smalley WE, Wu H, Chen Z, Shyr Y, Ness RM, Zheng W (2012) Lifestyle factors and their combined impact on the risk of colorectal polyps. Am J Epidemiol 176:766–776
Sanchez NF, Stierman B, Saab S, Mahajan D, Yeung H, Francois F (2012) Physical activity reduces risk for colon polyps in a multiethnic colorectal cancer screening population. BMC Res Notes 5:312
Wang F, Sun MY, Shi SL, Lv ZS (2014) Helicobacter pylori infection and normal colorectal mucosa-adenomatous polyp-adenocarcinoma sequence: a meta-analysis of 27 case–control studies. Colorectal Dis 16:246–252
Zhao YS, Wang F, Chang D, Han B, You DY (2008) Meta-analysis of different test indicators: Helicobacter pylori infection and the risk of colorectal cancer. Int J Colorectal Dis 23:875–882
Zumkeller N, Brenner H, Zwahlen M, Rothenbacher D (2006) Helicobacter pylori infection and colorectal cancer risk: a meta-analysis. Helicobacter 11:75–80
Zhang Y, Hoffmeister M, Weck MN, Chang-Claude J, Brenner H (2012) Helicobacter pylori infection and colorectal cancer risk: evidence from a large population-based case–control study in Germany. Am J Epidemiol 175:441–450
Guo Y, Li HY (2014) Association between Helicobacter pylori infection and colorectal neoplasm risk: a meta-analysis based on East Asian population. J Cancer Res Ther 10(Suppl):263–266
Sonnenberg A, Genta RM (2013) Helicobacter pylori is a risk factor for colonic neoplasms. Am J Gastroenterol 108:208–215
Inoue I, Mukoubayashi C, Yoshimura N, Niwa T, Deguchi H, Watanabe M, Enomoto S, Maekita T, Ueda K, Iguchi M, Yanaoka K, Tamai H, Arii K, Oka M, Fujishiro M, Takeshita T, Iwane M, Mohara O, Ichinose M (2011) Elevated risk of colorectal adenoma with Helicobacter pylori-related chronic gastritis: a population-based case–control study. Int J Cancer 129:2704–2711
Nam KW, Baeg MK, Kwon JH, Cho SH, Na SJ, Choi MG (2013) Helicobacter pylori seropositivity is positively associated with colorectal neoplasms. Korean J Gastroenterol 61:259–264
Hong SN, Lee SM, Kim JH, Lee TY, Kim JH, Choe WH, Lee SY, Cheon YK, Sung IK, Park HS, Shim CS (2012) Helicobacter pylori infection increases the risk of colorectal adenomas: cross-sectional study and meta-analysis. Dig Dis Sci 57:2184–2194
Lim SH, Kwon JW, Kim N, Kim GH, Kang JM, Park MJ, Yim JY, Kim HU, Baik GH, Seo GS, Shin JE, Joo YE, Kim JS, Jung HC (2013) Prevalence and risk factors of Helicobacter pylori infection in Korea: nationwide multicenter study over 13 years. BMC Gastroenterol 13:104
Winawer SJ, Zauber AG (2002) The advanced adenoma as the primary target of screening. Gastrointest Endosc Clin N Am 12:1–9
Kim HS, Baik SJ, Kim KH, Oh CR, Lee SI (2013) Prevalence and risk factors of colorectal adenoma in 14,932 Koreans undergoing screening colonoscopy. Korean J Gastroenterol 62:104–110
Georgopoulos SD, Polymeros D, Triantafyllou K, Spiliadi C, Mentis A, Karamanolis DG, Ladas SD (2006) Hypergastrinemia is associated with increased risk of distal colon adenomas. Digestion 74:42–46
Houli N, Loh SW, Giraud AS, Baldwin GS, Shulkes A (2006) Mitogenic effects of both amidated and glycine-extended gastrin-releasing peptide in defunctioned and azoxymethane-treated rat colon in vivo. Regul Pept 134:9–16
