Abstract
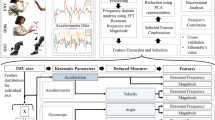
Cerebellar dysfunction results in impairments in co-ordination or ‘ataxia’. Bedside examination of cerebellar function has changed little since the early nineteenth century with the exception being the oculomotor examination which has become instrumented. Otherwise, competence and confidence in performing the clinical assessment relies heavily on the skill and experience of the clinician. Potentially, instrumented objective measurement will more accurately assess the severity of ataxia and the changes brought about by advancing therapies in pharmaceutical trials and in rehabilitation intervention. This study describes instrumented versions of several bedside tests of cerebellar function, including rhythmic tapping of the hand (RTH), finger-nose test (FNT), dysdiadochokinesia (DDK), ramp tracking (RMT), ballistic tracking (BT), rhythmic tapping of the foot (RTF) and the heel shin (HST) examination which were validated against scores from Ataxia Rating Scales (ARS) such as the Scale of Assessment and Rating of Ataxia (SARA). While all of the instrumented tests accurately distinguished between ataxic subjects and controls, there was a difference in performance, with the best four performing upper limb tests being RTH, FNT, DDK and BT. A combination of BT plus RTH provided the best correlation with the SARA and outperformed a combination of all the bedside tests (Spearman 0.8; p < 0.001 compared to 0.68; p < 0.001 for the combined set) in identifying the presence and severity of ataxia. This indicates that there is redundancy in the information provided by the bedside tests and that adding other tests to BT plus RTH does not add accuracy to the assessment of ataxia. This analysis highlighted the need for metrics that could be generalised to each of the assessments of ataxia, so, in turn, domains of stability, timing, accuracy and rhythmicity (STAR domains) were developed and compared to the SARA. The STAR criteria could potentially influence the future of instrumented assessment in CA and pave the way for further research into the objective measurement of the cerebellar examination.



Similar content being viewed by others
Notes
It must be emphasised that the relevant publications must be followed for the details of model building for each test as each followed a slightly different path.
References
Fine EJ. The History of the Development of the Cerebellar Examination. Semin Neurol. 2002;22(4):375–84.
Luciani L. Il Cervelletto: Nuovi Studi di Fisiologia normale e palologica. Firenze; Le Monnier, 1891.
Russell JSR. Experimental researchers into the functions of the cerebellum. Philos Trans R Soc Lond B. 1894;185:819–61.
Lewandowsky M. Ueber die Verrichtungen des Kleinhirns. 1903.
Holmes G. The Croonian Lectures On The Clinical Symptoms Of Cerebellar Disease And Their Interpretation. Lecture I. 1922. Cerebellum. 2007;6(2):142–7.
Holmes G. The symptoms of acute cerebellar injuries due to gunshot injuries. Brain. 1917;40(4):461–535.
Saute JAM, et al. Ataxia Rating Scales--Psychometric Profiles, Natural History and Their Application in Clinical Trials. Cerebellum. 2012;2:488.
Trouillas P, Takayanagi T, Hallett M, Currier RD, Subramony SH, Wessel K, et al. International Cooperative Ataxia Rating Scale for pharmacological assessment of the cerebellar syndrome. The Ataxia Neuropharmacology Committee of the World Federation of Neurology. J Neurol Sci. 1997;145(2):205–11.
Schmitz-Hubsch T, et al. Scale for the assessment and rating of Ataxia: Development of a new clinical scale. Neurology. 2006;66:1717–20.
Schmahmann JD, et al. Development of a brief ataxia rating scale (BARS) based on a modified form of the ICARS. Hoboken: Wiley; 2009. p. 1820.
Subramony SH, May W, Lynch D, Gomez C, Fischbeck K, Hallett M, et al. Measuring Friedreich ataxia: Interrater reliability of a neurologic rating scale. Neurology. 2005;64(7):1261–2.
Holmes G. The Croonian Lectures on the clinical symptoms of cerebellar disease and thier interpretation. Lecture II. Cerebellum. 1922;6(2):148–53.
Babinski J. De J’asynergie cérébelleuse. Rev Neurol. 1899;7:789.
Marr D. A theory of cerebellar cortex. J Physiol. 1969;202(2):437–70.
Albus JS. A theory of cerebellar function. Math Biosci. 1971;10:25–61.
Llinas RL. The Olivo-cerebellar System: A Key to understanding the functional significance of intrinsic oscillatory brain properties. Front Neural Circuits. 2014;7:96.
Popa LS, Ebner TJ. Cerebellum, Predictions and Errors. Front Cell Neurosci. 2019.
Becker MI, Person AL. Cerebellar Control of Reach Kinematics for Endpoint Precision. Neuron. 2019;103(2):335–348.e5.
Phan D, Nguyen N, Pathirana P, Horne M, Power L, Szmulewicz D. A Random Forest Approach for Quantifying Gait Ataxia with Truncal and Peripheral Measurements using Multiple Wearable Sensors. IEEE Sensors J. 2019;99:1.
Nguyen KD, Pathirana PN, Horne M, Power L, Szmulewicz D. Quantitative Assessment of Cerebellar Ataxia with Kinematic sensing during Rhythmic Tapping, In: Engineering in Medicine and Biology Society (EMBC). 2018.
Tran H, Pathirana P, Horne M, Power L, Szmulewicz D. Automated finger chase (ballistic tracking) in the assessment of cerebellar ataxia, In: 40th Annual international conference of the IEEE, Engineering in Medicine and Biology: Honolulu, Hawaii; 2018.
