Abstract
Purpose
Electroporation-based therapies deliver brief electric pulses into a targeted volume to destabilize cellular membranes. Nonthermal irreversible electroporation (IRE) provides focal ablation with effects dependent on the electric field distribution, which changes in heterogeneous environments. It should be determined if highly conductive metallic implants in targeted regions, such as radiotherapy brachytherapy seeds in prostate tissue, will alter treatment outcomes. Theoretical and experimental models determine the impact of prostate brachytherapy seeds on IRE treatments.
Materials and Methods
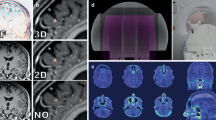
This study delivered IRE pulses in nonanimal, as well as in ex vivo and in vivo tissue, with and in the absence of expired radiotherapy seeds. Electrical current was measured and lesion dimensions were examined macroscopically and with magnetic resonance imaging. Finite-element treatment simulations predicted the effects of brachytherapy seeds in the targeted region on electrical current, electric field, and temperature distributions.
Results
There was no significant difference in electrical behavior in tissue containing a grid of expired radiotherapy seeds relative to those without seeds for nonanimal, ex vivo, and in vivo experiments (all p > 0.1). Numerical simulations predict no significant alteration of electric field or thermal effects (all p > 0.1). Histology showed cellular necrosis in the region near the electrodes and seeds within the ablation region; however, there were no seeds beyond the ablation margins.
Conclusion
This study suggests that electroporation therapies can be implemented in regions containing small metallic implants without significant changes to electrical and thermal effects relative to use in tissue without the implants. This supports the ability to use IRE as a salvage therapy option for brachytherapy.





Similar content being viewed by others
References
Al-Sakere B, Andre F, Bernat C et al (2007) Tumor ablation with irreversible electroporation. PLoS One 2(11):e1135
Appelbaum L, Ben-David E, Sosna J, Nissenbaum Y, Goldberg SN (2012) US findings after irreversible electroporation ablation: radiologic-pathologic correlation. Radiology 262(1):117–125
Ball C, Thomson KR, Kavnoudias H (2010) Irreversible electroporation: a new challenge in “out of operating theater” anesthesia. Anesth Analg 110(5):1305–1309
Boukaram C, Hannoun-Levi J-M (2010) Management of prostate cancer recurrence after definitive radiation therapy. Cancer Treat Rev 36(2):91–100
Carrara N (2007) Dielectric properties of body tissues. Italian National Research Council, Institute for Applied Physics, Florence
Davalos R, Mir L, Rubinsky B (2005) Tissue ablation with irreversible electroporation. Ann Biomed Eng 33(2):223–231
Edd JF, Horowitz L, Davalos RV, Mir LM, Rubinsky B (2006) In vivo results of a new focal tissue ablation technique: irreversible electroporation. IEEE Trans Biomed Eng 53(5):1409–1415
Finley D, Belldegrun A (2011) Salvage cryotherapy for radiation-recurrent prostate cancer: outcomes and complications. Curr Urol Rep 12(3):209–215
Foster KR, Schwan HP (1989) Dielectric properties of tissues and biological materials: a critical review. Crit Rev Biomed Eng 17(1):25–104
Gabriel S, Lau RW, Gabriel C (1996) The dielectric properties of biological tissues: II. Measurements in the frequency range 10 Hz to 20 GHz. Phys Med Biol 41(11):2251–2269
Garcia PA, Pancotto T, Rossmeisl JH Jr et al (2011) Non-thermal irreversible electroporation (N-TIRE) and adjuvant fractionated radiotherapeutic multimodal therapy for intracranial malignant glioma in a canine patient. Technol Cancer Res Treat 10(1):73–83
Garcia PA, Rossmeisl JH Jr, Neal RE 2nd, Ellis TL, Davalos RV (2011) A parametric study delineating irreversible electroporation from thermal damage based on a minimally invasive intracranial procedure. Biomed Eng Online 10(1):34
Hjouj M, Rubinsky B (2010) Magnetic resonance imaging characteristics of nonthermal irreversible electroporation in vegetable tissue. J Membr Biol 236(1):137–146
