Abstract
Background
Unmasking the residual cardiovascular risk is a major research challenge in the attempt to reduce cardiovascular disease (CVD) morbidity and mortality. Mounting evidence suggests that a high circulating level of trimethylamine N-oxide is a new potential CVD risk factor. We performed a systematic review of the published studies to clarify the association between circulating high levels of TMAO and cardiovascular events.
Methods
Studies evaluating the association between TMAO and CVD events were searched by electronic databases up to December 2018. Pooled results were expressed as risk ratio (RR) with 95% pertinent confidence interval (CI).
Results
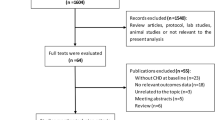
Three studies for a total of 923 patients at high/very high CVD risk were included in our analysis. Overall, a high TMAO level was associated with both major adverse cardiovascular events (RR = 2.05; 95% CI 1.61–2.61) and all-cause mortality (RR = 3.42; 95% CI 2.27–5.15).
Conclusions
Our findings support a role of high TMAO levels in predicting CVD events. High levels of TMAO may be a new CVD risk factor, potentially useful to better plan personalized CVD prevention strategies.


Similar content being viewed by others
References
De Carlo M, Mazzolai L, Bossone E, Brodmann M, Micari A, Muiesan ML et al (2017) Eur Heart J 38:1028–1033
Ridker PM, Danielson E, Fonseca FA, Genest J, Gotto AM Jr, Kastelein JJ et al (2008) Rosuvastatin to prevent vascular events in men and women with elevated C-reactive protein. N Engl J Med 359:2195–2207
Libby P (2005) The forgotten majority: unfinished business in cardiovascular risk reduction. J Am Coll Cardiol 46:1225–1228
Wang Z, Klipfell E, Bennett BJ, Koeth R, Levison BS, Dugar B et al (2011) Gut flora metabolism of phosphatidylcholine promotes cardiovascular disease. Nature 472:57–63
van Mens TE, Büller HR, Nieuwdorp M (2019) Targeted inhibition of gut microbiota proteins involved in TMAO production to reduce platelet aggregation and arterial thrombosis: a blueprint for drugging the microbiota in the treatment of cardiometabolic disease? J Thromb Haemost 17:3–5
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 62:1006–1012
Kip KE, Hollabaugh K, Marroquin OC, Williams DO (2008) The problem with composite end points in cardiovascular studies: the story of major adverse cardiac events and percutaneous coronary intervention. J Am Coll Cardiol 51:701–707
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Stubbs JR, House JA, Ocque AJ, Zhang S, Johnson C, Kimber C et al (2016) Serum trimethylamine-N-oxide is elevated in CKD and correlates with coronary atherosclerosis burden. J Am Soc Nephrol 27:305–313
Kaysen GA, Johansen KL, Chertow GM, Dalrymple LS, Kornak J, Grimes B et al (2015) Associations of trimethylamine N-oxide with nutritional and inflammatory biomarkers and cardiovascular outcomes in patients new to dialysis. J Ren Nutr 25:351–356
Missailidis C, Hällqvist J, Qureshi AR, Barany P, Heimbürger O, Lindholm B et al (2016) Serum trimethylamine-N-oxide is strongly related to renal function and predicts outcome in chronic kidney disease. PLoS ONE 11:e0141738
Kim RB, Morse BL, Djurdjev O, Tang M, Muirhead N, Barrett B et al (2016) Advanced chronic kidney disease populations have elevated trimethylamine N-oxide levels associated with increased cardiovascular events. Kidney Int 89:1144–1152
Robinson-Cohen C, Newitt R, Shen DD, Rettie AE, Kestenbaum BR, Himmelfarb J et al (2016) Association of FMO3 variants and trimethylamine N-oxide concentration, disease progression, and mortality in CKD patients. PLoS ONE 11:e0161074
Ottiger M, Nickler M, Steuer C, Odermatt J, Huber A, Christ-Crain M et al (2016) Trimethylamine-N-oxide (TMAO) predicts fatal outcomes in community-acquired pneumonia patients without evident coronary artery disease. Eur J Intern Med 36:67–73
