Abstract
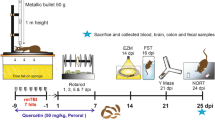
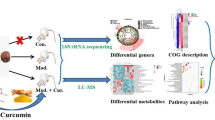
Repetitive mild traumatic brain injury (rmTBI) is associated with a range of neural changes which is characterized by axonal injury and neuroinflammation. Ketogenic diet (KD) is regarded as a potential therapy for facilitating recovery after moderate-severe traumatic brain injury (TBI). However, its effect on rmTBI has not been fully studied. In this study, we evaluated the anti-neuroinflammation effects of KD after rmTBI in adolescent mice and explored the potential mechanisms. Experimentally, specific pathogen-free (SPF) adolescent male C57BL/6 mice received a sham surgery or repetitive mild controlled cortical impacts consecutively for 7 days. The uninjured mice received the standard diet, and the mice with rmTBI were fed either the standard diet or KD for 7 days. One week later, all mice were subjected to behavioral tests and experimental analysis. Results suggest that KD significantly increased blood beta-hydroxybutyrate (β-HB) levels and improved neurological function. KD also reduced white matter damage, microgliosis, and astrogliosis induced by rmTBI. Aryl hydrocarbon receptor (AHR) signaling pathway, which was mediated by indole-3-acetic acid (3-IAA) from Lactobacillus reuteri (L. reuteri) in gut and activated in microglia and astrocytes after rmTBI, was inhibited by KD. The expression level of the toll-like receptor 4 (TLR4)/myeloid differentiation primary response 88 (MyD88) in inflammatory cells, which mediates the NF-κB pathway, was also attenuated by KD. Taken together, our results indicated that KD can promote recovery following rmTBI in adolescent mice. KD may modulate neuroinflammation by altering L. reuteri in gut and its metabolites. The inhibition of indole/AHR pathway and the downregulation of TLR4/MyD88 may play a role in the beneficial effect of KD against neuroinflammation in rmTBI mice.
Graphical abstract









Similar content being viewed by others
Data Availability
The original contributions presented in the study are included in the article. Further inquiries can be directed to the corresponding author.
Abbreviations
- 3-IAA:
-
Indole-3-acetic-acid
- AHR:
-
Aryl hydrocarbon receptor
- β-HB:
-
Beta-hydroxybutyrate
- CXCL1:
-
Chemokine (C-X-C motif) ligand 1
- CCI:
-
Controlled cortical impact
- DTI:
-
Diffusion tensor imaging
- ELISA:
-
Enzyme-linked immunosorbent assay
- FA:
-
Fractional anisotropy
- GFAP:
-
Glial fibrillary acidic protein
- HE:
-
Hematoxylin and eosin
- IL-1β:
-
Interleukin β1
- IRF-3:
-
Interferon regulatory Factor 3
- Iba-1:
-
Ionized calcium-binding adapter molecule 1
- KD:
-
Ketogenic diet
- MyD88:
-
Myeloid differentiation primary response 88
- MCT1:
-
Monocarboxylate transporter 1
- MD:
-
Mean diffusivity
- NF-κB:
-
Nuclear factor kappa light chain enhancer of activated B cells
- OCT:
-
Optimal cutting temperature compound
- PBS:
-
Phosphate-buffered saline
- rmTBI:
-
Repetitive mild traumatic brain injury
- TLR4:
-
Toll-like receptor 4
- TNF:
-
Tumor necrosis factor
References
Agus A et al (2018) Gut microbiota regulation of tryptophan metabolism in health and disease. Cell Host Microbe 23(6):716–724. https://doi.org/10.1016/j.chom.2018.05.003
Ameen-Ali K et al (2015) Moving beyond standard procedures to assess spontaneous recognition memory. Neurosci Biobehav Rev 53:37–51. https://doi.org/10.1016/j.neubiorev.2015.03.013
Appelberg KS et al (2009) The effects of a ketogenic diet on behavioral outcome after controlled cortical impact injury in the juvenile and adult rat. J Neurotrauma 26(4):497–506. https://doi.org/10.1089/neu.2008.0664
Blanco MMB et al (2016) Cerebral metabolism and the role of glucose control in acute traumatic brain injury. Neurosurg Clin 27(4):453–463. https://doi.org/10.1016/j.nec.2016.05.003
Cervantes-Barragan L et al (2017) Lactobacillus reuteri induces gut intraepithelial CD4+ CD8αα+ T cells. Science 357(6353):806–810. https://doi.org/10.1126/science.aah5825
Chen W-C et al (2019) Aryl hydrocarbon receptor modulates stroke-induced astrogliosis and neurogenesis in the adult mouse brain. J Neuroinflammation 16(1):1–13. https://doi.org/10.1186/s12974-019-1572-7
Constante M et al (2021) Saccharomyces boulardii CNCM I-745 modulates the microbiota–gut–brain axis in a humanized mouse model of Irritable Bowel Syndrome. Neurogastroenterol Motil 33(3):e13985. https://doi.org/10.1111/nmo.13985
