Abstract
Purpose
To characterize solid maltose microneedles and assess their ability to increase transdermal drug delivery.
Materials and Methods
Microneedles and microchannels were characterized using methylene blue staining and scanning electron microscopy. Diffusion pattern of calcein was observed using confocal scanning laser microscopy. Transepidermal water loss (TEWL) measurements were made to study the skin barrier recovery after treatment. Uniformity in calcein uptake by the pores was characterized and percutaneous penetration of nicardipine hydrochloride (NH) was studied in vitro and in vivo across hairless rat skin.
Results
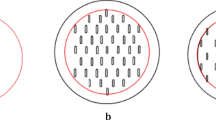
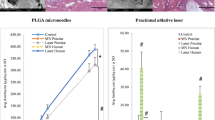
Microneedles were measured to be 508.46 ± 9.32 μm long with a radius of curvature of 3 μm at the tip. They penetrated the skin while creating microchannels measuring about 55.42 ± 8.66 μm in diameter. Microchannels were visualized by methylene blue staining. Pretreatment with microneedles resulted in the migration of calcein into the microchannels. TEWL increased after pretreatment and uptake of calcein by the pores was uniform as measured by the pore permeability index values. NH in vitro transport across skin increased significantly after pretreatment (flux 7.05 μg/cm2/h) as compared to the untreated skin (flux 1.72 μg/cm2/h) and the enhanced delivery was also demonstrated in vivo in hairless rats.
Conclusion
Maltose microneedles were characterized and shown to create microchannels in the skin, which were also characterized and shown to improve the transdermal delivery of NH.








Similar content being viewed by others
Abbreviations
- NH:
-
Nicardipine hydrochloride
- PPI:
-
Pore Permeability Index
- SC:
-
Stratum corneum
- SEM:
-
Scanning electron microscope
- TEWL:
-
Transepidermal water loss
References
M. Kendall. Engineering of needle-free physical methods to target epidermal cells for DNA vaccination. Vaccine 24:4651–4656 (2006).
S. Coulman, C. Allender, and J. Birchall. Microneedles and other physical methods for overcoming the stratum corneum barrier for cutaneous gene therapy. Crit. Rev. Ther. Drug Carr. Syst. 23:205–258 (2006).
A. K. Banga. New technologies to allow transdermal delivery of therapeutic proteins and small water-soluble drugs. Am. J. Drug Deliv. 4:221–230 (2006).
S. Henry, D. V. McAllister, M. G. Allen, and M. R. Prausnitz. Microfabricated microneedles: a novel approach to transdermal drug delivery. J. Pharm. Sci. 87:922–925 (1998).
A. L. Teo, C. Shearwood, K. C. Ng, L. Jia, and S. Moochhala. Transdermal microneedles for drug delivery applications. Mater. Sci. Eng. B 132:155–158 (2006).
Y. Ito, E. Hagiwara, A. Saeki, N. Sugioka, and K. Takada. Feasibility of microneedles for percutaneous absorption of insulin. Eur. J. Pharm. Sci. 29:82–88 (2006).
S. C. Kuo and Y. Chou. A novel polymer microneedle arrays and PDMS micromolding technique. Tamkang J. Sci. Eng. 7:95–98 (2004).
J. H. Park, M. G. Allen, and M. R. Prausnitz. Biodegradable polymer microneedles: fabrication, mechanics and transdermal drug delivery. J. Control. Release 104:51–66 (2005).
C. M. Fernandes, V. M. Teresa, and F. J. Veiga. Physicochemical characterization and in vitro dissolution behavior of nicardipine-cyclodextrins inclusion compounds. Eur. J. Pharm. Sci. 15:79–88 (2002).
E. M. Sorkin and S. P. Clissold. Nicardipine. A review of its pharmacodynamic and pharmacokinetic properties, and therapeutic efficacy, in the treatment of angina pectoris, hypertension and related cardiovascular disorders. Drugs 33:296–345 (1987).
I. Diez, H. Colom, J. Moreno, R. Obach, C. Peraire, and J. Domenech. A comparative in vitro study of transdermal absorption of a series of calcium channel antagonists. J. Pharm. Sci. 80:931–934 (1991).
T. Miyano, Y. Tobinaga, T. Kanno, Y. Matsuzaki, H. Takeda, M. Wakui, and K. Hanada. Sugar micro needles as transdermic drug delivery system. Biomed. Microdevices. 7:185–188 (2005).
J. Pinnagoda, R. A. Tupker, T. Agner, and J. Serup. Guidelines for transepidermal water loss (TEWL) measurement. A report from the Standardization Group of the European Society of Contact Dermatitis. Contact Dermatitis 22:164–178 (1990).
P. J. Caspers, G. W. Lucassen, H. A. Bruining, and G. J. Puppels. Automated depth-scanning confocal Raman microspectrometer for rapid in vivo determination of water concentration profiles in human skin. J. Raman Spectrosc. 31:813–818 (2000).
W. Martanto, J. S. Moore, T. Couse, and M. R. Prausnitz. Mechanism of fluid infusion during microneedle insertion and retraction. J. Control. Release 112:357–361 (2006).
N. G. Turner and R. H. Guy. Visualization and quantitation of iontophoretic pathways using confocal microscopy. J. Investig. Dermatol. Symp. Proc. 3:136–142 (1998).
G. Cevc and G. Blume. Lipid vesicles penetrate into intact skin owing to the transdermal osmotic gradients and hydration force. Biochim. Biophys. Acta 1104:226–232 (1992).
K. V. Roskos and R. H. Guy. Assessment of skin barrier function using transepidermal water loss: effect of age. Pharm. Res. 6:949–953 (1989).
F. Benech-Kieffer, P. Wegrich, and H. Schaefer. Transepidermal water loss as an integrity test for skin barrier function in vitro: assay standardization. In K. R. Brain, V. J. James, and K. A. Walters (eds.), Perspectives in Percutaneous Penetration, STS, Cardiff, (1997), p. 56.
A. C. Sintov, I. Krymberk, D. Daniel, T. Hannan, Z. Sohn, and G. Levin. Radiofrequency-driven skin microchanneling as a new way for electrically assisted transdermal delivery of hydrophilic drugs. J. Control. Release 89:311–320 (2003).
Cardene (nicardipine hydrochloride) injection; http://dailymed.nlm.nih.gov/dailymed/fdaDrugXsl.cfm?id=3820&type=display (Accessed 4-25-2007).
R. Panchagnula, R. Bokalial, P. Sharma, and S. Khandavilli. Transdermal delivery of naloxone: skin permeation, pharmacokinetic, irritancy and stability studies. Int. J. Pharm. 293:213–223 (2005).
Nicardipine Hydrochloride capsule [GENPHARM INC.]; http://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?id=2762 (Accessed 05-05-07).
Acknowledgements
Microneedles required for the study were developed and supplied by Texmac Inc. We thank Dr. Lisa Hoskin and Gautam Patel (Georgia Tech Research Institute, Atlanta, GA) for their help with SEM and Videomicroscope images; Janice Taylor, University of Nebraska Medical center (Omaha, NE) for help with confocal microscopy and David Farquhar, Altea Therapeutics (Tucker, GA), for help in image processing.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kolli, C.S., Banga, A.K. Characterization of Solid Maltose Microneedles and their Use for Transdermal Delivery. Pharm Res 25, 104–113 (2008). https://doi.org/10.1007/s11095-007-9350-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-007-9350-0