Tang WH, Topol EJ, Fan Y, Wu Y, Cho L, Stevenson C et al (2014) Prognostic value of estimated functional capacity incremental to cardiac biomarkers in stable cardiac patients. J Am Heart Assoc 3(5):e000960
Tang WH, Wang Z, Kennedy DJ, Wu Y, Buffa JA, Agatisa-Boyle B et al (2015) Gut microbiota-dependent trimethylamine N-oxide (TMAO) pathway contributes to both development of renal insufficiency and mortality risk in chronic kidney disease. Circ Res 116:448–455
Tang WH, Wang Z, Li XS, Fan Y, Li DS, Wu Y et al (2017) Increased trimethylamine N-oxide portends high mortality risk independent of glycemic control in patients with type 2 diabetes mellitus. Clin Chem 63:297–306
Suzuki T, Heaney LM, Bhandari SS, Jones DJ, Ng LL (2016) Trimethylamine N-oxide and prognosis in acute heart failure. Heart 102:841–848
Senthong V, Wang Z, Fan Y, Wu Y, Hazen SL, Tang WH (2016) Trimethylamine N-oxide and mortality risk in patients with peripheral artery disease. J Am Heart Assoc 5:e004237
Tang WH, Wang Z, Levison BS, Koeth RA, Britt EB, Fu X et al (2013) Intestinal microbial metabolism of phosphatidylcholine and cardiovascular risk. N Engl J Med 368:1575–1584
Li XS, Obeid S, Klingenberg R, Gencer B, Mach F, Räber L et al (2017) Gut microbiota-dependent trimethylamine N-oxide in acute coronary syndromes: a prognostic marker for incident cardiovascular events beyond traditional risk factors. Eur Heart J 38:814–824
Suzuki T, Heaney LM, Jones DJ, Ng LL (2017) Trimethylamine N-oxide and risk stratification after acute myocardial infarction. Clin Chem 63:420–428
Piepoli FM (2017) European Guidelines on cardiovascular disease prevention in clinical practice: the sixth joint task force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of 10 societies and by invited experts). Int J Behav Med. 24:321–419
Wang Z, Zhao Y (2018) Gut microbiota derived metabolites in cardiovascular health and disease. Protein Cell 9:416–431
Seldin MM, Meng Y, Qi H, Zhu W, Wang Z, Hazen SL et al (2016) Trimethylamine N-oxide promotes vascular inflammation through signalling of mitogen-activated protein kinase and nuclear factor-κB. J Am Heart Assoc 5(2):e002767
Zhu W, Gregory JC, Org E, Buffa JA, Gupta N, Wang Z et al (2016) Gut microbial metabolite TMAO enhances platelet hyperreactivity and thrombosis risk. Cell 165:111–124
Zhu W, Wang Z, Tang WHW, Hazen SL (2017) Gut microbe-generated trimethylamine N-oxide from dietary choline is prothrombotic in subjects. Circulation 135:1671–1673
Loscalzo J (2013) Gut microbiota, the genome, and diet in atherogenesis. N Engl J Med 368:1647–1649
Abbasi J (2019) TMAO and heart disease: the new red meat risk? JAMA 321:2149–2151
Bogiatzi C, Gloor G, Allen-Vercoe E, Reid G, Wong RG, Urquhart BL et al (2018) Metabolic products of the intestinal microbiome and extremes of atherosclerosis. Atherosclerosis 273:91–97
Roberts AB, Gu X, Buffa JA, Hurd AG, Wang Z, Zhu W et al (2018) Development of a gut microbe-targeted nonlethal therapeutic to inhibit thrombosis potential. Nat Med 24:1407–1417
Bennett BJ, de Aguiar Vallim TQ, Wang Z, Shih DM, Meng Y, Gregory J et al (2013) Trimethylamine-N-oxide, a metabolite associated with atherosclerosis, exhibits complex genetic and dietary regulation. Cell Metab 17:49–60
Shih DM, Wang Z, Lee R, Meng Y, Che N, Charugundla S et al (2015) Flavin containing monooxygenase 3 exerts broad effects on glucose and lipid metabolism and atherosclerosis. J Lipid Res 56:22–37
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Statement of human and animal rights
This article does not contain any studies with human participants or animals preformed by any of the authors.
Informed consent
For this study, formal consent was not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Guasti, L., Galliazzo, S., Molaro, M. et al. TMAO as a biomarker of cardiovascular events: a systematic review and meta-analysis. Intern Emerg Med 16, 201–207 (2021). https://doi.org/10.1007/s11739-020-02470-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-020-02470-5