Abstract
Introduction
The last systematic review on this topic was published in 2008. With advances in surgical techniques, patients with mangled extremities may now be potentially salvageable with comparable outcomes. This review aims to evaluate the outcomes of limb salvage compared to primary amputation in patients with severe open tibial fractures.
Materials and methods
A comprehensive search on PubMed, MEDLINE, Embase, Web of Science, Scopus, CENTRAL and CINAHL was performed from inception to 19 January 2022. The primary outcome was to evaluate clinical and functional outcomes. Secondary outcomes were to evaluate pain, patient preference, quality of life, and patient preferences. Methodological quality was evaluated using the MINORS criteria. Pooled estimates of relative risk (RR) and mean difference (MD) with 95% confidence interval (CI) were used as a summary statistic for dichotomous variables and continuous variables, respectively.
Results
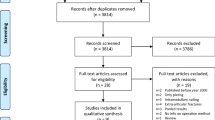
Sixteen studies with 645 patients met inclusion criteria. The methodological quality was moderate based on the MINORS score. The majority were male. Mean age was 36.3 years. There was no significant differences in the length of hospitalization (n = 8), return to work rates (n = 9), return to sport rates (n = 4) and quality of life scores (n = 4). Patients with primary amputation had a significantly lower risk of total complications (RR 0.21, 95% CI 0.08–0.53, p = 0.001) (n = 10), infections (RR 0.46, 95% CI 0.25–0.85, p = 0.01) (n = 9), and number of surgeries (MD – 4.17, 95% CI − 6.49 to − 1.85, p = 0.0004) (n = 6). Patients with primary amputation were able to ambulate significantly earlier (MD − 4.06, 95% CI − 7.65 to − 0.46, p = 0.03) (n = 3). Three studies found a significantly higher cost of hospitalization in limb salvage patients. Functional outcomes were similar in both groups.
Conclusion
While patients with primary amputation had better clinical outcomes in the short-term, functional outcomes were not significantly different in both groups. Despite the heterogenicity of the results in this review, surgeons need to contextualize the decision making for their patients and incorporate these findings.
Level of evidence
III.
Trial registration
PROSPERO CRD42022303357.










Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- AKA:
-
Above knee amputation
- BKA:
-
Below knee amputation
- CI:
-
Confidence interval
- LEFS:
-
Lower-extremity functional scale
- MCS:
-
Mental component score
- MD:
-
Mean difference
- MINORS:
-
Methodological Index for Randomized Studies
- PCS:
-
Physical component score
- ROM:
-
Range of motion
- RR:
-
Relative risk
- SD:
-
Standard deviation
- SF-12:
-
12-Item Short Form Survey
- SF-36:
-
36-Item Short Form Survey
- WOMAC:
-
Western Ontario and McMaster Universities Arthritis Index
References
Patel MB, Richter KM, Shafi S (2015) Mangled extremity: amputation versus salvage. Curr Trauma Rep 1:45–49. https://doi.org/10.1007/s40719-014-0003-6
Harris AM, Althausen PL, Kellam J et al (2009) Complications following limb-threatening lower extremity trauma. J Orthop Trauma 23:1–6. https://doi.org/10.1097/BOT.0b013e31818e43dd
Huh J, Stinner DJ, Burns TC et al (2011) Infectious complications and soft tissue injury contribute to late amputation after severe lower extremity trauma. J Trauma 71:S47-51. https://doi.org/10.1097/TA.0b013e318221181d
Chung KC, Shauver MJ, Saddawi-Konefka D, Haase SC (2011) A decision analysis of amputation versus reconstruction for severe open tibial fracture from the physician and patient perspectives. Ann Plast Surg 66:185–191. https://doi.org/10.1097/SAP.0b013e3181cbfcce
