Abstract
Drug delivery into the inner ear is a significant challenge due to its inaccessibility as a fluid-filled cavity within the temporal bone of the skull. The round window membrane (RWM) is the only delivery portal from the middle ear to the inner ear that does not require perforation of bone. Recent advances in microneedle fabrication enable the RWM to be perforated safely with polymeric microneedles as a means to enhance the rate of drug delivery from the middle ear to the inner ear. However, the polymeric material is not biocompatible and also lacks the strength of other materials. Herein we describe the design and development of gold-coated metallic microneedles suitable for RWM perforation. When developing microneedle technology for drug delivery, we considered three important general attributes: (1) high strength and ductility material, (2) high accuracy and precision of fabrication, and (3) broad design freedom. We developed a hybrid additive manufacturing method using two-photon lithography and electrochemical deposition to fabricate ultra-sharp gold-coated copper microneedles with these attributes. We refer to the microneedle fabrication methodology as two-photon templated electrodeposition (2PTE). We demonstrate the use of these microneedles by inducing a perforation with a minimal degree of trauma in a guinea pig RWM while the microneedle itself remains undamaged. Thus, this microneedle has the potential literally of opening the RWM for enhanced drug delivery into the inner ear. Finally, the 2PTE methodology can be applied to many different classes of microneedles for other drug delivery purposes as well the fabrication of small scale structures and devices for non-medical applications.

Fully metallic ultra-sharp microneedle mounted at end of a 24-gauge stainless steel blunt syringe needle tip: (left) Size of microneedle shown relative to date stamp on U.S. one-cent coin; (right) Perforation through guinea pig round window membrane introduced with microneedle.









Similar content being viewed by others
References
McCall AA, Swan EEL, Borenstein JT, Sewell WF, Kujawa SG, McKenna MJ. 2010. Drug delivery for treatment of inner ear disease: current state of knowledge. Ear and Hearing 31(2).
Naples JG, Miller LE, Ramsey A, Li D. 2019. Cochlear protein biomarkers as potential sites for targeted inner ear drug delivery. Drug delivery and translational research, pp 1–12.
Szeto B, Chiang H, Valentini C, Yu M, Kysar JW, Lalwani AK. 2019, Inner ear delivery: challenges and opportunities. Laryngoscope Investigative Otolaryngology.
Early S, Moon IS, Bommakanti K, Hunter I, Stankovic KM. 2019. A novel microneedle device for controlled and reliable liquid biopsy of the human inner ear. Hearing Research.
Plontke SK, Hartsock JJ, Gill RM, Salt AN. Intracochlear drug injections through the round window membrane: measures to improve drug retention. Audiology and Neuro-Otology 2016;21(2):72–79. https://doi.org/10.1159/000442514.
Salt AN, Sirjani DB, Hartsock JJ, Gill RM, Plontke SK. Marker retention in the cochlea following injections through the round window membrane. Hearing Research 2007;232(1):78–86. https://doi.org/10.1016/j.heares.2007.06.010.
Musazzi UM, Franzé S, Cilurzo F. Innovative pharmaceutical approaches for the management of inner ear disorders. Drug Delivery and Translational Research 2018;8(2):436–449.
Salt AN, Plontke SK. Pharmacokinetic principles in the inner ear: influence of drug properties on intratympanic applications. Hearing research 2018;368:28–40.
Aksit A, Arteaga DN, Arriaga M, Wang X, Watanabe H, Kasza KE, Lalwani AK, Kysar JW. In-vitro perforation of the round window membrane via direct 3-d printed microneedles. Biomed Microdevices 2018;20(2):47. https://doi.org/10.1007/s10544-018-0287-3.
Kelso C, Watanabe H, Wazen J, Bucher T. Microperforations significantly enhance diffusion across round window membrane. Otology & Neurotology 2015;36(4):694–700.
Santimetaneedol A, Wang Z, Arteaga D, Aksit A, Prevoteau C, Yu M, Chiang H, Fafalis D, Lalwani A, Kysar J. Small molecule delivery across a perforated artificial membrane by thermoreversible hydrogel poloxamer 407. Colloids Surf B: Biointerfaces 2019;182:110300.
Yu M, Arteaga DN, Aksit A, Chiang H, Olson ES, Kysar JW, Lalwani AK. Anatomical and functional consequences of microneedle perforation of round window membrane. Otology & Neurotology 2020;41(2): e280–e287.
Chiang H, Yu M, Aksit A, Wang W, Stern-Shavit S, Kysar JW, Lalwani AK. 3D-printed microneedles create precise perforations in human round window membrane in situ. Otology & Neurotology 2020;41(2): 277–284.
Kaushik S, Hord AH, Denson DD, McAllister DV, Smitra S, Allen MG, Prausnitz MR. Lack of pain associated with microfabricated microneedles. Anesthesia & Analgesia 2001;92(2):502–504.
