Abstract
Purpose
Spinal metastases are common in cancer. This preferential migration/growth in the spine is not fully understood. Dura has been shown to affect the surrounding microenvironment and promote cancer growth. Here, we investigate the role of dural cytokines in promoting the metastatic potential of prostate cancer (PCa) and the involvement of the CXCR2 signaling pathway.
Methods
The role of dural conditioned media (DCM) in proliferation, migration and invasion of five PCa cell lines with various hormone sensitivities was assessed in the presence or absence of the CXCR2 inhibitor, SB225002. CXCR2 surface protein was examined by FACS. Cytokine levels were measured using a mouse cytokine array.
Results
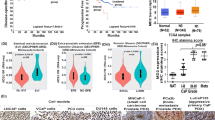
We observed high levels of cytokines produced by dura and within the vertebral body bone marrow, namely CXCL1 and CXCL2, that act on the CXCR2 receptor. All prostate cell lines treated with DCM demonstrated significant increase in growth, migration and invasion regardless of androgen sensitivity, except PC3, which did not significantly increase in invasiveness. When treated with SB225002, the growth response to DCM by cells expressing the highest levels of CXCR2 as measured by FACS (LNCaP and 22Rv1) was blunted. The increase in migration was significantly decreased in all lines in the presence of SB225002. Interestingly, the invasion increase seen with DCM was unchanged when these cells were treated with the CXCR2 inhibitor, except PC3 did demonstrate a significant decrease in invasion.
Conclusion
DCM enhances the metastatic potential of PCa with increased proliferation, migration and invasion. This phenomenon is partly mediated through the CXCR2 pathway.




Similar content being viewed by others
Availability of data and material
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
References
Roodman GD (2009) Pathophysiology of bone metastases. In: Kardamakis D, Vassiliou V, Chow E (eds) Bone metastases: a translational and clinical approach. Springer, Dordrecht
Mundy GR (2002) Metastasis to bone: causes, consequences and therapeutic opportunities. Nat Rev Cancer 2(8):584–593. https://doi.org/10.1038/nrc867
Jiang W, Rixiati Y, Zhao B, Li Y, Tang C, Liu J (2020) Incidence, prevalence, and outcomes of systemic malignancy with bone metastases. J Orthop Surg 28(2):2309499020915989. https://doi.org/10.1177/2309499020915989
Algra PR, Heimans JJ, Valk J, Nauta J, Lachniet M, Van Kooten B (1992) Do metastases in vertebrae begin in the body or the pedicles? Imaging study in 45 patients. AJR Am J Roentgenol 158(6):1275–1279
Guo M, Kolberg KL, Smith EC, Smith BW, Yousif JE, Kessler JL, Linzey JR, Calinescu A-A, Clines GA, Spratt DE, Szerlip NJ (2018) Predominance of spinal metastases involving the posterior vertebral body. World Neurosurg 119:e991–e996. https://doi.org/10.1016/j.wneu.2018.08.029
Tiwana MS, Barnes M, Yurkowski E, Roden K, Olson RA (2016) Incidence and treatment patterns of complicated bone metastases in a population-based radiotherapy program. Radiother Oncol 118(3):552–556. https://doi.org/10.1016/j.radonc.2015.10.015
Sciubba DM, Petteys RJ, Dekutoski MB, Fisher CG, Fehlings MG, Ondra SL, Rhines LD, Gokaslan ZL (2010) Diagnosis and management of metastatic spine disease. J Neurosurg Spine 13(1):94–108. https://doi.org/10.3171/2010.3.SPINE09202
Bohm P, Huber J (2002) The surgical treatment of bony metastases of the spine and limbs. J Bone Joint Surg Br 84(4):521–529
Cameron Hatrick N, Lucas JD, Timothy AR, Smith MA (2000) The surgical treatment of metastatic disease of the spine. Radiother Oncol 56(3):335–339. https://doi.org/10.1016/S0167-8140(00)00199-7
