Abstract
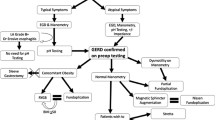
The Indian Society of Gastroenterology developed this evidence-based practice guideline for management of gastroesophageal reflux disease (GERD) in adults. A modified Delphi process was used to develop this consensus containing 58 statements, which were generated by electronic voting iteration as well as face-to-face meeting and review of the supporting literature primarily from India. These statements include 10 on epidemiology, 8 on clinical presentation, 10 on investigations, 23 on treatment (including medical, endoscopic, and surgical modalities), and 7 on complications of GERD. When the proportion of those who voted either to accept completely or with minor reservation was 80% or higher, the statement was regarded as accepted. The prevalence of GERD in India ranges from 7.6% to 30%, being < 10% in most population studies, and higher in cohort studies. The dietary factors associated with GERD include use of spices and non-vegetarian food. Helicobacter pylori is thought to have a negative relation with GERD; H. pylori negative patients have higher grade of symptoms of GERD and esophagitis. Less than 10% of GERD patients in India have erosive esophagitis. In patients with occasional or mild symptoms, antacids and histamine H2 receptor blockers (H2RAs) may be used, and proton pump inhibitors (PPI) should be used in patients with frequent or severe symptoms. Prokinetics have limited proven role in management of GERD.

Similar content being viewed by others
References
Bhatia SJ, Reddy DN, Ghoshal UC, et al. Epidemiology and symptom profile of gastroesophageal reflux in the Indian population: report of the Indian Society of Gastroenterology Task Force. Indian J Gastroenterol. 2011;30:118–27.
Chowdhury SD, George G, Ramakrishna K, et al. Prevalence and factors associated with gastroesophageal reflux disease in southern India: a community-based study. Indian J Gastroenterol. 2019;38:77–82.
Wang HY, Leena KB, Plymoth A, et al. Prevalence of gastro-esophageal reflux disease and its risk factors in a community-based population in southern India. BMC Gastroenterol. 2016;16:36.
Kumar S, Sharma S, Norboo T, et al. Population based study to assess prevalence and risk factors of gastroesophageal reflux disease in a high altitude area. Indian J Gastroenterol. 2011;30:135–43.
Amarapurkar AD, Vora IM, Dhawan PS. Barrett’s esophagus. Indian J Pathol Microbiol. 1998;41:431–5.
Linstone H, Turoff M. The Delphi method: techniques and application http://www.is.njit.edu/pubs/delphibook/. Accessed 15 Aug 2012.
Periodic health examination: 2. 1984 update. Canadian Task Force on the Periodic Health Examination. Can Med Assoc J. 1984;130:1278–85.
Vakil N, van Zanten SV, Kahrilas P, Dent J, Jones R, Global Consensus G. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol. 2006;101:1900–20.
Sharma PK, Ahuja V, Madan K, Gupta S, Raizada A, Sharma MP. Prevalence, severity, and risk factors of symptomatic gastroesophageal reflux disease among employees of a large hospital in northern India. Indian J Gastroenterol. 2011;30:128–34.
Bhalaghuru CM, Vijaya S, Jayanthi V. Symptomatic gastroesophageal reflux amongst hospital personnel in South India. Indian J Med Sci. 2011;65:355–9.
Bhatia S, Gupta D, Vennalaganti P. Epidemiology of gastroesophageal reflux in Asia. The rise of acid reflux in Asia. J Neurogastroenterol Motil. 2017;17:14–27.
El-Serag HB, Sweet S, Winchester CC, Dent J. Update on the epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut. 2014;63:871–80.
Eusebi LH, Ratnakumaran R, Yuan Y, Solaymani-Dodaran M, Bazzoli F, Ford AC. Global prevalence of, and risk factors for, gastro-oesophageal reflux symptoms: a meta-analysis. Gut. 2018;67:430–40.
Chang P, Friedenberg F. