Abstract
Introduction
Although intra-articular injections (IAIs) serve as the first-line non-surgical management for severe osteoarthritis (OA), recent analyses have suggested they are associated with an increased infection risk following primary total hip arthroplasty (THA). Therefore, our systematic review and meta-analysis explored the relationship between IAIs and periprosthetic joint infection (PJI) following THA reported in the current literature.
Methods
Five online databases were queried for analyses published from January 1st, 2000–May 1st, 2021 reporting on PJI rates between patients undergoing primary THA who did and did not preoperatively receive an IAI. The overall pooled effect of injection status on PJI incidence was determined using Mantel–Haenszel (M-H) models. This was similarly conducted for segregated preoperative intervals: 0–3 months, > 3–6 months, > 6 + months.
Results
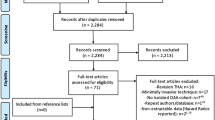
A total of 11 articles were included in our analysis reporting on 278,782 THAs (IAI: n = 41,138; no IAI: n = 237,644). Patients receiving pre-operative injections had a significantly higher risk of PJI (OR: 1.31, 95% CI 1.07–1.62; p = 0.009). However, this finding was not robust. IAI receipt within 3-months of THA was associated with significantly higher PJI rates (OR: 1.68, 95% CI 1.48–1.90; p < 0.001). However, no significant difference was demonstrated in the > 3–6 month (OR: 1.19, 95% CI 0.94–1.52; p = 0.16) and > 6 + month sub-analyses (OR: 1.20, 95% CI 0.96–1.50; p = 0.11). The results of all sub-analyses remained were robust.
Discussion
Our findings suggest that patients requiring THA should wait at least 3-months following IAI to reduce post-operative infection risk. This information can help inform patients considering OA management options, as well as adult reconstruction surgeons during preoperative optimization.






Similar content being viewed by others
References
O’Toole P, Maltenfort MG, Chen AF, Parvizi J (2016) Projected increase in periprosthetic joint infections secondary to rise in diabetes and obesity. J Arthroplasty 31:7–10. https://doi.org/10.1016/j.arth.2015.07.034
Premkumar A, Kolin DA, Farley KX et al (2021) Projected economic burden of periprosthetic joint infection of the hip and knee in the United States. J Arthroplasty 36:1484-1489.e3. https://doi.org/10.1016/j.arth.2020.12.005
Sloan M, Premkumar A, Sheth NP (2018) Projected volume of primary total joint arthroplasty in the U.S., 2014 to 2030. J Bone Jt Surg 100:1455–1460. https://doi.org/10.2106/JBJS.17.01617
Senneville E, Joulie D, Legout L et al (2011) Outcome and predictors of treatment failure in total hip/knee prosthetic joint infections due to Staphylococcus aureus. Clin Infect Dis 53:334–340. https://doi.org/10.1093/cid/cir402
Marculescu CE, Berbari EF, Hanssen AD et al (2006) Outcome of prosthetic joint infections treated with debridement and retention of components. Clin Infect Dis 42:471–478. https://doi.org/10.1086/499234
Lentino JR (2003) Prosthetic joint infections: bane of orthopedists, challenge for infectious disease specialists. Clin Infect Dis 36:1157–1161. https://doi.org/10.1086/374554
Peel TN, Dowsey MM, Buising KL et al (2013) Cost analysis of debridement and retention for management of prosthetic joint infection. Clin Microbiol Infect 19:181–186. https://doi.org/10.1111/J.1469-0691.2011.03758.X
Hofmann AA, Goldberg TD, Tanner AM, Cook TM (2005) Ten-year experience using an articulating antibiotic cement hip spacer for the treatment of chronically infected total hip. J Arthroplasty 20:874–879. https://doi.org/10.1016/j.arth.2004.12.055
Berend KR, Lombardi AV, Morris MJ et al (2013) Two-stage treatment of hip periprosthetic joint infection is associated with a high rate of infection control but high mortality. Clin Orthop Relat Res 471:510–518. https://doi.org/10.1007/s11999-012-2595-x
Leung F, Richards CJ, Garbuz DS et al (2011) Two-stage total hip arthroplasty: how often does it control methicillin-resistant infection? Clin Orthop Relat Res 469:1009–1015. https://doi.org/10.1007/s11999-010-1725-6
Natsuhara KM, Shelton TJ, Meehan JP, Lum ZC (2019) Mortality during total hip periprosthetic joint infection. J Arthroplasty 34:S337–S342. https://doi.org/10.1016/j.arth.2018.12.024
Akgün D, Trampuz A, Perka C, Renz N (2017) High failure rates in treatment of streptococcal periprosthetic joint infection. Bone Jt J 99B:653–659. https://doi.org/10.1302/0301-620X.99B5.BJJ-2016-0851.R1
Kandel CE, Jenkinson R, Daneman N et al (2019) Predictors of treatment failure for hip and knee prosthetic joint infections in the setting of 1-and 2-stage exchange arthroplasty: a multicenter retrospective cohort. Open Forum Infect Dis. https://doi.org/10.1093/ofid/ofz452
