Abstract
Purpose
Research on employment in people with severe mental illnesses (SMI) in developing countries is sparse and largely limited to employment rates. We conducted a comprehensive study of work, interest in work, and perceived benefits and barriers to work in people with SMI in India.
Methods
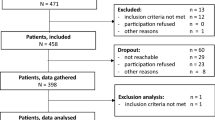
Semi-structured interviews were conducted with 550 individuals with SMI receiving private psychiatric outpatient services in two districts in western India, one urban (Pune) and the other rural (Ahmednagar).
Results
More than half of the participants were employed, with significantly more men working (79.4%) than women (35.9%). Higher rates of work were found in rural areas (77.8%), where most work was in family agricultural businesses, than in urban areas (48.9%), where most work was for independent employers. Participants in rural areas worked fewer hours and earned less money, and reported fewer benefits and fewer problems related to work than urban participants. Over 45% of participants working for independent employers found jobs with help from families and extended social networks. Most unemployed participants wanted to work, and desired a variety of supports, including assistance with job finding and illness management.
Conclusions
Gender-specific social role expectations and families play an important role in work in people with SMI in India. Despite higher rates of work in this sample than most studies from developed countries, a significant subgroup was unemployed but wanted to work. Persons with SMI in developing countries may benefit from the adaptation of validated vocational rehabilitation approaches in developed countries to their cultural context.
Similar content being viewed by others
References
Vos T, Abajobir AA, Abbafati C et al (2017) Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet 390:1211–1259. https://doi.org/10.1016/S0140-6736(17)32154-2
Ruggeri M, Leese M, Thornicroft G et al (2000) Definition and prevalence of severe and persistent mental illness. Br J Psychiatry 177:149–155. https://doi.org/10.1192/bjp.177.2.149
Haro JM, Novick D, Bertsch J et al (2011) Cross-national clinical and functional remission rates: Worldwide Schizophrenia Outpatient Health Outcomes (W-SOHO) study. Br J Psychiatry 199:194–201. https://doi.org/10.1192/bjp.bp.110.082065
Baron RC, Salzer MS (2002) Accounting for unemployment among people with mental illness. Behav Sci Law 20:585–599. https://doi.org/10.1002/bsl.513
Tsang HWH, Leung AY, Chung RCK et al (2010) Review on vocational predictors: a systematic review of predictors of vocational outcomes among individuals with schizophrenia: an update since 1998. Aust N Z J Psychiatry 44:495–504. https://doi.org/10.3109/00048671003785716
Wewiorski NJ, Fabian ES (2004) Association between demographic and diagnostic factors and employment outcomes for people with psychiatric disabilities: a synthesis of recent research. Ment Health Serv Res 6:9–21. https://doi.org/10.1023/B:MHSR.0000011253.36712.15
McGurk SR, Mueser KT (2004) Cognitive functioning, symptoms, and work in supported employment: a review and heuristic model. Schizophr Res 70:147–173. https://doi.org/10.1016/j.schres.2004.01.009
Frounfelker RL, Wilkniss SM, Bond GR et al (2011) Enrollment in supported employment services for clients with a co-occurring disorder. Psychiatr Serv 62:545–547. https://doi.org/10.1176/ps.62.5.pss6205_0545
Mueser K, McGurk S (2014) Supported employment for persons with serious mental illness: Current status and future directions. Encephale 40:s45–s46. https://doi.org/10.1016/j.encep.2014.04.008
Westcott C, Waghorn G, McLean D et al (2015) Interest in employment among people with schizophrenia. Am J Psychiatr Rehabil 18:187–207. https://doi.org/10.1080/15487768.2014.954162
