Abstract
Purpose
To determine if adolescent athletics increases the risk of structural abnormalities in the lumbar spine.
Methods
A retrospective review of patients (ages 10–18) between 2004 and 2012 was performed. Pediatric patients with symptomatic low back pain, a lumbar spine MRI, and reported weekly athletic activity were included. Patients were stratified to an “athlete” and “non-athlete” group. Lumbar magnetic resonance and plain radiographic imaging was randomized, blinded, and evaluated by two authors for a Pfirrmann grade, herniated disc, and/or pars fracture.
Results
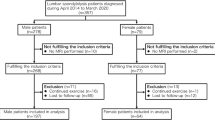
A total of 114 patients met the inclusion criteria and were stratified into 66 athletes and 48 non-athletes. Athletes were more likely to have abnormal findings compared to non-athletes (67 vs. 40 %, respectively, p = 0.01). Specifically, the prevalence of a spondylolysis with or without a slip was higher in athletes vs. non-athletes (32 vs. 2 %, respectively, p = 0.0003); however, there was no difference in the average Pfirrmann grade (1.19 vs. 1.14, p = 0.41), percentage of patients with at least one degenerative disc (39 vs. 31 %, p = 0.41), or disc herniation (27 vs. 33 %, p = 0.43). Body mass index, smoking history, and pelvic incidence (51.5° vs. 48.7°, respectively, p = 0.41) were similar between the groups.
Conclusion
Adolescents with low back pain have a higher-than-expected prevalence of structural pathology regardless of athletic activity. Independent of pelvic incidence, adolescent athletes with low back pain had a higher prevalence of spondylolysis compared to adolescent non-athletes with back pain, but there was no difference in associated disc degenerative changes or herniation.



Similar content being viewed by others
References
Hartvigsen J, Christensen K, Frederiksen H, Petersen HC (2004) Genetic and environmental contributions to back pain in old age: a study of 2108 danish twins aged 70 and older. Spine (Phila Pa 1976) 29:897–901 (discussion 902)
Hartvigsen J, Nielsen J, Kyvik KO, Fejer R, Vach W, Iachine I, Leboeuf-Yde C (2009) Heritability of spinal pain and consequences of spinal pain: a comprehensive genetic epidemiologic analysis using a population-based sample of 15,328 twins ages 20–71 years. Arthritis Rheum 61:1343–1351. doi:10.1002/art.24607
Patel AA, Spiker WR, Daubs M, Brodke D, Cannon-Albright LA (2011) Evidence for an inherited predisposition to lumbar disc disease. J Bone Joint Surg Am 93:225–229. doi:10.2106/JBJS.J.00276
Baranto A, Hellstrom M, Cederlund CG, Nyman R, Sward L (2009) Back pain and MRI changes in the thoraco-lumbar spine of top athletes in four different sports: a 15-year follow-up study. Knee Surg Sports Traumatol Arthrosc 17:1125–1134. doi:10.1007/s00167-009-0767-3
Ferguson RJ, McMaster JH, Stanitski CL (1974) Low back pain in college football linemen. J Sports Med 2:63–69
Hsu WK (2010) Performance-based outcomes following lumbar discectomy in professional athletes in the National Football League. Spine (Phila Pa 1976) 35:1247–1251. doi:10.1097/BRS.0b013e3181bf8bb5
Micheli LJ, Wood R (1995) Back pain in young athletes. Significant differences from adults in causes and patterns. Arch Pediatr Adolesc Med 149:15–18
Ong A, Anderson J, Roche J (2003) A pilot study of the prevalence of lumbar disc degeneration in elite athletes with lower back pain at the Sydney 2000 Olympic Games. Br J Sports Med 37:263–266
Jackson DW, Wiltse LL, Cirincoine RJ (1976) Spondylolysis in the female gymnast. Clin Orthop Relat Res 117:68–73
Beutler WJ, Fredrickson BE, Murtland A, Sweeney CA, Grant WD, Baker D (2003) The natural history of spondylolysis and spondylolisthesis: 45-year follow-up evaluation. Spine (Phila Pa 1976) 28:1027–1035. doi:10.1097/01.BRS.0000061992.98108.A0 (discussion 1035)
Boden SD, Davis DO, Dina TS, Patronas NJ, Wiesel SW (1990) Abnormal magnetic-resonance scans of the lumbar spine in asymptomatic subjects. A prospective investigation. J Bone Joint Surg Am 72:403–408
