Abstract
Purpose
This pilot study assessed the independent and incremental value of 68Ga-V/Q PET/CT as compared with CT pulmonary angiography (CTPA) for the management of cancer patients with suspected acute pulmonary embolism (PE).
Methods
All 24 cancer patients with suspected acute PE prospectively recruited underwent both 68Ga-V/Q PET/CT and CTPA within 24 h. PET/CT was acquired after inhalation of Galligas prepared using a Technegas generator and administration of 68Ga-macroaggregated albumin. Initially, PET/CT and CTPA scans were read independently with the reader blinded to the results of the other imaging study. CTPA and PET/CT were then coregistered and reviewed by consensus between a radiologist and nuclear medicine physician. The therapeutic management was established by the managing physician based on all available data.
Results
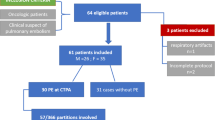
The diagnostic conclusion was concordantly negative in 18 patients (75%). Of the six discordant diagnoses on independent reading, combined interpretation of V/Q PET/CTPA enabled a consensus conclusion in two patients, excluding PE in one and confirming PE in the other, similar to the initial diagnostic conclusion of the V/Q PET/CT. Of the remaining four patients, three had a single subsegmental thrombus on CTPA but a negative V/Q PET/CT scan, and two of these did not receive long-term anticoagulation and did not have a venous thromboembolic event during a 3-year follow-up period. The third patient, along with a patient with a positive V/Q PET/CT scan but a negative CTPA scan, presented with acute complications preventing any conclusions with regard to the appropriateness of the V/Q PET/CT results in the management of PE. Overall, V/Q PET had an impact on management in four patients (17%).
Conclusion
In this pilot study, we demonstrated the feasibility and potential utility of V/Q PET/CT for the management of patients with suspected PE. V/Q PET/CT may be of particular relevance in patients with equivocal findings or isolated subsegmental findings on CTPA, adding further discriminatory information to allow important decision-making regarding the use or withholding of anticoagulation. Given the other advantages of V/Q PET/CT (reduced acquisition time, low radiation dose), and with the increasing availability of 68Ga generators, PET/CT is a potential replacement for V/Q SPECT/CT imaging.




Similar content being viewed by others
References
Barritt DW, Jordan SC. Anticoagulant drugs in the treatment of pulmonary embolism. A controlled trial. Lancet. 1960;1(7138):1309–12.
Carrier M, Le Gal G, Wells PS, Rodger MA. Systematic review: case-fatality rates of recurrent venous thromboembolism and major bleeding events among patients treated for venous thromboembolism. Ann Intern Med. 2010;152(9):578–89. https://doi.org/10.7326/0003-4819-152-9-201005040-00008.
Kuderer NM, Ortel TL, Francis CW. Impact of venous thromboembolism and anticoagulation on cancer and cancer survival. J Clin Oncol. 2009;27(29):4902–11. https://doi.org/10.1200/JCO.2009.22.4584.
Chew HK, Wun T, Harvey D, Zhou H, White RH. Incidence of venous thromboembolism and its effect on survival among patients with common cancers. Arch Intern Med. 2006;166(4):458–64. https://doi.org/10.1001/archinte.166.4.458.
Prandoni P, Lensing AW, Piccioli A, Bernardi E, Simioni P, Girolami B, et al. Recurrent venous thromboembolism and bleeding complications during anticoagulant treatment in patients with cancer and venous thrombosis. Blood. 2002;100(10):3484–8. https://doi.org/10.1182/blood-2002-01-0108.
Douketis JD, Crowther MA, Foster GA, Ginsberg JS. Does the location of thrombosis determine the risk of disease recurrence in patients with proximal deep vein thrombosis? Am J Med. 2001;110(7):515–9.
Anderson DR, Kahn SR, Rodger MA, Kovacs MJ, Morris T, Hirsch A, et al. Computed tomographic pulmonary angiography vs ventilation-perfusion lung scanning in patients with suspected pulmonary embolism: a randomized controlled trial. JAMA. 2007;298(23):2743–53. https://doi.org/10.1001/jama.298.23.2743.
