Abstract
Background
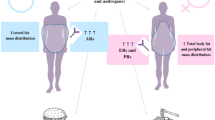
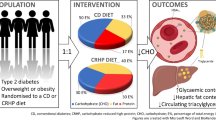
To assess the relationship of body composition measures and basal metabolic rate (BMR) with gastrointestinal hormones in weight regain 5 years after gastric bypass.
Methods
A total of 42 patients were divided into two groups: with and without weight regain 5 years after gastric bypass. Hormone assessments were performed after a fasting period and at 30, 60, and 120 min after the standard meal intake.
Results
Patients with no weight regain had significantly lower visceral fat (VF), lower fat body mass (FBM), and lower fat percentage (%F) in relation to the other group. In the group without weight regain, at baseline, glucose-dependent insulinotropic polypeptide (GIP) showed a negative correlation with weight and BMI and a positive correlation with BMR, skeletal muscle mass (SMM), and fat-free mass (FFM). After the standard meal, the following results were found: a negative correlation with %F, a positive correlation of glucagon-like peptide-1 (GLP-1) with FFM, and a positive correlation of GLP-2 and PYY with BMR, SMM, and FFM. In the group with weight regain, at baseline, GIP, PYY, and GLP-1 showed a negative correlation with %F. After the standard meal, PYY and GLP-1 showed a negative correlation with VF, FBM, and %F. On the other hand, GLP-2 negatively correlated with VF and FBM.
Conclusion
It is possible to conclude that there is a different relationship of concentrations of PYY, GIP, GLP-1, and GLP-2 with body composition and BMR in patients with and without weight regain in the late gastric bypass postoperative period.




Similar content being viewed by others
References
Karmali S, Brar B, Shi X, et al. Weight recidivism post-bariatric surgery: a systematic review. Obes Surg. 2013;23(11):1922–33.
Tran DD, Nwokeabia ID, Purnell S, et al. Revision of Roux-en-Y gastric bypass for weight regain: a systematic review of techniques and outcomes. Obes Surg. 2016;26(7):1627–34.
Sheppard CE, Lester EL, Chuck AW, et al. The economic impact of weight regain. Gastroenterol Res Pract. 2013;2013:379564. Review
Kanerva N, Larsson I, Peltonen M, et al. Changes in total energy intake and macronutrient composition after bariatric surgery predict long-term weight outcome: findings from the Swedish obese subjects (SOS) study. Am J Clin Nutr. 2017;106(1):136–45.
Magro DO, Geloneze B, Delfini R, et al. Long-term weight regain after gastric by-pass: a 5-year prospective study. Obes Surg. 2008;18(6):648–51.
Hopkins M, Finlayson G, Duarte C, et al. Modelling the associations between fat-free mass, resting metabolic rate and energy intake in the context of total energy balance. Int J Obes. 2016;40(2):312–8.
Hopkins M, Blundell JE. Energy balance, body composition, sedentariness and appetite regulation: pathways to obesity. Clin Sci (Lond). 2016;130(18):1615–28.
Svane MS, Jørgensen NB, Bojsen-Møller KN, et al. Peptide YY and glucagon-like peptide-1 contribute to decreased food intake after Roux-en-Y gastric bypass surgery. Int J Obes. 2016;40(11):1699–706.
Malin SK, Kashyap SR. Effects of various gastrointestinal procedures on β-cell function in obesity and type 2 diabetes. Surg Obes Relat Dis. 2016;12(6):1213–9.
Holst JJ, Gribble F, Horowitz M, et al. Roles of the gut in glucose homeostasis. Diabetes Care. 2016;39(6):884–92.
Reinhold RB. Critical analysis of long term weight loss following gastric bypass. Surg Gynecol Obstet. 1982;155:385–94.
Larrad A, Sanchez-Cabezudo C. Indicadores de calidad en cirurgia bariátrica y critérios de êxito a largo plazo. Cir Esp. 2004;75(3):301–4.
Christou NV, Look D, Maclean L. Weight gain after short and long-limb gastric bypass in patients followed for longer than 10 years. Ann Surg. 2006;244:734–40.
Gumbs AA, Pomp A, Gagner M. Revisional bariatric surgery for inadequate weight loss. Obes Surg. 2007;17(9):1137–45.
Deitel M. Overweight and obesity worldwide now estimated to involve 1.7 billion people. Obes Surg. 2003;13:329–30.
Lauti M, Lemanu D, Zeng ISL, et al. Definition determines weight regain outcomes after sleeve gastrectomy. Surg Obes Relat Dis. 2017;13(7):1123–9.
Le Roux CW, Welbourn R, Werling M, et al. Gut hormones as mediators of appetite and weight loss after Roux-en-Y gastric bypass. Ann Surg. 2007;246(5):780–5.