Nguyen K, Phan D, Pathirana PN, Horne M, Power L, Szmulewicz D. Quantification of axial abnormality due to cerebellar ataxia with inertial measurements. Sensors. 2018;18(9):2791.
Krishna R, Pathirana PN, Horne M, Power L, Szmulewicz DJ. Quantitative assessment of cerebellar ataxia, through automated limb functional tests. J Neuroeng Rehabil. 2019;16(1):31.
Kashyap B, Pathirana P, Horne M, Power L, Szmulewicz D. Identification of Cerebellar Dysarthria with SISO Characterisation, In: 17th International Conference on Bioinformatics and Bioengineering (BIBE): Washington, DC, USA; 2017.
Kashyap B, Pathirana P, Horne M, Power L, Szmulewicz D. Quantitative assessment of syllabic timing deficits in ataxic dysarthria, In: Engineering in medicine and Biology Society 40th Annual conference. Piscataway, New Jersey; 2017. p. 1-4.
Tran H, et al. Automated Finger Chase (ballistic tracking) in the Assessment of Cerebellar Ataxia. Conference proceedings : ... Annual International Conference of the IEEE Engineering in Medicine and Biology Society. IEEE Engineering in Medicine and Biology Society. Annual Conference, 2018. 2018. p. 3521-3524.
Nguyen KD, et al. Quantitative Assessment of Cerebellar Ataxia With Kinematic Sensing During Rhythmic Tapping. In: 2018 40th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC). 2018.
Kashyap B, Pathirana P, Horne M, Power L, Szmulewicz D. Automated tongue-twister phrase-based screening for Cerebellar Ataxia using Vocal tract Acoustic Biomarkers, In: 2019 41st Annual International Conference of the IEEE Engineering in Medicine & Biology Society (EMBC). 2019.
Phan D, Nguyen N, Pathirana PN, Horne M, Power L, Szmulewicz D. Assessment of abnormal gait due to cerebellar ataxia using inertial sensing at different walking speeds, In: 2019 41st Annual International Conference of the IEEE Engineering in Medicine & Biology Society (EMBC). 2019.
Tran H, Pathirana PN, Horne M, Power L, Szmulewicz DJ. Quantitative Evaluation of Cerebellar Ataxia Through Automated Assessment of Upper Limb Movements. IEEE Trans Neural Syst Rehabil Eng. 2019;27(5):1081–91.
Therrien AS, Bastian AJ. The cerebellum as a movement sensor. Neurosci Lett. 2019;688:37–40.
Sherrington CS. The integrative action of the nervous system. Yale University Press; 1961.
Nguyen KD, Pathirana PN, Horne M, Power L, Szmulewicz D. Quantitative assessment of cerebellar ataxia with kinematic sensing during rhythmic tapping. Annual International Conference IEEE. Eng Med Biol Soc. 2018;2018:1098–1101.
Phan D, Nguyen N, Pathirana PN, Horne M, Power L, Szmulewicz D. Quantitative assessment of ataxic gait using inertial sensing at different walking speeds. Annu Int Conf IEEE Eng Med Biol Soc. 2019;2019:4600–3.
Kashyap B, Phan D, Pathirana P, Horne M, Power L, Szmulewicz D. Objective Assessment of Cerebellar Ataxia: A Comprehensive and Refined Approach. Nat Sci Rep. 2020;10:9493.
Ekanayake SW, Morris AJ, Forrester M, Pathirana PN. BioKin: an ambulatory platform for gait kinematic and feature assessment. Healthc Technol Lett. 2015;2(1):40–5.
Ding WL, Zheng YZ, Su YP, Li XL. Kinect-based virtual rehabilitation and evaluation system for upper limb disorders: A case study. J Back Musculoskelet Rehabil. 2018;31(4):611–21.
Tran H, Nguyen KD, Pathirana PN, Horne MK, Power L, Szmulewicz DJ. A comprehensive scheme for the objective upper body assessments of subjects with cerebellar ataxia. J Neuroeng Rehabil. 2020;17(1):162.
Krishna R, Pathirana PN, Horne M, Power L, Szmulewicz D. Quantitative assessment of cerebellar ataxia through automated upper limb functional tests. J Neuroeng Rehabil. 2018;16(31):6.
Tran H, Pathirana PN, Horne M, Power L, Szmulwewicz DJ. Quantitative Evaluation of Cerebellar Ataxia through Automated Assessment of Upper Limb Movements, In: IEEE Transactions on Neural Systems and Rehabilitation Engineering. 2019.
Nguyen KD, Pathirana PN, Horne M, Szmulewicz D. Entropy based analysis of rhythmic tapping for the quantitative assessment of cerebellar ataxia. Biomed Signal Process Control. 2020;59:101916.
Funding
This research is supported by the Royal Victorian Eye and Ear Hospital (RVEEH) and the Florey Institute of Neuroscience and Mental Health, Melbourne, Australia, through the National Health and Medical Research Council (NHMRC) (Grant: GNT1101304 and APP1129595) and CSIRO Data61.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 24 kb).
Rights and permissions
About this article
Cite this article
Power, L., Pathirana, P., Horne, M. et al. Instrumented Objective Clinical Examination of Cerebellar Ataxia: the Upper and Lower Limb—a Review. Cerebellum 21, 145–158 (2022). https://doi.org/10.1007/s12311-021-01253-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12311-021-01253-8