Abstract
Purpose
Patients with cancer are at increased risk for infection, but the relative morbidity and mortality of all infections is not well understood. The objectives of this study were to determine the prevalence, incidence, time-trends and risk of mortality of infections associated with hospital admissions in patients with haematological- and solid-tumour malignancies over 11 years.
Methods
A retrospective, longitudinal cohort study of inpatient admissions between 1 January 2007 and 31 December 2017 at the Peter MacCallum Cancer Centre was conducted using administratively coded and patient demographics data. Descriptive analyses, autoregressive integrated moving average, Kaplan-Meier and Cox regression modelling were applied.
Results
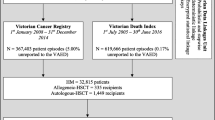
Of 45,116 inpatient hospitalisations consisting of 3033 haematological malignancy (HM), 18,372 solid tumour neoplasm (STN) patients and 953 autologous haematopoietic stem cell transplantation recipients, 67%, 29% and 88% were coded with ≥ 1 infection, respectively. Gastrointestinal tract and bloodstream infections were observed with the highest incidence, and bloodstream infection rates increased significantly over time in both HM- and STN-cohorts. Inpatient length of stay was significantly higher in exposed patients with coded infection compared to unexposed in HM- and STN-cohorts (22 versus 4 days [p < 0.001] and 15 versus 4 days [p < 0.001], respectively). Risk of in-hospital mortality was higher in exposed than unexposed patients in the STN-cohort (adjusted hazard ratio [aHR] 1.61 [95% CI 1.41–1.83]; p < 0.001)) and HM-cohort (aHR 1.30 [95% CI 0.90–1.90]; p = 0.166).
Conclusion
Infection burden among cancer patients is substantial and findings reflect the need for targeted surveillance in high-risk patient groups (e.g. haematological malignancy), in whom enhanced monitoring may be required to support infection prevention strategies.




Similar content being viewed by others
References
Valentine JC, Hall L, Verspoor KM, Worth LJ (2019) The current scope of healthcare-associated infection surveillance activities in hospitalized immunocompromised patients: a systematic review. Int J Epidemiol 48(6):1768–1782. https://doi.org/10.1093/ije/dyz162
Valentine JC, Morrissey CO, Tacey MA, Liew D, Patil S, Peleg AY, Ananda-Rajah MR (2019) A population-based analysis of invasive fungal disease in haematology-oncology patients using data linkage of state-wide registries and administrative databases: 2005–2016. BMC Infect Dis 19(1):274. https://doi.org/10.1186/s12879-019-3901-y
Kochanek M, Kiehl M, Liebregts T (2019) Intensivmedizinisches management schwerer Infektionen bei Krebspatienten. Dtsch Med Wochenschr 144(19):1333–1341. https://doi.org/10.1055/a-0853-4739
Valentine JC, Morrissey CO, Tacey MA, Liew D, Patil S, Ananda-Rajah M (2020) A population-based analysis of attributable hospitalisation costs of invasive fungal diseases in haematological malignancy patients using data linkage of state-wide registry and costing databases: 2009–2015. Mycoses 63(2):162–171. https://doi.org/10.1111/myc.13033
Teh BW, Harrison SJ, Worth LJ, Thursky KA, Slavin MA (2016) Infection risk with immunomodulatory and proteasome inhibitor-based therapies across treatment phases for multiple myeloma: a systematic review and meta-analysis. Eur J Cancer 67:21–37. https://doi.org/10.1016/j.ejca.2016.07.025
Even C, Bastuji-Garin S, Hicheri Y, Pautas C, Botterel F, Maury S, Cabanne L, Bretagne S, Cordonnier C (2011) Impact of invasive fungal disease on the chemotherapy schedule and event-free survival in acute leukemia patients who survived fungal disease: a case-control study. Haematologica 96(2):337–341. https://doi.org/10.3324/haematol.2010.030825
