Abstract
Purpose
To develop a live oral delivery system of Glucagon like peptide-1 (GLP-1), for the treatment of Type-2 Diabetes.
Methods
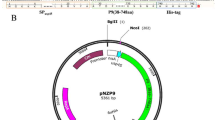
LL-pUBGLP-1, a recombinant Lactococcus lactis (L. lactis)) transformed with a plasmid vector encoding GLP-1 cDNA was constructed and was used as a delivery system. Secretion of rGLP-1 from LL-pUBGLP-1 was characterized by ELISA. The bioactivity of the rGLP-1 was examined for its insulinotropic activity on HIT-T15 cells. Transport of rGLP-1 across MDCK cell monolayer when delivered by LL-pUBGLP-1 was studied. The therapeutic effect of LL-pUBGLP-1 after oral administration was investigated in ZDF rats.
Results
DNA sequencing and ELISA confirmed the successful construction of the LL-pUBGLP-1 and secretion of the active form of rGLP-1. In vitro insulinotropic studies demonstrated that LL-pUBGLP-1 could significantly (p < 0.05) stimulate HIT-T15 cells to secrete insulin as compared to the controls. When delivered by LL-pUBGLP-1, the GLP-1 transport rate across the MDCK cell monolayer was increased by eight times (p < 0.01) as compared to the free solution form. Oral administration of LL-pUBGLP-1 in ZDF rats resulted in a significant decrease (10–20%, p < 0.05) in blood glucose levels during 2–11 h post dosing and a significant increase in insulin AUC0-11h (2.5 times, p < 0.01) as compared to the free solution.
Conclusion
The present study demonstrates that L. lactis when genetically modified with a recombinant plasmid can be used for the oral delivery of GLP-1.








Similar content being viewed by others
Abbreviations
- GLP-1:
-
Glucagon like peptide-1
- L. lactis :
-
Lactococcus lactis sub sp. lactis
- LL-pUB1000:
-
Lactococcus lactis transformed with pUB1000 plasmid
- LL-pUBGLP-1:
-
Lactococcus lactis transformed with pUBGLP-1 plasmid
- M17G:
-
M17 growth media supplemented with 5% glucose
- pUB1000:
-
Expression host plasmid vector
- pUBGLP-1:
-
Recombinant plasmid with GLP-1 c-DNA
- rGLP-1:
-
recombinant GLP-1 secreted extracellularly by LL-pUBGLP-1
- T2DM:
-
Type 2 Diabetes mellitus
References
Perfetti R, Brown TA, Velikina R, Busselen S. Control of glucose homeostasis by incretin hormones. Diabetes Technol Ther. 1999;1(3):297–305.
Kim W, Egan JM. The role of incretins in glucose homeostasis and diabetes treatment. Pharmacol Rev. 2008;60(4):470–512.
Vilsboll T. On the role of the incretin hormones GIP and GLP-1 in the pathogenesis of Type 2 diabetes mellitus. Dan Med Bull. 2004;51(4):364–70.
Elliott RM, Morgan LM, Tredger JA, Deacon S, Wright J, Marks V. Glucagon-like peptide-1 (7–36)amide and glucose-dependent insulinotropic polypeptide secretion in response to nutrient ingestion in man: acute post-prandial and 24-h secretion patterns. J Endocrinol. 1993;138(1):159–66.
Kjems LL, Holst JJ, Volund A, Madsbad S. The influence of GLP-1 on glucose-stimulated insulin secretion: effects on beta-cell sensitivity in type 2 and nondiabetic subjects. Diabetes. 2003;52(2):380–6.
Perry T, Greig NH. The glucagon-like peptides: a double-edged therapeutic sword? Trends Pharmacol Sci. 2003;24(7):377–83.
Mest HJ, Mentlein R. Dipeptidyl peptidase inhibitors as new drugs for the treatment of type 2 diabetes. Diabetologia. 2005;48(4):616–20.
Mentlein R. Dipeptidyl-peptidase IV, (CD26)–role in the inactivation of regulatory peptides. Regul Pept. 1999;85(1):9–24.
Elashoff M, Matveyenko AV, Gier B, Elashoff R, Butler PC. Pancreatitis, pancreatic, and thyroid cancer with glucagon-like peptide-1-based therapies. Gastroenterology. 2011;141(1):150–6.
Singh S, Chang HY, Richards TM, Weiner JP, Clark JM, Segal JB. Glucagonlike peptide 1-based therapies and risk of hospitalization for acute pancreatitis in type 2 diabetes mellitus: a population-based matched case–control study. JAMA Intern Med. 2013;173(7):534–9.
