Abstract
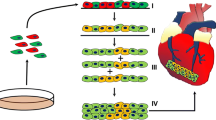
Recently, the tubular shape has been suggested as an effective geometry for tissue-engineered heart valves, allowing easy fabrication, fast implantation, and a minimal crimped footprint from a transcatheter delivery perspective. This simple design is well suited for the self-assembly method, with which the only support for the cells is the extracellular matrix they produce, allowing the tissue to be completely free from exogenous materials during its entire fabrication process. Tubular constructs were produced by rolling self-assembled human fibroblast sheets on plastic mandrels. After maturation, the tubes were transferred onto smaller diameter mandrels and allowed to contract freely. This precontraction phase thickened the tissue and prevented further contraction, while improving fusion between the self-assembled layers and aligning the cells circumferentially. When mounted in a pulsed-flow bioreactor, the valves showed good functionality with large leaflets coaptation and opening area. Although physiological aortic flow conditions were not reached, the leaflets could withstand a 1 Hz pulsed flow with a 300 mL/s peak flow rate and a 70 mmHg peak transvalvular pressure. This study shows that the self-assembly method, which has already proven its potential for the production of small diameter vascular grafts, could also be used to achieve functional tubular heart valves.








Similar content being viewed by others
References
Arjunon, S., S. Rathan, H. Jo, and A. P. Yoganathan. Aortic valve: mechanical environment and mechanobiology. Ann. Biomed. Eng. 41:1331–1346, 2013.
Auger, F. A., F. Berthod, V. Moulin, R. Pouliot, and L. Germain. Tissue-engineered skin substitutes: from in vitro constructs to in vivo applications. Biotechnol. Appl. Biochem. 39:263–275, 2004.
Axis Research Mind. Prosthetic heart valves—global trends, estimates and forecasts, 2012–2018. Report code: ARMMR119N.1, 2014.
Aymard, T., A. Kadner, N. Walpoth, V. Göber, L. Englberger, M. Stalder, F. Eckstein, C. Zobrist, and T. Carrel. Clinical experience with the second-generation 3f Enable sutureless aortic valve prosthesis. J. Thorac. Cardiovasc. Surg. 140:313–316, 2010.
Bouhout, S., E. Perron, R. Gauvin, G. Bernard, G. Ouellet, V. Cattan, and S. Bolduc. In vitro reconstruction of an autologous, watertight, and resistant vesical equivalent. Tissue Eng. Part A 16:1539–1548, 2010.
Bourget, J. M., R. Gauvin, D. Larouche, A. Lavoie, R. Labbé, F. A. Auger, and L. Germain. Human fibroblast-derived ECM as a scaffold for vascular tissue engineering. Biomaterials 33:9205–9213, 2012.
Cheng, C. P., R. J. Herfkens, A. L. Lightner, C. A. Taylor, and J. A. Feinstein. Blood flow conditions in the proximal pulmonary arteries and vena cavae: healthy children during upright cycling exercise. Am. J. Physiol. Heart Circ. Physiol. 287:H921–H926, 2004.
Cox, J. L., N. Ad, K. Myers, M. Gharib, and R. C. Quijano. Tubular heart valves: a new tissue prosthesis design: preclinical evaluation of the 3F aortic bioprosthesis. J. Thorac. Cardiovasc. Surg. 130:520–527, 2005.
Dubé, J., J. M. Bourget, R. Gauvin, H. Lafrance, C. J. Roberge, F. A. Auger, and L. Germain. Progress in developing a living human tissue-engineered tri-leaflet heart valve assembled from tissue produced by the self-assembly approach. Acta Biomater. 10:3563–3570, 2014.
Flanagan, T. C., J. S. Sachweh, J. Frese, H. Schnöring, N. Gronloh, S. Koch, R. H. Tolba, T. Schmitz-Rode, and S. Jockenhoevel. In vivo remodeling and structural characterization of fibrin-based tissue-engineering heart valves in the adult sheep model. Tissue Eng. Part A 15:2965–2976, 2009.
Guillemette, M. D., B. Cui, E. Roy, R. Gauvin, C. J. Giasson, M. B. Esch, P. Carrier, A. Deschambeault, M. Dumoulin, M. Toner, L. Germain, T. Veres, and F. A. Auger. Surface topography induces 3D self-orientation of cells and extracellular matrix resulting in improved tissue function. Integr. Biol. (Camb.) 1:196–204, 2009.
