Abstract
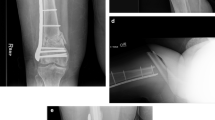
Inter-implant fractures are associated with reduced quality of life and increased 1-year mortality. For that reason, we propose, instead of treating, a novel, preventative surgical approach that involves splinting the inter-implant femoral shaft interval. In patients with a previous femoral implant in whom a second surgery for new material implantation was necessary (including knee or hip arthroplasty, plate or femoral nailing), an overlapping technique using the minimally invasive plate osteosynthesis technique was performed during the second surgery. Nine patients were included, all females with median (range) age of 78 (55–88) years. No surgery-related complications or mortality occurred. Two patients suffered fractures from a casual fall postoperatively with no implant failure or hospital admission required. In conclusion, instead of treating such fractures after they occur, we propose an effective, safe and reproducible preventative surgical approach, not previously reported, which involves internal femoral splinting, a plate and the minimally invasive plate osteosynthesis technique.




Similar content being viewed by others
References
Liporace FA, Yoon RS, Collinge CA (2017) Interprosthetic and peri-implant fractures: principles of operative fixation and future directions. J Orthop Trauma 31(5):287–292
Weiser L, Korecki MA, Sellenschloh K, Fensky F, Püschel K, Morlock MM et al (2014) The role of inter-prosthetic distance, cortical thickness and bone mineral density in the development of inter-prosthetic fractures of the femur: a biomechanical cadaver study. Bone Jt J 96-B(10):1378–1384
Kenny P, Rice J, Quinlan W (1998) Interprosthetic fracture of the femoral shaft. J Arthroplasty 13(3):361–364
Lyons RF, Piggott RP, Curtin W, Murphy CG (2018) Periprosthetic hip fractures: a review of the economic burden based on length of stay. J Orthop 15(1):118–121
Shields E, Behrend C, Bair J, Cram P, Kates S (2014) Mortality and financial burden of periprosthetic fractures of the femur. Geriatr Orthop Surg Rehabil 5(4):147–153
Rupprecht M, Sellenschloh K, Grossterlinden L, Püschel K, Morlock M, Amling M et al (2011) Biomechanical evaluation for mechanisms of periprosthetic femoral fractures. J Trauma 70(4):E62–E66
Lehmann W, Rupprecht M, Nuechtern J, Melzner D, Sellenschloh K, Kolb J et al (2012) What is the risk of stress risers for interprosthetic fractures of the femur? A biomechanical analysis. Int Orthop 36(12):2441–2446
Fu MC, Buerba RA, Grauer JN (2016) Preoperative nutritional status as an adjunct predictor of major postoperative complications following anterior cervical discectomy and fusion. Clin Spine Surg 29(4):167–172
Lohsiriwat V, Lohsiriwat D, Boonnuch W, Chinswangwatanakul V, Akaraviputh T, Lert-Akayamanee N (2008) Pre-operative hypoalbuminemia is a major risk factor for postoperative complications following rectal cancer surgery. World J Gastroenterol 14(8):1248–1251
Hou Z, Moore B, Bowen TR, Irgit K, Matzko ME, Strohecker KA et al (2011) Treatment of interprosthetic fractures of the femur. J Trauma 71(6):1715–1719
Funding
This research received no specific grants from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors David Campillo-Recio, Miquel Videla-Ces, Miquel Sales-Pérez, Guillem Molina-Olivella and Sebastian Videla declare that they have no conflict of interest. Dr. Miquel Videla-Cés is a Ph.D. candidate in the Universitat de Barcelona, Spain.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Campillo-Recio, D., Videla-Ces, M., Sales-Pérez, M. et al. Inter-implant fractures: an unmet medical need—a preventive approach proposal. Eur J Orthop Surg Traumatol 30, 539–543 (2020). https://doi.org/10.1007/s00590-019-02581-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-019-02581-6