Harrington KD (1986) Metastatic disease of the spine. J Bone Joint Surg Am 68(7):1110–1115
Bubendorf L, Schöpfer A, Wagner U, Sauter G, Moch H, Willi N, Gasser TC, Mihatsch MJ (2000) Metastatic patterns of prostate cancer: an autopsy study of 1,589 patients. Hum Pathol 31(5):578–583. https://doi.org/10.1053/hp.2000.6698
Harada M, Shimizu A, Nakamura Y, Nemoto R (1992) Role of the vertebral venous system in metastatic spread of cancer cells to the bone. Adv Exp Med Biol 324:83–92
Muresan MM, Olivier P, Leclère J, Sirveaux F, Brunaud L, Klein M, Zarnegar R, Weryha G (2008) Bone metastases from differentiated thyroid carcinoma. Endocr Relat Cancer 15(1):37–49. https://doi.org/10.1677/ERC-07-0229
Simmons JK, Hildreth BE 3rd, Supsavhad W, Elshafae SM, Hassan BB, Dirksen WP, Toribio RE, Rosol TJ (2015) Animal models of bone metastasis. Vet Pathol 52(5):827–841. https://doi.org/10.1177/0300985815586223
Paget S (1889) The distribution of secondary growths in cancer of the breast. The Lancet 133(3421):571–573. https://doi.org/10.1016/S0140-6736(00)49915-0
Quail DF, Joyce JA (2013) Microenvironmental regulation of tumor progression and metastasis. Nat Med 19(11):1423–1437. https://doi.org/10.1038/nm.3394
Gagan JR, Tholpady SS, Ogle RC (2007) Cellular dynamics and tissue interactions of the dura mater during head development. Birth Defects Res C Embryo Today 81(4):297–304. https://doi.org/10.1002/bdrc.20104
Spector JA, Greenwald JA, Warren SM, Bouletreau PJ, Detch RC, Fagenholz PJ, Crisera FE, Longaker MT (2002) Dura mater biology: autocrine and paracrine effects of fibroblast growth factor 2. Plast Reconstr Surg 109(2):645–654. https://doi.org/10.1097/00006534-200202000-00035
Levi B, Nelson ER, Li S, James AW, Hyun JS, Montoro DT, Lee M, Glotzbach JP, Commons GW, Longaker MT (2011) Dura mater stimulates human adipose-derived stromal cells to undergo bone formation in mouse calvarial defects. Stem Cells 29(8):1241–1255. https://doi.org/10.1002/stem.670
Szerlip NJ, Calinescu A, Smith E, Tagett R, Clines KL, Moon HH, Taichman RS, Van Poznak CH, Clines GA (2018) Dural cells release factors which promote cancer cell malignancy and induce immunosuppressive markers in bone marrow myeloid cells. Neurosurgery 83(6):1306–1316. https://doi.org/10.1093/neuros/nyx626
Olson TS, Ley K (2002) Chemokines and chemokine receptors in leukocyte trafficking. Am J Physiol Regul Integr Comp Physiol 283(1):R7–R28. https://doi.org/10.1152/ajpregu.00738.2001
Strieter RM, Burdick MD, Mestas J, Gomperts B, Keane MP, Belperio JA (2006) Cancer CXC chemokine networks and tumour angiogenesis. Eur J Cancer 42(6):768–778. https://doi.org/10.1016/j.ejca.2006.01.006
Veenstra M, Ransohoff RM (2012) Chemokine receptor CXCR2: physiology regulator and neuroinflammation controller? J Neuroimmunol 246(1):1–9. https://doi.org/10.1016/j.jneuroim.2012.02.016
Le Y, Zhou Y, Iribarren P, Wang J (2004) Chemokines and chemokine receptors: their manifold roles in homeostasis and disease. Cell Mol Immunol 1(2):95–104
Jaffer T, Ma D (2016) The emerging role of chemokine receptor CXCR2 in cancer progression. Transl Cancer Res 5:S616–S628
Zhang H, Ye YL, Li MX, Ye SB, Huang WR, Cai TT, He J, Peng JY, Duan TH, Cui J, Zhang XS, Zhou FJ, Wang RF, Li J (2017) CXCL2/MIF-CXCR2 signaling promotes the recruitment of myeloid-derived suppressor cells and is correlated with prognosis in bladder cancer. Oncogene 36(15):2095–2104. https://doi.org/10.1038/onc.2016.367
Cheng Y, Ma X-l, Wei Y-Q, Wei X-W (2019) Potential roles and targeted therapy of the CXCLs/CXCR2 axis in cancer and inflammatory diseases. Biochim Biophys Acta Rev Cancer 1872(2):289–312. https://doi.org/10.1016/j.bbcan.2019.01.005
