Abstract
Purpose
Increasing numbers of transgender adolescents are receiving gender-affirming treatments (GAT). Given GAT can impair reproductive function, clinical guidelines advise prior counselling regarding fertility preservation (FP). For transgender adults assigned male at birth, FP is usually achieved via a masturbatory sample and sperm cryopreservation. This is less straightforward in transgender adolescents, since they may not be developmentally ready to masturbate and/or masturbation may cause unacceptable gender dysphoria. Testicular biopsy represents an alternative method for sperm retrieval in these adolescents, but for those in early/mid puberty, it is difficult to predict whether sperm will be found. The purpose of this study was therefore to identify factors that predict successful sperm retrieval for cryopreservation via testicular biopsy.
Methods
A retrospective cohort study was undertaken at a tertiary-referral pediatric gender service. Subjects were included if they’d received a testicular biopsy in association with the commencement of GAT between 2010 and 2019. The primary outcome measure was successful sperm retrieval, and potential predictors included age, testicular volume and serum testosterone, LH and FSH levels.
Results
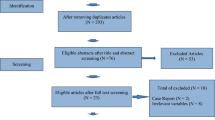
Of 25 subjects who received a biopsy prior to starting any GAT, 17 had successful sperm retrieval. While age, testosterone, LH and FSH levels showed minimal differences, testicular volume was significantly higher in those with successful sperm retrieval, and a threshold of ≥ 10 mL showed 92% sensitivity and 71% specificity in predicting successful retrieval. An additional 6 patients received a biopsy after starting puberty suppression and before commencement of oestrogen, and one of these individuals had sperm successfully retrieved despite > 2 years of regular puberty suppression.
Conclusion
These findings suggest that testicular volume is most useful in predicting successful sperm retrieval following testicular biopsy in transgender adolescents and are likely to be of relevance to other young people undertaking FP, including those with cancer.

Similar content being viewed by others
Data availability
Data will be available upon reasonable request.
Code availability
Not applicable.
References
Chen M, Fuqua J, Eugster EA. Characteristics of referrals for gender dysphoria over a 13-year period. J Adolesc Health. 2016 [cited 2020 Jul 19];58(3):369–71. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1054139X1500676X.
Lai TC, McDougall R, Feldman D, Elder CV, Pang KC. Fertility counseling for transgender adolescents: a review. J Adolesc Health. 2020 [cited 2020 Jul 19];66(6):658–65. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1054139X20300343.
Linde R, Doelle GC, Alexander N, Kirchner F, Vale W, Rivier J, et al. Reversible inhibition of testicular steroidogenesis and spermatogenesis by a potent gonadotropin-releasing hormone agonist in normal men: an approach toward the development of a male contraceptive. N Engl J Med. 1981 [cited 2020 Jul 19];305(12):663–7. Available from: https://doi.org/10.1056/NEJM198109173051203.
Schagen SEE, Cohen-Kettenis PT, Delemarre-van de Waal HA, Hannema SE. Efficacy and safety of gonadotropin-releasing hormone agonist treatment to suppress puberty in gender dysphoric adolescents. J Sex Med. 2016 [cited 2020 Jul 19];13(7):1125–32. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1743609516302193.
Schulze C. Response of the human testis to long-term estrogen treatment: morphology of Sertoli cells, Leydig cells and spermatogonial stem cells. Cell Tissue Res. 1988;251(1):31–43.
Leavy M, Trottmann M, Liedl B, Reese S, Stief C, Freitag B, et al. Effects of elevated β-estradiol levels on the functional morphology of the testis — new insights. Sci Rep. 2017 [cited 2020 Jul 19];7(1):39931. Available from: http://www.nature.com/articles/srep39931.
Thiagaraj D, Gunasegaram R, Loganath A, Peh KL, Kottegoda SR, Ratnam SS. Histopathology of the testes from male transsexuals on oestrogen therapy. Ann Acad Med Singap. 1987;16(2):347–8.
Venizelos ID, Paradinas FJ. Testicular atrophy after oestrogen therapy. Histopathology. 1988 [cited 2020 Jul 19];12(4):451–4. Available from: https://doi.org/10.1111/j.1365-2559.1988.tb01961.x.
Lübbert H, Leo-Roßberg I, Hammerstein J. Effects of ethinyl estradiol on semen quality and various hormonal parameters in a eugonadal male. Fertil Steril. 1992 [cited 2020 Jul 19];58(3):603–8. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0015028216552716.
Adeleye AJ, Reid G, Kao C-N, Mok-Lin E, Smith JF. Semen parameters among transgender women with a history of hormonal treatment. Urology. 2019 [cited 2020 Jul 19];124:136–41. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0090429518310872.
Schneider F, Neuhaus N, Wistuba J, Zitzmann M, Heß J, Mahler D, et al. Testicular functions and clinical characterization of patients with gender dysphoria (GD) undergoing Sex Reassignment Surgery (SRS). J Sex Med. 2015 [cited 2020 Jul 19];12(11):2190–200. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1743609515344489.