Stewart T, Henderson R, Grayson H, Opelz G (1997) Reduced incidence of rectal cancer, compared to gastric and colonic cancer, in a population of 73,076 men and women chronically immunosuppressed. Clin Cancer Res 3:51–55
Perez-Ruiz E, Berraondo P (2016) Immunological landscape and clinical management of rectal cancer. Front Immunol 7:61
Tamas K, Walenkamp AM, de Vries EG, van Vugt MA, Beets-Tan RG, van Etten B, de Groot DJ, Hospers GA (2015) Rectal and colon cancer: not just a different anatomic site. Cancer Treat Rev 41:671–679
Abbass K, Gul W, Beck G, Markert R, Akram S (2011) Association of Helicobacter pylori infection with the development of colorectal polyps and colorectal carcinoma. South Med J 104:473–476
Bae RC, Jeon SW, Cho HJ, Jung MK, Kweon YO, Kim SK (2009) Gastric dysplasia may be an independent risk factor of an advanced colorectal neoplasm. World J Gastroenterol 15:5722–5726
Lin YL, Chiang JK, Lin SM, Tseng CE (2010) Helicobacter pylori infection concomitant with metabolic syndrome further increase risk of colorectal adenomas. World J Gastroenterol 16:3841–3846
Thorburn CM, Friedman GD, Dickinson CJ, Vogelman JH, Orentreich N, Parsonnet J (1998) Gastrin and colorectal cancer: a prospective study. Gastroenterology 115:275–280
Robertson DJ, Sandler RS, Ahnen DJ, Greenberg ER, Mott LA, Cole BF, Baron JA (2009) Gastrin, Helicobacter pylori, and colorectal adenomas. Clin Gastroenterol Hepatol 7:163–167
Selgrad M, Bornschein J, Kandulski A, Hille C, Weigt J, Roessner A, Wex T, Malfertheiner P (2014) Helicobacter pylori but not gastrin is associated with the development of colonic neoplasms. Int J Cancer 135:1127–1131
Jones M, Helliwell P, Pritchard C, Tharakan J, Mathew J (2007) Helicobacter pylori in colorectal neoplasms: is there an aetiological relationship? World J Surg Oncol 5:51
Soylu A, Ozkara S, Alis H, Dolay K, Kalayci M, Yasar N, Kumbasar AB (2008) Immunohistochemical testing for Helicobacter pylori existence in neoplasms of the colon. BMC Gastroenterol 8:35
Epplein M, Pawlita M, Michel A, Peek RM Jr, Cai Q, Blot WJ (2013) Helicobacter pylori protein-specific antibodies and risk of colorectal cancer. Cancer Epidemiol Biomarkers Prev 22:1964–1974
Shmuely H, Passaro D, Figer A, Niv Y, Pitlik S, Samra Z, Koren R, Yahav J (2001) Relationship between Helicobacter pylori CagA status and colorectal cancer. Am J Gastroenterol 96:3406–3410
Hartwich A, Konturek SJ, Pierzchalski P, Zuchowicz M, Labza H, Konturek PC, Karczewska E, Bielanski W, Marlicz K, Starzynska T, Lawniczak M, Hahn EG (2001) Helicobacter pylori infection, gastrin, cyclooxygenase-2, and apoptosis in colorectal cancer. Int J Colorectal Dis 16:202–210
Chen XZ, Schottker B, Castro FA, Chen H, Zhang Y, Holleczek B, Brenner H (2016) Association of Helicobacter pylori infection and chronic atrophic gastritis with risk of colonic, pancreatic and gastric cancer: a ten-year follow-up of the ESTHER cohort study. Oncotarget 7:17182–17193
Strofilas A, Lagoudianakis EE, Seretis C, Pappas A, Koronakis N, Keramidaris D, Koukoutsis I, Chrysikos I, Manouras I, Manouras A (2012) Association of Helicobacter pylori infection and colon cancer. J Clin Med Res 4:172–176
Inoue I, Kato J, Tamai H, Iguchi M, Maekita T, Yoshimura N, Ichinose M (2014) Helicobacter pylori-related chronic gastritis as a risk factor for colonic neoplasms. World J Gastroenterol 20:1485–1492