Davenport EM et al (2016) Abnormalities in diffusional kurtosis metrics related to head impact exposure in a season of high school varsity football. J Neurotrauma 33(23):2133–2146. https://doi.org/10.1089/neu.2015.4267
Ding M et al (2021) Microbiota–gut–brain axis and epilepsy: a review on mechanisms and potential therapeutics. Front Immunol 4131. https://doi.org/10.3389/fimmu.2021.742449
Dowling C, Allen NJ (2018) Mice lacking glypican 4 display juvenile hyperactivity and adult social interaction deficits. Brain Plasticity 4(2):197–209. https://doi.org/10.3233/BPL-180079
Gao K et al (2020) Tryptophan metabolism: a link between the gut microbiota and brain. Adv Nutr 11(3):709–723. https://doi.org/10.1093/advances/nmz127
Garrett L et al (2020) A truncating Aspm allele leads to a complex cognitive phenotype and region-specific reductions in parvalbuminergic neurons. Transl Psychiatry 10(1):1–14. https://doi.org/10.1038/s41398-020-0686-0
Guan Y-F et al (2020) Anti-depression effects of ketogenic diet are mediated via the restoration of microglial activation and neuronal excitability in the lateral habenula. Brain Behav Immun 88:748–762. https://doi.org/10.1016/j.bbi.2020.05.032
Gzielo K et al (2019) The impact of the ketogenic diet on glial cells morphology. A quantitative morphological analysis. Neuroscience 413:239–251. https://doi.org/10.1016/j.neuroscience.2019.06.009
Hofstetter S, Assaf Y (2017) The rapid development of structural plasticity through short water maze training: A DTI study. Neuroimage 155:202–208. https://doi.org/10.1016/j.neuroimage.2017.04.056
Hylin MJ et al (2013) Behavioral and histopathological alterations resulting from mild fluid percussion injury. J Neurotrauma 30(9):702–715. https://doi.org/10.1089/neu.2012.2630
Jomehzadeh N et al (2020) Quantification of intestinal lactobacillus species in children with functional constipation by quantitative real-time PCR. Clin Exp Gastroenterol 13:141. https://doi.org/10.2147/CEG.S250755
Klein MS et al (2016) Metabolomic modeling to monitor host responsiveness to gut microbiota manipulation in the BTBRT+ tf/j mouse. J Proteome Res 15(4):1143–1150. https://doi.org/10.1021/acs.jproteome.5b01025
Kobayashi K et al (2013) Minocycline selectively inhibits M1 polarization of microglia. Cell Death Dis 4(3):e525–e525. https://doi.org/10.1038/cddis.2013.54
Koppel SJ et al (2021) A ketogenic diet differentially affects neuron and astrocyte transcription. J Neurochem 157(6):1930–1945. https://doi.org/10.1111/jnc.15313
Koppel SJ, Swerdlow RH (2018) Neuroketotherapeutics: a modern review of a century-old therapy. Neurochem Int 117:114–125. https://doi.org/10.1016/j.neuint.2017.05.019
Kraeuter A-K et al (2019) The Y-maze for assessment of spatial working and reference memory in mice. Pre-Clinical Models. https://doi.org/10.1007/978-1-4939-8994-2_10
Lee YH et al (2015) Aryl hydrocarbon receptor mediates both proinflammatory and anti-inflammatory effects in lipopolysaccharide-activated microglia. Glia 63(7):1138–1154. https://doi.org/10.1002/glia.22805
Maas AI et al (2017) Traumatic brain injury: integrated approaches to improve prevention, clinical care, and research. Lancet Neurol 16(12):987–1048. https://doi.org/10.1016/S1474-4422(17)30371-X
McDonald TJ, Cervenka MC (2018) The expanding role of ketogenic diets in adult neurological disorders. Brain Sci 8(8):148. https://doi.org/10.3390/brainsci8080148
Morris A (2005) Cerebral ketone body metabolism. J Inherit Metab Dis 28(2):109–121. https://doi.org/10.1007/s10545-005-5518-0
Murray AJ et al (2011) Parvalbumin-positive CA1 interneurons are required for spatial working but not for reference memory. Nat Neurosci 14(3):297–299. https://doi.org/10.1038/nn.2751
Mychasiuk R, Rho JM (2017) Genetic modifications associated with ketogenic diet treatment in the BTBRT+ Tf/J mouse model of autism spectrum disorder. Autism Res 10(3):456–471. https://doi.org/10.1002/aur.1682
Olson CA et al (2018) The gut microbiota mediates the anti-seizure effects of the ketogenic diet. Cell 173(7):1728–1741. https://doi.org/10.1016/j.cell.2018.04.027
