Abstract
Background
Approximately 60–70% of breast cancer survivors experience sexuality problems resulting from treatment. This study investigated information and communication preferences with professionals on the topic intimacy and sexuality of women diagnosed with breast cancer.
Methods
Members of the Dutch Breast Cancer Patient Association were surveyed regarding their experiences and preferences about information on intimacy and sexuality. An online questionnaire was developed that included five close-ended and one open-ended question regarding: information received; type of professional preferred; method and timing of communication on the topics of intimacy and sexuality. Quantitative data were analysed using descriptive statistics. A deductive framework analysis was performed on the open-ended answers to enrich the data of the close-ended questions.
Results
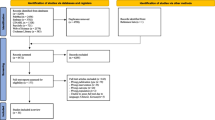
In total, 667 female breast cancer (ex-)patients participated. In 46% of the women, the information received matched their needs. Most women preferred to receive information about the impact on intimacy and sexuality from a nurse (66.4%) or primary doctor (27.9%). The preferred method of communication was a conversation with a professional together with their partner (51.6%) or a personal conversation with a professional. Respondents emphasized the importance of appropriate timing of information, preferably at least shortly after the treatment started (45.1%).
Conclusions
This study shows that intimacy and sexuality should be repeatedly included in consultations, at every stage of the disease but especially shortly after treatment started. Women with breast cancer expect that professionals (preferably nurse or primary doctor) initiate this subject via a personal conversation (alone or with their partner).
Similar content being viewed by others
References
Ferlay J, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer. 2015;136(5):E359–86.
IKNL. Statistics about cancer [cijfers over kanker]. 2016 (cited 16 June 2016). https://www.cijfersoverkanker.nl.
Renard F, Van Eycken L, Arbyn M. High burden of breast cancer in Belgium: recent trends in incidence (1999–2006) and historical trends in mortality (1954–2006). Arch Public Health. 2011;69(1):2.
Bastiaannet E, et al. Lack of survival gain for elderly women with breast cancer. Oncologist. 2011;16(4):415–23.
Schultz PN, et al. Breast cancer: relationship between menopausal symptoms, physiologic health effects of cancer treatment and physical constraints on quality of life in long-term survivors. J Clin Nurs. 2005;14(2):204–11.
Malinovszky KM, et al. Quality of life and sexual function after high-dose or conventional chemotherapy for high-risk breast cancer. Br J Cancer. 2006;95(12):1626–31.
Panjari M, Bell RJ, Davis SR. Sexual function after breast cancer. J Sex Med. 2011;8(1):294–302.
Kedde H, et al. Sexual dysfunction in young women with breast cancer. Support Care Cancer. 2013;21(1):271–80.
Ussher JM, Perz J, Gilbert E. Changes to sexual well-being and intimacy after breast cancer. Cancer Nurs. 2012;35(6):456–65.
Gilbert E, Ussher JM, Perz J. Sexuality after breast cancer: a review. Maturitas. 2010;66(4):397–407.
Taylor S, et al. Breast cancer, sexuality, and intimacy: addressing the unmet need. Breast J. 2016;22(4):478–9.
Loaring JM, et al. Renegotiating sexual intimacy in the context of altered embodiment: the experiences of women with breast cancer and their male partners following mastectomy and reconstruction. Health Psychol. 2015;34(4):426–36.
Manne SL, et al. Cancer-specific relationship awareness, relationship communication, and intimacy among couples coping with early stage breast cancer. J Soc Pers Relat. 2014;31(3):314–34.
Milbury K, Badr H. Sexual problems, communication patterns, and depressive symptoms in couples coping with metastatic breast cancer. Psychooncology. 2013;22(4):814–22.
Ussher JM, Perz J, Gilbert E. Perceived causes and consequences of sexual changes after cancer for women and men: a mixed method study. BMC Cancer. 2015;15:268.
Borstkankervereniging Nederland. Who are the 1800 participants? [Wie zijn de 1800 deelnemers?]; 2016. https://bforce.nl/nl/deelnemers. Accessed 15 Sept 2016.
Burnard P, et al. Analysing and presenting qualitative data. Br Dent J. 2008;204(8):429–32.
Johnson JK, Barach P, Vernooij-Dassen M. Conducting a multicentre and multinational qualitative study on patient transitions. BMJ Qual Saf. 2012;21(Suppl 1):i22-8.
Kedde H, et al. Subjective sexual well-being and sexual behavior in young women with breast cancer. Support Care Cancer. 2013;21(7):1993–2005.
Ussher JM, Perz J, Gilbert E. Information needs associated with changes to sexual well-being after breast cancer. J Adv Nurs. 2013;69(2):327–37.
Cleary V, Hegarty J. Understanding sexuality in women with gynaecological cancer. Eur J Oncol Nurs. 2011;15(1):38–45.
Leung MW, Goldfarb S, Dizon DS. Communication about sexuality in advanced illness aligns with a palliative care approach to patient-centered care. Curr Oncol Rep. 2016;18(2):11.
Seidler ZE, et al. Let’s talk about sex after cancer: exploring barriers and facilitators to sexual communication in male cancer survivors. Psychooncology. 2016;25:670–6.
O’Brien R, et al. “I wish I’d told them”: a qualitative study examining the unmet psychosexual needs of prostate cancer patients during follow-up after treatment. Patient Educ Couns. 2011;84(2):200–7.
Zhou ES, Nekhlyudov L, Bober SL. The primary health care physician and the cancer patient: tips and strategies for managing sexual health. Transl Androl Urol. 2015;4(2):218–31.
Jonsdottir JI, et al. Changes in attitudes, practices and barriers among oncology health care professionals regarding sexual health care: Outcomes from a 2-year educational intervention at a University Hospital. Eur J Oncol Nurs. 2016;21:24–30.
de Vocht HM, et al. Stepped Skills: a team approach towards communication about sexuality and intimacy in cancer and palliative care. Australas Med J. 2011;4(11):610–9.
Canzona MR, et al. Communication about sexual health with breast cancer survivors: variation among patient and provider perspectives. Patient Educ Couns. 2016;99(11):1814–20.
Reese JB, et al. Effective patient-provider communication about sexual concerns in breast cancer: a qualitative study. Support Care Cancer. 2017;25:3199–207.
Tennant B, et al. eHealth literacy and Web 2.0 health information seeking behaviors among baby boomers and older adults. J Med Internet Res. 2015;17(3):e70.
WHO. Track 2: health literacy and health behaviour. 2018. https://www.who.int/healthpromotion/conferences/7gchp/track2/en/. Accessed 15 Sept.
Guetterman TC, Fetters MD, Creswell JW. Integrating quantitative and qualitative results in health science mixed methods research through joint displays. Ann Fam Med. 2015;13(6):554–61.
Acknowledgements
The authors gratefully acknowledge the Dutch Breast Cancer Patient Association (‘Borstkankervereniging Nederland’) for their contribution to the data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Den Ouden, M.E.M., Pelgrum-Keurhorst, M.N., Uitdehaag, M.J. et al. Intimacy and sexuality in women with breast cancer: professional guidance needed. Breast Cancer 26, 326–332 (2019). https://doi.org/10.1007/s12282-018-0927-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-018-0927-8