Schirò GR, Sessa S, Piccioli A, Maccauro G (2015) Primary amputation vs limb salvage in mangled extremity: a systematic review of the current scoring system. BMC Musculoskelet Disord 16:372. https://doi.org/10.1186/s12891-015-0832-7
Akula M, Gella S, Shaw CJ et al (2011) A meta-analysis of amputation versus limb salvage in mangled lower limb injuries—the patient perspective. Injury 42:1194–1197. https://doi.org/10.1016/j.injury.2010.05.003
Black CK, Ormiston LD, Fan KL et al (2021) amputations versus salvage: reconciling the differences. J Reconstr Microsurg 37:32–41. https://doi.org/10.1055/s-0039-1696733
Rossiter ND, Higgins TF, Pallister I (2014) (ii) The mangled extremity: limb salvage versus amputation. Orthop Trauma 28:137–140. https://doi.org/10.1016/j.mporth.2014.05.002
Busse JW, Jacobs CL, Swiontkowski MF et al (2007) Complex limb salvage or early amputation for severe lower-limb injury: a meta-analysis of observational studies. J Orthop Trauma 21:70–76. https://doi.org/10.1097/BOT.0b013e31802cbc43
Saddawi-Konefka D, Kim HM, Chung KC (2008) A systematic review of outcomes and complications of reconstruction and amputation for type IIIB and IIIC fractures of the Tibia. Plast Reconstr Surg 122:1796–1805. https://doi.org/10.1097/PRS.0b013e31818d69c3
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700–b2700. https://doi.org/10.1136/bmj.b2700
Higgins J, Thomas J, Chandler J et al (2022) Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). Cochrane
OCEBM Levels of Evidence Working Group The Oxford Levels of Evidence 2
Slim K, Nini E, Forestier D et al (2003) Methodological index for non-randomized studies (MINORS): development and validation of a new instrument: methodological index for non-randomized studies. ANZ J Surg 73:712–716. https://doi.org/10.1046/j.1445-2197.2003.02748.x
Yeung M, Kowalczuk M, Simunovic N, Ayeni OR (2016) Hip arthroscopy in the setting of hip dysplasia: a systematic review. Bone Jt Res 5:225–231. https://doi.org/10.1302/2046-3758.56.2000533
Walter SD, Yao X (2007) Effect sizes can be calculated for studies reporting ranges for outcome variables in systematic reviews. J Clin Epidemiol 60:849–852. https://doi.org/10.1016/j.jclinepi.2006.11.003
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13. https://doi.org/10.1186/1471-2288-5-13
Higgins JPT (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Aravind M, Shauver MJ, Chung KC (2010) A qualitative analysis of the decision-making process for patients with severe lower leg trauma. Plast Reconstr Surg 126:2019–2029. https://doi.org/10.1097/PRS.0b013e3181f4449e
Chung KC, Saddawi-Konefka D, Haase SC, Kaul G (2009) A cost-utility analysis of amputation versus salvage for gustilo type IIIB and IIIC open tibial fractures. Plast Reconstr Surg 124:1965–1973. https://doi.org/10.1097/PRS.0b013e3181bcf156
Dagum AB, Best AK, Schemitsch EH et al (1999) Salvage after Severe Lower-Extremity Trauma: Are the Outcomes Worth the Means? Plast Reconstr Surg 103:1212–1220. https://doi.org/10.1097/00006534-199904010-00017
Dahl B, Andersson AP, Andersen M et al (1995) Functional and social long-term results after free tissue transfer to the lower extremity. Ann Plast Surg 34:372–375. https://doi.org/10.1097/00000637-199504000-00005
Fioravanti M, Maman P, Curvale G et al (2018) Amputation versus conservative treatment in severe open lower-limb fracture: A functional and quality-of-life study. Orthop Traumatol Surg Res 104:277–281. https://doi.org/10.1016/j.otsr.2017.12.013
Frisvoll C, Clarke-Jenssen J, Madsen JE et al (2019) Long-term outcomes after high-energy open tibial fractures: Is a salvaged limb superior to prosthesis in terms of physical function and quality of life? Eur J Orthop Surg Traumatol 29:899–906. https://doi.org/10.1007/s00590-019-02382-x