Pitt J et al (2017) Neuroprotective astrocyte-derived insulin/insulin-like growth factor 1 stimulates endocytic processing and extracellular release of neuron-bound Aβ oligomers. Mol Biol Cell 28(20):2623–2636. https://doi.org/10.1091/mbc.E17-06-0416
Prins M et al (2005) Age-dependent reduction of cortical contusion volume by ketones after traumatic brain injury. J Neurosci Res 82(3):413–420. https://doi.org/10.1002/jnr.20633
Prins M et al (2004) Increased cerebral uptake and oxidation of exogenous βHB improves ATP following traumatic brain injury in adult rats. J Neurochem 90(3):666–672. https://doi.org/10.1111/j.1471-4159.2004.02542.x
Prins ML, Matsumoto J (2016) Metabolic response of pediatric traumatic brain injury. J Child Neurol 31(1):28–34. https://doi.org/10.1177/0883073814549244
Qin H et al (2012) Signal transducer and activator of transcription-3/suppressor of cytokine signaling-3 (STAT3/SOCS3) axis in myeloid cells regulates neuroinflammation. Proc Natl Acad Sci USA 109(13):5004–5009. https://doi.org/10.1073/pnas.1117218109
Rho JM, Stafstrom CE (2012) The ketogenic diet as a treatment paradigm for diverse neurological disorders. Front Pharmacol 3:59. https://doi.org/10.3389/fphar.2012.00059
Rothhammer V et al (2016) Type I interferons and microbial metabolites of tryptophan modulate astrocyte activity and central nervous system inflammation via the aryl hydrocarbon receptor. Nat Med 22(6):586–597. https://doi.org/10.1038/nm.4106
Salberg S et al (2019) The behavioural and pathophysiological effects of the ketogenic diet on mild traumatic brain injury in adolescent rats. Behav Brain Res 376:112225. https://doi.org/10.1016/j.bbr.2019.112225
Shitaka Y et al (2011) Repetitive closed-skull traumatic brain injury in mice causes persistent multifocal axonal injury and microglial reactivity. J Neuropathol Exp Neurol 70(7):551–567. https://doi.org/10.1097/NEN.0b013e31821f891f
Stumpf SK et al (2019) Ketogenic diet ameliorates axonal defects and promotes myelination in Pelizaeus-Merzbacher disease. Acta Neuropathol 138(1):147–161. https://doi.org/10.1007/s00401-019-01985-2
Sun L et al (2012) Microglial cathepsin B contributes to the initiation of peripheral inflammation-induced chronic pain. J Neurosci 32(33):11330–11342. https://doi.org/10.1523/JNEUROSCI.0677-12.2012
Tanaka T et al (2015) Interferon regulatory factor 7 participates in the M 1-like microglial polarization switch. Glia 63(4):595–610. https://doi.org/10.1002/glia.22770
Thau-Zuchman O et al (2021) A new ketogenic formulation improves functional outcome and reduces tissue loss following traumatic brain injury in adult mice. Theranostics 11(1):346. https://doi.org/10.7150/thno.48995
Verboon LN et al (2021) The immune system’s role in the consequences of mild traumatic brain injury (concussion). Front Immunol 12:313. https://doi.org/10.3389/fimmu.2021.620698
Vogel CF, Matsumura F (2009) A new cross-talk between the aryl hydrocarbon receptor and RelB, a member of the NF-κB family. Biochem Pharmacol 77(4):734–745. https://doi.org/10.1016/j.bcp.2008.09.036
Vuong HE et al (2017) The microbiome and host behavior. Annu Rev Neurosci 40:21–49. https://doi.org/10.1146/annurev-neuro-072116-031347
Walrave L et al (2016) Inhibition of connexin43 hemichannels impairs spatial short-term memory without affecting spatial working memory. Front Cell Neurosci 10:288. https://doi.org/10.3389/fncel.2016.00288
Winston CN et al (2016) Dendritic spine loss and chronic white matter inflammation in a mouse model of highly repetitive head trauma. Am J Pathol 186(3):552–567. https://doi.org/10.1016/j.ajpath.2015.11.006
Yu J et al (2018) Impact of nutrition on inflammation, tauopathy, and behavioral outcomes from chronic traumatic encephalopathy. J Neuroinflammation 15(1):1–16. https://doi.org/10.1186/s12974-018-1312-4
Zelante T et al (2013) Tryptophan catabolites from microbiota engage aryl hydrocarbon receptor and balance mucosal reactivity via interleukin-22. Immunity 39(2):372–385. https://doi.org/10.1016/j.immuni.2013.08.003
Zhang F et al (2018) Moderate hypothermia inhibits microglial activation after traumatic brain injury by modulating autophagy/apoptosis and the MyD88-dependent TLR4 signaling pathway. J Neuroinflamm 15(1):1–12. https://doi.org/10.1186/s12974-018-1315-1
Acknowledgements
We thank the entire the laboratory of Neurosurgery Department for supporting experimental space and technical services.
