Abstract
Objective
The aim of this study was to evaluate the remineralization ability of three endodontic sealer materials at different root dentin regions.
Material and methods
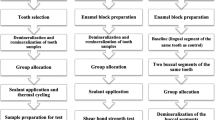
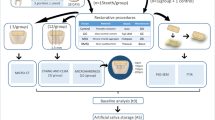
Cervical, medial, and apical root dentin surfaces were treated with two experimental hydroxyapatite-based cements, containing sodium hydroxide (calcypatite) or zinc oxide (oxipatite); an epoxy resin-based canal sealer, AH Plus; and gutta-percha. Remineralization, at the inner and outer zones of dentin disk surfaces, was studied by nanohardness (Hi) and Raman analysis. Nanoroughness and collagen fibrils width measurements were performed. Numerical data, at 24 h or 12 m, were analyzed by ANOVA and Student-Newman-Keuls (p < 0.05).
Results
At the outer and inner zones of the cervical dentin treated with oxipatite, the highest Hi after 12 m of immersion was achieved. The same group showed the highest intensity of phosphate peak, markers for calcification and crystallinity. Nanoroughness was lower and fibril diameter was higher at the inner zone of the dentin treated with oxipatite. Dentin mineralization occurred in every region of the root dentin treated with oxipatite and calcypatite, especially at the inner zone of the dentin after 12 m.
Conclusions
Oxipatite reinforced the inner root zone at any third of the radicular dentin, by increasing both nanohardness and remineralization. When using calcypatite, the highest nanohardness was found at the apical third of the inner root dentin, but the lowest mechanical performance was obtained at the cervical and the medial thirds of the roots. Therefore, application of oxipatite as sealing cement of root canals is recommended.
Clinical relevance
Oxipatite, when used as an endodontic sealing material, strengthens radicular dentin.







Similar content being viewed by others
References
Huynh N, Li F-C, Friedman S, Kishen A (2018) Biomechanical effects of bonding pericervical dentin in maxillary premolars. J Endod 44:659–664. https://doi.org/10.1016/j.joen.2018.01.002
Brosh T, Metzger Z, Pilo R (2018) Circumferential root strains generated during lateral compaction with stainless steel vs. nickel-titanium finger spreaders. Eur J Oral Sci 126:518–525. https://doi.org/10.1111/eos.12569
Chai H, Tamse A (2018) Vertical root fracture in buccal roots of bifurcated maxillary premolars from condensation of gutta-percha. J Endod 44:1159–1163. https://doi.org/10.1016/j.joen.2018.03.017
Patil P, Banga KS, Pawar AM, Pimple S, Ganeshan R (2017) Influence of root canal obturation using gutta-percha with three different sealers on root reinforcement of endodontically treated teeth. An in vitro comparative study of mandibular incisors. J Conserv Dent 20:241–244. https://doi.org/10.4103/JCD.JCD_233_16
Marshall GW, Marshall SJ, Kinney JH, Balooch M (1997) The dentin substrate: structure and properties related to bonding. J Dent 25:441–458
Kinney JH, Nalla RK, Pople JA, Breunig TM, Ritchie RO (2005) Age-related transparent root dentin: mineral concentration, crystallite size, and mechanical properties. Biomaterials 26:3363–3376. https://doi.org/10.1016/j.biomaterials.2004.09.004
Nalla RK, Kinney JH, Ritchie RO (2003) Effect of orientation on the in vitro fracture toughness of dentin: the role of toughening mechanisms. Biomaterials 24:3955–3968
Cheron RA, Marshall SJ, Goodis HE, Peters OA (2011) Nanomechanical properties of endodontically treated teeth. J Endod 37:1562–1565. https://doi.org/10.1016/j.joen.2011.08.006
