Abstract
Purpose
Terlipressin bolus infusion may contribute to overshooting increases in systemic vascular resistance with concomitant reductions in systemic blood flow and oxygen delivery. Whether these effects negatively impact on microcirculatory perfusion is still not known. The objective of the present study was, therefore, to elucidate the effects of a single terlipressin bolus dose of 0.5 mg on microcirculatory perfusion in patients with catecholamine-dependent septic shock.
Methods
This prospective clinical cohort study was performed in a multidisciplinary intensive care unit at a university hospital. We enrolled 20 patients suffering from catecholamine-dependent septic shock. After restoring normovolaemia, norepinephrine (NE) was titrated to maintain mean arterial pressure (MAP) between 65 and 75 mmHg. Thereafter, all patients received a bolus infusion of 0.5 mg terlipressin, and NE was adjusted to maintain MAP between the threshold values. Sublingual microcirculatory blood flow of small vessels was assessed by sidestream dark-field imaging. All measurements, including data from right heart catheterization and NE requirements, were obtained at baseline and 6 h after terlipressin administration.
Results
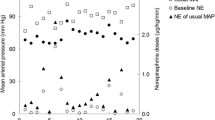
Terlipressin stabilized haemodynamics and, at the same time, decreased NE requirements (0.42±0.67 vs. 0.74±0.73 μg/kg per minute, p < 0.05). Whereas the pH and arterial lactate concentrations remained unchanged, microcirculatory flow index of small vessels had increased at the end of the 6-h study period (2.6±0.6 vs. 2.0±0.5 units, p < 0.05).
Conclusion
In fluid-resuscitated patients with septic shock (with a MAP between 65 and 75 mmHg), a bolus infusion of 0.5 mg terlipressin was effective in reducing NE requirements without worsening microcirculatory blood flow. Randomized clinical trials are now warranted to verify these preliminary results.

Similar content being viewed by others
References
Lange M, Ertmer C, Westphal M (2008) Vasopressin vs terlipressin in the treatment of cardiovascular failure in sepsis. Intensive Care Med 34:821–832
Morelli A, Ertmer C, Pietropaoli P, Westphal M (2009) Terlipressin, a promising vasoactive agent in the hemodynamic support of septic shock. Expert Opin Pharmacother 10:2569–2575
Scharte M, Meyer J, Van Aken H, Bone HG (2001) Hemodynamic effects of terlipressin (a synthetic analog of vasopressin) in healthy and endotoxemic sheep. Crit Care Med 29:1756–1760
De Backer D, Hollenberg S, Boerma C, Goedhart P, Büchele G, Ospina-Tascon G, Dobbe I, Ince C (2007) How to evaluate the microcirculation? Report of a round table conference. Crit Care 11:R101–R111
Dellinger RP, Levy MM, Carlet JM, Bion J, Parker MM, Jaeschke R, Reinhart K, Angus DC, Brun-Buisson C, Beale R, Calandra T, Dhainaut JF, Gerlach H, Harvey M, Marini JJ, Marshall J, Ranieri M, Ramsay G, Sevransky J, Thompson BT, Townsend S, Vender JS, Zimmerman JL, Vincent JL (2008) Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock. Intensive Care Med 34:17–60
Russell JA, Walley KR, Singer J, Gordon AC, Hébert PC, Cooper DJ, Holmes CL, Mehta S, Granton JT, Storms MM, Cook DJ, Presneill JJ, Ayers D; VASST Investigators (2008) Vasopressin versus norepinephrine infusion in patients with septic shock. N Engl J Med 358:877–887
Dubois MJ, De Backer D, Creteur J, Anane S, Vincent JL (2003) Effect of vasopressin on sublingual microcirculation in a patient with distributive shock. Intensive Care Med 29:1020–1023
Boerma EC, van Der Voort PHJ, Ince C (2005) Sublingual microcirculatory flow is impaired by the vasopressin-analogue terlipressin in a patient with catecholamine-resistant septic shock. Acta Anaesthesiol Scand 49:1387–1390
