Abstract
Summary
The aim of the present study was to identify patient factors associated with higher costs in hip fracture patients. The mean costs of a prospectively observed sample of 402 patients were 8853 €. The ASA score, Charlson comorbidity index, and fracture location were associated with increased costs.
Purpose
Fractures of the proximal end of the femur (hip fractures) are of increasing incidence due to demographic changes. Relevant co-morbidities often present in these patients cause high complication rates and prolonged hospital stays, thus leading to high costs of acute care. The aim of this study was to perform a precise cost analysis of the actual hospital costs of hip fractures and to identify patient factors associated with increased costs.
Methods
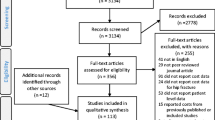
The basis of this analysis was a prospectively observed single-center trial, which included 402 patients with fractures of the proximal end of the femur. All potential cost factors were recorded as accurately as possible for each of the 402 patients individually, and statistical analysis was performed to identify associations between pre-existing patient factors and acute care costs.
Results
The mean total acute care costs per patient were 8853 ± 5676 € with ward costs (5828 ± 4294 €) and costs for surgical treatment (1972 ± 956 €) representing the major cost factors. The ASA score, Charlson comorbidity index, and fracture location were identified as influencing the costs of acute care for hip fracture treatment.
Conclusion
Hip fractures are associated with high acute care costs. This study underlines the necessity of sophisticated risk-adjusted payment models based on specific patient factors. Economic aspects should be an integral part of future hip fracture research due to limited health care resources.

Similar content being viewed by others
References
Marks R (2010) Hip fracture epidemiological trends, outcomes, and risk factors, 1970-2009. Int J Gen Med 3:1–17
Icks A, Haastert B, Wildner M, Becker C, Meyer G (2008) Trend of hip fracture incidence in Germany 1995-2004: a population-based study. Osteoporos Int 19:1139–1145
White SM, Griffiths R (2011) Projected incidence of proximal femoral fracture in England: a report from the NHS Hip Fracture Anaesthesia Network (HIPFAN). Injury 42:1230–1233
Kanis JA, Odén A, McCloskey EV, Johansson H, Wahl DA, Cooper C, Life IWGoEaQo (2012) A systematic review of hip fracture incidence and probability of fracture worldwide. Osteoporos Int 23:2239–2256
Dolan P, Torgerson DJ (1998) The cost of treating osteoporotic fractures in the United Kingdom female population. Osteoporos Int 8:611–617
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A (2007) Incidence and economic burden of osteoporosis-related fractures in the United States, 2005-2025. J Bone Miner Res 22:465–475
Ström O, Borgström F, Kanis JA, Compston J, Cooper C, McCloskey EV, Jönsson B (2011) Osteoporosis: burden, health care provision and opportunities in the EU: a report prepared in collaboration with the International Osteoporosis Foundation (IOF) and the European Federation of Pharmaceutical Industry Associations (EFPIA). Arch Osteoporos 6:59–155
Singer A, Exuzides A, Spangler L, O’Malley C, Colby C, Johnston K, Agodoa I, Baker J, Kagan R (2015) Burden of illness for osteoporotic fractures compared with other serious diseases among postmenopausal women in the United States. Mayo Clin Proc 90:53–62
Braithwaite RS, Col NF, Wong JB (2003) Estimating hip fracture morbidity, mortality and costs. J Am Geriatr Soc 51:364–370
Sahota O, Morgan N, Moran CG (2012) The direct cost of acute hip fracture care in care home residents in the UK. Osteoporos Int 23:917–920
Buecking B, Struewer J, Waldermann A, Horstmann K, Schubert N, Balzer-Geldsetzer M, Dodel R, Bohl K, Ruchholtz S, Bliemel C (2014) What determines health-related quality of life in hip fracture patients at the end of acute care?—a prospective observational study. Osteoporos Int 25:475–484
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Anaestesiologists ASo (2015) American Society of Anesthesiologists. ASA physical status classification system. Accessed Accessed: 18 February 2015
Sheikh JI, Yesavage, J.A. (1986) Geriatric Depression Scale (GDS). Recent evidence and development of a shorter version. In (Ed.) TLB (ed) Clinical gerontology: a guide to assessment and intervention. The Haworth Press, NY, pp 165–173.
