Abstract
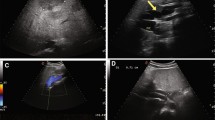
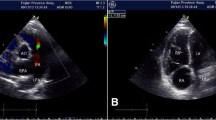
Congenital extrahepatic portosystemic shunt (CEPS) is an extremely rare anomaly. In these malformations splanchnic blood bypasses the liver and drains into the systemic circulation through the inferior vena cava (IVC) or the left renal vein (LRV). Extrahepatic shunts may be divided into type 1 [end-to-side mesenterico-caval fistula with congenital absence of the portal vein (PV)] and type 2 (partial portocaval shunt caused by side-to-side mesenterico-caval fistula with normal or hypoplasic PV). Type 2 shunts typically are wholly extrahepatic between the PV or its right branch and the retrohepatic IVC. This report describes an asymptomatic case of CEPS not previously documented and not classifiable as type 1 or 2. CT revealed a normal PV with communication between the inferior mesenteric vein (IMV) and the LRV. The inferior mesenteric vein appeared tortuous, abnormally long and with a large calibre, and presented a connection with the LRV, in addition to a normal confluence into the splenic vein. Colour Doppler revealed hepatopetal normal flow in the PV and superior mesenteric vein with mild portal hypertension and an inversion of flow in the IMV directed to the LRV. Biochemical parameters showed a normal liver function without hyperammonaemia.

Similar content being viewed by others
References
Abernethy J. Account of two instances of uncommon formation in the viscera of the human body. Philos Trans R Soc. 1793;83:59–66.
Alvarez AE, Ribeiro AF, Hessel G, Baracat J, ribeiro JD. Abernethy malformation: one of the etiologies of hepatopulmonary syndrome. Pediatr Pulmonol. 2002;34:391–4.
Kanamori Y, Hashizume K, Kitano Y, Sugiyama M, Motoi T, Tange T. Congenital extrahepatic portocaval shunt (Abernethy type 2), huge liver mass, and patent ductus arteriosus—a case report of its rare clinical presentation in a young girl. J Pediatr Surg. 2003;38:E15.
Takayama Y, Moriura S, Nagata J, Akutagawa A, Hirano A, Ishiguro S, et al. Embolization of the left portal vein to inferior vena cava shunts for chronic recurrent hepatic encephalopathy via the mesenteric vein. J Gastroenterol Hepatol. 2001;16:1425–8.
Stringer MD. The clinical anatomy of congenital portosystemic venous shunts. Clin Anat. 2008;21:147–57.
Altavilla G, Cusatelli P. Ultrastructural analysis of the liver with portal vein agenesis: a case report. Ultrastruct Pathol. 1998;22:477–83.
Morgan G, Superina R. Congenital absence of the portal vein: two cases and a proposed classification system for portasystemic vascular anomalies. J Pediatr Surg. 1994;29:1239–41.
Uchino T, Endo F, Ikeda S, Shiraki K, Sera Y, Matsuda I. Three brothers with progressive hepatic dysfunction and severe hepatic steatosis due to a patent ductus venosus. Gastroenterology. 1997;110:1964–8.
Henderson JM, Nagle A, Curtas S, Geisinger M, Barnes D. Surgical shunts and TIPS for variceal decompression in the 1990s. Surgery. 2000;128(4):540–7.
Handerson JM, Boyer TD, Kutner MH, Galloway GR, Rikkers LF, Jeffers LJ, et al. Distal splenorenal shunt versus transjugular intrahepatic portal systematic shunt for variceal bleeding: a randomized trial. Gastroenterology. 2006;130(6):1643–51.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bazzocchi, G., Pastorelli, D., Laviani, F. et al. New type of asymptomatic congenital portosystemic shunt. Clin J Gastroenterol 2, 43–46 (2009). https://doi.org/10.1007/s12328-008-0037-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-008-0037-9