[01/10/2014]; Available from: http://www.fda.gov/Drugs/DrugSafety/ucm343187.htm.
Bond A. Exenatide (Byetta) as a novel treatment option for type 2 diabetes mellitus. Proc (Bayl Univ Med Cent). 2006;19(3):281–4.
Moriya H, Moriwaki C, Akimoto S, Yamaguchi K, Iwadare M. Studies on the passage of alpha-chymotrypsin across the intestine. Chem Pharm Bull (Tokyo). 1967;15(11):1662–8.
Shao J, Kaushal G. Normal flora: living vehicles for non-invasive protein drug delivery. Int J Pharm. 2004;286(1–2):117–24.
Antolin J, Ciguenza R, Saluena I, Vazquez E, Hernandez J, Espinos D. Liver abscess caused by Lactococcus lactis cremoris: a new pathogen. Scand J Infect Dis. 2004;36(6–7):490–1.
Shanahan F. Immunology. Therapeutic manipulation of gut flora. Science. 2000;289(5483):1311–2.
Buchelli-Ramirez HL, Alvarez-Alvarez C, Rojo-Alba S, Garcia-Clemente M, Cimadevilla-Suarez R, Pando-Sandoval A, et al. Necrotising pneumonia caused by Lactococcus lactis cremoris. Int J Tuberc Lung Dis. 2013;17(4):565–7.
Kaushal G, Trombetta L, Ochs RS, Shao J. Delivery of TEM beta-lactamase by gene-transformed Lactococcus lactis subsp. lactis through cervical cell monolayer. Int J Pharm. 2006;313(1–2):29–35.
Piard JC, Hautefort I, Fischetti VA, Ehrlich SD, Fons M, Gruss A. Cell wall anchoring of the Streptococcus pyogenes M6 protein in various lactic acid bacteria. J Bacteriol. 1997;179(9):3068–72.
Savijoki K, Kahala M, Palva A. High level heterologous protein production in Lactococcus and Lactobacillus using a new secretion system based on the Lactobacillus brevis S-layer signals. Gene. 1997;186(2):255–62.
Le Loir Y, Nouaille S, Commissaire J, Bretigny L, Gruss A, Langella P. Signal peptide and propeptide optimization for heterologous protein secretion in Lactococcus lactis. Appl Environ Microbiol. 2001;67(9):4119–27.
Brashears MM, Galyean ML, Loneragan GH, Mann JE, Killinger-Mann K. Prevalence of Escherichia coli O157:H7 and performance by beef feedlot cattle given Lactobacillus direct-fed microbials. J Food Prot. 2003;66(5):748–54.
Brashears MM, Jaroni D, Trimble J. Isolation, selection, and characterization of lactic acid bacteria for a competitive exclusion product to reduce shedding of Escherichia coli O157:H7 in cattle. J Food Prot. 2003;66(3):355–63.
Tannock GW. Probiotic properties of lactic-acid bacteria: plenty of scope for fundamental R & D. Trends Biotechnol. 1997;15(7):270–4.
Gilbert C, Atlan D, Blanc B, Portailer R, Germond JE, Lapierre L, et al. A new cell surface proteinase: sequencing and analysis of the prtB gene from Lactobacillus delbruekii subsp. bulgaricus. J Bacteriol. 1996;178(11):3059–65.
Grangette C, Muller-Alouf H, Goudercourt D, Geoffroy MC, Turneer M, Mercenier A. Mucosal immune responses and protection against tetanus toxin after intranasal immunization with recombinant Lactobacillus plantarum. Infect Immun. 2001;69(3):1547–53.
Scheppler L, Vogel M, Marti P, Muller L, Miescher SM, Stadler BM. Intranasal immunisation using recombinant Lactobacillus johnsonii as a new strategy to prevent allergic disease. Vaccine. 2005;23(9):1126–34.
Scheppler L, Vogel M, Zuercher AW, Zuercher M, Germond JE, Miescher SM, et al. Recombinant Lactobacillus johnsonii as a mucosal vaccine delivery vehicle. Vaccine. 2002;20(23–24):2913–20.
Shaw DM, Gaerthe B, Leer RJ, Van Der Stap JG, Smittenaar C, Heijne Den Bak-Glashouwer M, et al. Engineering the microflora to vaccinate the mucosa: serum immunoglobulin G responses and activated draining cervical lymph nodes following mucosal application of tetanus toxin fragment C-expressing lactobacilli. Immunology. 2000;100(4):510–8.
