Abstract
Background
Bacterial infection is one of the most frequent complications in acute-on-chronic liver failure (ACLF), which leads to high mortality. However, a specific prognostic model for ACLF patients with bacterial infection has not been well established.
Aim
To establish and validate a nomogram for predicting 30-day mortality of hepatitis B virus-related ACLF (HBV-ACLF) patients with bacterial infection.
Methods
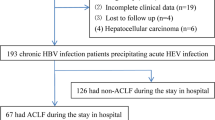
A total of 513 ACLF patients for HBV reactivation were enrolled in the prospective cohort, and 224 patients with bacterial infection were for derivation. Independent predictors were identified using multivariate logistic model and then assembled into a nomogram to predict 30-day mortality. The performance of the nomogram was assessed based on its calibration, discrimination and clinical utility in a retrospective cohort of 192 HBV-ACLF patients with bacterial infection.
Results
Age, total bilirubin, lactate dehydrogenase, international normalized ratio and soluble interleukin-2 receptor were shown to be independent risk factors for 30-day mortality of HBV-ACLF patients with bacterial infection and the nomogram was constructed. The nomogram showed a good calibration and discrimination in the derivation cohort, with an area under the receiver operating characteristic curve (AUC) of 0.883. Application of the nomogram in the validation cohort also showed a good calibration and discrimination, with the AUC of 0.852. Decision curve analysis confirmed the clinical utility of the nomogram.
Conclusion
The nomogram was established and validated for predicting 30-day mortality of HBV-ACLF patients with bacterial infection, which may facilitate optimal therapeutic strategies to improve the prognosis of these patients.



Similar content being viewed by others
Availability of data
We declared that data described in the manuscript would be freely available to any scientist wishing to use them for non-commercial purposes.
References
Bajaj JS, O’Leary JG, Wong F, et al. Bacterial infections in end-stage liver disease: current challenges and future directions. Gut 2012;61(8):1219–1225
Yang L, Wu T, Li J, et al. Bacterial infections in acute-on-chronic liver failure. Semin Liver Dis 2018;38(2):121–133
Mücke MM, Rumyantseva T, Mücke VT, et al. Bacterial infection-triggered acute-on-chronic liver failure is associated with increased mortality. Liver Int 2018;38(4):645–653
Fernandez J, Acevedo J, Wiest R, et al. Bacterial and fungal infections in acute-on-chronic liver failure: prevalence, characteristics and impact on prognosis. Gut 2018;67(10):1870–1880
Said A, Williams J, Holden J, et al. Model for end stage liver disease score predicts mortality across a broad spectrum of liver disease. J Hepatol 2004;40(6):897–903
Nagai S, Chau LC, Schilke RE, et al. Effects of allocating livers for transplantation based on model for end-stage liver disease-sodium scores on patient outcomes. Gastroenterology 2018;155(5):1451–1462
Jalan R, Saliba F, Pavesi M, et al. Development and validation of a prognostic score to predict mortality in patients with acute-on-chronic liver failure. J Hepatol 2014;61(5):1038–1047
Choudhury A, Jindal A, Maiwall R, et al. Liver failure determines the outcome in patients of acute-on-chronic liver failure (ACLF): comparison of APASL ACLF research consortium (AARC) and CLIF-SOFA models. Hepatol Int 2017;11(5):461–471
Chen T, Yang Z, Choudhury AK, et al. Complications constitute a major risk factor for mortality in hepatitis B virus-related acute-on-chronic liver failure patients: a multi-national study from the Asia–Pacific region. Hepatol Int 2019;13(6):695–705
Li Q, Wang J, Lu M, et al. Acute-on-chronic liver failure from chronic-hepatitis-B, who is the behind scenes. Front Microbiol 2020;11:583423
Sarin SK, Kedarisetty CK, Abbas Z, et al. Acute-on-chronic liver failure: consensus recommendations of the Asian Pacific Association for the Study of the Liver (APASL) 2014. Hepatol Int 2014;8(4):453–471
Sarin SK, Kumar M, Lau GK, et al. Asian-Pacific clinical practice guidelines on the management of hepatitis B: a 2015 update. Hepatol Int 2016;10(1):1–98
Patidar KR, Bajaj JS. Covert and overt hepatic encephalopathy: diagnosis and management. Clin Gastroenterol Hepatol 2015;13(12):2048–2061