te Marvelde L, Whitfield A, Shepheard J, Read C, Milne RL, Whitfield K (2020) Epidemiology of sepsis in cancer patients in Victoria, Australia: a population-based study using linked data. Aust N Z J Public Health 44(1):53–58. https://doi.org/10.1111/1753-6405.12935
WHO ICD Implementation Database (WHOFIC). (2016) World Health Organization. http://apps.who.int/gho/data/node.whofic.S01bQ01_02?lang=en. Accessed 11 Feb 2020
ICD-10-AM/ACHI/ACS. (2019) National Centre for Classification in Health. https://sydney.edu.au/health-sciences/ncch/icd-10-am.shtml. Accessed 21 May 2019
Slavin MA, Thursky KA, Worth LJ, Chang CC, Morrissey CO, Blyth CC, Chen SC, Szer J (2014) Introduction to the updated Australian and New Zealand consensus guidelines for the use of antifungal agents in the haematology/oncology setting, 2014. Intern Med J 44(12b):1267–1276. https://doi.org/10.1111/imj.12593
Doan TN, Kirkpatrick CM, Walker P, Slavin MA, Ananda-Rajah MR, Morrissey CO, Urbancic KF, Grigg A, Spencer A, Szer J, Seymour JF, Kong DC (2016) Primary antifungal prophylaxis in adult patients with acute lymphoblastic leukaemia: a multicentre audit. J Antimicrob Chemother 71(2):497–505. https://doi.org/10.1093/jac/dkv343
Lingaratnam S, Slavin MA, Koczwara B, Seymour JF, Szer J, Underhill C, Prince M, Mileshkin L, O'Reilly M, Kirsa SW, Bennett CA, Davis ID, Morrissey O, Thursky KA, Australian Consensus Guidelines Steering C (2011) Introduction to the Australian consensus guidelines for the management of neutropenic fever in adult cancer patients, 2010/2011. Australian consensus guidelines 2011 steering committee. Intern Med J 41(1b):75–81. https://doi.org/10.1111/j.1445-5994.2010.02338.x
Morrissey CO, Gilroy NM, Macesic N, Walker P, Ananda-Rajah M, May M, Heath CH, Grigg A, Bardy PG, Kwan J, Kirsa SW, Slavin M, Gottlieb T, Chen S (2014) Consensus guidelines for the use of empiric and diagnostic-driven antifungal treatment strategies in haematological malignancy, 2014. Intern Med J 44(12b):1298–1314. https://doi.org/10.1111/imj.12596
Connell L, MacDonald R, McBride T, Peiperl L, Ross A, Simpson P, Winker M (2014) Observational studies: getting clear about transparency. PLoS Med 11(8):e1001711. https://doi.org/10.1371/journal.pmed.1001711
Benchimol EI, Smeeth L, Guttmann A, Harron K, Moher D, Petersen I, Sørensen HT, von Elm E, Langan SM (2015) The REporting of studies conducted using observational routinely-collected data (RECORD) statement. PLoS Med 12(10):e1001885. https://doi.org/10.1371/journal.pmed.1001885
Victorian additions to Australian Coding Standards (2020) Victorian Agency for Health Information. https://www.bettersafercare.vic.gov.au/our-work/information-management-and-standards/clinical-coding-and-classifications/additions. Accessed 14 Feb 2020
Baker MG, Bernard LT, Kvalsig A, Verrall A, Zhang J, Keall M, Wilson N, Wall T, Howden-Chapman P (2012) Increasing incidence of serious infectious diseases and inequalities in New Zealand: a national epidemiological study. Lancet 379:1112–1119. https://doi.org/10.1016/S0140-6736(11)61780-7
Quan H, Sundararajan V, Halfon P, Fong A, Burnand B, Luthi J-C, Saunders LD, Beck CA, Feasby TE, Ghali WA (2005) Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care 43(11):1130–1139. https://doi.org/10.1097/01.mlr.0000182534.19832.83
Wang Q, Wu N (2012) Menu-driven X-12-ARIMA seasonal adjustment in Stata. Stata J 12(2):214–241. https://doi.org/10.1177/1536867X1201200204
Walter SD, Elwood JM (1975) A test for seasonality of events with a variable population at risk. Br J Prev Soc Med 29(1):18–21. https://doi.org/10.1136/jech.29.1.18
Thursky K, Lingaratnam S, Jayarajan J, Haeusler GM, Teh B, Tew M, Venn G, Hiong A, Brown C, Leung V, Worth LJ, Dalziel K, Slavin MA (2018) Implementation of a whole of hospital sepsis clinical pathway in a cancer hospital: impact on sepsis management, outcomes and costs. BMJ Open Qual 7(3):e000355. https://doi.org/10.1136/bmjoq-2018-000355