Chu C-Y, Kuo T-C, Chang S-F, Shyu YC, Lin CP (2010) Comparison of the microstructure of crown and root dentin by a scanning electron microscopic study. J Dent Sci 5:14–20. https://doi.org/10.1016/S1991-7902(10)60003-7
Toledano M, Pérez-Álvarez MC, Aguilera FS et al (2017) A zinc oxide-modified hydroxyapatite-based cement facilitated new crystalline-stoichiometric and amorphous apatite precipitation on dentine. Int Endod J 50(Suppl 2):e109–e119. https://doi.org/10.1111/iej.12807
Toledano M, Osorio R, Pérez-Álvarez M-C et al (2018) A zinc-doped endodontic cement facilitates functional mineralization and stress dissipation at the dentin surface. Med Oral Patol Oral Cirugia Bucal 23:e646–e655. https://doi.org/10.4317/medoral.22751
Gandolfi MG, Ciapetti G, Taddei P, Perut F, Tinti A, Cardoso MV, van Meerbeek B, Prati C (2010) Apatite formation on bioactive calcium-silicate cements for dentistry affects surface topography and human marrow stromal cells proliferation. Dent Mater 26:974–992. https://doi.org/10.1016/j.dental.2010.06.002
Osorio R, Sauro S, Watson TF, Toledano M (2016) Polyaspartic acid enhances dentine remineralization bonded with a zinc-doped Portland-based resin cement. Int Endod J 49:874–883. https://doi.org/10.1111/iej.12518
Hakki SS, Bozkurt BS, Ozcopur B, Gandolfi MG, Prati C, Belli S (2013) The response of cementoblasts to calcium phosphate resin-based and calcium silicate-based commercial sealers. Int Endod J 46:242–252. https://doi.org/10.1111/j.1365-2591.2012.02122.x
Kitikuson P, Srisuwan T (2016) Attachment ability of human apical papilla cells to root dentin surfaces treated with either 3Mix or calcium hydroxide. J Endod 42:89–94. https://doi.org/10.1016/j.joen.2015.08.021
Miñana M, Carnes DL, Walker WA (2001) PH changes at the surface of root dentin after intracanal dressing with calcium oxide and calcium hydroxide. J Endod 27:43–45. https://doi.org/10.1097/00004770-200101000-00015
Al-Sanabani JS, Madfa AA, Al-Sanabani FA (2013) Application of calcium phosphate materials in dentistry. Int J Biomater 2013:876132. https://doi.org/10.1155/2013/876132
Matsunaga K (2008) First-principles study of substitutional magnesium and zinc in hydroxyapatite and octacalcium phosphate. J Chem Phys 128:245101. https://doi.org/10.1063/1.2940337
Viapiana R, Guerreiro-Tanomaru JM, Hungaro-Duarte MA, Tanomaru-Filho M, Camilleri J (2014) Chemical characterization and bioactivity of epoxy resin and Portland cement-based sealers with niobium and zirconium oxide radiopacifiers. Dent Mater 30:1005–1020. https://doi.org/10.1016/j.dental.2014.05.007
Balooch M, Habelitz S, Kinney JH, Marshall SJ, Marshall GW (2008) Mechanical properties of mineralized collagen fibrils as influenced by demineralization. J Struct Biol 162:404–410. https://doi.org/10.1016/j.jsb.2008.02.010
Poon B, Rittel D, Ravichandran G (2008) An analysis of nanoindentation in linearly elastic solids. Int J Solids Struct 45:6018–6033. https://doi.org/10.1016/j.ijsolstr.2008.07.021
Xu H, Zheng Q, Shao Y, Song F, Zhang L, Wang Q, Huang D (2014) The effects of ageing on the biomechanical properties of root dentine and fracture. J Dent 42:305–311. https://doi.org/10.1016/j.jdent.2013.11.025
Ossareh A, Rosentritt M, Kishen A (2018) Biomechanical studies on the effect of iatrogenic dentin removal on vertical root fractures. J Conserv Dent JCD 21:290–296. https://doi.org/10.4103/JCD.JCD_126_18
Kunstar A, Leijten J, van Leuveren S, Hilderink J, Otto C, van Blitterswijk CA, Karperien M, van Apeldoorn AA (2012) Recognizing different tissues in human fetal femur cartilage by label-free Raman microspectroscopy. J Biomed Opt 17:116012. https://doi.org/10.1117/1.JBO.17.11.116012
Toledano M, Aguilera FS, Osorio E, López-López MT, Cabello I, Toledano-Osorio M, Osorio R (2015) On modeling and nanoanalysis of caries-affected dentin surfaces restored with Zn-containing amalgam and in vitro oral function. Biointerphases 10:041004. https://doi.org/10.1116/1.4933243
Wang L, Zhao Y, Mei L, Yu H, Muhammad I, Pan Y, Huang S (2017) Effect of application time of maleic acid on smear layer removal and mechanical properties of root canal dentin. Acta Odontol Scand 75:59–66. https://doi.org/10.1080/00016357.2016.1248789
Verdelis K, Eliades G, Oviir T, Margelos J (1999) Effect of chelating agents on the molecular composition and extent of decalcification at cervical, middle and apical root dentin locations. Endod Dent Traumatol 15:164–170
O’Connell MS, Morgan LA, Beeler WJ, Baumgartner JC (2000) A comparative study of smear layer removal using different salts of EDTA. J Endod 26:739–743. https://doi.org/10.1097/00004770-200012000-00019
Mestres G, Aguilera FS, Manzanares N, Sauro S, Osorio R, Toledano M, Ginebra MP (2014) Magnesium phosphate cements for endodontic applications with improved long-term sealing ability. Int Endod J 47:127–139. https://doi.org/10.1111/iej.12123
Monticelli F, Osorio R, Toledano M, Ferrari M, Pashley DH, Tay FR (2010) Sealing properties of one-step root-filling fibre post-obturators vs. two-step delayed fibre post-placement. J Dent 38:547–552. https://doi.org/10.1016/j.jdent.2010.03.014
Vizgirda PJ, Liewehr FR, Patton WR et al (2004) A comparison of laterally condensed gutta-percha, thermoplasticized gutta-percha, and mineral trioxide aggregate as root canal filling materials. J Endod 30:103–106. https://doi.org/10.1097/00004770-200402000-00010
Bouillaguet S, Shaw L, Barthelemy J, Krejci I, Wataha JC (2008) Long-term sealing ability of Pulp Canal Sealer, AH-Plus, GuttaFlow and Epiphany. Int Endod J 41:219–226. https://doi.org/10.1111/j.1365-2591.2007.01343.x
Ryou H, Niu L-N, Dai L, Pucci CR, Arola DD, Pashley DH, Tay FR (2011) Effect of biomimetic remineralization on the dynamic nanomechanical properties of dentin hybrid layers. J Dent Res 90:1122–1128. https://doi.org/10.1177/0022034511414059
Toledano M, Sauro S, Cabello I, Watson T, Osorio R (2013) A Zn-doped etch-and-rinse adhesive may improve the mechanical properties and the integrity at the bonded-dentin interface. Dent Mater 29:e142–e152. https://doi.org/10.1016/j.dental.2013.04.024
Habelitz S, Balooch M, Marshall SJ, Balooch G, Marshall GW Jr (2002) In situ atomic force microscopy of partially demineralized human dentin collagen fibrils. J Struct Biol 138:227–236
Takeyasu K, Omote H, Nettikadan S, Tokumasu F, Iwamoto-Kihara A, Futai M (1996) Molecular imaging of Escherichia coli F0F1-ATPase in reconstituted membranes using atomic force microscopy. FEBS Lett 392:110–113
Ager JW, Nalla RK, Breeden KL, Ritchie RO (2005) Deep-ultraviolet Raman spectroscopy study of the effect of aging on human cortical bone. J Biomed Opt 10:034012. https://doi.org/10.1117/1.1924668
Toledano M, Osorio R, Osorio E, García-Godoy F, Toledano-Osorio M, Aguilera FS (2016) Advanced zinc-doped adhesives for high performance at the resin-carious dentin interface. J Mech Behav Biomed Mater 62:247–267. https://doi.org/10.1016/j.jmbbm.2016.05.013