Saxena S, Thornicroft G, Knapp M, Whiteford H (2007) Resources for mental health: scarcity, inequity, and inefficiency. Lancet 370:878–889. https://doi.org/10.1016/S0140-6736(07)61239-2
Burns JK (2015) Why searching for psychosis in diverse settings is important for global research and mental health systems development. Soc Psychiatry Psychiatr Epidemiol 50:895–897. https://doi.org/10.1007/s00127-015-1056-8
World Health Organization (2017) Mental Health Atlas. WHO, Geneva, pp 1–72
Knapp M, Mangalore R, Simon J (2004) The global costs of schizophrenia. Schizophr Bull 30:279–293. https://doi.org/10.1093/oxfordjournals.schbul.a007078
Charlson FJ, Ferrari AJ, Santomauro DF et al (2018) Global epidemiology and burden of schizophrenia: findings from the Global Burden of Disease Study 2016. Schizophr Bull. https://doi.org/10.1093/schbul/sby058
Ran MS, Chen S, Chen EY et al (2011) Risk factors for poor work functioning of persons with schizophrenia in rural China. Soc Psychiatry Psychiatr Epidemiol 46:1087–1093. https://doi.org/10.1007/s00127-010-0285-0
Yang LH, Phillips MR, Li X et al (2013) Employment outcome for people with schizophrenia in rural v. urban China: population-based study. Br J Psychiatry 203:272–279. https://doi.org/10.1192/bjp.bp.112.118927
Shibre T, Medhin G, Alem A et al (2015) Long-term clinical course and outcome of schizophrenia in rural Ethiopia: 10-year follow-up of a population-based cohort. Schizophr Res 161:414–420. https://doi.org/10.1016/j.schres.2014.10.053
Midin M, Razali R, ZamZam R et al (2011) Clinical and cognitive correlates of employment among patients with schizophrenia: a cross-sectional study in Malaysia. Int J Ment Health Syst 5:14. https://doi.org/10.1186/1752-4458-5-14
Rahman MBA, Indran SK (1997) Disability in schizophrenia and mood disorders in a developing country. Soc Psychiatry Psychiatr Epidemiol 32:387–390
Akinsulore A, Mapayi BM, Aloba OO et al (2015) Disability assessment as an outcome measure: a comparative study of Nigerian outpatients with schizophrenia and healthy control. Ann Gen Psychiatry 14:1–7. https://doi.org/10.1186/s12991-015-0079-6
Olagunju AT, Adegbaju DA, Uwakwe R (2016) Disability among attendees with schizophrenia in a Nigerian hospital: further evidence for integrated rehabilitative treatment designs. Ment Illn 8:40–46. https://doi.org/10.4081/mi.2016.6647
Srinivasan TN, Thara R (1997) How do men with schizophrenia fare at work? A follow-up study from India. Schizophr Res 25:149–154. https://doi.org/10.1016/S0920-9964(97)00016-9
Thara R (2004) Twenty Year Course of Schizophrenia: the Madras Longitudinal Study. Can J Psychiatry 49:564–569
Srinivasan L, Tirupati S (2005) Relationship between cognition and work functioning among patients with schizophrenia in an urban area of India. Psychiatr Serv 56:1423–1428. https://doi.org/10.1176/appi.ps.56.11.1423
Srivastava AK, Stitt L, Thakar M et al (2009) The abilities of improved schizophrenia patients to work and live independently in the community: a 10-year long-term outcome study from Mumbai India. Ann Gen Psychiatry 8:24. https://doi.org/10.1186/1744-859X-8-24
Suresh KK, Kumar CN, Thirthalli J et al (2012) Work functioning of schizophrenia patients in a rural south Indian community: status at 4-year follow-up. Soc Psychiatry Psychiatr Epidemiol 47:1865–1871. https://doi.org/10.1007/s00127-012-0495-8
Prasad HG, Acharya V (2014) A cross sectional study of employment pattern in patients with severe mental illness. Indian J Occup Ther 46:35–40
Bucci GA (1993) Explaining urban-rural income & wage differentials: a study using aggregate data for India. Appl Econ 25:1167–1174
Fields GS (2010) Labor market analysis for developing countries. Labour Econ 18:S16–S22