Douglas AP, Thursky KA, Worth LJ, Harrison SJ, Hicks RJ, Slavin MA (2019) FDG-PET/CT in managing infection in patients with hematological malignancy: clinician knowledge and experience in Australia. Leuk Lymphoma 60(10):2471–2476. https://doi.org/10.1080/10428194.2019.1590571
Teh BW, Harrison SJ, Worth LJ, Spelman T, Thursky KA, Slavin MA (2015) Risks, severity and timing of infections in patients with multiple myeloma: a longitudinal cohort study in the era of immunomodulatory drug therapy. Br J Haematol 171(1):100–108. https://doi.org/10.1111/bjh.13532
Dettenkofer M, Wenzler-Röttele S, Babikir R, Bertz H, Ebner H, Meyer E, Rüden H, Gastmeier P, Daschner FD (2005) Surveillance of nosocomial sepsis and pneumonia in patients with bone marrow or peripheral blood stem cell transplant: a multicenter project. Clin Infect Dis 40(7):926–931. https://doi.org/10.1086/428046
Kontoyiannis DP, Marr KA, Park BJ, Alexander BD, Anaissie EJ, Walsh TJ, Ito J, Andes DR, Baddley JW, Brown JM, Brumble LM, Freifeld AG, Hadley S, Herwaldt LA, Kauffman CA, Knapp K, Lyon GM, Morrison VA, Papanicolaou G, Patterson TF, Perl TM, Schuster MG, Walker R, Wannemuehler KA, Wingard JR, Chiller TM, Pappas PG (2010) Prospective surveillance for invasive fungal infections in hematopoietic stem cell transplant recipients, 2001-2006: overview of the transplant-associated infection surveillance network (TRANSNET) database. Clin Infect Dis 50(8):1091–1100. https://doi.org/10.1086/651263
Avery RK, Silveira FP, Benedict K, Cleveland AA, Kauffman CA, Schuster MG, Dubberke ER, Husain S, Paterson DL, Chiller T, Pappas P (2017) Cytomegalovirus infections in lung and hematopoietic cell transplant recipients in the organ transplant infection prevention and detection study: a multi-year, multicenter prospective cohort study. Transpl Infect Dis 20(3):e12877. https://doi.org/10.1111/tid.12877
Marín M, Gudiol C, Ardanuy C, Garcia-Vidal C, Calvo M, Arnan M, Carratalà J (2014) Bloodstream infections in neutropenic patients with cancer: differences between patients with haematological malignancies and solid tumours. J Inf Secur 69(5):417–423. https://doi.org/10.1016/j.jinf.2014.05.018
Marín M, Gudiol C, Ardanuy C, Garcia-Vidal C, Jimenez L, Domingo-Domenech E, Pérez FJ, Carratalà J (2015) Factors influencing mortality in neutropenic patients with haematologic malignancies or solid tumours with bloodstream infection. Clin Microbiol Infect 21(6):583–590. https://doi.org/10.1016/j.cmi.2015.01.029
Kato Y, Hagihara M, Kurumiya A, Takahashi T, Sakata M, Shibata Y, Kato H, Shiota A, Watanabe H, Asai N, Koizumi Y, Yamagishi Y, Mikamo H (2018) Impact of mucosal barrier injury laboratory-confirmed bloodstream infection (MBI-LCBI) on central line-associated bloodstream infections (CLABSIs) in department of hematology at single university hospital in Japan. J Infect Chemother 24(1):31–35. https://doi.org/10.1016/j.jiac.2017.08.013
Li Y, Klippel Z, Shih X, Reiner M, Wang H, Page JH (2016) Relationship between severity and duration of chemotherapy-induced neutropenia and risk of infection among patients with nonmyeloid malignancies. Support Care Cancer 24(10):4377–4383. https://doi.org/10.1007/s00520-016-3277-0
Rodrigues FG, Dasilva G, Wexner SD (2017) Neutropenic enterocolitis. World J Gastroenterol 23(1):42–47. https://doi.org/10.3748/wjg.v23.i1.42
Isaji S, Mizuno S, Windsor JA, Bassi C, Fernandez-Del Castillo C, Hackert T, Hayasaki A, Katz MHG, Kim SW, Kishiwada M, Kitagawa H, Michalski CW, Wolfgang CL (2018) International consensus on definition and criteria of borderline resectable pancreatic ductal adenocarcinoma 2017. Pancreatology 18(1):2–11. https://doi.org/10.1016/j.pan.2017.11.011