Hoerstrup, S. P., R. Sodian, S. Daebritz, J. Wang, E. A. Bacha, D. P. Martin, A. M. Moran, K. J. Guleserian, J. S. Sperling, S. Kaushal, J. P. Vacanti, F. J. Schoen, and J. E. Mayer, Jr. Functional living trileaflet heart valves grown in vitro. Circulation 102:44–49, 2000.
Kheradvar, A., E. M. Groves, L. P. Dasi, S. H. Alavi, R. Tranquillo, K. J. Grande-Allen, C. A. Simmons, B. Griffith, A. Falahatpisheh, C. J. Goergen, M. R. Mofrad, F. Baaijens, S. H. Little, and S. Canic. Emerging trends in heart valve engineering: part I—solutions for future. Ann. Biomed. Eng. 43:833–843, 2015.
Kheradvar, A., E. M. Groves, C. J. Goergen, S. H. Alavi, R. Tranquillo, C. A. Simmons, L. P. Dasi, K. J. Grande-Allen, M. R. Mofrad, A. Falahatpisheh, B. Griffith, F. Baaijens, S. H. Little, and S. Canic. Emerging trends in heart valve engineering: part II—novel and standard technologies for aortic valve replacement. Ann. Biomed. Eng. 43:844–857, 2015.
Konduri, S. The influence of normal physiological forces on porcine aortic heart valves in a sterile ex vivo pulsatile organ culture system. M.Sc. Thesis, Georgia Institute of Technology, Atlanta, GA, 2005.
Laterreur, V., J. Ruel, F. A. Auger, K. Vallières, C. Tremblay, D. Lacroix, M. Tondreau, J. M. Bourget, and L. Germain. Comparison of the direct burst pressure and the ring tensile test methods for mechanical characterization of tissue-engineered vascular substitutes. J. Mech. Behav. Biomed. Mater. 34:253–263, 2014.
L’Heureux, N., T. McAllister, N. Dusserre. Tissue-engineered heart valve for transcatheter repair. U.S. Patent WO 2013142879 A1, 2013.
L’Heureux, N., S. Paquet, R. Labbe, L. Germain, and F. A. Auger. A completely biological tissue-engineered human blood vessel. FASEB J. 12:47–56, 1998.
MacGrogan, D., G. Luxán, A. Driessen-Mol, C. Bouten, F. Baaijens, and J. L. de la Pompa. How to make a heart valve: from embryonic development to bioengineering of living valve substitutes. Cold Spring Harb. Perspect. Med. 4:a013912, 2014.
Martens, S., A. Ploss, S. Sirat, A. Miskovic, A. Moritz, and M. Doss. Sutureless aortic valve replacement with the 3f enable aortic bioprosthesis. Ann. Thorac. Surg. 87:1914–1918, 2009.
Misfeld, M., and H. H. Sievers. Heart valve macro- and microstructure. Philos. Trans. R. Soc. Lond. B 362:1421–1436, 2007.
Mol, A. Functional tissue engineering of human heart valve leaflets. Ph.D. Thesis, Eindhoven University of Technology, Eindhoven, The Netherlands, 2005.
Moreira, R., T. Velz, N. Alves, V. N. Gesche, A. Malischewski, T. Schmitz-Rode, J. Frese, S. Jockenhoevel, and P. Mela. Tissue-engineered heart valve with a tubular leaflet design for minimally invasive transcatheter implantation. Tissue Eng. Part C 21:530–540, 2015.
Mueller, X. M., and L. K. von Segesser. A new equine pericardial stentless valve. J. Thorac. Cardiovasc. Surg. 125:1405–1411, 2003.
Proulx, S., and I. Brunette. methods being developed for preparation, delivery and transplantation of a tissue-engineered corneal endothelium. Exp. Eye Res. 95:68–75, 2012.
Proulx, S., J. Fradette, R. Gauvin, D. Larouche, and L. Germain. Stem cells of the skin and cornea: their clinical applications in regenerative medicine. Curr. Opin. Organ. Transplant. 16:83–89, 2011.
Reimer, J. M., Z. H. Syedain, B. H. Haynie, and R. T. Tranquillo. Pediatric tubular pulmonary heart valve from decellularized engineered tissue tubes. Biomaterials 62:88–94, 2015.
Ruel, J., and G. Lachance. A new bioreactor for the development of tissue-engineered heart valves. Ann. Biomed. Eng. 37:674–681, 2009.
