Abstract
Objective
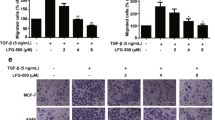
To examine the effect of brucine on the migration, invasion, adhesion and expressions of epithelial-to-mesenchymal transition (EMT) markers and matrix metalloproteinases (MMPs) in the highly metastatic breast cancer cell lines MDA-MB-231 and Hs578-T.
Methods
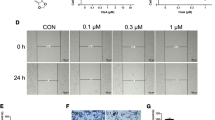
MDA-MB-231 and Hs578-T cells were divided to 4 groups: the control group (0.1% DMSO), and 25, 50 and 100 μmol/L brucine groups. The cell viability was determined using a CellTiter-Glo® luminescent cell viability. The scratch wound healing assay and tanswell migration assay were used to determine the migration ability of these cells treated by different concentrations of brucine. The proliferation rate, invasive potential and adhesive ability were respectively performed by colony formation assay, transwell invasion assay and adhension assay. The protein and mRNA expressions of EMT biomarkers, MMP-2 and MMP-9 were investigated by real-time reverse transcription polymerase chain reaction and Western blot.
Results
Compared with the control group, brucine had little effect on cell viability or proliferation (P>0.05), but led to a dose-dependent decrease on migration, invasion, adhension of MDA-MB-231 and Hs578-T cells (P<0.01). Furthermore, brucine increased the protein and mRNA levels of EMT markers such as E-cadherin and β-catenin in MDA-MB-231 and Hs578-T cells, and decreased the protein and mRNA levels of mesenychmal markers such as vimentin and fibronectin, as well as the expressions of MMP-2 and MMP-9 (all P<0.01).
Conclusion
Brucine inhibited triple negative breast cancer cells metastasis potentially through EMT reversion and MMP-2 and MMP-9 inhibition.
Similar content being viewed by others
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin 2011;61:69–90.
Come C, Laine A, Chanrion M, Edgren H, Mattila E, Liu X, et al. CIP2A is associated with human breast cancer aggressivity. Clin Cancer Res 2009;15:5092–5100.
Al Dhaheri Y, Attoub S, Arafat K, AbuQamar S, Viallet J, Saleh A, et al. Anti-metastatic and anti-tumor growth effects of Origanum majorana on highly metastatic human breast cancer cells: inhibition of NFκB signaling and reduction of nitric oxide production. PLoS One 2013;8:e68808.
Kalluri R, Weinberg RA. The basics of epithelialmesenchymal transition. J Clin Invest 2009;119:1420–1428.
Agrawal SS, Saraswati S, Mathur R, Pandey M. Cytotoxic and antitumor effects of brucine on Ehrlich ascites tumor and human cancer cell line. Life Sci 2011;89:147–158.
Bisset NG, Phillipson JD. The tertiary alkaloids of some Asian species of strychnos. J Pharm Pharmacol 1971;23:244S.
Guizhi M. The long period clinical observation of the effect of Strychnos nux-vomica on Kaschin-Beck's disease. Chi J Reg Dis Prev Ther 1996;11:120–124.
Yin W, Wang TS, Yin FZ, Cai BC. Analgesic and antiinflammatory properties of brucine and brucine N-oxide extracted from seeds of Strychnox nux-vomica. J Ethnopharmacol 2003;88:205–214.
Tripathi YB, Chaurasia S. Interaction of Strychnos nux-vomica products and iron: with reference to lipid peroxidation. Phytomedicine 2000;7:523–528.
Cai BC, Wang TS, Kurokawa M, Shiraki K, Hattori M. Cytotoxicities of alkaloids from processed and unprocessed seeds of Strychnos nux-vomica L. Acta Pharmacol Sin 1998;19:425–428.
Deng XK, Yin W, Li WD, Yin FZ, Lu XY, Zang XC, et al. The anti-tumor effects of alkaloids from the seeds of Strychnos nux-vomica on HepG2 cells and its possible mechanism. J Ethnopharmacol 2006;106:179–186.
Yin W, Deng XK, Yin FZ, Zhang XC, Cai BC, et al. The cytotoxicity induced by Strychnos nux-vomica proceeds via apoptosis by Cox 2 and caspase-3 in SMMC 7221 cells. Food Chem Toxicol 2007;45:1700–1708.
Rao PS, Ramanadham M, Prasad MNV. Anti-proliferative and cytotoxic effects of Strychnos nux-vomica root extract on human multiple myeloma cell line-RPMI 8226. Food Chem Toxicol 2009;47:283–288.