Coleman E, Bockting W, Botzer M, Cohen-Kettenis P, DeCuypere G, Feldman J, et al. Standards of care for the health of transsexual, transgender, and gender-nonconforming people, Version 7. Int J Transgenderism. 2012 [cited 2020 Jul 19];13(4):165–232. Available from: https://doi.org/10.1080/15532739.2011.700873.
Telfer MM, Tollit MA, Pace CC, Pang KC. Australian standards of care and treatment guidelines for transgender and gender diverse children and adolescents. Med J Aust. 2018;209(3):132–6.
Wierckx K, Van Caenegem E, Pennings G, Elaut E, Dedecker D, Van de Peer F, et al. Reproductive wish in transsexual men. Hum Reprod. 2012 [cited 2020 Jul 19];27(2):483–7. Available from: https://doi.org/10.1093/humrep/der406.
De Sutter P, Verschoor A, Hotimsky A, Kira K. The desire to have children and the preservation of fertility in transsexual women: A survey. Int J Transgend. 2002;6(3):215–221.
von Doussa H, Power J, Riggs D. Imagining parenthood: the possibilities and experiences of parenthood among transgender people. Cult Health Sex. 2015 [cited 2020 Jul 19];17(9):1119–31. Available from: https://doi.org/10.1080/13691058.2015.1042919.
Jones CA, Reiter L, Greenblatt E. Fertility preservation in transgender patients. Int J Transgenderism. 2016;17:76–82.
Armuand G, Dhejne C, Olofsson JI, Rodriguez-Wallberg KA. Transgender men’s experiences of fertility preservation: a qualitative study. Hum Reprod. 2017;32(2):383–90.
Nahata L, Tishelman AC, Caltabellotta NM, Quinn GP. Low fertility preservation utilization among transgender youth. J Adolesc Health. 2017 [cited 2020 Jul 19];61(1):40–4. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1054139X16309582.
Auer MK, Fuss J, Nieder TO, Briken P, Biedermann SV, Stalla GK, et al. Desire to have children among transgender people in Germany: a cross-sectional multi-center study. J Sex Med. 2018;15(5):757–67.
Kyweluk MA, Sajwani A, Chen D. Freezing for the future: transgender youth respond to medical fertility preservation. Int J Transgenderism. 2018;19:401–16.
Riggs DW, Bartholomaeus C. Fertility preservation decision making amongst Australian transgender and non-binary adults. Reprod Health. 2018;15(1):181.
Brik T, Vrouenraets LJJJ, Schagen SEE, Meissner A, de Vries MC, Hannema SE. Use of fertility preservation among a cohort of transgirls in the Netherlands. J Adolesc Health. 2019;64(5):589–93.
Chiniara LN, Viner C, Palmert M, Bonifacio H. Perspectives on fertility preservation and parenthood among transgender youth and their parents. Arch Dis Child. 2019;104(8):739–44.
Pang KC, Peri A, Chung HE, Telfer M, Elder CV, Grover S, Jayasinghe Y. Rates of fertility preservation use among transgender adolescents. JAMA Pediatr. 2020;174(9):890–891. https://doi.org/10.1001/jamapediatrics.2020.0264.
Picton HM, Wyns C, Anderson RA, Goossens E, Jahnukainen K, Kliesch S, et al. A European perspective on testicular tissue cryopreservation for fertility preservation in prepubertal and adolescent boys. Hum Reprod. 2015 [cited 2020 Jul 19];30(11):2463–75. Available from: https://doi.org/10.1093/humrep/dev190.
Jahnukainen K, Stukenborg J-B. Clinical review: present and future prospects of male fertility preservation for children and adolescents. J Clin Endocrinol Metab. 2012;97(12):4341–51.
Wallace SA, Blough KL, Kondapalli LA. Fertility preservation in the transgender patient: expanding oncofertility care beyond cancer. Gynecol Endocrinol. 2014;30(12):868–71.
Müller J, Skakkebaek NE. Quantification of germ cells and seminiferous tubules by stereological examination of testicles from 50 boys who suffered from sudden death. Int J Androl. 1983;6(2):143–56.
Hovatta O. Cryopreservation of testicular tissue in young cancer patients. Hum Reprod Update. 2001;7(4):378–83.
Nielsen CT, Skakkebaek NE, Richardson DW, Darling JA, Hunter WM, Jørgensen M, et al. Onset of the release of spermatozoa (spermarche) in boys in relation to age, testicular growth, pubic hair, and height. J Clin Endocrinol Metab. 1986;62(3):532–5.
Schaefer F, Marr J, Seidel C, Tilgen W, Schärer K. Assessment of gonadal maturation by evaluation of spermaturia. Arch Dis Child. 1990;65(11):1205–7.
Kliesch S, Behre HM, Jürgens H, Nieschlag E. Cryopreservation of semen from adolescent patients with malignancies. Med Pediatr Oncol. 1996;26(1):20–7.