Rathod S, Pinninti N, Irfan M et al (2017) Mental health service provision in low- and middle-income countries. Health Serv Insights 10:1–7. https://doi.org/10.1177/1178632917694350
Patel V, Xiao S, Chen H et al (2016) The magnitude of and health system responses to the mental health treatment gap in adults in India and China. Lancet 388:3074–3084. https://doi.org/10.1016/S0140-6736(16)00160-4
Nagaswami V, Valecha V, Thara R et al (1985) Rehabilitation needs of schizophrenic patients: a preliminary report. Indian J Psychiatry 27:213–220
Koschorke M, Padmavati R, Kumar S et al (2014) Experiences of stigma and discrimination of people with schizophrenia in India. Soc Sci Med 123:149–159. https://doi.org/10.1016/j.socscimed.2014.10.035
Loganathan S, Murthy S (2011) Living with schizophrenia in India: gender perspectives. Transcult Psychiatry 48:569–584. https://doi.org/10.1016/j.immuni.2010.12.017.Two-stage
Tsui MCM, Tsang HWH (2017) Views of people with schizophrenia and their caregivers towards the needs for psychiatric rehabilitation in urban and rural areas of mainland China. Psychiatry Res 258:72–77. https://doi.org/10.1016/j.psychres.2017.09.052
Government of India, Ministry of Labour and Employment (2016) Report on fifth annual employment—unemployment survey (2015–2016) Volume I. Chandigarh, pp 1–360
Harvey PD, Heaton RK, Carpenter WT et al (2012) Diagnosis of schizophrenia: Consistency across information sources and stability of the condition. Schizophr Res 140:9–14. https://doi.org/10.1016/j.schres.2012.03.026
McGurk SR, Mueser KT, Xie H et al (2015) Cognitive enhancement treatment for people with mental illness who do not respond to supported employment: a randomized controlled trial. Am J Psychiatry 172:852–861. https://doi.org/10.1176/appi.ajp.2015.14030374
Mueser KT, Clark RE, Haines M et al (2004) The Hartford study of supported employment for persons with severe mental illness. J Consult Clin Psychol 72:479–490. https://doi.org/10.1037/0022-006X.72.3.479
Directorate of Census Operations, Maharashtra (2011) District census handbook Pune. Mumbai, pp 1–652
Directorate of Census Operations Maharashtra (2011) District census handbook Ahmednagar. Mumbai, pp 1–376
Government of India, Ministry of Labour and Employment (2015) National Classification of Occupations-2015 Vol—I. New Delhi, pp 1–384
Government of India, Ministry of Labour and Employment (2015) National Classification of Occupations-2015 Vol II—A. New Delhi, pp 1–587
Government of India, Ministry of Labour and Employment (2015) National Classification of Occupations-2015 Vol II—B. New Delhi, pp 1–581
Field A (2009) Discovering statistics using SPSS, 3rd edn. Sage, Los Angeles, p 388
Kumar A, Kumar S, Singh DK (2011) Rural employment diversification in India: trends, determinants and implications on poverty. Agric Econ Res Rev 24:361–372
Chadda R, Deb K (2013) Indian family systems, collectivistic society and psychotherapy. Indian J Psychiatry 55:299. https://doi.org/10.4103/0019-5545.105555
Gee LK, Jones JJ, Fariss CJ et al (2017) The paradox of weak ties in 55 countries. J Econ Behav Organ 133:362–372. https://doi.org/10.1016/j.jebo.2016.12.004
Randolph ET (1998) Social networks and schizophrenia. In: Mueser KT, Tarrier N (eds) Handbook of social functioning in schizophrenia. Allyn & Bacon, Boston, pp 238–246
Evert H, Harvey C, Trauer T, Herrman H (2003) The relationship between social networks and occupational and self-care functioning in people with psychosis. Soc Psychiatry Psychiatr Epidemiol 38:180–188. https://doi.org/10.1007/s00127-003-0617-4
Government of India, Ministry of Statistics and Programme Implementation (2019) Key indicators of social consumption in India: Health, New Delhi, p 11
Rajkumar S (2015) Mental health services in India. J Soc Soc Welf 18:41–55