Wiener RS, Schwartz LM, Woloshin S. Time trends in pulmonary embolism in the United States: evidence of overdiagnosis. Arch Intern Med. 2011;171(9):831–7. https://doi.org/10.1001/archinternmed.2011.178.
Wiener RS, Schwartz LM, Woloshin S. When a test is too good: how CT pulmonary angiograms find pulmonary emboli that do not need to be found. BMJ. 2013;347:f3368. https://doi.org/10.1136/bmj.f3368.
Sheh SH, Bellin E, Freeman KD, Haramati LB. Pulmonary embolism diagnosis and mortality with pulmonary CT angiography versus ventilation-perfusion scintigraphy: evidence of overdiagnosis with CT? AJR Am J Roentgenol. 2012;198(6):1340–5. https://doi.org/10.2214/AJR.11.6426.
Kearon C, Akl EA, Ornelas J, Blaivas A, Jimenez D, Bounameaux H, et al. Antithrombotic therapy for VTE disease: CHEST guideline and expert panel report. Chest. 2016;149(2):315–52. https://doi.org/10.1016/j.chest.2015.11.026.
Salaun PY, Couturaud F, Le Duc-Pennec A, Lacut K, Le Roux PY, Guillo P, et al. Noninvasive diagnosis of pulmonary embolism. Chest. 2011;139(6):1294–8. https://doi.org/10.1378/chest.10-1209.
Wells PS. Integrated strategies for the diagnosis of venous thromboembolism. J Thromb Haemost. 2007;5(Suppl 1):41–50. https://doi.org/10.1111/j.1538-7836.2007.02493.x.
Le Roux PY, Robin P, Delluc A, Abgral R, Le Duc-Pennec A, Nowak E, et al. V/Q SPECT interpretation for pulmonary embolism diagnosis: which criteria to use? J Nucl Med. 2013;54(7):1077–81. https://doi.org/10.2967/jnumed.112.113639.
Le Duc-Pennec A, Le Roux PY, Cornily JC, Jaffrelot M, Delluc A, de Saint-Martin L, et al. Diagnostic accuracy of single-photon emission tomography ventilation/perfusion lung scan in the diagnosis of pulmonary embolism. Chest. 2012;141(2):381–7. https://doi.org/10.1378/chest.11-0090.
Le Roux PY, Palard X, Robin P, Delluc A, Abgral R, Querellou S, et al. Safety of ventilation/perfusion single photon emission computed tomography for pulmonary embolism diagnosis. Eur J Nucl Med Mol Imaging. 2014;41(10):1957–64. https://doi.org/10.1007/s00259-014-2763-1.
Le Roux PY, Robin P, Delluc A, Abgral R, Palard X, Tissot V, et al. Additional value of combining low-dose computed tomography to V/Q SPECT on a hybrid SPECT-CT camera for pulmonary embolism diagnosis. Nucl Med Commun. 2015;36(9):922–30. https://doi.org/10.1097/MNM.0000000000000351.
Gutte H, Mortensen J, Jensen CV, Johnbeck CB, von der Recke P, Petersen CL, et al. Detection of pulmonary embolism with combined ventilation-perfusion SPECT and low-dose CT: head-to-head comparison with multidetector CT angiography. J Nucl Med. 2009;50(12):1987–92. https://doi.org/10.2967/jnumed.108.061606.
Hicks RJ, Hofman MS. Is there still a role for SPECT-CT in oncology in the PET-CT era? Nat Rev Clin Oncol. 2012;9(12):712–20. https://doi.org/10.1038/nrclinonc.2012.188.
Oehme L, Zophel K, Golgor E, Andreeff M, Wunderlich G, Brogsitter C, et al. Quantitative analysis of regional lung ventilation and perfusion PET with (68)Ga-labelled tracers. Nucl Med Commun. 2014;35(5):501–10. https://doi.org/10.1097/MNM.0000000000000084.
Le Roux PY, Robin P, Salaun PY. New developments and future challenges of nuclear medicine and molecular imaging for pulmonary embolism. Thromb Res. 2018;163:236–41. https://doi.org/10.1016/j.thromres.2017.06.031.
Hofman MS, Lau WF, Hicks RJ. Somatostatin receptor imaging with 68Ga DOTATATE PET/CT: clinical utility, normal patterns, pearls, and pitfalls in interpretation. Radiographics. 2015;35(2):500–16. https://doi.org/10.1148/rg.352140164.