Ruel, J., and G. Lachance. Mathematical modeling and experimental testing of three bioreactor configurations based on windkessel models. Heart Int. 5:1–6, 2010.
Sauter, J. Evaluation of bioprosthetic valve performance as a function of geometric orifice area and space efficiency—a reliable alternative to effective orifice area. In: Aortic root surgery, the biological solution, edited by A. C. Yankah, Y. Weng, and R. Hetzer. New-York: Springer, 2010, pp. 313–337.
Silbernagl, S., and A. Despopoulos. Atlas de physiologie. Paris: Flammarion Médecine-Sciences, 2008.
Stradins, P., R. Lacis, I. Ozolanta, B. Purina, V. Ose, L. Feldmane, and V. Kasyanov. Comparison of biomechanical and structural properties between human aortic and pulmonary valve. Eur. J. Cardiothorac. Surg. 26:634–639, 2004.
Syedain, Z. H., A. R. Bradee, S. Kren, D. A. Taylor, and R. T. Tranquillo. Decellularized tissue-engineered heart valve leaflets with recellularization potential. Tissue Eng. Part A 19:759–769, 2013.
Syedain, Z. H., M. T. Lahti, S. L. Johnson, P. S. Robinson, G. R. Ruth, R. W. Bianco, and R. T. Tranquillo. Implantation of a tissue-engineered heart valve from human fibroblasts exhibiting short term function in the sheep pulmonary artery. Cardiovasc. Eng. Technol. 2:101–112, 2011.
Syedain, Z. H., L. A. Meier, J. M. Reimer, and R. T. Tranquillo. Tubular heart valves from decellularized engineered tissue. Ann. Biomed. Eng. 41:2645–2654, 2013.
Tondreau, M. Y., V. Laterreur, R. Gauvin, K. Vallières, J. M. Bourget, D. Lacroix, C. Tremblay, L. Germain, J. Ruel, and F. A. Auger. Mechanical properties of endothelialized fibroblast-derived vascular scaffolds stimulated in a bioreactor. Acta Biomater. 18:176–185, 2015.
Tremblay, C., J. Ruel, J. M. Bourget, V. Laterreur, K. Vallières, M. Y. Tondreau, D. Lacroix, L. Germain, and F. A. Auger. A new construction technique for tissue-engineered heart valves using the self-assembly method. Tissue Eng. Part C 20:905–915, 2014.
Weber, B., P. E. Dijkman, J. Scherman, B. Sanders, M. Y. Emmert, J. Grünenfelder, R. Verbeek, M. Bracher, M. Black, T. Franz, J. Kortsmit, P. Modregger, S. Peter, M. Stampanoni, J. Robert, D. Kehl, M. van Doeselaar, M. Schweiger, C. E. Brokopp, T. Wälchli, V. Falk, P. Zilla, A. Driessen-Mol, F. P. Baaijens, and S. P. Hoerstrup. Off-the-shelf human decellularized tissue-engineered heart valves in a non-human primate model. Biomaterials 34:7269–7280, 2013.
Weber, M., E. Heta, R. Moreira, V. N. Gesche, T. Schermer, J. Frese, S. Jockenhoevel, and P. Mela. Tissue-engineered fibrin-based heart valve with a tubular leaflet design. Tissue Eng. Part C 20:265–275, 2014.
Acknowledgments
This research was funded by the Fonds de recherche du Québec—Nature et technologies (FRQNT), the Fonds de Recherche du Québec—Santé (FRQS) and ThéCell Network: Réseau de thérapie cellulaire et tissulaire du FRQS, the Canadian Institute for Health Research (CIHR) and the Natural Sciences and Engineering Research Council of Canada (NSERC). M.P.D. and C.T. were the recipients of scholarships from the NSERC and worked under the direction of J.R. and F.A.A. The authors would also like to thank Véronique Laterreur, Dan Lacroix, Cindy Perron and Maxime Tondreau for their generous time and knowledge contributions on tissue engineering and Marc-André Plourde-Campagna, Jean-Claude Gariépy and Pierre Carrier for their essential technical assistance on mechanical design and fabrication.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Lakshmi Prasad Dasi oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Picard-Deland, M., Ruel, J., Galbraith, T. et al. Tissue-Engineered Tubular Heart Valves Combining a Novel Precontraction Phase with the Self-Assembly Method. Ann Biomed Eng 45, 427–438 (2017). https://doi.org/10.1007/s10439-016-1708-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-016-1708-1