Timlin JA, Carden A, Morris MD, Rajachar RM, Kohn DH (2000) Raman spectroscopic imaging markers for fatigue-related microdamage in bovine bone. Anal Chem 72:2229–2236. https://doi.org/10.1021/ac9913560
Lussi A, Schlueter N, Rakhmatullina E, Ganss C (2011) Dental erosion—an overview with emphasis on chemical and histopathological aspects. Caries Res 45(Suppl 1):2–12. https://doi.org/10.1159/000325915
Schwartz AG, Pasteris JD, Genin GM, Daulton TL, Thomopoulos S (2012) Mineral distributions at the developing tendon enthesis. PLoS One 7:e48630. https://doi.org/10.1371/journal.pone.0048630
Salehi H, Terrer E, Panayotov I et al (2013) Functional mapping of human sound and carious enamel and dentin with Raman spectroscopy. J Biophotonics 6:765–774. https://doi.org/10.1002/jbio.201200095
Wang C, Wang Y, Huffman NT, Cui C, Yao X, Midura S, Midura RJ, Gorski JP (2009) Confocal laser Raman microspectroscopy of biomineralization foci in UMR 106 osteoblastic cultures reveals temporally synchronized protein changes preceding and accompanying mineral crystal deposition. J Biol Chem 284:7100–7113. https://doi.org/10.1074/jbc.M805898200
Kaushik M, Kumar U, Sharma R, Mehra N, Rathi A (2018) Stress distribution in endodontically treated abfracted mandibular premolar restored with different cements and crowns: a three-dimensional finite element analysis. J Conserv Dent 21:557–561. https://doi.org/10.4103/JCD.JCD_206_18
Toledano M, Osorio R, Osorio E, Medina-Castillo AL, Toledano-Osorio M, Aguilera FS (2017) Ions-modified nanoparticles affect functional remineralization and energy dissipation through the resin-dentin interface. J Mech Behav Biomed Mater 68:62–79. https://doi.org/10.1016/j.jmbbm.2017.01.026
Bertassoni LE, Stankoska K, Swain MV (2012) Insights into the structure and composition of the peritubular dentin organic matrix and the lamina limitans. Micron Oxf Engl 1993 43:229–236. https://doi.org/10.1016/j.micron.2011.08.003
Clarkson BH, McCurdy SP, Gaz D, Hand AR (1993) Effects of phosphoprotein on collagen fibril formation in vitro. Arch Oral Biol 38:737–743. https://doi.org/10.1016/0003-9969(93)90068-W
He G, George A (2004) Dentin matrix protein 1 immobilized on type I collagen fibrils facilitates apatite deposition in vitro. J Biol Chem 279:11649–11656. https://doi.org/10.1074/jbc.M309296200
Tramini P, Pélissier B, Valcarcel J, Bonnet B, Maury L (2000) A Raman spectroscopic investigation of dentin and enamel structures modified by lactic acid. Caries Res 34:233–240. https://doi.org/10.1159/000016596
Liu Y, Tjäderhane L, Breschi L, Mazzoni A, Li N, Mao J, Pashley DH, Tay FR (2011) Limitations in bonding to dentin and experimental strategies to prevent bond degradation. J Dent Res 90:953–968. https://doi.org/10.1177/0022034510391799
Low I-M (2004) Depth-profiling of crystal structure, texture, and microhardness in a functionally graded tooth enamel. J Am Ceram Soc 87:2125–2131. https://doi.org/10.1111/j.1151-2916.2004.tb06369.x
Toledano M, Aguilera FS, Osorio E, Cabello I, Toledano-Osorio M, Osorio R (2015) Self-etching zinc-doped adhesives improve the potential of caries-affected dentin to be functionally remineralized. Biointerphases 10:031002. https://doi.org/10.1116/1.4926442
Bertassoni LE, Habelitz S, Pugach M, Soares PC, Marshall SJ, Marshall GW Jr (2010) Evaluation of surface structural and mechanical changes following remineralization of dentin. Scanning 32:312–319. https://doi.org/10.1002/sca.20199