Donnelly RF, Singh TRR, Woolfson AD. Microneedle-based drug delivery systems: microfabrication, drug delivery, and safety. Drug Delivery 2010;17(4):187–207.
Gardeniers HJ, Luttge R, Berenschot EJ, De Boer MJ, Yeshurun SY, Hefetz M, van’t Oever R, van den Berg A. Silicon micromachined hollow microneedles for transdermal liquid transport. Journal of Microelectromechanical Systems 2003;12(6):855–862.
Park JH, Allen MG, Prausnitz MR. Biodegradable polymer microneedles: fabrication, mechanics and transdermal drug delivery. Journal of Controlled Release 2005;104(1):51–66.
Prausnitz MR. Microneedles for transdermal drug delivery. Advanced Drug Delivery Reviews 2004;56(5):581–587. https://doi.org/10.1016/j.addr.2003.10.023, breaking the Skin Barrier.
Jiang J, Moore JS, Edelhauser HF, Prausnitz MR. Intrascleral drug delivery to the eye using hollow microneedles. Pharmaceutical Research 2009;26(2):395–403.
Kim YC, Park JH, Prausnitz MR. Microneedles for drug and vaccine delivery. Advanced Drug Delivery Reviews 2012;64(14):1547–1568. https://doi.org/10.1016/j.addr.2012.04.005. emerging micro- and nanotechnologies for the development of novel drug delivery devices and systems.
Ma G, Wu C. Microneedle, bio-microneedle and bio-inspired microneedle: a review. J Control Release 2017; 251:11–23.
Rzhevskiy AS, Singh TRR, Donnelly RF, Anissimov YG. Microneedles as the technique of drug delivery enhancement in diverse organs and tissues. J Control Release 2018; 270: 184–202. https://doi.org/10.1016/j.jconrel.2017.11.048.
Baek C, Han M, Min J, Prausnitz MR, Park JH, Park JH. Local transdermal delivery of phenylephrine to the anal sphincter muscle using microneedles. Journal of Controlled Release 2011;154(2):138–147.
Chiu WS, Belsey NA, Garrett NL, Moger J, Price GJ, Delgado-Charro MB, Guy RH. Drug delivery into microneedle-porated nails from nanoparticle reservoirs. J Control Release 2015;220:98–106.
Choi CK, Kim JB, Jang EH, Youn YN, Ryu WH. Curved biodegradable microneedles for vascular drug delivery. Small 2012;8(16):2483–2488.
Dhurat R, Sukesh M, Avhad G, Dandale A, Pal A, Pund P. A randomized evaluator blinded study of effect of microneedling in androgenetic alopecia: a pilot study. International Journal of Trichology 2013;5(1):6.
Ma Y, Tao W, Krebs SJ, Sutton WF, Haigwood NL, Gill HS. Vaccine delivery to the oral cavity using coated microneedles induces systemic and mucosal immunity. Pharmaceutical Research 2014;31(9): 2393–2403.
Traverso G, Schoellhammer CM, Schroeder A, Maa R, Lauwers GY, Polat BE, Anderson DG, Blankschtein D, Langer R. Microneedles for drug delivery via the gastrointestinal tract. Journal of Pharmaceutical Sciences 2015;104(2):362–367.
Wang N, Zhen Y, Jin Y, Wang X, Li N, Jiang S, Wang T. Combining different types of multifunctional liposomes loaded with ammonium bicarbonate to fabricate microneedle arrays as a vaginal mucosal vaccine adjuvant-dual delivery system (vadds). J Control Release 2017;246:12–29.
Watanabe H, Lalwani AK, Kysar JW Tekalur S A, Zavattieri P, Korach C S, (eds). 2016. In situ nano-indentation of round window membrane, Vol. 6. Cham: Springer International Publishing.
Donnelly RF, Singh TRR, Tunney MM, Morrow DI, McCarron PA, O’Mahony C, Woolfson AD. Microneedle arrays allow lower microbial penetration than hypodermic needles in vitro. Pharmaceutical Research 2009; 26(11):2513–2522.
Henry S, McAllister DV, Allen MG, Prausnitz MR. Microfabricated microneedles: a novel approach to transdermal drug delivery. Journal of Pharmaceutical Sciences 1998;87(8):922–925.
Bean KE, Runyan W. 1990. Semiconductor integrated circuit processing technology. Addison-Wesley.
Braybrook JH. 1996. Biocompatiblity: assessment of medical devices and materials. Biocompatiblity: assessment of medical devices and materials, by Julian H Braybrook (Editor), pp 246 ISBN 0-471-96597-9 Wiley-VCH, December 1996 p 246.