Almeida OP, Almeida SA (1999) Short versions of the geriatric depression scale: a study of their validity for the diagnosis of a major depressive episode according to ICD-10 and DSM-IV. Int J Geriatr Psychiatry 14:858–865
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
(AWMF) AWMF (2009) S3-guideline “dementia”, long version. Accessed 5 October 2015
Dunn G, Mirandola M, Amaddeo F, Tansella M (2003) Describing, explaining or predicting mental health care costs: a guide to regression models. Methodological review. Br J Psychiatry 183:398–404
Rolfson O, Ström O, Kärrholm J, Malchau H, Garellick G (2012) Costs related to hip disease in patients eligible for total hip arthroplasty. J Arthroplast 27:1261–1266
Nikkel LE, Fox EJ, Black KP, Davis C, Andersen L, Hollenbeak CS (2012) Impact of comorbidities on hospitalization costs following hip fracture. J Bone Joint Surg Am 94:9–17
Wong MK, Arjandas CLK, Lim SL, Lo NN (2002) Osteoporotic hip fractures in Singapore—costs and patient’s outcome. Ann Acad Med Singap 31:3–7
Lawrence TM, White CT, Wenn R, Moran CG (2005) The current hospital costs of treating hip fractures. Injury 36:88–91 discussion 92
Kammerlander C, Roth T, Friedman SM, Suhm N, Luger TJ, Kammerlander-Knauer U, Krappinger D, Blauth M (2010) Ortho-geriatric service—a literature review comparing different models. Osteoporos Int 21:S637–S646
Garcia AE, Bonnaig JV, Yoneda ZT, Richards JE, Ehrenfeld JM, Obremskey WT, Jahangir AA, Sethi MK (2012) Patient variables which may predict length of stay and hospital costs in elderly patients with hip fracture. J Orthop Trauma 26:620–623
Leal J, Gray AM, Prieto-Alhambra D, Arden NK, Cooper C, Javaid MK, Judge A, group Rs (2015) Impact of hip fracture on hospital care costs: a population-based study. Osteoporos Int
Kirkland LL, Kashiwagi DT, Burton MC, Cha S, Varkey P (2011) The Charlson comorbidity index score as a predictor of 30-day mortality after hip fracture surgery. Am J Med Qual 26:461–467
Souza RC, Pinheiro RS, Coeli CM, Camargo KR Jr (2008) The Charlson comorbidity index (CCI) for adjustment of hip fracture mortality in the elderly: analysis of the importance of recording secondary diagnoses. Cad Saude Publica 24:315–322
Neuhaus V, King J, Hageman MG, Ring DC (2013) Charlson comorbidity indices and in-hospital deaths in patients with hip fractures. Clin Orthop Relat Res 471:1712–1719
Johnson DJ, Greenberg SE, Sathiyakumar V, Thakore R, Ehrenfeld JM, Obremskey WT, Sethi MK (2015) Relationship between the Charlson comorbidity index and cost of treating hip fractures: implications for bundled payment. J Orthop Traumatol 16:209–213
Chen LT, Lee JA, Chua BS, Howe TS (2007) Hip fractures in the elderly: the impact of comorbid illnesses on hospitalisation costs. Ann Acad Med Singap 36:784–787
Thakore RV, Lee YM, Sathiyakumar V, Obremskey WT, Sethi MK (2014) Geriatric hip fractures and inpatient services: predicting hospital charges using the ASA score. Curr Gerontol Geriatr Res 2014:923717
Acknowledgments
The authors want to thank Gerhard Bodenbender for his valuable contribution to the acquisition of data. We also wish to acknowledge Monika Balzer-Geldsetzer and Richard Dodel for their assistance in planning the study design.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Electronic supplementary material
ESM 1
(DOCX 21 kb)
Rights and permissions
About this article
Cite this article
Aigner, R., Meier Fedeler, T., Eschbach, D. et al. Patient factors associated with increased acute care costs of hip fractures: a detailed analysis of 402 patients. Arch Osteoporos 11, 38 (2016). https://doi.org/10.1007/s11657-016-0291-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-016-0291-2