Abstract
Purpose
Rural and highly religious Intermountain West states demonstrate low levels of HPV vaccination uptake. The Intermountain West HPV Vaccination Coalition (IWHVC) was formed to improve HPV vaccination by enhancing collaborations between cancer centers, health departments, health clinics, religious groups, and community organizations. Coalition members’ perceptions and experiences are described within.
Methods
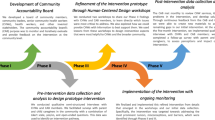
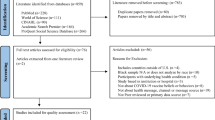
A cross-sectional online survey was distributed to the IWHVC. N = 86 responded to the online survey. Six subsequent focus groups were conducted (N = 36). Participant demographics, barriers, and facilitators of HPV vaccination were summarized. The first three focus groups were coded in an iterative manner based on a coding scheme. The final three focus groups were selectively coded for content related to five themes: barriers and facilitators to HPV vaccination, how the coalition has been useful, future directions of the coalition, and how to engage religious communities.
Results
Participants suggested that HPV vaccination should occur in a doctor’s office (70.9%), public health clinic (64.0%), or at a community health fair (58.1%). Perceived barriers included a lack of education/low knowledge about the HPV vaccine (55.8%), concerns about sexuality/promiscuity (44.2%), and not knowing the vaccine is recommended for boys (38.4%). Participants stressed the importance of gaining buy-in from religious leaders, and felt the coalition helped them advocate for HPV vaccination through networking, idea and information sharing, and voicing their community’s needs. Future goals emphasized targeted outreach, sustainable funding, expanded environmental scans, gaining religious support, and policy reforms.
Conclusions
Targeted coalition work builds community capacity and coordinates HPV vaccination efforts. A community driven coalition approach could help improve HPV vaccination in other rural and highly religious regions.


Similar content being viewed by others
References
Recommendations on the Use of Quadrivalent Human Papillomavirus Vaccine in Males—Advisory Committee on Immunization Practices (ACIP). (2011). Retrieved February 14, 2014, from http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6050a3.htm.
Markowitz, L.E., Dunne, E.F., Saraiya, M., Lawson, H.W., Chesson, H., Unger, E.R. (2007). Quadrivalent human papillomavirus vaccine: Recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recommondations Report, 56(RR-2), 1–24.
Healthy People 2020 Topics & Objectives. (2014). Retrieved May 23, 2014, from http://www.healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicId=23.
Intermountain West HPV Vaccination Coalition. (2014). Retrieved January 03, 2017, from http://healthcare.utah.edu/huntsmancancerinstitute/cancer-information/outreach/hpv-coalition/.
State Area Measurements and Internal, Point Coordinates. (2010). Retrieved January 02, 2017, from https://www.census.gov/geo/reference/state-area.html.
Mapping Process and data. (2010). Retrieved January 03, 2017, from http://frontierus.org/mapping-process-and-data/.
Crosby, R. A., Casey, B. R., Vanderpool, R., Collins, T., & Moore, G. R. (2011). Uptake of free HPV vaccination among young women: A comparison of rural versus urban rates. The Journal of Rural Health, 27(4), 380–384.
Fazekas, K. I., Brewer, N. T., & Smith, J. S. (2008). HPV vaccine acceptability in a rural Southern area. J Womens Health, 17(4), 539–548.
Hopenhayn, C., Christian, A., & Schoenberg, N. E. (2007). Human papillomavirus vaccine: knowledge and attitudes in two Appalachian Kentucky counties. Cancer Causes & Control, 18(6), 627–634.
Sperber, N. R., Brewer, N. T., & Smith, J. S. (2008). Influence of parent characteristics and disease outcome framing on HPV vaccine acceptability among rural, Southern women. Cancer Causes & Control, 19(1), 115–118.
Cates, J. R., Brewer, N. T., Fazekas, K. I., Mitchell, C. E., & Smith, J. S. (2009). Racial differences in HPV knowledge, HPV vaccine acceptability, and related beliefs among rural, southern women. The Journal of Rural Health, 25(1), 93–97.
