Abstract
Objective
To measure renal blood flow (RBF) and renal function during recovery from experimental septic acute kidney injury (AKI).
Design
Controlled experimental study.
Subjects
Nine merino ewes.
Setting
University physiology laboratory.
Intervention
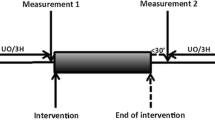
We recorded systemic and renal hemodynamics during a 96-h observation period (control) via implanted transit-time flow probes. We then compared this period with 96 h of septic AKI (48 h of Escherichia coli infusion) and subsequent recovery (48 h of observation after stopping E. coli).
Measurements and results
Compared with the control period, E. coli infusion induced hyperdynamic sepsis (increased cardiac output and decreased blood pressure) and septic AKI (serum creatinine 65.4 ± 8.7 vs. 139.9 ± 33.0 μmol/l; creatinine clearance 73.8 ± 12.2 vs. 40.2 ± 17.2 ml/min; p < 0.05) with a mortality of 22%. RBF increased (278.8 ± 33.9 vs. 547.9 ± 124.8 ml/min; p < 0.05) as did renal vascular conductance (RVC). During recovery, we observed a decrease in RVC and RBF with all values returning to control levels. Indices of tubular function [fractional excretion of sodium (FENa) and urea (FEUn) and urinary sodium concentration (UNa)], which had been affected by sepsis, returned to control values after 18 h of recovery, as did serum creatinine.
Conclusions
Infusion of E. coli induced a hyperdynamic circulatory state with hyperemic AKI. Recovery was associated with relative renal vasoconstriction and reduction in RBF and RVC back to control levels. Indices of tubular function normalized more rapidly than changes in RBF.


Similar content being viewed by others
References
Uchino S, Kellum JA, Bellomo R, Doig GS, Morimatsu H, Morgera S, Schetz M, Tan I, Bouman C, Macedo E, Gibney N, Tolwani A, Ronco C (2005) Acute renal failure in critically ill patients: a multinational, multicenter study. Jama 294:813–818
Uchino S, Doig GS, Bellomo R, Morimatsu H, Morgera S, Schetz M, Tan I, Bouman C, Nacedo E, Gibney N, Tolwani A, Ronco C, Kellum JA (2004) Diuretics and mortality in acute renal failure. Crit Care Med 32:1669–1677
Schrier RW, Wang W (2004) Acute renal failure and sepsis. N Engl J Med 351:159–169
Lameire N, Van Biesen W, Vanholder R (2005) Acute renal failure. Lancet 365:417–430
Brenner M, Schaer GL, Mallory DL, Suffredini AF, Parrillo JE (1990) Detection of renal blood flow abnormalities in septic and critically ill patients using a newly designed indwelling thermodilution renal vein catheter. Chest 98:170–179
Lucas CE, Rector FE, Werner M, Rosenberg IK (1973) Altered renal homeostasis with acute sepsis. Clinical significance. Arch Surg 106:444–449
Rector F, Goyal S, Rosenberg IK, Lucas CE (1973) Sepsis: a mechanism for vasodilatation in the kidney. Ann Surg 178:222–226
Langenberg C, Bellomo R, May C, Wan L, Egi M, Morgera S (2005) Renal blood flow in sepsis. Crit Care 9:R363–R374
Langenberg C, Bellomo R, May CN, Egi M, Wan L, Morgera S (2006) Renal vascular resistance in sepsis. Nephron Physiol 104:1–11
Langenberg C, Wan L, Egi M, May CN, Bellomo R (2006) Renal blood flow in experimental septic acute renal failure. Kidney Int 69:1996–2002
Parker MM, Shelhamer JH, Natanson C, Alling DW, Parrillo JE (1987) Serial cardiovascular variables in survivors and nonsurvivors of human septic shock: heart rate as an early predictor of prognosis. Crit Care Med 15:923–929
Nagai J, Takano M (2004) Molecular aspects of renal handling of aminoglycosides and strategies for preventing the nephrotoxicity. Drug Metab Pharmacokinet 19:159–170
Miller TR, Anderson RJ, Linas SL, Henrich WL, Berns AS, Gabow PA, Schrier RW (1978) Urinary diagnostic indices in acute renal failure: a prospective study. Ann Intern Med 89:47–50
Vaz AJ (1983) Low fractional excretion of urine sodium in acute renal failure due to sepsis. Arch Intern Med 143:738–739
Espinel CH (1976) The FENa test. Use in the differential diagnosis of acute renal failure. Jama 236:579–581
Carvounis CP, Nisar S, Guro-Razuman S (2002) Significance of the fractional excretion of urea in the differential diagnosis of acute renal failure. Kidney Int 62:2223–2229
Acknowledgements
The study was supported by a grant from the Australian and New Zealand College of Anaesthetists. Christoph Langenberg was funded by the Else Kröner–Fresenius Foundation (Germany).
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is discussed in the editorial available at: http://dx.doi.org/10.1007/s00134-007-0735-7.
Rights and permissions
About this article
Cite this article
Langenberg, C., Wan, L., Egi, M. et al. Renal blood flow and function during recovery from experimental septic acute kidney injury. Intensive Care Med 33, 1614–1618 (2007). https://doi.org/10.1007/s00134-007-0734-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-007-0734-8