Funding
This work was supported by grants from the National Natural Science Foundation of China (No. 82071359), the Shanghai Rising-Star Program (21QA1405600), the Natural Science Foundation of Shanghai (21ZR1439000) and Ren ji New Star Program (F. Jia).
Author information
Authors and Affiliations
Contributions
DD, FZ and YJ designed the experiments. DD, FZ and SS performed and analyzed most experiments with the help of TL, MC, QL. DD and FZ were major contributors in writing this manuscript. FJ and XZ participated in the discussions and revised the manuscript. YJ supervised the entire project and was responsible for finalizing and submitting the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical Approval
Animal protocols were approved by the Animal Care and Experimental Committee of the School of Medicine of Shanghai Jiao Tong University.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
10571_2022_1226_MOESM3_ESM.tif
Supplementary Figure 1 Serum levels of total bilirubin, biliverdin and hemin in mice of different groups. Bilirubin: n = 6; one-way ANOVA; *p = 0.0211 SCG vs TCG, *p = 0.0489 SCG vs TKG, p = 0.9017 TCG vs TKG; F2, 15 = 0.2121, p = 0.8113; biliverdin: n = 6; one-way ANOVA; p = 0.2009 SCG vs TCG, p = 0.0710 SCG vs TKG, p = 0.8210 TCG vs TKG; F2, 15 = 0.08621, p = 0.9179; hemin: n = 6; one-way ANOVA; p = 0.3920 SCG vs TCG, p = 0.5662 SCG vs TKG, p = 0.9483 TCG vs TKG; F2, 15 = 0.01908, p = 0.9811. Supplementary file3 (TIF 4196 KB)
10571_2022_1226_MOESM4_ESM.tif
Supplementary Figure 2 The morphological changes of microglia and astrocytes. A, C Fluorescence images showing microglia and astrocytes in the hippocampal CA1 region. Scale bar = 10 μm.B Graphs showing the morphological analyses in Iba-1+ microglia. Soma area: n = 6; one-way ANOVA; p = 0.2099 SCG vs TCG, p = 0.9224 SCG vs TKG, p = 0.1106 TCG vs TKG; F2, 15 = 1.281, p = 0.3065; process length: n = 6; one-way ANOVA; *p = 0.0102 SCG vs TCG, p = 0.7394 SCG vs TKG, *p = 0.0444 TCG vs TKG; F2, 15 = 1.452, p = 0.2653.D Graphs showing the morphological analyses in GFAP+ astrocytes. Soma area: n = 6; one-way ANOVA; p = 0.3629 SCG vs TCG, p = 0.2174 SCG vs TKG, *p = 0.0167 TCG vs TKG; F2, 15 = 0.09059, p = 0.9139; process length: n = 6; one-way ANOVA; *p = 0.0152 SCG vs TCG, p = 0.9847 SCG vs TKG, *p = 0.0212 TCG vs TKG; F2, 15 = 0.2645, p = 0.7711. Supplementary file4 (TIF 6632 KB)
10571_2022_1226_MOESM5_ESM.tif
Supplementary Figure 3 Negative control immunofluorescence images of AHR/RelB colocalization in microglia from the hippocampal CA1 region. Scale bar = 20 μm. Supplementary file5 (TIF 13068 KB)
Rights and permissions
About this article
Cite this article
Dilimulati, D., Zhang, F., Shao, S. et al. Ketogenic Diet Modulates Neuroinflammation via Metabolites from Lactobacillus reuteri After Repetitive Mild Traumatic Brain Injury in Adolescent Mice. Cell Mol Neurobiol 43, 907–923 (2023). https://doi.org/10.1007/s10571-022-01226-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-022-01226-3