Newmann, S. J., & Garner, E. O. (2005). Social inequities along the cervical cancer continuum: A structured review. Cancer Causes & Control, 16(1), 63–70.
Religious Landscape Study. (2008). PewResearchCenter: Religion & public life. Retrieved February 02, 2017, from http://www.pewforum.org/religious-landscape-study/.
U.S. Religious Landscape Survey: Religious Beliefs and Practices. (2008). PewResearchCenter: Religion & public life. Retrieved February 02, 2017, from http://www.pewforum.org/2008/06/01/u-s-religious-landscape-survey-religious-beliefs-and-practices/.
Shelton, R. C., Snavely, A. C., De Jesus, M., Othus, M. D., Allen, J. D. (2013). HPV vaccine decision-making and acceptance: does religion play a role? Journal of Religion and Health, 52(4), 1120–1130.
Thomas, T., Blumling, A., & Delaney, A. (2015). The Influence of religiosity and spirituality on rural parents’ health decision-making and human papillomavirus vaccine choices. ANS Advances in Nursing Science, 38(4), E1–E12.
Stewart, K. (2013). Utah health official bans Gardasil, stirring controversy. Salt Lake Tribune: Salt Lake City.
Editorial: Denying HPV vaccine is irresponsible. (2013). Retrieved February 02, 2017, from http://www.sltrib.com/sltrib/opinion/57229576-82/vaccine-cancer-percent-blodgett.html.csp.
Hamilton, C. (2007). HB 358: Lawmakers nix cervical cancer campaign, vaccinations for Utah women. The Salt Lake Tribune: Salt Lake City.
Lyon, J. (2012). Boys urged to get the HPV vaccine. The Salt Lake Tribune: Salt Lake City.
Stewart, K. (2013). Use of HPV vaccine for youths in Utah is low. The Salt Lake Tribune: Salt Lake City.
Kepka, D., Spigarelli, M.G., Warner, E.L., Yoneoka, Y., McConnell, N., Balch, A. (2016). Statewide analysis of missed opportunities for human papillomavirus vaccination using vaccine registry data. Papillomavirus Research, 2, 128–132.
Centers for Disease Control and Prevention. (2017). TeenVaxView. Retrieved April 01, 2017, from https://www.cdc.gov/vaccines/imz-managers/coverage/teenvaxview/index.html.
Elo, S., & Kyngas, H. (2008). The qualitative content analysis process. Journal of Advanced Nursing, 62(1), 107–115.
Holman, D.M., Benard, V., Roland, K.B., Watson, M., Liddon, N., Stokley, S. (2014). Barriers to human papillomavirus vaccination among US adolescents: A systematic review of the literature. JAMA Pediatrics, 168(1), 76–82.
Niccolai, L.M., C.E. Hansen. (2015). Practice- and community-based interventions to increase human papillomavirus vaccine coverage: A systematic review. JAMA Pediatrics, 169(7), 686–692.
Oltean, H. N., Lofy, K. H., Goldoft, M. J., & DeBolt, C. A. (2016). Human papillomavirus vaccination in Washington State: Estimated coverage and missed opportunities, 2006–2013. Public Health Reports, 131(3), 474–482 (Washington, D. C.: 1974).
National Institues of Health. (2017). Linking the Provider Recommendation to Adolescent HPV Vaccine Uptake (R01). Retrieved April 01, 2017, from https://grants.nih.gov/grants/guide/pa-files/PAR-16-338.html.
Acknowledgements
We would like to thank Guadalupe Tovar and Holdunn Rutkoski for their assistance conducting the focus groups. We are also grateful to the Intermountain West HPV Vaccination Coalition members for their contributions. The research reported in this publication was supported by Huntsman Cancer Foundation, the Beaumont Foundation, and the National Cancer Institute of the National Institutes of Health under Award Number P30CA042014. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Warner, E.L., Fowler, B., Martel, L. et al. Improving HPV Vaccination Through a Diverse Multi-state Coalition. J Community Health 42, 911–920 (2017). https://doi.org/10.1007/s10900-017-0334-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-017-0334-7