Zegers ND, Kluter E, van Der Stap H, van Dura E, van Dalen P, Shaw M, et al. Expression of the protective antigen of Bacillus anthracis by Lactobacillus casei: towards the development of an oral vaccine against anthrax. J Appl Microbiol. 1999;87(2):309–14.
Steidler L, Neirynck S, Huyghebaert N, Snoeck V, Vermeire A, Goddeeris B, et al. Biological containment of genetically modified Lactococcus lactis for intestinal delivery of human interleukin 10. Nat Biotechnol. 2003;21(7):785–9.
Steidler L, Hans W, Schotte L, Neirynck S, Obermeier F, Falk W, et al. Treatment of murine colitis by Lactococcus lactis secreting interleukin-10. Science. 2000;289(5483):1352–5.
Steidler L, Robinson K, Chamberlain L, Schofield KM, Remaut E, Le Page RW, et al. Mucosal delivery of murine interleukin-2 (IL-2) and IL-6 by recombinant strains of Lactococcus lactis coexpressing antigen and cytokine. Infect Immun. 1998;66(7):3183–9.
Steidler L, Wells JM, Raeymaekers A, Vandekerckhove J, Fiers W, Remaut E. Secretion of biologically active murine interleukin-2 by Lactococcus lactis subsp. lactis. Appl Environ Microbiol. 1995;61(4):1627–9.
Avall-Jaaskelainen S, Palva A. Secretion of biologically active porcine interleukin-2 by Lactococcus lactis. Vet Microbiol. 2006;115(1–3):278–83.
Fernandez A, Horn N, Wegmann U, Nicoletti C, Gasson MJ, Narbad A. Enhanced secretion of biologically active murine interleukin-12 by Lactococcus lactis. Appl Environ Microbiol. 2009;75(3):869–71.
Klijn N, Weerkamp AH, de Vos WM. Genetic marking of Lactococcus lactis shows its survival in the human gastrointestinal tract. Appl Environ Microbiol. 1995;61(7):2771–4.
Kaushal G, Shao J. Oral delivery of beta-lactamase by Lactococcus lactis subsp. lactis transformed with Plasmid ss80. Int J Pharm. 2006;312(1–2):90–5.
Jakubovics NS, Stromberg N, van Dolleweerd CJ, Kelly CG, Jenkinson HF. Differential binding specificities of oral streptococcal antigen I/II family adhesins for human or bacterial ligands. Mol Microbiol. 2005;55(5):1591–605.
Wells JM, Wilson PW, Le Page RW. Improved cloning vectors and transformation procedure for Lactococcus lactis. J Appl Bacteriol. 1993;74(6):629–36.
Mukherjee T, Squillantea E, Gillespieb M, Shao J. Transepithelial electrical resistance is not a reliable measurement of the Caco-2 monolayer integrity in Transwell. Drug Deliv. 2004;11(1):11–8.
Cogburn JN, Donovan MG, Schasteen CS. A model of human small intestinal absorptive cells. 1. Transport barrier. Pharm Res. 1991;8(2):210–6.
Wells JM, Mercenier A. Mucosal delivery of therapeutic and prophylactic molecules using lactic acid bacteria. Nat Rev Microbiol. 2008;6(5):349–62.
Irvine JD, Takahashi L, Lockhart K, Cheong J, Tolan JW, Selick HE, et al. MDCK (Madin-Darby canine kidney) cells: a tool for membrane permeability screening. J Pharm Sci. 1999;88(1):28–33.
Prego C, Torres D, Alonso MJ. The potential of chitosan for the oral administration of peptides. Expert Opin Drug Deliv. 2005;2(5):843–54.
Kompella UB, Lee VH. Delivery systems for penetration enhancement of peptide and protein drugs: design considerations. Adv Drug Deliv Rev. 2001;46(1–3):211–45.
Gomez-Orellana I. Strategies to improve oral drug bioavailability. Expert Opin Drug Deliv. 2005;2(3):419–33.
ACKNOWLEDGMENTS AND DISCLOSURES
We would like to thank Dr. H. F. Jenkinson and Dr. J. Brittan (Department of Oral and Dental Science, University of Bristol, Bristol, UK) for providing us with the L. lactis strain with pUB1000 plasmid and also for their valuable assistance. The animal work was supported by the Seed grant/Venture Capital Fund from St. John’s University, NY.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Agarwal, P., Khatri, P., Billack, B. et al. Oral Delivery of Glucagon Like Peptide-1 by a Recombinant Lactococcus lactis . Pharm Res 31, 3404–3414 (2014). https://doi.org/10.1007/s11095-014-1430-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-014-1430-3