Rueda M, Robertson Y, Acott A, Rueda S, Keikhoff A, Guerrero W, Mancino AT (2012) Association of tobacco and alcohol use with earlier development of colorectal pathology: should screening guidelines be modified to include these risk factors? Am J Surg 204:963–967
Laiyemo AO, Doubeni C, Badurdeen DS, Murphy G, Marcus PM, Schoen RE, Lanza E, Smoot DT, Cross AJ (2012) Obesity, weight change, and risk of adenoma recurrence: a prospective trial. Endoscopy 44:813–818
Fuchs CS, Giovannucci EL, Colditz GA, Hunter DJ, Speizer FE, Willett WC (1994) A prospective study of family history and the risk of colorectal cancer. N Engl J Med 331:1669–1674
Yang MH, Rampal S, Sung J, Choi YH, Son HJ, Lee JH, Kim YH, Chang DK, Rhee PL, Rhee JC, Guallar E, Cho J (2014) The prevalence of colorectal adenomas in asymptomatic Korean men and women. Cancer Epidemiol Biomarkers Prev 23:499–507
Chlebowski RT, Wactawski-Wende J, Ritenbaugh C, Hubbell FA, Ascensao J, Rodabough RJ, Rosenberg CA, Taylor VM, Harris R, Chen C, Adams-Campbell LL, White E, Women’s Health Initiative I (2004) Estrogen plus progestin and colorectal cancer in postmenopausal women. N Engl J Med 350:991–1004
Lu Y, Ness-Jensen E, Hveem K, Martling A (2015) Metabolic predispositions and increased risk of colorectal adenocarcinoma by anatomical location: a large population-based cohort study in Norway. Am J Epidemiol 182:883–893
Fujimori S, Kishida T, Kobayashi T, Sekita Y, Seo T, Nagata K, Tatsuguchi A, Gudis K, Yokoi K, Tanaka N, Yamashita K, Tajiri T, Ohaki Y, Sakamoto C (2005) Helicobacter pylori infection increases the risk of colorectal adenoma and adenocarcinoma, especially in women. J Gastroenterol 40:887–893
Wu Q, Yang ZP, Xu P, Gao LC, Fan DM (2013) Association between Helicobacter pylori infection and the risk of colorectal neoplasia: a systematic review and meta-analysis. Colorectal Dis 15:e352–e364
Yim JY, Kim N, Choi SH, Kim YS, Cho KR, Kim SS, Seo GS, Kim HU, Baik GH, Sin CS, Cho SH, Oh BH (2007) Seroprevalence of Helicobacter pylori in South Korea. Helicobacter 12:333–340
Nam JH, Choi IJ, Kook MC, Lee JY, Cho SJ, Nam SY, Kim CG (2014) OLGA and OLGIM stage distribution according to age and Helicobacter pylori status in the Korean population. Helicobacter 19:81–89
Hahm MI, Choi KS, Park EC, Kwak MS, Lee HY, Hwang SS (2008) Personal background and cognitive factors as predictors of the intention to be screened for stomach cancer. Cancer Epidemiol Biomarkers Prev 17:2473–2479
Kim CG, Choi IJ, Lee JY, Cho SJ, Nam BH, Kook MC, Hong EK, Kim YW (2009) Biopsy site for detecting Helicobacter pylori infection in patients with gastric cancer. J Gastroenterol Hepatol 24:469–474
Acknowledgments
This study was supported in part by Grants NCC-1410250-3, NCC-1610250, and NCC-0910221 from National Cancer Center, Korea. The authors thank Jeong-Hee Lee, MS for their help in manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nam, J.H., Hong, C.W., Kim, B.C. et al. Helicobacter pylori infection is an independent risk factor for colonic adenomatous neoplasms. Cancer Causes Control 28, 107–115 (2017). https://doi.org/10.1007/s10552-016-0839-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-016-0839-x