Angeli P, Gines P, Wong F, et al. Diagnosis and management of acute kidney injury in patients with cirrhosis: revised consensus recommendations of the International Club of Ascites. J Hepatol 2015;62(4):968–974
Wong F, Piano S, Singh V, et al. Clinical features and evolution of bacterial infection-related acute-on-chronic liver failure. J Hepatol 2020;74(2):330–339
Jalan R, Fernandez J, Wiest R, et al. Bacterial infections in cirrhosis: a position statement based on the EASL Special Conference 2013. J Hepatol 2014;60(6):1310–1324
Cao ZJ, Liu YH, Zhu CW, et al. Bacterial infection triggers and complicates acute-on-chronic liver failure in patients with hepatitis B virus-decompensated cirrhosis: a retrospective cohort study. World J Gastroenterol 2020;26(6):645–656
Hernaez R, Kramer JR, Liu Y, et al. Prevalence and short-term mortality of acute-on-chronic liver failure: a national cohort study from the USA. J Hepatol 2019;70(4):639–647
Wu D, Zhang S, Xie Z, et al. Plasminogen as a prognostic biomarker for HBV-related acute-on-chronic liver failure. J Clin Invest 2020;130(4):2069–2080
Ferriero R, Nusco E, De Cegli R, et al. Pyruvate dehydrogenase complex and lactate dehydrogenase are targets for therapy of acute liver failure. J Hepatol 2018;69(2):325–335
Cui J, Xiong J, Zhang Y, et al. Serum lactate dehydrogenase is predictive of persistent organ failure in acute pancreatitis. J Crit Care 2017;41:161–165
Duman A, Akoz A, Kapci M, et al. Prognostic value of neglected biomarker in sepsis patients with the old and new criteria: predictive role of lactate dehydrogenase. Am J Emerg Med 2016;34(11):2167–2171
Lu J, Wei Z, Jiang H, et al. Lactate dehydrogenase is associated with 28-day mortality in patients with sepsis: a retrospective observational study. J Surg Res 2018;228:314–321
Saito K, Wagatsuma T, Toyama H, et al. Sepsis is characterized by the increases in percentages of circulating CD4+CD25+ regulatory T cells and plasma levels of soluble CD25. Tohoku J Exp Med 2008;216(1):61–68
Delogu G, Casula MA, Mancini P, et al. Serum neopterin and soluble interleukin-2 receptor for prediction of a shock state in gram-negative sepsis. J Crit Care 1995;10(2):64–71
García De Guadiana-Romualdo L, Berger M, Jiménez-Santos E, et al. Pancreatic stone protein and soluble CD25 for infection and sepsis in an emergency department. Eur J Clin Investig 2017;47(4):297–304
Zhai XR, Tong JJ, Wang HM, et al. Infection deteriorating hepatitis B virus related acute-on-chronic liver failure: a retrospective cohort study. BMC Gastroenterol 2020;20(1):320
Funding
This study was funded by the National Thirteenth “Five Years” Project in Science and Technology of China (2017ZX10202201, 2018ZX10302-206).
Author information
Authors and Affiliations
Contributions
All authors were involved in the critical revision of the manuscript. TC and QN contributed to the study conception and design. ZZ, ZY, QC, XH, ML, YL, KM, TL, MZ enrolled patients and collected clinical data. ZZ analyzed clinical data and drafted the manuscript. XL had contributions to the revision of the manuscript in discussion, data re-evaluation and presentation, and manuscript edition. All authors approved the final version of the manuscript, including the authorship list.
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare no conflicts of interest about this work.
Ethical approval
Data of all patients were acquired from the electronic medical records system and analyzed anonymously according to the Declaration of Helsinki of 1975, as revised in 2008. A written informed consent of patient was acquired based on registered clinical trial (NCT03362632) in the prospective derivation cohort. However, the patient informed consent was waived in the retrospective validation cohort according to approved protocol by the Ethics Committee of Tongji Hospital.
Consent for publication
All authors read and approved the manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, Z., Yang, Z., Cheng, Q. et al. Establishment and validation of a prognostic model for hepatitis B virus‑related acute-on-chronic liver failure patients with bacterial infection. Hepatol Int 16, 38–47 (2022). https://doi.org/10.1007/s12072-021-10268-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-021-10268-6