van Mourik MSM, Troelstra A, Moons KGM, Bonten MJM (2013) Accuracy of hospital discharge coding data for the surveillance of drain-related meningitis. Infect Control Hosp Epidemiol 34(4):433–436. https://doi.org/10.1086/669867
Stevenson KB, Khan Y, Dickman J, Gillenwater T, Kulich P, Myers C, Taylor D, Santangelo J, Lundy J, Jarjoura D, Li X, Shook J, Mangino JE (2008) Administrative coding data, compared with CDC/NHSN criteria, are poor indicators of health care-associated infections. Am J Infect Control 36(3):155–164. https://doi.org/10.1016/j.ajic.2008.01.004
Stamm AM, Bettacchi CJ (2012) A comparison of 3 metrics to identify health care-associated infections. Am J Infect Control 40(8):688–691. https://doi.org/10.1016/j.ajic.2012.01.033
Doktorchik C, Lu M, Quan H, Ringham C, Eastwood C (2020) A qualitative evaluation of clinically coded data quality from health information manager perspectives. Health Inf Manag 49(1):19–27. https://doi.org/10.1177/1833358319855031
Babady NE (2016) Laboratory diagnosis of infections in cancer patients: challenges and opportunities. J Clin Microbiol 54(11):2635–2646. https://doi.org/10.1128/JCM.00604-16
Bajwa R, Cheema A, Khan T, Amirpour A, Paul A, Chaughtai S, Patel S, Patel T, Bramson J, Gupta V, Levitt M, Asif A, Hossain MA (2019) Adverse effects of immune checkpoint inhibitors (programmed death-1 inhibitors and cytotoxic T-lymphocyte-associated protein-4 inhibitors): results of a retrospective study. J Clin Med Res 11(4):225–236. https://doi.org/10.14740/jocmr3750
Cooksley CD, Avritscher EB, Rolston KV, Elting LS (2009) Hospitalizations for infection in cancer patients: impact of an aging population. Support Care Cancer 17(5):547–554. https://doi.org/10.1007/s00520-008-0520-3
Taplitz RA, Kennedy EB, Bow EJ, Crews J, Gleason C, Hawley DK, Langston AA, Nastoupil LJ, Rajotte M, Rolston KV, Strasfeld L, Flowers CR (2018) Antimicrobial prophylaxis for adult patients with cancer-related immunosuppression: ASCO and IDSA clinical practice guideline update. J Clin Oncol 36(30):3043–3056. https://doi.org/10.1200/JCO.18.00374
Mitchell BG, Hall L, White N, Barnett AG, Halton K, Paterson DL, Riley TV, Gardner A, Page K, Farrington A, Gericke CA, Graves N (2019) An environmental cleaning bundle and health-care-associated infections in hospitals (REACH): a multicentre, randomised trial. Lancet Infect Dis 19(4):410–418. https://doi.org/10.1016/S1473-3099(18)30714-X
Armen SB, Freer CV, Showalter JW, Crook T, Whitener CJ, West C, Terndrup TE, Grifasi M, DeFlitch CJ, Hollenbeak CS (2016) Improving outcomes in patients with sepsis. Am J Med Qual 31(1):56–63. https://doi.org/10.1177/1062860614551042
Naran K, Nundalall T, Chetty S, Barth S (2018) Principles of immunotherapy: implications for treatment strategies in cancer and infectious diseases. Front Microbiol 9:3158. https://doi.org/10.3389/fmicb.2018.03158
Valentine JC, Haeusler GM, Worth LJ, Thursky KA (2019) Sepsis incidence and mortality are underestimated in Australian intensive care unit administrative data. Med J Aust 210(4):188–188.e181. https://doi.org/10.5694/mja2.50017
van Mourik MSM, van Duijn PJ, Moons KG, Bonten MJ, Lee GM (2015) Accuracy of administrative data for surveillance of healthcare-associated infections: a systematic review. BMJ Open 5(8):e008424. https://doi.org/10.1136/bmjopen-2015-008424
Valentine JC, Hall L, Verspoor K, Spelman T, Worth L (2019) Hospital-coded infections in patients with cancer: evaluating disease burden and outcomes in Australian cancer patients. Infect Dis Health 24(Supplement 1):S2. https://doi.org/10.1016/j.idh.2019.09.006