Fredrickson BE, Baker D, McHolick WJ, Yuan HA, Lubicky JP (1984) The natural history of spondylolysis and spondylolisthesis. J Bone Joint Surg Am 66:699–707
Kalichman L, Kim DH, Li L, Guermazi A, Berkin V, Hunter DJ (2009) Spondylolysis and spondylolisthesis: prevalence and association with low back pain in the adult community-based population. Spine (Phila Pa 1976) 34:199–205. doi:10.1097/BRS.0b013e31818edcfd
Hanson DS, Bridwell KH, Rhee JM, Lenke LG (2002) Correlation of pelvic incidence with low- and high-grade isthmic spondylolisthesis. Spine (Phila Pa 1976) 27:2026–2029
Labelle H, Roussouly P, Berthonnaud E, Transfeldt E, O’Brien M, Chopin D, Hresko T, Dimnet J (2004) Spondylolisthesis, pelvic incidence, and spinopelvic balance: a correlation study. Spine (Phila Pa 1976) 29:2049–2054
Borenstein DG, O’Mara JW Jr, Boden SD, Lauerman WC, Jacobson A, Platenberg C, Schellinger D, Wiesel SW (2001) The value of magnetic resonance imaging of the lumbar spine to predict low-back pain in asymptomatic subjects: a seven-year follow-up study. J Bone Joint Surg Am 83-A:1306–1311
Salo S, Paajanen H, Alanen A (1995) Disc degeneration of pediatric patients in lumbar MRI. Pediatr Radiol 25:186–189
Samartzis D, Karppinen J, Mok F, Fong DY, Luk KD, Cheung KM (2011) A population-based study of juvenile disc degeneration and its association with overweight and obesity, low back pain, and diminished functional status. J Bone Joint Surg Am 93:662–670. doi:10.2106/JBJS.I.01568
American Academy of Pediatrics Committee on Sports Medicine and Fitness (1994) Medical conditions affecting sports participation. Pediatrics 94:757–760
Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 26:1873–1878
Hollenberg GM, Beattie PF, Meyers SP, Weinberg EP, Adams MJ (2002) Stress reactions of the lumbar pars interarticularis: the development of a new MRI classification system. Spine (Phila Pa 1976) 27:181–186
Benjamin HJ, Briner WW Jr (2005) Little league elbow. Clin J Sport Med 15:37–40
Klingele KE, Kocher MS (2002) Little league elbow: valgus overload injury in the paediatric athlete. Sports Med 32:1005–1015
Wall EJ (1998) Osgood-schlatter disease: practical treatment for a self-limiting condition. Phys Sportsmed 26:29–34. doi:10.3810/psm.1998.03.802
Soler T, Calderon C (2000) The prevalence of spondylolysis in the Spanish elite athlete. Am J Sports Med 28:57–62
Ruiz-Cotorro A, Balius-Matas R, Estruch-Massana AE, Vilaro Angulo J (2006) Spondylolysis in young tennis players. Br J Sports Med 40:441–446. doi:10.1136/bjsm.2005.023960 (discussion 446)
Noormohammadpour P, Rostami M, Mansournia MA, Farahbakhsh F, Pourgharib Shahi MH, Kordi R (2016) Low back pain status of female university students in relation to different sport activities. Eur Spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc 25:1196–1203. doi:10.1007/s00586-015-4034-7
Zaina F, Donzelli S, Lusini M, Minnella S, Negrini S (2015) Swimming and spinal deformities: a cross-sectional study. J Pediatr 166:163–167. doi:10.1016/j.jpeds.2014.09.024
Roy SL, Shaw PC, Beattie TF (2015) Low back pain in the paediatric athlete. Eur J Emerg Med Off J Eur Soc Emerg Med 22:348–354. doi:10.1097/MEJ.0000000000000154
Kujala UM, Kinnunen J, Helenius P, Orava S, Taavitsainen M, Karaharju E (1999) Prolonged low-back pain in young athletes: a prospective case series study of findings and prognosis. Eur Spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc 8:480–484
Acknowledgments
No funding was received for this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest specifically related to this work; however the authors have multiple conflicts that are not related to this work.
Rights and permissions
About this article
Cite this article
Schroeder, G.D., LaBella, C.R., Mendoza, M. et al. The role of intense athletic activity on structural lumbar abnormalities in adolescent patients with symptomatic low back pain. Eur Spine J 25, 2842–2848 (2016). https://doi.org/10.1007/s00586-016-4647-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4647-5