Yang G, Rosen DG, Liu G, Yang F, Guo X, Xiao X, Xue F, Mercado-Uribe I, Huang J, Lin S-H, Mills GB, Liu J (2010) CXCR2 promotes ovarian cancer growth through dysregulated cell cycle, diminished apoptosis, and enhanced angiogenesis. Clin Cancer Res 16(15):3875–3886. https://doi.org/10.1158/1078-0432.CCR-10-0483
Gabellini C, Trisciuoglio D, Desideri M, Candiloro A, Ragazzoni Y, Orlandi A, Zupi G, Del Bufalo D (2009) Functional activity of CXCL8 receptors, CXCR1 and CXCR2, on human malignant melanoma progression. Eur J Cancer 45(14):2618–2627. https://doi.org/10.1016/j.ejca.2009.07.007
Singh S, Singh AP, Sharma B, Owen LB, Singh RK (2010) CXCL8 and its cognate receptors in melanoma progression and metastasis. Future Oncol 6(1):111–116. https://doi.org/10.2217/fon.09.128
Matsuo Y, Raimondo M, Woodward TA, Wallace MB, Gill KR, Tong Z, Burdick MD, Yang Z, Strieter RM, Hoffman RM, Guha S (2009) CXC-chemokine/CXCR2 biological axis promotes angiogenesis in vitro and in vivo in pancreatic cancer. Int J Cancer 125(5):1027–1037. https://doi.org/10.1002/ijc.24383
Reiland J, Furcht LT, McCarthy JB (1999) CXC-chemokines stimulate invasion and chemotaxis in prostate carcinoma cells through the CXCR2 receptor. Prostate 41(2):78–88
Liu Z, Yang L, Xu J, Zhang X, Wang B (2011) Enhanced expression and clinical significance of chemokine receptor CXCR2 in hepatocellular carcinoma. J Surg Res 166(2):241–246. https://doi.org/10.1016/j.jss.2009.07.014
Han L, Jiang B, Wu H, Wang X, Tang X, Huang J, Zhu J (2012) High expression of CXCR2 is associated with tumorigenesis, progression, and prognosis of laryngeal squamous cell carcinoma. Med Oncol 29(4):2466–2472. https://doi.org/10.1007/s12032-011-0152-1
Saintigny P, Massarelli E, Lin S, Ahn Y-H, Chen Y, Goswami S, Erez B, O’Reilly MS, Liu D, Lee JJ, Zhang L, Ping Y, Behrens C, Solis Soto LM, Heymach JV, Kim ES, Herbst RS, Lippman SM, Wistuba II, Hong WK, Kurie JM, Koo JS (2013) CXCR2 expression in tumor cells is a poor prognostic factor and promotes invasion and metastasis in lung adenocarcinoma. Cancer Res 73(2):571–582. https://doi.org/10.1158/0008-5472.CAN-12-0263
Cooper CR, Chay CH, Gendernalik JD, Lee HL, Bhatia J, Taichman RS, McCauley LK, Keller ET, Pienta KJ (2003) Stromal factors involved in prostate carcinoma metastasis to bone. Cancer 97(3 Suppl):739–747. https://doi.org/10.1002/cncr.11181
Wang J, Loberg R, Taichman RS (2006) The pivotal role of CXCL12 (SDF-1)/CXCR4 axis in bone metastasis. Cancer Metastasis Rev 25(4):573–587. https://doi.org/10.1007/s10555-006-9019-x
Steele CW, Karim SA, Leach JDG, Bailey P, Upstill-Goddard R, Rishi L, Foth M, Bryson S, McDaid K, Wilson Z, Eberlein C, Candido JB, Clarke M, Nixon C, Connelly J, Jamieson N, Carter CR, Balkwill F, Chang DK, Evans TRJ, Strathdee D, Biankin AV, Nibbs RJB, Barry ST, Sansom OJ, Morton JP (2016) CXCR2 inhibition profoundly suppresses metastases and augments immunotherapy in pancreatic ductal adenocarcinoma. Cancer Cell 29(6):832–845. https://doi.org/10.1016/j.ccell.2016.04.014
Araki S, Omori Y, Lyn D, Singh RK, Meinbach DM, Sandman Y, Lokeshwar VB, Lokeshwar BL (2007) Interleukin-8 is a molecular determinant of androgen independence and progression in prostate cancer. Cancer Res 67(14):6854–6862. https://doi.org/10.1158/0008-5472.Can-07-1162
Liu Q, Li A, Tian Y, Wu JD, Liu Y, Li T, Chen Y, Han X, Wu K (2016) The CXCL8-CXCR1/2 pathways in cancer. Cytokine Growth Factor Rev. https://doi.org/10.1016/j.cytogfr.2016.08.002
Murphy C, McGurk M, Pettigrew J, Santinelli A, Mazzucchelli R, Johnston PG, Montironi R, Waugh DJ (2005) Nonapical and cytoplasmic expression of interleukin-8, CXCR1, and CXCR2 correlates with cell proliferation and microvessel density in prostate cancer. Clin Cancer Res 11(11):4117–4127. https://doi.org/10.1158/1078-0432.Ccr-04-1518