Donnelly JP, Chen SC, Kauffman CA, Steinbach WJ, Baddley JW, Verweij PE, Clancy CJ, Wingard JR, Lockhart SR, Groll AH, Sorrell TC, Bassetti M, Akan H, Alexander BD, Andes D, Azoulay E, Bialek R, Bradsher RW, Bretagne S, Calandra T, Caliendo AM, Castagnola E, Cruciani M, Cuenca-Estrella M, Decker CF, Desai SR, Fisher B, Harrison T, Heussel CP, Jensen HE, Kibbler CC, Kontoyiannis DP, Kullberg BJ, Lagrou K, Lamoth F, Lehrnbecher T, Loeffler J, Lortholary O, Maertens J, Marchetti O, Marr KA, Masur H, Meis JF, Morrisey CO, Nucci M, Ostrosky-Zeichner L, Pagano L, Patterson TF, Perfect JR, Racil Z, Roilides E, Ruhnke M, Prokop CS, Shoham S, Slavin MA, Stevens DA, Thompson GR, Vazquez JA, Viscoli C, Walsh TJ, Warris A, Wheat LJ, White PL, Zaoutis TE, Pappas PG (2019) Revision and update of the consensus definitions of invasive fungal disease from the European Organization for Research and Treatment of Cancer and the mycoses study group education and research consortium. Clin Infect Dis. https://doi.org/10.1093/cid/ciz1008
Horan TC, Andrus M, Dudeck MA (2008) CDC/NHSN surveillance definition of health care-associated infection and criteria for specific types of infections in the acute care setting. Am J Infect Control 36(5):309–332. https://doi.org/10.1016/j.ajic.2008.03.002
Zhang X, Zhang T, Young AA, Li X (2014) Applications and comparisons of four time series models in epidemiological surveillance data. PLoS One 9(2):e88075. https://doi.org/10.1371/journal.pone.0088075
Smibert OC, Slavin MA, Teh B, Heriot AG, Penno J, Ismail H, Thursky KA, Worth LJ (2019) Epidemiology and risks for infection following cytoreductive surgery and hyperthermic intra-peritoneal chemotherapy. Support Care Cancer:1–8. https://doi.org/10.1007/s00520-019-05093-5
Acknowledgments
The authors would like to acknowledge Ms. Janice Yeung and Ms. Kathryn Baxter of the PMCC’s Health Information Services for allowing the investigators to access their administrative coding data and for their ongoing assistance in data interpretation. The authors thank Ms. Cathy Ma of the PMCC’s Operational Planning and Performance for authorizing administrative access to the patient data. We also thank Mr. Matthew Ha, PMCC Reporting and Data Analyst, for preparing the data for collection. The authors acknowledge the statistical services provided by Mr. Cameron Patrick, Biostatistician at the Melbourne Statistical Consulting Platform, School of Mathematics and Statistics, University of Melbourne. The authors also extend their appreciation to Ms. Frances Martin, Mr. Chris Kearney, Ms. Heather Grain, Associate Professor Deborah Williamson, Dr. Megan Crane, Dr. Michelle K. Yong and colleagues of the NHMRC National Centre for Infections in Cancer for their academic rigour, intellectual input and insight into systems and coding frameworks.
Funding
This study was supported by an Australian Government Research Training Program Scholarship awarded to J.C.V. by the University of Melbourne and a Cardinal Health Infection Control Scholarship awarded to J.C.V. by the Australasian College for Infection Prevention and Control.
Author information
Authors and Affiliations
Contributions
Manuscript preparation was by J.C.V., L.H., T.S., K.M.V., J.F.S., D.R., K.A.T., M.A.S. and L.J.W.; statistical analysis and data retrieval were by J.C.V.; study conception and design were by J.C.V., L.H., K.M.V. and L.J.W.; statistical support was provided from T.S.; all authors (J.C.V., L.H., T.S., K.M.V., J.F.S., D.R., K.A.T., M.A.S. and L.J.W.) contributed to the data interpretation and the critical revision of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Valentine, J.C., Hall, L., Spelman, T. et al. Burden and clinical outcomes of hospital-coded infections in patients with cancer: an 11-year longitudinal cohort study at an Australian cancer centre. Support Care Cancer 28, 6023–6034 (2020). https://doi.org/10.1007/s00520-020-05439-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-020-05439-4