García-López E, Siller HR, Rodríguez CA. Study of the fabrication of AISI 316L microneedle arrays. Procedia Manufacturing 2018;26:117–124. https://doi.org/10.1016/j.promfg.2018.07.014, http://www.sciencedirect.com/science/article/pii/S235197891830684X, 46th SME North American Manufacturing Research Conference NAMRC 46.
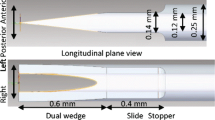
Watanabe H, Cardoso L, Lalwani AK, Kysar JW. A dual wedge microneedle for sampling of perilymph solution via round window membrane. Biomed Microdevices 2016;18(2):24. https://doi.org/10.1007/s10544-016-0046-2.
Martanto W, Davis SP, Holiday NR, Wang J, Gill HS, Prausnitz MR. Transdermal delivery of insulin using microneedles in vivo. Pharm Res 2004;21(6):947–952. https://doi.org/10.1023/B:PHAM.0000029282.44140.2e.
Cahill EM, Keaveney S, Stuettgen V, Eberts P, Ramos-Luna P, Zhang N, Dangol M, O’Cearbhaill ED. Metallic microneedles with interconnected porosity: a scalable platform for biosensing and drug delivery. Acta Biomaterialia 2018;80:401–411. https://doi.org/10.1016/j.actbio.2018.09.007, http://www.sciencedirect.com/science/article/pii/S1742706118305245.
Li J, Liu B, Zhou Y, Chen Z, Jiang L, Yuan W, Liang L. Fabrication of a Ti porous microneedle array by metal injection molding for transdermal drug delivery. PLOS ONE 2017;12(2):1–15. https://doi.org/10.1371/journal.pone.0172043.
Chandrasekaran S, Brazzle JD, Frazier AB. Surface micromachined metallic microneedles. J Microelectromech Syst 2003;12(3):281–288. https://doi.org/10.1109/JMEMS.2003.809951.
Davis SP, Prausnitz MR, Allen MG. Fabrication and characterization of laser micromachined hollow microneedles. TRANSDUCERS ’03. 12th International Conference on Solid-State Sensors, Actuators and Microsystems. Digest of Technical Papers (Cat. No.03TH8664); 2003. p. 1435–1438. https://doi.org/10.1109/SENSOR.2003.1217045.
Davis SP, Landis BJ, Adams ZH, Allen MG, Prausnitz MR. Insertion of microneedles into skin: measurement and prediction of insertion force and needle fracture force. Journal of Biomechanics 2004;37(8): 1155–1163. https://doi.org/10.1016/j.jbiomech.2003.12.010, http://www.sciencedirect.com/science/article/pii/S0021929003004731.
Kim K, Lee JB. High aspect ratio tapered hollow metallic microneedle arrays with microfluidic interconnector. Microsystem Technologies 2007;13(3):231–235. https://doi.org/10.1007/s00542-006-0221-0.
Kim K, Park DS, Lu HM, Che W, Kim K, Lee JB, Ahn CH. A tapered hollow metallic microneedle array using backside exposure of SU-8. J Micromech Microeng 2004;14(4):597–603. https://doi.org/10.1088/0960-1317/14/4/021.
Li CG, Lee CY, Lee K, Jung H. An optimized hollow microneedle for minimally invasive blood extraction. Biomedical Microdevices 2013;15(1):17–25. https://doi.org/10.1007/s10544-012-9683-2.
Serbin J, Egbert A, Ostendorf A, Chichkov BN, Houbertz R, Domann G, Schulz J, Cronauer C, Fröhlich L, Popall M. Femtosecond laser-induced two-photon polymerization of inorganic–organic hybrid materials for applications in photonics. Opt Lett 2003;28(5):301–303. https://doi.org/10.1364/OL.28.000301.
Rad ZF, Nordon RE, Anthony CJ, Bilston L, Prewett PD, Arns JY, Arns CH, Zhang L, Davies GJ. High-fidelity replication of thermoplastic microneedles with open microfluidic channels. Microsystems & Nanoengineering 2017;3:17034.
Suzuki M, Sawa T, Takahashi T, Aoyagi S. 2015. Ultrafine three-dimensional (3D) laser lithographic fabrication of microneedle and its application to painless insertion and blood sampling inspired by mosquito. In: 2015 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS), pp 2748–2753. https://doi.org/10.1109/IROS.2015.7353754.
Forvi E, Bedoni M, Carabalona R, Soncini M, Mazzoleni P, Rizzo F, O’Mahony C, Morasso C, Cassarà D G, Gramatica F. Preliminary technological assessment of microneedles-based dry electrodes for biopotential monitoring in clinical examinations. Sensors Actuators A Phys 2012;180:177–186.
O’Mahony C, Pini F, Blake A, Webster C, O’Brien J, McCarthy KG. Microneedle-based electrodes with integrated through-silicon via for biopotential recording. Sensors Actuators A Phys 2012;186:130–136.
Backer E, Ehrfeld W, Münchmeyer D, Betz H, Heuberger A, Pongratz S, Glashauser W, Michel H, Rv Siemens. Production of separation-nozzle systems for uranium enrichment by a combination of x-ray lithography and galvanoplastics. Naturwissenschaften 1982;69(11):520–523.
Daryadel S, Behroozfar A, Minary-Jolandan M. Toward control of microstructure in microscale additive manufacturing of copper using localized electrodeposition. Advanced Engineering Materials 2019;21(1):1800946. https://doi.org/10.1002/adem.201800946.
Hasegawa M, Yoon S, Guillonneau G, Zhang Y, Frantz C, Niederberger C, Weidenkaff A, Michler J, Philippe L. The electrodeposition of FeCrNi stainless steel: microstructural changes induced by anode reactions. Phys Chem Chem Phys 2014;16:26375–26384. https://doi.org/10.1039/C4CP03744H.
Schürch P, Pethö L, Schwiedrzik J, Michler J, Philippe L. Additive manufacturing through galvanoforming of 3D nickel microarchitectures: simulation-assisted synthesis. Advanced Materials Technologies 2018; 3(12):1800274. https://doi.org/10.1002/admt.201800274.
Schürch P, Ramachandramoorthy R, Pethö L, Michler J, Philippe L. 2019. Additive manufacturing by template-assisted 3D electrodeposition: nanocrystalline nickel microsprings and microspring arrays. Applied Materials Today, p 100472 https://doi.org/10.1016/j.apmt.2019.100472. http://www.sciencedirect.com/science/article/pii/S2352940719305918.
Hall EO. The deformation and ageing of mild steel: III discussion of results. Proceedings of the Physical Society Section B 1951;64(9):747.
Petch NJ. The cleavage strength of polycrystals. Journal of the Iron and Steel Institute 1953;174(19):25–28.
Kratchman LB, Schuster D, Deitrich MS, Labadie RF. Force perception thresholds in cochlear implantation surgery. Audiology and Neurotology 2016;21(4):244–249.
Wazen JM, Stevens JP, Watanabe H, Kysar JW, Lalwani AK. Silver/silver chloride microneedles can detect penetration through the round window membrane. Journal of Biomedical Materials Research Part B: Applied Biomaterials 2017; 105(2): 307–311. https://doi.org/10.1002/jbm.b.33557, https://onlinelibrary.wiley.com/doi/abs/10.1002/jbm.b.33557.
Micallef J. 2015. Design strategies for 3D printing, Apress, Berkeley, CA, pp 175–200. https://doi.org/10.1007/978-1-4842-0946-2.
Izumi H, Suzuki M, Aoyagi S, Kanzaki T. Realistic imitation of mosquito’s proboscis: electrochemically etched sharp and jagged needles and their cooperative inserting motion. Sensors Actuators A Phys 2011;165(1):115–123.
Kelly JJ, Tian C, West AC. Leveling and microstructural effects of additives for copper electrodeposition. Journal of The Electrochemical Society 1999;146(7):2540–2545.
Roxhed N, Gasser TC, Griss P, Holzapfel GA, Stemme G. Penetration-enhanced ultrasharp microneedles and prediction on skin interaction for efficient transdermal drug delivery. J Microelectromech Syst 2007; 16(6):1429–1440.
Watanabe H, Lalwani AK, Kysar JW. In situ NANO-indentation of round window membrane. Mechanics of Biological Systems and Materials, vol 6, Springer International Publishing, Cham Heidelberg New York Dordrecht London, chap 3, pp 17–29. In: Tekalur SA, Zavattieri P, and Korach CS, editors; 2016.
Acknowledgments
The authors gratefully acknowledge Ryan Gusley, Jonathan Vardner, Professor Elizabeth Olson, Dr. Miguel Arriaga, Wenbin Wang, Richard Li, Dr. Dimitrios Fafalis, Chaoqun Zhou, Young Jae Ryu, Dr. Daniel N. Arteaga, Betsy Szeto, Michelle Yu, Harry Chiang, and Chris Valentini for helpful discussions. This work was performed in part at the Advanced Science Research Center NanoFabrication Facility of the Graduate Center at the City University of New York. This research was supported by NIH National Institute on Deafness and Other Communication Disorders of the National Institutes of Health under award number R01DC014547.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All institutional and national guidelines for the care and use of laboratory animals were followed.
Conflict of interest
All authors declare that they have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Anil K. Lalwani, Alan C. West and Jeffrey W. Kysar are Senior Authors.
Rights and permissions
About this article
Cite this article
Aksit, A., Rastogi, S., Nadal, M.L. et al. Drug delivery device for the inner ear: ultra-sharp fully metallic microneedles. Drug Deliv. and Transl. Res. 11, 214–226 (2021). https://doi.org/10.1007/s13346-020-00782-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-020-00782-9