Rosenheck RA, Estroff SE, Sint K et al (2017) Incomes and outcomes: social security disability benefits in first-episode psychosis. Am J Psychiatry 174:886–894. https://doi.org/10.1176/appi.ajp.2017.16111273
Metcalfe JD, Drake RE, Bond GR (2018) Economic, labor, and regulatory moderators of the effect of individual placement and support among people with severe mental illness: a systematic review and meta-analysis. Schizophr Bull 44:22–31. https://doi.org/10.1093/schbul/sbx132
Medora N (2007) Strengths and challenges in the Indian family. Marriage Fam Rev 41:165–193. https://doi.org/10.1300/J002v41n01
Russinova Z, Bloch P, Wewiorski N et al (2018) Predictors of sustained employment among individuals with serious mental illness. J Nerv Ment Dis 206:669–679. https://doi.org/10.1097/NMD.0000000000000876
Bond GR, Campbell K, Drake RE (2012) Standardizing measures in four domains of employment outcomes for individual placement and support. Psychiatr Serv 63:751–757. https://doi.org/10.1176/appi.ps.201100270
Government of India, Ministry of Statistics and Programme Implementation (2019) Annual Report: Periodic Labour Force Survey, 2017–18. New Delhi, p vi
Lewis WA (1954) Economic Development with Unlimited Supplies of Labour. Manchester Sch 1–25
Foster AD, Rosenzweig MR (2012) Is there surplus labor in rural India? SSRN Electron J. https://doi.org/10.2139/ssrn.1696026
Mueser KT, Salyers MP, Mueser PR (2001) A prospective analysis of work in schizophrenia. Schizophr Bull 27:281–296. https://doi.org/10.1093/oxfordjournals.schbul.a006874
McQuilken M, Zahniser JH, Novak J et al (2003) The work project survey: consumer perspective on work. J Vocat Rehabil 18:59–68
Drake RE, Bond GR, Goldman HH et al (2016) Individual placement and support services boost employment for people with serious mental illnesses, but funding is lacking. Health Aff 35:1098–1105. https://doi.org/10.1377/hlthaff.2016.0001
Jaleel F, Nirmala BP, Thirthalli J (2014) Supported employment initiative for persons with mental illness in Indian setting: an expanded case report. Asian J Psychiatr 9:91–92. https://doi.org/10.1016/j.ajp.2013.10.015
Mueser KT, Meyer PS, Penn DL et al (2006) The illness management and recovery program: rationale, development, and preliminary findings. Schizophr Bull. https://doi.org/10.1093/schbul/sbl022
McFarlane WR, Dushay RA, Deakins SM et al (2000) Employment outcomes in family-aided assertive community treatment. Am J Orthopsychiatry 70:203–214
Acknowledgements
We are grateful to the following people for their help and contributions to various aspects of conducting the research project:
India: Kedar Deshmukh, Dr. Manjiri Dixit, Dr. Kaustubh Joag, Suchitra Joshi, Dr. Amruta Karande-Patil, Dr. Himani Kulkarni, Dr. Sameer Kulkarni, Chitra Lele, Pranita Pathak, Dr. Shirisha Sathe, staff of Manasdeep Psychiatric and Deaddiction Center, Ahmednagar and Poona Hospital and Research Center, Pune, and all the study participants.
US: Drs. Gary Bond, Robert Drake, Matthew Kurtz, Uma Millner, Peter R. Mueser, E. Sally Rogers, and staff at the Center for Psychiatric Rehabilitation, Boston University.
Funding
This research was supported by the Dudley Allen Sargent Research Fund at Boston University to C. Khare.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
The study was conducted in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. The study protocol was approved by the Institutional Review Board of Boston University, USA. All participants gave informed consent prior to their inclusion in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Khare, C., Mueser, K.T., Fulford, D. et al. Employment functioning in people with severe mental illnesses living in urban vs. rural areas in India. Soc Psychiatry Psychiatr Epidemiol 55, 1593–1606 (2020). https://doi.org/10.1007/s00127-020-01901-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-020-01901-0