Ivorra A, Mir LM, Rubinsky B (2009) Electric field redistribution due to conductivity changes during tissue electroporation: experiments with a simple vegetal model. Springer, Berlin, pp 59–62
Ivorra A, Rubinsky B (2007) In vivo electrical impedance measurements during and after electroporation of rat liver. Bioelectrochemistry 70(2):287–295 Epub 2006 Oct 2021
Kimura M, Mouraviev V, Tsivian M, Mayes JM, Satoh T, Polascik TJ (2010) Current salvage methods for recurrent prostate cancer after failure of primary radiotherapy. BJU Int 105(2):191–201
Miklavcic D, Semrov D, Mekid H, Mir LM (2000) A validated model of in vivo electric field distribution in tissues for electrochemotherapy and for DNA electrotransfer for gene therapy. Biochim Biophys Acta 1523(1):73–83
Mir LM, Orlowski S, Belehradek JJ, Teissie J, Rols MP (1995) Biomedical applications of electric pulses with special emphasis on antitumor electrochemotherapy. Bioelectrochem Bioenerg 38:203–207
Narayanan G, Froud T, Lo K, Barbery KJ, Perez-Rojas E, Yrizarry J (2012) Pain analysis in patients with hepatocellular carcinoma: irreversible electroporation versus radiofrequency ablation-initial observations. Cardiovasc Intervent Radiol 30:30
Neal RE 2nd, Davalos RV (2009) The feasibility of irreversible electroporation for the treatment of breast cancer and other heterogeneous systems. Ann Biomed Eng 37(12):2615–2625
Neal RE 2nd, Garcia PA, Robertson JL, Davalos RV (2012) Experimental characterization and numerical modeling of tissue electrical conductivity during pulsed electric fields for irreversible electroporation treatment planning. IEEE Trans Biomed Eng 59(4):1076–1085 Epub 2012 Jan 1076
Neal RE 2nd, Rossmeisl JH Jr, Garcia PA, Lanz OI, Henao-Guerrero N, Davalos RV (2011) Successful treatment of a large soft tissue sarcoma with irreversible electroporation. J Clin Oncol 29(13):e372–e377
Neal RE 2nd, Singh R, Hatcher HC, Kock ND, Torti SV, Davalos RV (2010) Treatment of breast cancer through the application of irreversible electroporation using a novel minimally invasive single needle electrode. Breast Cancer Res Treat 123(1):295–301
Neumann E, Schaefer-Ridder M, Wang Y, Hofschneider PH (1982) Gene transfer into mouse lyoma cells by electroporation in high electric fields. EMBO J 1(7):841–845
Onik G, Mikus P, Rubinsky B (2007) Irreversible electroporation: implications for prostate ablation. Technol Cancer Res Treat 6(4):295–300
Potters L, Morgenstern C, Calugaru E et al (2008) 12-year outcomes following permanent prostate brachytherapy in patients with clinically localized prostate cancer. J Urol 179(5):S20–S24
Rabin Y, Stahovich TF (2003) Cryoheater as a means of cryosurgery control. Phys Med Biol 48(5):619–632
Neal RE II, Cheung W, Kavnoudias H, Thomson KR (2012) Spectrum of imaging and characteristics for liver tumors treated with irreversible electroporation. J Biomed Sci Eng 5(12A):813–818
Thomson KR, Cheung W, Ellis SJ et al (2011) Investigation of the safety of irreversible electroporation in humans. J Vasc Interv Radiol 22(5):611–621
Acknowledgments
This work is supported by the Flack Trustees, NSF CAREER Award CBET-1055913, and the Whitaker International Program. The authors thank Anatoly Dritschilo for advising experimental analysis as well as Victoria Earl and the radiology staff of The Alfred Hospital for assistance.
Conflict of interest
R. E. Neal and R. V. Davalos hold pending patents and are recipients of royalty payments from Angiodynamics, Inc., for unrelated IRE work. R. V. Davalos received consultancy and research grants from Angiodynamics, Inc., for unrelated IRE work. H. Kavnoudias and K.R. Thomson received donated research materials for unrelated IRE work. R. L. Smith, F. Rosenfeldt, R. Ou, C. A. Mclean have no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Neal, R.E., Smith, R.L., Kavnoudias, H. et al. The Effects of Metallic Implants on Electroporation Therapies: Feasibility of Irreversible Electroporation for Brachytherapy Salvage. Cardiovasc Intervent Radiol 36, 1638–1645 (2013). https://doi.org/10.1007/s00270-013-0704-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-013-0704-1