Hofman MS, Beauregard JM, Barber TW, Neels OC, Eu P, Hicks RJ. 68Ga PET/CT ventilation-perfusion imaging for pulmonary embolism: a pilot study with comparison to conventional scintigraphy. J Nucl Med. 2011;52(10):1513–9. https://doi.org/10.2967/jnumed.111.093344.
Le Roux PY, Hicks RJ, Siva S, Hofman MS. PET/CT lung ventilation and perfusion scanning using Galligas and gallium-68-MAA. Semin Nucl Med. 2019;49(1):71–81. https://doi.org/10.1053/j.semnuclmed.2018.10.013.
Le Roux PY, Siva S, Steinfort DP, Callahan J, Eu P, Irving LB, et al. Correlation of 68Ga ventilation-perfusion PET/CT with pulmonary function test indices for assessing lung function. J Nucl Med. 2015;56(11):1718–23. https://doi.org/10.2967/jnumed.115.162586.
Le Roux PY, Siva S, Callahan J, Claudic Y, Bourhis D, Steinfort DP, et al. Automatic delineation of functional lung volumes with (68)Ga-ventilation/perfusion PET/CT. EJNMMI Res. 2017;7(1):82. https://doi.org/10.1186/s13550-017-0332-x.
Hardcastle N, Hofman MS, Hicks RJ, Callahan J, Kron T, MacManus MP, et al. Accuracy and utility of deformable image registration in (68)Ga 4D PET/CT assessment of pulmonary perfusion changes during and after lung radiation therapy. Int J Radiat Oncol Biol Phys. 2015;93(1):196–204. https://doi.org/10.1016/j.ijrobp.2015.05.011.
Siva S, Thomas R, Callahan J, Hardcastle N, Pham D, Kron T, et al. High-resolution pulmonary ventilation and perfusion PET/CT allows for functionally adapted intensity modulated radiotherapy in lung cancer. Radiother Oncol. 2015;115(2):157–62. https://doi.org/10.1016/j.radonc.2015.04.013.
Siva S, Hardcastle N, Kron T, Bressel M, Callahan J, MacManus MP, et al. Ventilation/perfusion positron emission tomography-based assessment of radiation injury to lung. Int J Radiat Oncol Biol Phys. 2015;93(2):408–17. https://doi.org/10.1016/j.ijrobp.2015.06.005.
Leong P, Le Roux PY, Callahan J, Siva S, Hofman MS, Steinfort DP. Reduced ventilation-perfusion (V/Q) mismatch following endobronchial valve insertion demonstrated by gallium-68 V/Q photon emission tomography/computed tomography. Respirol Case Rep. 2017;5(5):e00253. https://doi.org/10.1002/rcr2.253.
Le Roux PY, Leong TL, Barnett SA, Hicks RJ, Callahan J, Eu P, et al. Gallium-68 perfusion positron emission tomography/computed tomography to assess pulmonary function in lung cancer patients undergoing surgery. Cancer Imaging. 2016;16(1):24. https://doi.org/10.1186/s40644-016-0081-5.
Callahan J, Hofman MS, Siva S, Kron T, Schneider ME, Binns D, et al. High-resolution imaging of pulmonary ventilation and perfusion with 68Ga-VQ respiratory gated (4-D) PET/CT. Eur J Nucl Med Mol Imaging. 2014;41(2):343–9. https://doi.org/10.1007/s00259-013-2607-4.
Bajc M, Neilly JB, Miniati M, Schuemichen C, Meignan M, Jonson B. EANM guidelines for ventilation/perfusion scintigraphy: part 1. Pulmonary imaging with ventilation/perfusion single photon emission tomography. Eur J Nucl Med Mol Imaging. 2009;36(8):1356–70. https://doi.org/10.1007/s00259-009-1170-5.
Le Roux PY, Pelletier-Galarneau M, De Laroche R, Hofman MS, Zuckier LS, Roach P, et al. Pulmonary scintigraphy for the diagnosis of acute pulmonary embolism: a survey of current practices in Australia, Canada, and France. J Nucl Med. 2015;56(8):1212–7. https://doi.org/10.2967/jnumed.115.157743.
