Abstract
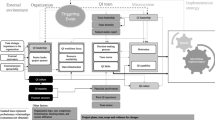
The outcomes of lean projects have been mixed, with some being successful while many others have not. An explanation for this is a paradox that can develop depending on the focus of the project. Ironically, in projects where the focus is on maximizing the efficiency of a resource (‘resource efficiency’), this focus might lead to worsening of the resource’s efficiency, thereby generating an ‘efficiency paradox’. This paradox does not usually arise in projects where the focus is on the subject of interest being processed through the system in the most efficient manner (‘flow efficiency’). The aim of this paper is to investigate the factors that give rise to either form of efficiency. We conducted a detailed study of eight lean projects in two large hospitals. In doing so, we advance the theory of lean service operations by identifying four key contextual factors that drive the orientation of a project to resource or flow efficiency. These are: service variety, interdependency, capital resource intensity, and service uniqueness. We propose a conceptual framework and four propositions that integrate the contextual factors to determine the dominant focus in lean projects. Through this, recommendations are made as to how the efficiency paradox can be avoided.


Similar content being viewed by others
References
Ahlstrom P (2004) Lean service operations: translating lean production principles to service operations. Int J Serv Technol Manag 5:545–564
Anand G, Chhajed D, Delfin L (2012) Job autonomy, trust in leadership, and continuous improvement: an empirical study in health care. Oper Manag Res 5:70–80
Arkader R (2001) The perspective of suppliers on lean supply in a developing country context. Integr Manuf Syst 12:87–93
Arlbjørn JS, Freytag PV (2013) Evidence of lean: a review of international peer-reviewed journal articles. Eur Bus Rev 25:174–205
Balle M (2005) Lean attitude. Manuf Eng 84:14–19
Bamford D, Forrester P, Dehe B, Leese RG (2015) Partial and iterative lean implementation: two case studies. Int J Oper Prod Manag 35:702–727
Belter D et al (2012) Evaluation of outpatient oncology services using lean methodology. Oncol Nurs Forum 39:136–140
Coelli TJ, Rao DSP, O'Donnell CJ, Battese GE (2005) An introduction to efficiency and productivity analysis, 2nd edn. Springer Science & Business Media, New York
Dahlgaard JJ, Dahlgaard-Park SM (2006) Lean production, six sigma quality, TQM and company culture. TQM Mag 18:263–281
De Souza LB (2009) Trends and approaches in lean healthcare. Leadersh Health Serv 22:121–139
De Treville S, Antonakis J (2006) Could lean production job design be intrinsically motivating? Contextual, configurational, and levels-of-analysis issues. J Oper Manag 24:99–123
DelliFraine JL, Langabeer JR, Nembhard IM (2010) Assessing the evidence of six sigma and lean in the health care industry. Qual Manag Healthcare 19:211–225
Eisenhardt KM (1989) Building theories from case study research. Acad Manag Rev 14:532–550
Gioia DA, Corley KG, Hamilton AL (2013) Seeking qualitative rigor in inductive research: notes on the Gioia methodology. Organ Res Methods 16:15–31
Hillman K, Braithwaite J, Chen J (2011) Healthcare systems and their (lack of ) integration. In: DeVita MA, Hillman K, Bellomo R (eds) Textbook of rapid respond systems. Springer, New York, pp 79–86
Holweg M (2007) The genealogy of lean production. J Oper Manag 25:420–437
Hopp WJ, Spearman ML (2004) To pull or not to pull: what is the question? Manuf Serv Oper Manag 6:133–148
Krafcik JF (1988) Triumph of the lean production system. Sloan Manag Rev 30:41–52
LaGanga LR (2011) Lean service operations: reflections and new directions for capacity expansion in outpatient clinics. J Oper Manag 29:422–433
Lee RH, Bott MJ, Gajewski B, Taunton RL (2009) Modeling efficiency at the process level: an examination of the care planning process in nursing homes. Health Serv Res 44:15–32
Marley K, Ward P (2013) Lean management as a countermeasure for “normal” disruptions. Oper Manag Res 6:44–52
Mazzocato P, Savage C, Brommels M, Aronsson H, Thor J (2010) Lean thinking in healthcare: a realist review of the literature. Qual Saf Health Care 19:376–382
McDermott C, Venditti F (2015) Implementing lean in knowledge work: implications from a study of the hospital discharge planning process. Oper Manag Res:1–13