Cancienne JM, Granadillo VA, Patel KJ et al (2018) Risk factors for repeat debridement, spacer retention, amputation, arthrodesis, and mortality after removal of an infected total knee arthroplasty with spacer placement. J Arthroplasty 33:515–520. https://doi.org/10.1016/j.arth.2017.08.037
Fagotti L, Tatka J, Salles MJC, Queiroz MC (2018) Risk factors and treatment options for failure of a two-stage exchange. Curr Rev Musculoskelet Med 11:420–427
Suda AJ, Heppert V (2010) Vastus lateralis muscle flap for infected hips after resection arthroplasty. J Bone Jt Surg Ser B 92:1654–1658. https://doi.org/10.1302/0301-620X.92B12.25212
Mahmoud SSS, Sukeik M, Alazzawi S et al (2016) Salvage procedures for management of prosthetic joint infection after hip and knee replacements. Open Orthop J 10:600–614. https://doi.org/10.2174/1874325001610010600
Tande AJ, Patel R (2014) Prosthetic joint infection. Clin Microbiol Rev 27:302–345. https://doi.org/10.1128/CMR.00111-13
Kapadia BH, Banerjee S, Cherian JJ et al (2016) The economic impact of periprosthetic infections after total hip arthroplasty at a specialized tertiary-care center. J Arthroplasty 31:1422–1426. https://doi.org/10.1016/j.arth.2016.01.021
Villa JM, Pannu TS, Piuzzi N et al (2020) Evolution of diagnostic definitions for periprosthetic joint infection in total hip and knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/j.arth.2019.10.032
Lenguerrand E, Whitehouse MR, Beswick AD et al (2018) Risk factors associated with revision for prosthetic joint infection after hip replacement: a prospective observational cohort study. Lancet Infect Dis 18:1004–1014. https://doi.org/10.1016/S1473-3099(18)30345-1
Parvizi J, Tan TL, Goswami K et al (2018) The 2018 definition of periprosthetic hip and knee infection: an evidence-based and validated criteria. J Arthroplasty 33:1309-1314.e2. https://doi.org/10.1016/j.arth.2018.02.078
Zhong HM, Zhao GF, Lin T et al (2020) Intra-articular steroid injection for patients with hip osteoarthritis: a systematic review and meta-analysis. Biomed Res Int. https://doi.org/10.1155/2020/6320154
Martin SD, Conaway WK, Lei P (2018) Use of intra-articular corticosteroids in orthopaedics. J Bone Jt Surg Am 100:885–891
Katz JN, Arant KR, Loeser RF (2021) Diagnosis and treatment of hip and knee osteoarthritis: a review. J Am Med Assoc 325:568–578
Colen S, Hoorntje A, Maeckelbergh L et al (2021) Intra-articular hyaluronic acid injections less than 6 months before total hip arthroplasty: is it safe? A retrospective cohort study in 565 patients. J Arthroplasty 36:1003–1008. https://doi.org/10.1016/j.arth.2020.09.024
de Kaspar SJ (2005) Infection in hip arthroplasty after previous injection of steroid. J Bone Jt Surg Ser B 87:454–457. https://doi.org/10.1302/0301-620X.87B4.15546
Sreekumar R, Venkiteswaran R, Raut V (2007) Infection in primary hip arthroplasty after previous steroid infiltration. Int Orthop 31:125–128
Croft S, Rockwood P (2013) Risk of intraarticular steroid injection before total hip arthroplasty. Curr Orthop Pract 24:185–188. https://doi.org/10.1097/BCO.0b013e3182847788
Forlenza EM, Burnett RA, Korrapati A et al (2021) Preoperative corticosteroid injections demonstrate a temporal and dose-dependent relationship with the rate of postoperative infection following total hip arthroplasty. J Arthroplasty 36:2033-2037.e1. https://doi.org/10.1016/j.arth.2021.01.076
Ravi B, Escott BG, Wasserstein D et al (2015) Intraarticular hip injection and early revision surgery following total hip arthroplasty: a retrospective cohort study. Arthritis Rheumatol 67:162–168. https://doi.org/10.1002/art.38886
Schairer WW, Nwachukwu BU, Mayman DJ et al (2016) Preoperative hip injections increase the rate of periprosthetic infection after total hip arthroplasty. J Arthroplasty 31:166-169.e1. https://doi.org/10.1016/j.arth.2016.04.008
Wang Q, Jiang X, Tian W (2014) Does previous intra-articular steroid injection increase the risk of joint infection following total hip arthroplasty or total knee arthroplasty? A meta-analysis. Med Sci Monit 20:1878–1883. https://doi.org/10.12659/MSM.890750
Pereira LC, Kerr J, Jolles BM (2016) Intra-articular steroid injection for osteoarthritis of the hip prior to total hip arthroplasty: is it safe? A systematic review. Bone Jt J 98-B:1027–1035
Acuña AJ, Do MT, Samuel LT et al (2021) Periprosthetic joint infection rates across primary total hip arthroplasty surgical approaches: a systematic review and meta-analysis of 653,633 procedures. Arch Orthop Trauma Surg 1:1–13. https://doi.org/10.1007/S00402-021-04186-3/FIGURES/7
Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) PRISMA checklist. https://doi.org/10.1371/journal.pmed1000097