Kamischke A, Jürgens H, Hertle L, Berdel WE, Nieschlag E. Cryopreservation of sperm from adolescents and adults with malignancies. J Androl. 2004;25(4):586–92.
Adank MC, van Dorp W, Smit M, van Casteren NJ, Laven JSE, Pieters R, et al. Electroejaculation as a method of fertility preservation in boys diagnosed with cancer: a single-center experience and review of the literature. Fertil Steril. 2014 [cited 2020 Jul 20];102(1):199–205.e1. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0015028214002933.
Hagenas I, Jorgensen N, Rechnitzer C, Sommer P, Holm M, Schmiegelow K, et al. Clinical and biochemical correlates of successful semen collection for cryopreservation from 12–18-year-old patients: a single-center study of 86 adolescents. Hum Reprod. 2010 [cited 2020 Jul 20];25(8):2031–8. Available from: https://doi.org/10.1093/humrep/deq147.
Ho WLC, Bourne H, Gook D, Clarke G, Kemertzis M, Stern K, et al. A short report on current fertility preservation strategies for boys. Clin Endocrinol. 2017 [cited 2020 Dec 28];87(3):279–85. https://doi.org/10.1111/cen.13377.
Ji C-Y, Ohsawa S. Onset of the release of spermatozoa (spermarche) in Chinese male youth. Am J Hum Biol. 2000;12(5):577–87.
Zachmann M, Prader A, Kind HP, Häfliger H, Budliger H. Testicular volume during adolescence Cross-sectional and longitudinal studies. Helv Paediatr Acta. 1974;29(1):61–72.
Biro FM, Lucky AW, Huster GA, Morrison JA. Pubertal staging in boys. J Pediatr. 1995;127(1):100–2.
Ankarberg-Lindgren C, Norjavaara E. Changes of diurnal rhythm and levels of total and free testosterone secretion from pre to late puberty in boys: testis size of 3 ml is a transition stage to puberty. Eur J Endocrinol. 2004;151(6):747–57.
Wu FC, Brown DC, Butler GE, Stirling HF, Kelnar CJ. Early morning plasma testosterone is an accurate predictor of imminent pubertal development in prepubertal boys. J Clin Endocrinol Metab. 1993;76(1):26–31.
Keene DJB, Sajjad Y, Makin G, Cervellione RM. Sperm banking in the United Kingdom is feasible in patients 13 years old or older with cancer. J Urol. 2012;188(2):594–7.
Bahadur G, Ling KLE, Hart R, Ralph D, Wafa R, Ashraf A, et al. Semen quality and cryopreservation in adolescent cancer patients. Hum Reprod. 2002;17(12):3157–61.
Dabaja AA, Wosnitzer MS, Bolyakov A, Schlegel PN, Paduch DA. When to ask male adolescents to provide semen sample for fertility preservation? Transl Androl Urol. 2014;3(1):2–8.
Pang KC, de Graaf NM, Chew D, Hoq M, Keith DR, Carmichael P, et al. Association of media coverage of transgender and gender diverse issues with rates of referral of transgender children and adolescents to specialist gender clinics in the UK and Australia. JAMA Netw Open. 2020 [cited 2020 Dec 28];3(7):e2011161. Available from: https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2768726.
Bourne H, Archer J, Edgar DH, Baker HWG. Sperm preparation techniques. In: Textbook of assisted reproductive techniques. Taylor & Francis: London; 2012. p. 61–74.
Emmanuel M, Bokor BR. Tanner Stages. In: StatPearls. Treasure Island: StatPearls Publishing; 2020 [cited 2021 Jan 8]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK470280/.
Hembree WC, Cohen-Kettenis P, Delemarre-van de Waal HA, Gooren LJ, Meyer WJ, Spack NP, et al. Endocrine treatment of transsexual persons: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2009 [cited 2020 Jul 19];94(9):3132–54. Available from: https://academic.oup.com/jcem/article/94/9/3132/2596324.
van Casteren NJ, Dohle GR, Romijn JC, de Muinck K-S, Weber RFA, van den Heuvel-Eibrink MM. Semen cryopreservation in pubertal boys before gonadotoxic treatment and the role of endocrinologic evaluation in predicting sperm yield. Fertil Steril. 2008;90(4):1119–25.
Acknowledgements
KCP is supported by the Hugh Williamson Foundation Trust and the Royal Children’s Hospital Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was conducted with the approval of the RCH Human Research Ethics Committee (#36323). As a retrospective audit of clinical files, consent was not required. However, consent was obtained from the individual who had sperm identified despite being on GnRHa, given the information shared about their case made them potentially identifiable.
Consent for publication
All named authors consent to the publication of this manuscript.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Peri, A., Ahler, A., Gook, D. et al. Predicting successful sperm retrieval in transfeminine adolescents after testicular biopsy. J Assist Reprod Genet 38, 2735–2743 (2021). https://doi.org/10.1007/s10815-021-02293-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-021-02293-z