Carrasco F, Papapietro K, Csendes A, et al. Changes in resting energy expenditure and body composition after weight loss following Roux-en-Y gastric bypass. Obes Surg. 2007;17:608–16.
Faria SL, Faria OP, Buffington C, et al. Energy expenditure before and after Roux-en-Y gastric bypass. Obes Surg. 2012;22(9):1450–5.
Ravussin E, Lillioja S, Anderson TE, et al. Determinants of 24-hour energy expenditure in man. Methods and results using a metabolic chamber. J Clin Invest. 1986;78(6):1568–78.
Rubino F, Gagner M, Gentileschi P, et al. The early effect of the Roux-en-Y gastric bypass on hormones involved in body weight regulation and glucose metabolism. Ann Surg. 2004;240:236–42.
DePaula AL, Macedo AL, Schraibman V, et al. Hormonal evaluation following laparoscopic treatment of type 2 diabetes mellitus patients with BMI 20–34. Surg Endosc. 2009;23(8):1724–32.
Bergmann NC, Lund A, Gasbjerg LS, et al. Separate and combined effects of GIP and GLP-1 infusions on bone metabolism in overweight men without diabetes. J Clin Endocrinol Metab. 2019;104(7):2953–60.
Deacon CF, Nauck MA, Meier J, et al. Degradation of endogenous and exogenous gastric inhibitory polypeptide in healthy and in type 2 diabetic subjects as revealed using a new assay for the intact peptide. J Clin Endocrinol Metab. 2000;85(10):3575–81.
Le Roux CW, Borg C, Wallis K, et al. Gut hypertrophy after gastric by-pass is associated with increased glucagon-like peptide 2 and intestinal crypt cell proliferation. Ann Surg. 2010;252(1):50–6.
Vidal J, de Hollanda A, Jiménez A. GLP-1 is not the key mediator of the health benefits of metabolic surgery. Surg Obes Relat Dis. 2016;
Santo MA, Riccioppo D, Pajecki D, et al. Weight regain after gastric bypass: influence of gut hormones. Obes Surg. 2016;26(5):919–25.
Cazzo E, Gestic MA, Utrini MP, et al. Correlation between pre and postoperative levels of GLP-1/GLP-2 and weight loss after Roux-en-Y gastric bypass: a prospective study. Arq Bras Cir Dig. 2016;29(4):257–9.
Vincent RP, Ashrafian H, Le Roux C. Mechanisms of disease: the role of gastrointestinal hormones in appetite and obesity. Nat Clin Pract Gastroenterol Hepatol. 2008;5(5):268–77.
Browning MG, Rabl C, Campos GM. Blunting of adaptive thermogenesis as a potential additional mechanism to promote weight loss after gastric bypass. Surg Obes Relat Dis. 2017;13(4):669–73.
Meguid MM, Glade MJ, Middleton FA. Weight regain after Roux-en-Y: a significant complication related to PYY. Nutrition. 2008;24(9):832–42.
Le Roux CW, Batterham RL, Aylwin SJ, et al. Attenuated peptide YY release in obese subjects is associated with reduced satiety. Endocrinology. 2006;147(1):3–8.
Taqi E, Wallace LE, de Heuvel E, et al. The influence of nutrients, biliary-pancreatic secretions, and systemic trophic hormones on intestinal adaptation in a Roux-en-Y bypass model. J Pediatr Surg. 2010;45(5):987–95.
Le Roux CW, Aylwin SJ, Batterham RL, et al. Gut hormone profiles following bariatric surgery favor an anorectic state, facilitate weight loss, and improve metabolic parameters. Ann Surg. 2006;243(1):108–14.
Jacobsen SH, Olesen SC, Dirksen C, et al. Changes in gastrointestinal hormone responses, insulin sensitivity, and beta-cell function within 2 weeks after gastric bypass in non-diabetic subjects. Obes Surg. 2012;22(7):1084–96.
DeHollanda A, Jiménez A, Corcelles R, et al. Gastrointestinal hormones and weight loss response after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2014;10(5):814–9.
Cazzo E, Gestic MA, Utrini MP, et al. GLP-2: a poorly understood mediator enrolled in various bariatric/metabolic surgery-related pathophysiologic mechanisms. Arq Bras Cir Dig. 2016;29(4):272–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pereira, S., Saboya, C. & Ramalho, A. Relationship of Body Composition Measures and Metabolic Basal Rate with Gastrointestinal Hormones in Weight Regain 5 Years After Gastric Bypass. OBES SURG 30, 1536–1543 (2020). https://doi.org/10.1007/s11695-019-04342-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-04342-0