Meijboom BR, Bakx SJWGC, Westert GP (2010) Continuity in health care: lessons from supply chain management. Int J Health Plann Manag 25:304–317
Meredith J, Grove A, Walley P, Young F, Macintyre M (2011) Are we operating effectively? A lean analysis of operating theatre changeovers. Oper Manag Res 4:89–98
Meyer V Jr, Pascucci L, Murphy JP (2012) Implementing strategies in complex systems: lessons from Brazilian hospitals. Braz Adm Rev 9:19–37
Modig N, Åhlström P (2012) This is Lean: Resolving the Efficiency Paradox. Rheologica, Sweden
New SJ (2007) Celebrating the enigma: the continuing puzzle of the Toyota production system. Int J Prod Res 45:3545–3554
Papadopoulos T, Radnor Z, Merali Y (2011) The role of actor associations in understanding the implementation of lean thinking in healthcare. Int J Oper Prod Manag 31:167–191
Pegels CC (1984) The Toyota production system-lessons for American management. Int J Oper Prod Manag 4:3–11
Poksinska B (2010) The current state of lean implementation in health care: literature review. Qual Manag Healthcare 19:319–329
Radnor Z (2010) Transferring lean into government. J Manuf Technol Manag 21:411–428
Radnor Z (2011) Implementing lean in health care: making the link between the approach, readiness and sustainability. Int J Ind Eng Manag 2:1–12
Radnor ZJ, Holweg M, Waring J (2012) Lean in healthcare: the unfilled promise? Soc Sci Med 74:364–371
Seddon J (2011) Lean is a waning fad. Manag Serv 55:34–36
Shah R, Ward PT (2003) Lean manufacturing: context, practice bundles, and performance. J Oper Manag 21:129–149
Shah R, Ward PT (2007) Defining and developing measures of lean production. J Oper Manag Organ Rev 25:785–805
Shah R, Goldstein SM, Unger BT, Henry TD (2008) Explaining anomalous high performance in a health care supply chain*. Decis Sci 39:759–789
Spear SJ (2005) Fixing health care from the inside, today. Harv Bus Rev 83:78
Staats B, Upton DM (2011) Lean knowledge work. Harv Bus Rev 89:100–110
Staats B, Brunner DJ, Upton DM (2011) Lean principles, learning, and knowledge work: evidence from a software services provider. J Oper Manag 29:376–390
Stake RE (1995) The art of case study research. Sage, London
Strauss A, Corbin J (1990) Basics of qualitative research. Sage, Newbury Park
Taylor A, Taylor M, McSweeney A (2013) Towards greater understanding of success and survival of lean systems. Int J Prod Res 51:6607–6630
Tucker AL, Singer SJ, Hayes JE, Falwell A (2008) Front-line staff perspectives on opportunities for improving the safety and efficiency of hospital work systems. Health Serv Res 43:1807–1829
Van Aken EM (2010) A framework for designing, managing, and improving kaizen event programs. Int J Product Perform Manag 59:641–667
Van Maanen J (1979) The fact of fiction in organizational ethnography. Adm Sci Q 24:539–550
Waring JJ, Bishop S (2010) Lean healthcare: rhetoric, ritual and resistance. Soc Sci Med 71:1332–1340
Weber D (2006) Toyota-style management drives. Va Mason Physician Exec 32:12
Womack JP, Jones DT (1996) Lean thinking: banish waste and create wealth in your corporation. Simon and Schuster, New York
Womack JP, Jones DT, Roos D (1990) The machine that changed the world. Rawson Associates, New York
Yin RK (2003) Case study research: design and methods. Sage, London
Young TP, McClean SI (2008) A critical look at lean thinking in healthcare. Qual Saf Health Care 17:382–386
Author information
Authors and Affiliations
Corresponding author
Appendices
Appendix 1: Questions in the Semi-Structured Interview Protocol
-
How would you describe the constraints that are limiting the work processes in this project?
-
What are the main causes of these limiting factors?
-
How has lean affected the current practice in managing the internal operations in your service areas?
-
How would you describe the impact of the lean project in your service areas?
-
Is there improvement in efficiency performance?
-
What outcomes have resulted from the lean practices?
-
Have the expected outcome/s been achieved?
-
Have the improved outcomes been able to sustain over time?
Appendix 2
Rights and permissions
About this article
Cite this article
Tay, H.L., Singh, P.J., Bhakoo, V. et al. Contextual factors: assessing their influence on flow or resource efficiency orientations in healthcare lean projects. Oper Manag Res 10, 118–136 (2017). https://doi.org/10.1007/s12063-017-0126-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12063-017-0126-3