Mayer I, Apfelbaum F, Featherstone JDB (1994) Zinc ions in synthetic carbonated hydroxyapatites. Arch Oral Biol 39:87–90. https://doi.org/10.1016/0003-9969(94)90040-X
Li Y, Chen X, Fok A, Rodriguez-Cabello JC, Aparicio C (2015) Biomimetic mineralization of recombinamer-based hydrogels toward controlled morphologies and high mineral density. ACS Appl Mater Interfaces 7:25784–25792. https://doi.org/10.1021/acsami.5b07628
Tay FR, Pashley DH, Rueggeberg FA, Loushine RJ, Weller RN (2007) Calcium phosphate phase transformation produced by the interaction of the Portland cement component of white mineral trioxide aggregate with a phosphate-containing fluid. J Endod 33:1347–1351. https://doi.org/10.1016/j.joen.2007.07.008
Gandolfi MG, Prati C (2010) MTA and F-doped MTA cements used as sealers with warm gutta-percha. Long-term study of sealing ability. Int Endod J 43:889–901. https://doi.org/10.1111/j.1365-2591.2010.01763.x
Tay FR, Pashley DH (2007) Monoblocks in root canals: a hypothetical or a tangible goal. J Endod 33:391–398. https://doi.org/10.1016/j.joen.2006.10.009
Mohammadi Z, Dummer PMH (2011) Properties and applications of calcium hydroxide in endodontics and dental traumatology. Int Endod J 44:697–730. https://doi.org/10.1111/j.1365-2591.2011.01886.x
Jainaen A, Palamara JEA, Messer HH (2009) The effect of resin-based sealers on fracture properties of dentine. Int Endod J 42:136–143. https://doi.org/10.1111/j.1365-2591.2008.01496.x
Gandolfi MG, Taddei P, Modena E, Siboni F, Prati C (2013) Biointeractivity-related versus chemi/physisorption-related apatite precursor-forming ability of current root end filling materials. J Biomed Mater Res B Appl Biomater 101:1107–1123. https://doi.org/10.1002/jbm.b.32920
Ryou H, Amin N, Ross A, Eidelman N, Wang DH, Romberg E, Arola D (2011) Contributions of microstructure and chemical composition to the mechanical properties of dentin. J Mater Sci Mater Med 22:1127–1135. https://doi.org/10.1007/s10856-011-4293-8
Ramakrishnaiah R, ur Rehman G, Basavarajappa S et al (2015) Applications of Raman spectroscopy in dentistry: analysis of tooth structure. Appl Spectrosc Rev 50:332–350. https://doi.org/10.1080/05704928.2014.986734
Daood U, Iqbal K, Nitisusanta LI, Fawzy AS (2013) Effect of chitosan/riboflavin modification on resin/dentin interface: spectroscopic and microscopic investigations. J Biomed Mater Res A 101:1846–1856. https://doi.org/10.1002/jbm.a.34482
Toledano M, Cabello I, Osorio E, et al (2018) Zn-containing polymer nanogels promote cervical dentin remineralization
Bakland LK, Andreasen JO (2012) Will mineral trioxide aggregate replace calcium hydroxide in treating pulpal and periodontal healing complications subsequent to dental trauma? A review. Dent Traumatol 28:25–32. https://doi.org/10.1111/j.1600-9657.2011.01049.x
Acknowledgements
Project MAT2017-85999-P MINECO/AEI/FEDER/UE supported by the Ministry of Economy and Competitiveness and European Regional Development Fund.
Funding
Project MAT2017-85999-P MINECO/AEI/FEDER/UE supported by the Ministry of Economy and Competitiveness (MINECO) and European Regional Development Fund (FEDER).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the present study, involving human participants, were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Toledano, M., Muñoz-Soto, E., Aguilera, F.S. et al. The mineralizing effect of zinc oxide-modified hydroxyapatite-based sealer on radicular dentin. Clin Oral Invest 24, 285–299 (2020). https://doi.org/10.1007/s00784-019-02938-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-02938-5