Georgiadis GM, Behrens FF, Joyce MJ et al (1993) Open tibial fractures with severe soft-tissue loss. Limb salvage compared with below-the-knee amputation. J Bone Jt Surg 75:1431–1441. https://doi.org/10.2106/00004623-199310000-00003
Hertel R, Strebel N, Ganz R (1996) Amputation versus reconstruction in traumatic defects of the leg: outcome and costs. J Orthop Trauma 10:223–229. https://doi.org/10.1097/00005131-199605000-00001
Hutchins PM (1981) The outcome of severe tibial injury. Injury 13:216–219. https://doi.org/10.1016/0020-1383(81)90242-4
Lange RH, Bach AW, Hansen ST, Johansen KH (1985) Open tibial fractures with associated vascular injuries: prognosis for limb salvage. J Trauma 25:203–208. https://doi.org/10.1097/00005373-198503000-00006
Penn-Barwell JG, Myatt RW, Bennett PM et al (2015) Medium-term outcomes following limb salvage for severe open tibia fracture are similar to trans-tibial amputation. Injury 46:288–291. https://doi.org/10.1016/j.injury.2014.12.004
Puno RM, Grossfeld SL, Henry SL et al (1996) Functional outcome of patients with salvageable limbs with grades III-B and III-C open fractures of the tibia. Microsurgery 17:167–173. https://doi.org/10.1002/(SICI)1098-2752(1996)17:3%3c167::AID-MICR14%3e3.0.CO;2-Y
Ritchie AJ, Small JO, Hart NB, Mollan RAB (1991) Type III tibial fractures in the elderly: results of 23 fractures in 20 patients. Injury 22:267–270. https://doi.org/10.1016/0020-1383(91)90003-W
Sethuraman AS, Devendra A, Rajasekaran RB et al (2021) Is lower limb salvage worthwhile after severe open tibial fractures in a developing country? An analysis of surgical outcomes, quality of life and cost implications. Injury 52:996–1001. https://doi.org/10.1016/j.injury.2020.12.027
Sügün TS (2013) Limb salvage and amputation in Type 3C tibial fractures. Acta Orthop Traumatol Turc 47:19–26. https://doi.org/10.3944/AOTT.2013.2823
Tekin L, Safaz Ý, Göktepe AS, Yazýcýođlu K (2009) Comparison of quality of life and functionality in patients with traumatic unilateral below knee amputation and salvage surgery. Prosthet Orthot Int 33:17–24. https://doi.org/10.1080/03093640802482542
Schade AT, Khatri C, Nwankwo H et al (2021) The economic burden of open tibia fractures: a systematic review. Injury 52:1251–1259. https://doi.org/10.1016/j.injury.2021.02.022
Rees S, Tutton E, Achten J et al (2019) Patient experience of long-term recovery after open fracture of the lower limb: a qualitative study using interviews in a community setting. BMJ Open 9:e031261. https://doi.org/10.1136/bmjopen-2019-031261
Ribeiro D, Cimino SR, Mayo AL et al (2021) 3D printing and amputation: a scoping review. Disabil Rehabil Assist Technol 16:221–240. https://doi.org/10.1080/17483107.2019.1646825
Nightingale J, Shu’anScammell KLBE et al (2022) What is important to patients who are recovering from an open tibial fracture? a qualitative study. Clin Orthop 480:263–272. https://doi.org/10.1097/CORR.0000000000002031
Errasti-Ibarrondo B, Jordán JA, Díez-Del-Corral MP, Arantzamendi M (2018) Conducting phenomenological research: Rationalizing the methods and rigour of the phenomenology of practice. J Adv Nurs 74:1723–1734. https://doi.org/10.1111/jan.13569
Funding
No sources of funding were available for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Each author certifies that there are no financial and non-financial competing interests in connection with the submitted article related to the author or any immediate family members.
Ethical approval
Not applicable /None required.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ng, H.J.H., Ang, E.J.G., Premchand, A.X.R. et al. Limb salvage versus primary amputation in Gustilo–Anderson IIIB and IIIC tibial fractures: a systematic review and meta-analysis. Arch Orthop Trauma Surg 143, 4961–4976 (2023). https://doi.org/10.1007/s00402-023-04804-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04804-2