Abstract
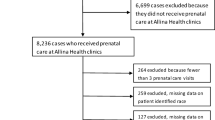
Care coordination services that link pregnant women to health-promoting resources, avoid duplication of effort, and improve communication between families and providers have been endorsed as a strategy for reducing disparities in adverse pregnancy outcomes, however empirical evidence regarding the effects of these services is contradictory and incomplete. This study investigates the effects of maternity care coordination (MCC) on pregnancy outcomes in North Carolina. Birth certificate and Medicaid claims data were analyzed for 7,124 women delivering live infants in North Carolina from October 2008 through September 2010, of whom 2,255 received MCC services. Propensity-weighted analyses were conducted to reduce the influence of selection bias in evaluating program participation. Sensitivity analyses compared these results to conventional ordinary least squares analyses. The unadjusted preterm birth rate was lower among women who received MCC services (7.0 % compared to 8.3 % among controls). Propensity-weighted analyses demonstrated that women receiving services had a 1.8 % point reduction in preterm birth risk; p < 0.05). MCC services were also associated with lower pregnancy weight gain (p = 0.10). No effects of MCC were seen for birthweight. These findings suggest that coordination of care in pregnancy can significantly reduce the risk of preterm delivery among Medicaid-enrolled women. Further research evaluating specific components of care coordination services and their effects on preterm birth risk among racial/ethnic and geographic subgroups of Medicaid enrolled mothers could inform efforts to reduce disparities in pregnancy outcome.
Similar content being viewed by others
References
US Department of Health and Human Services. Healthy People 2020 [Internet]. [cited 2013 Jan 7]. http://www.healthypeople.gov/2020/topicsobjectives2020/default.aspx.
Heisler E. J. (2012). The US infant mortality rate: International comparisons, underlying factors, and federal programs [Internet]. Congressional Research Service; [cited 2013 Jan 7]. http://www.fas.org/sgp/crs/misc/R41378.pdf.
Johnson, K., & Rosenthal, J. (2009). Improving care coordination, case management, and linkages to service for young children: Opportunities for states. Washington, DC: Commonwealth Fund.
Buescher, P. A., Roth, M. S., Williams, D., & Goforth, C. M. (1991). An evaluation of the impact of maternity care coordination on Medicaid birth outcomes in North Carolina. American Journal of Public Health, 81(12), 1625–1629.
Alexander, G. R., & Korenbrot, C. C. (1995). The role of prenatal care in preventing low birth weight. Future of Children, 5(1), 103–120.
Berry, E., Brady, C., Cunningham, S. D., et al. (2010). National healthy start initiative: A national network for effective home visitation and family support services. Washington, DC: National Healthy Start Association.
Agency for Healthcare Research and Quality. (2010). Findings on children’s health care quality and disparities. Rockville, MD. http://www.ahrq.gov/qual/nhqrdr09/nhqrdrchild09.htm.
Piper, J. M., Mitchel, E. F., & Ray, W. A. (1996). Evaluation of a program for prenatal care case management. Family Planning Perspectives, 28(2), 65–68.
Kitzman, H., Olds, D. L., Henderson, C. R., et al. (1997). Effect of prenatal and infancy home visitation by nurses on pregnancy outcomes, childhood injuries, and repeated childbearing: A randomized controlled trial. JAMA, 278(8), 644–652.
Margolis, P. A., Stevens, R., Bordley, W. C., et al. (2001). From concept to application: The impact of a community-wide intervention to improve the delivery of preventive services to children. Pediatrics, 108(3), E42.
Keeton, K., Saunders, S. E., & Koltun, D. (2004). The effect of the Family Case Management Program on 1996 birth outcomes in Illinois. Journal of Women’s Health (Larchmt), 13(2), 207–215.
Newman, R. B., Sullivan, S. A., & Menard, M. K., et al. (2008). South Carolina Partners for Preterm Birth Prevention: A regional perinatal initiative for the reduction of premature birth in a Medicaid population. American Journal of Obstetrics and Gynecology, 199(4), 393 e1–8.
Scheideberg, D. (1997). Improved perinatal outcomes with perinatal case management. Journal of Nursing Care Quality, 12(1), 36–45.
Silva, R., Thomas, M., Caetano, R., & Aragaki, C. (2006). Preventing low birth weight in Illinois: Outcomes of the family case management program. Maternal and Child Health Journal, 10(6), 481–488.
Van Dijk, J. W., Anderko, L., & Stetzer, F. (2011). The impact of prenatal care coordination on birth outcomes. Journal of Obstetric, Gynecologic, and Neonatal Nursing, 40(1), 98–108.
Mason, M. V., Poole-Yaeger, A., Lucas, B., Krueger, C. R., Ahmed, T., & Duncan, I. (2011). Effects of a pregnancy management program on birth outcomes in managed Medicaid. Managed Care, 20(4), 39–46.
Rosenbach, M., O’Neil, S., Cook, B., Trebino, L., & Walker, D. K. (2010). Characteristics, access, utilization, satisfaction, and outcomes of healthy start participants in eight sites. Maternal and Child Health Journal, 14(5):666–679.
Schulman, E. D., Sheriff, D. J., & Momany, E. T. (1997). Primary care case management and birth outcomes in the Iowa Medicaid program. American Journal of Public Health, 87(1), 80–84.
Issel, L. M. (2000). Women’s perceptions of outcomes of prenatal case management. Birth, 27(2), 120–126.
Callaghan, W. M., MacDorman, M. F., Rasmussen, S. A., Qin, C., & Lackritz, E. M. (2006). The contribution of preterm birth to infant mortality rates in the United States. Pediatrics, 118(4), 1566–1573.
Mathews, T. J., & MacDorman, M. F. (2008). Infant mortality statistics from the period linked birth/infant death data set. National Vital Statistics Reports, 60(5), 1–28.
Culhane, J. F., & Goldenberg, R. L. (2011). Racial disparities in preterm birth. Seminars in Perinatology, 35(4), 234–239.
Chu, S. Y., Callaghan, W. M., Bish, C. L., & D’Angelo, D. (2009). Gestational weight gain by body mass index among US women delivering live births, 2004–2005: Fueling future obesity. American Journal of Obstetrics and Gynecology, 200(3), 271 e1–7.
Institute of Medicine. (2009). Weight gain during pregnancy: Reexamining the guidelines. Washington, DC: National Academies Press.
North Carolina Department of Health and Human Services. (2008). North Carolina preconception health strategic plan, September 2008–September 2013 [Internet]. http://www.beforeandbeyond.org/uploads/preconception_health_strategic_plan.pdf.
Hillemeier, M. M., Farkas, G., Morgan, P. L., Martin, M. A., & Maczuga, S. A. (2009). Disparities in the prevalence of cognitive delay: How early do they appear? Paediatric and Perinatal Epidemiology, 23(3), 186–198.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hillemeier, M.M., Domino, M.E., Wells, R. et al. Effects of Maternity Care Coordination on Pregnancy Outcomes: Propensity-Weighted Analyses. Matern Child Health J 19, 121–127 (2015). https://doi.org/10.1007/s10995-014-1502-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-014-1502-3