Sakr Y, Dubois MJ, De Backer D, Creteur J, Vincent JL (2004) Persistent microcirculatory alterations are associated with organ failure and death in patients with septic shock. Crit Care Med 32:1825–1831
De Backer D, Ospina-Tascon G, Salgado D, Favory R, Creteur J, Vincent JL (2010) Monitoring the microcirculation in the critically ill patient: current methods and future approaches. Intensive Care Med 36:1813–1825
Trzeciak S, Dellinger RP, Parrillo JE, Guglielmi M, Bajaj J, Abate NL, Arnold RC, Colilla S, Zanotti S, Hollenberg SM; Microcirculatory Alterations in Resuscitation and Shock Investigators (2007) Early microcirculatory perfusion derangements in patients with severe sepsis and septic shock: relationship to hemodynamics, oxygen transport, and survival. Ann Emerg Med 49:88–98
Ryckwaert F, Virsolvy A, Fort A, Murat B, Richard S, Guillon G, Colson PH (2009) Terlipressin, a pro-vasopressin drug exhibits direct vasoconstrictor properties: consequences on heart perfusion and performance. Crit Care Med 37:876–881
Rehberg S, Ertmer C, Köhler G, Spiegel HU, Morelli A, Lange M, Moll K, Schlack K, Van Aken H, Su F, Vincent JL, Westphal M (2009) Role of arginine vasopressin and terlipressin as first-line vasopressor agents in fulminant ovine septic shock. Intensive Care Med 35:1286–1296
Morelli A, Ertmer C, Rehberg S, Lange M, Orecchioni A, Cecchini V, Bachetoni A, D’Alessandro M, Van Aken H, Pietropaoli P, Westphal M (2009) Continuous terlipressin versus vasopressin infusion in septic shock (TERLIVAP): a randomized, controlled pilot study. Crit Care 13:R130
Dubin A, Pozo MO, Casabella CA, Pálizas F Jr, Murias G, Moseinco MC, Kanoore Edul VS, Pálizas F, Estenssoro E, Ince C (2009) Increasing arterial blood pressure with norepinephrine does not improve microcirculatory blood flow: a prospective study. Crit Care 13:R92
Jhanji S, Stirling S, Patel N, Hinds CJ, Pearse RM (2009) The effect of increasing doses of norepinephrine on tissue oxygenation and microvascular flow in patients with septic shock. Crit Care Med 37:1961–1966
De Backer D, Ortiz JA, Salgado D (2010) Coupling microcirculation to systemic hemodynamics. Curr Opin Crit Care 16:250–254
Trzeciak S, McCoy JV, Phillip Dellinger R, Arnold RC, Rizzuto M, Abate NL, Shapiro NI, Parrillo JE, Hollenberg SM; Microcirculatory Alterations in Resuscitation and Shock (MARS) investigators (2008) Early increases in microcirculatory perfusion during protocol-directed resuscitation are associated with reduced multi-organ failure at 24 h in patients with sepsis. Intensive Care Med 34:2210–2217
Gattinoni L, Brazzi L, Pelosi P, Latini R, Tognoni G, Pesenti A, Fumagalli R (1995) A trial of goal-oriented hemodynamic therapy in critically ill patients. SvO2 Collaborative Group. N Engl J Med 333:1025–1032
Trzeciak S, Cinel I, Phillip Dellinger R, Shapiro NI, Arnold RC, Parrillo JE, Hollenberg SM; Microcirculatory Alterations in Resuscitation and Shock (MARS) Investigators (2008) Resuscitating the microcirculation in sepsis: the central role of nitric oxide, emerging concepts for novel therapies, and challenges for clinical trials. Acad Emerg Med 15:399–413
Acknowledgments
This study was funded by an independent department research grant.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Morelli, A., Donati, A., Ertmer, C. et al. Short-term effects of terlipressin bolus infusion on sublingual microcirculatory blood flow during septic shock. Intensive Care Med 37, 963–969 (2011). https://doi.org/10.1007/s00134-011-2148-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-011-2148-x