Shu GW, Mi X, Cai J, Zhang XL, Yin W, Yang XZ, et al. Brucine, an alkaloid from seeds of Strychnos nux-vomica Linn., represses hepatocellular carcinoma cell migration and metastasis: the role of hypoxia inducible factor 1 pathway. Toxicol Lett 2013;222: 91–101.
Saraswati S, Agrawal SS. Brucine, an indole alkaloid from Strychnos nux-vomica attenuates VEGF-induced angiogenesis via inhibiting VEGFR2 signaling pathway in vitro and in vivo. Cancer Letters 2013;332:83–93.
Li P, Zhang M, Ma WJ, Sun X, Jin FP. Effects of brucine on vascular endothelial growth factor expression and microvessel density in a nude mouse model of bone metastasis due to breast cancer. Chin J Integr Med 2012;18:605–609.
Zheng GY, Xin HL, Li B, Xu YF, Yi TJ, Ling CQ. Total saponin from root of Actinidia Valvata Dunn prevents the metastasis of human hepatocellular carcinoma cells. Chin J Integr Med 2012;18:197–202.
Gunasinghe NP, Wells A, Thompson EW, Hugo HJ. Mesenchymal-epithelial transition (MET) as a mechanism for metastatic colonisation in breast cancer. Cancer Metastasis Rev 2012;31:469–478.
Li HR, Li XR. Feasibility for inhibiting tumor metastasis with Chinese herbal medicines as angiogenesis inhibitors. J Chin Integr Med 2007;5:378–382.
Wang F, Pan LQ. Tumor micrometastasis and its treatment with traditional Chinese medicine. J Chin Integr Med 2003;1:171–172,204.
Chaffer CL, Weinberg RA. A perspective on cancer cell metastasis. Science 2011;33:1559–1564.
Qin JM, Yin PH, Li Q, Sa ZQ, Sheng X, Yang L, et al. Anti-tumor effects of brucine immuno-nanoparticles on hepatocellular carcinoma. Int J Nanomed 2012;7:369–379.
Zheng L, Wang XL, Luo WJ, Zhan YZ, Zhang YM. Brucine, an effective natural compound derived from nux-vomica, induces G1 phase arrest and apoptosis in LoVo cells. Food Chem Toxicol 2013;58:332–339.
Ma YP, Zhao JP, Wang YH,Li ZH, Feng J, Ren H. Effects of brucine on bone metabolism in multiple myeloma. Molecul Med Reports 2012;6:367–370.
Thiery JP. Epithelial-mesenchymal transitions in tumour progression. Nat Rev Cancer 2002;6:442–454.
Singh A, Settleman J. EMT, cancer stem cells and drug resistance: an emerging axis of evil in the war on cancer. Oncogene 2010;34:4741–4751.
Raimondi C, Gianni W, Cortesi E, Gazzaniga P. Cancer stem cells and epithelial-mesenchymal transition: revisiting minimal residual disease. Curr Cancer Drug Targets 2010;5:496–508.
Roxanis I. Occurrence and significance of epithelial mesenchymal transition in breast cancer. J Clin Pathol 2013;6:517–521.
Takebe N, Warren RQ, Ivy SP. Breast cancer growth and metastasis: interplay between cancer stem cells, embryonic signaling pathways and epithelial-to-mesenchymal transition. Breast Cancer Res 2011;3:1–11.
Hardy KM, Booth BW, Hendrix MJ, Salomon DS, Strizzi L. ErbB/EGF signaling and EMT in mammary development and breast cancer. J Mammary Gland Biol Neoplasia 2010;2:191–199.
Taylor MA, Parvani JG, Schiemann WP. The pathophysiology of epithelial-mesenchymal transition induced by transforming growth factor-beta in normal and malignant mammary epithelial cells. J Mammary Gland Biol Neoplasia 2010;2:169–190.
García-Olmo DC, Picazo MG, García-Olmo D. Transformation of non-tumor host cells during tumor progression: theories and evidence. Expert Opin Biol Ther 2012;12(Suppl 1):S199–S207.
Deakin NE, Chaplain MA. Mathematical modeling of cancer invasion: the role of membrane-bound matrix metalloproteinases. Front Oncol 2013;3:70.
Escaff S, Fernández JM, González LO, Suárez A, González-Reyes S, González JM, et al. Study of matrix metalloproteinases and their inhibitors in prostate cancer. Br J Cancer 2010;102:922–929.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the State Administration of Traditional Chinese Medicine of China (2009-No.30)
Rights and permissions
About this article
Cite this article
Li, M., Li, P., Zhang, M. et al. Brucine suppresses breast cancer metastasis via inhibiting epithelial mesenchymal transition and matrix metalloproteinases expressions. Chin. J. Integr. Med. 24, 40–46 (2018). https://doi.org/10.1007/s11655-017-2805-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-017-2805-1