Tang A, Almetwali O, Zak SG et al (2021) Do preoperative intra-articular corticosteroid and hyaluronic acid injections affect time to total joint arthroplasty? J Clin Orthop Trauma 16:49–57. https://doi.org/10.1016/j.jcot.2020.12.016
McIntosh AL, Hanssen AD, Wenger DE, Osmon DR (2006) Recent intraarticular steroid injection may increase infection rates in primary THA. Clinical orthopaedics and related research. Lippincott Williams and Wilkins, pp 50–54
Meermans G, Corten K, Simon JP (2012) Is the infection rate in primary THA increased after steroid injection? Clinical orthopaedics and related research. Springer, New York, pp 3213–3219
Werner BC, Cancienne JM, Browne JA (2016) The timing of total hip arthroplasty after intraarticular hip injection affects postoperative infection risk. J Arthroplasty 31:820–823. https://doi.org/10.1016/j.arth.2015.08.032
Öhlin A, Karlsson L, Senorski EH et al (2019) Quality assessment of prospective cohort studies evaluating arthroscopic treatment for femoroacetabular impingement syndrome: a systematic review. Orthop J Sport Med 7(5):2325967119838533. https://doi.org/10.1177/2325967119838533
Cochrane Training Cochrane Handbook for Systematic Reviews of Interventions | Cochrane Training. https://training.cochrane.org/cochrane-handbook-systematic-reviews-interventions. Accessed 23 Feb 2021
Charalambous CP, Prodromidis AD, Kwaees TA (2014) Do intra-articular steroid injections increase infection rates in subsequent arthroplasty? A systematic review and meta-analysis of comparative studies. J Arthroplasty 29:2175–2180. https://doi.org/10.1016/J.ARTH.2014.07.013
McMahon S, Le Roux J, Smith T, Hing C (2013) Total joint arthroplasty following intra-articular steroid injection: a literature review. Acta Orthop Belg 79:672–679
Chandrasekaran S, Lodhia P, Suarez-Ahedo C et al (2016) Symposium: evidence for the use of intra-articular cortisone or hyaluronic acid injection in the hip. J Hip Preserv Surg 3:5. https://doi.org/10.1093/JHPS/HNV020
Charalambous CP, Tryfonidis M, Sadiq S et al (2003) Septic arthritis following intra-articular steroid injection of the knee—a survey of current practice regarding antiseptic technique used during intra-articular steroid injection of the knee. Clin Rheumatol 22:386–390. https://doi.org/10.1007/s10067-003-0757-7
Chitre AR, Fehily MJ, Bamford DJ (2007) Total hip replacement after intra-articular injection of local anaesthetic and steroid. J Bone Jt Surg Ser B 89:166–168. https://doi.org/10.1302/0301-620X.89B2.18428
Papavasiliou AV, Isaac DL, Marimuthu R et al (2006) Infection in knee replacements after previous injection of intra-articular steroid. J Bone Jt Surg Ser B 88:321–323
Shirtliff ME, Mader JT (2002) Acute septic arthritis. Clin Microbiol Rev 15:527–544
Guo J, Dou D (2020) Influence of prior hip arthroscopy on outcomes after hip arthroplasty: a meta-analysis of matched control studies. Medicine (Baltimore) 99:e21246. https://doi.org/10.1097/MD.0000000000021246
American Academy of Orthopaedic Surgeons (AAOS) Limited evidence suggests intra-articular injection performed prior to total joint arthroplasty may have a time-dependent association for increased risk of PJI. https://www.orthoguidelines.org/go/cpg/detail.cfm?id=1495. Accessed 11 Jul 2021
Blankstein M, Lentine B, Nelms NJ (2021) Common practices in intra-articular corticosteroid injection for the treatment of knee osteoarthritis: a survey of the American Association of Hip and Knee Surgeons Membership. J Arthroplasty 36:845–850. https://doi.org/10.1016/J.ARTH.2020.09.022
Funding
No funding was received for our analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A.F.K. reports the following disclosures: research support (Signature Orthopaedics), paid presenter or speaker (DePuy Synthes and Zimmer Biomet), paid consultant (DePuy Synthes and Zimmer Biomet), stock or stock options (Zimmer Biomet, Johnson & Johnson, and Procter & Gamble), IP royalties (Innomed), and board or committee member (AAOS, AAHKS, and Anterior Hip Foundation). J.E.O. reports the following disclosures: board or committee member (AAHKS), paid consultant (Depuy), and research support (DePuy). A.J.A., L.T.S., M.T.D., and A.A. have nothing to disclose.
Ethical approval
Our analysis included de-identified information and therefore, IRB approval was not required.
Informed consent
Our analysis included de-identified information and therefore, patient consent was not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Avila, A., Do, M.T., Acuña, A.J. et al. How do pre-operative intra-articular injections impact periprosthetic joint infection risk following primary total hip arthroplasty? A systematic review and meta-analysis. Arch Orthop Trauma Surg 143, 1627–1635 (2023). https://doi.org/10.1007/s00402-022-04375-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04375-8