Le Gal G, Righini M, Roy PM, Sanchez O, Aujesky D, Bounameaux H, et al. Prediction of pulmonary embolism in the emergency department: the revised Geneva score. Ann Intern Med. 2006;144(3):165–71.
Burge AJ, Freeman KD, Klapper PJ, Haramati LB. Increased diagnosis of pulmonary embolism without a corresponding decline in mortality during the CT era. Clin Radiol. 2008;63(4):381–6. https://doi.org/10.1016/j.crad.2007.10.004.
Ghanima W, Nielssen BE, Holmen LO, Witwit A, Al-Ashtari A, Sandset PM. Multidetector computed tomography (MDCT) in the diagnosis of pulmonary embolism: interobserver agreement among radiologists with varied levels of experience. Acta Radiol. 2007;48(2):165–70. https://doi.org/10.1080/02841850601100859.
Di Nisio M, Lee AY, Carrier M, Liebman HA, Khorana AA, Subcommittee on Haemostasis and Malignancy. Diagnosis and treatment of incidental venous thromboembolism in cancer patients: guidance from the SSC of the ISTH. J Thromb Haemost. 2015;13(5):880–3. https://doi.org/10.1111/jth.12883.
Konstantinides SV, Torbicki A, Agnelli G, Danchin N, Fitzmaurice D, Galie N, et al. 2014 ESC guidelines on the diagnosis and management of acute pulmonary embolism. Eur Heart J. 2014;35(43):3033–80. https://doi.org/10.1093/eurheartj/ehu283.
Perrier A, Desmarais S, Miron MJ, de Moerloose P, Lepage R, Slosman D, et al. Non-invasive diagnosis of venous thromboembolism in outpatients. Lancet. 1999;353(9148):190–5. https://doi.org/10.1016/S0140-6736(98)05248-9.
Wells PS, Ginsberg JS, Anderson DR, Kearon C, Gent M, Turpie AG, et al. Use of a clinical model for safe management of patients with suspected pulmonary embolism. Ann Intern Med. 1998;129(12):997–1005.
Leblanc M, Leveillee F, Turcotte E. Prospective evaluation of the negative predictive value of V/Q SPECT using 99mTc-Technegas. Nucl Med Commun. 2007;28(8):667–72. https://doi.org/10.1097/MNM.0b013e32827a8e99.
Truffault B, Robin P, Tromeur C, Le Duc Pennec A, Abgral R, Bourhis D, et al. Time trend analysis of pulmonary embolism diagnosis with single-photon emission computed tomography ventilation/perfusion imaging. Nucl Med Commun. 2019. https://doi.org/10.1097/MNM.0000000000000990.
Hofman MS, Hicks RJ, Maurer T, Eiber M. Prostate-specific membrane antigen PET: clinical utility in prostate cancer, normal patterns, pearls, and pitfalls. Radiographics. 2018;38(1):200–17. https://doi.org/10.1148/rg.2018170108.
Sorensen HT, Mellemkjaer L, Steffensen FH, Olsen JH, Nielsen GL. The risk of a diagnosis of cancer after primary deep venous thrombosis or pulmonary embolism. N Engl J Med. 1998;338(17):1169–73. https://doi.org/10.1056/NEJM199804233381701.
Le Gal G, Le Roux PY. How to assess quality of primary research studies in the medical literature? Semin Nucl Med. 2019;49(2):115–20. https://doi.org/10.1053/j.semnuclmed.2018.11.007.
Acknowledgments
We acknowledge the doctors, radiopharmacists, technologists, nurses and medical physicists at the Peter MacCallum Cancer Team who enabled this research to occur.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
None.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the principles of the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. The protocol was approved by the Ethics Committee of our institution (14/117). The study was registered with the Australian New Zealand Clinical Trial Registry (ACTRN12614001170617).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Le Roux, PY., Iravani, A., Callahan, J. et al. Independent and incremental value of ventilation/perfusion PET/CT and CT pulmonary angiography for pulmonary embolism diagnosis: results of the PECAN pilot study. Eur J Nucl Med Mol Imaging 46, 1596–1604 (2019). https://doi.org/10.1007/s00259-019-04338-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-019-04338-z