Li S, Quarto N, Longaker MT (2007) Dura mater-derived FGF-2 mediates mitogenic signaling in calvarial osteoblasts. Am J Physiol Cell Physiol 293(6):C1834–C1842
Spector JA, Greenwald JA, Warren SM, Bouletreau PJ, Crisera FE, Mehrara BJ, Longaker MT (2002) Co-culture of osteoblasts with immature dural cells causes an increased rate and degree of osteoblast differentiation. Plast Reconstr Surg 109(2):631–642 (discussion 643-634)
Ahuja SK, Murphy PM (1996) The CXC chemokines growth-regulated oncogene (GRO) alpha, GRObeta, GROgamma, neutrophil-activating peptide-2, and epithelial cell-derived neutrophil-activating peptide-78 are potent agonists for the type B, but not the type A, human interleukin-8 receptor. J Biol Chem 271(34):20545–20550. https://doi.org/10.1074/jbc.271.34.20545
Murphy PM, Tiffany HL (1991) Cloning of complementary DNA encoding a functional human interleukin-8 receptor. Science 253(5025):1280–1283. https://doi.org/10.1126/science.1891716
Lee J, Horuk R, Rice GC, Bennett GL, Camerato T, Wood WI (1992) Characterization of two high affinity human interleukin-8 receptors. J Biol Chem 267(23):16283–16287
Rajagopalan L, Rajarathnam K (2004) Ligand selectivity and affinity of chemokine receptor CXCR1. Role of N-terminal domain. J Biol Chem 279(29):30000–30008. https://doi.org/10.1074/jbc.M313883200
Attal H, Cohen-Hillel E, Meshel T, Wang JM, Gong W, Ben-Baruch A (2008) Intracellular cross-talk between the GPCR CXCR1 and CXCR2: role of carboxyl terminus phosphorylation sites. Exp Cell Res 314(2):352–365. https://doi.org/10.1016/j.yexcr.2007.09.019
Richardson RM, Pridgen BC, Haribabu B, Ali H, Snyderman R (1998) Differential cross-regulation of the human chemokine receptors CXCR1 and CXCR2. Evidence for time-dependent signal generation. J Biol Chem 273(37):23830–23836. https://doi.org/10.1074/jbc.273.37.23830
Shamaladevi N, Lyn DA, Escudero DO, Lokeshwar BL (2009) CXC receptor-1 silencing inhibits androgen-independent prostate cancer. Cancer Res. https://doi.org/10.1158/0008-5472.CAN-09-0374
Lee LF, Louie MC, Desai SJ, Yang J, Chen HW, Evans CP, Kung HJ (2004) Interleukin-8 confers androgen-independent growth and migration of LNCaP: differential effects of tyrosine kinases Src and FAK. Oncogene 23(12):2197–2205. https://doi.org/10.1038/sj.onc.1207344
Seaton A, Scullin P, Maxwell PJ, Wilson C, Pettigrew J, Gallagher R, O’Sullivan JM, Johnston PG, Waugh DJ (2008) Interleukin-8 signaling promotes androgen-independent proliferation of prostate cancer cells via induction of androgen receptor expression and activation. Carcinogenesis 29(6):1148–1156. https://doi.org/10.1093/carcin/bgn109
Acknowledgements
The authors would like to thank Tom Cichonski for assistance with the preparation of this manuscript.
Funding
This work was supported in part by National Institutes of Health grant R21NS107879 (Alexandra Calinescu), P01CA093900 (R.T.), Rogel Cancer Center Grant G020989 (Alexandra Calinescu, N.J.S.), the Department of Defense Prostate Cancer Research Program PC170089 Early Investigator Award (N.J.S.), and VA Merit Review 1I01BX001370 (G.A.C.).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation and data collection and analysis were performed by MS, SR, RT, GC, and NS. The first draft of the manuscript was written by MS and NS, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Strong, M.J., Rocco, S., Taichman, R. et al. Dura promotes metastatic potential in prostate cancer through the CXCR2 pathway. J Neurooncol 153, 33–42 (2021). https://doi.org/10.1007/s11060-021-03752-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-021-03752-4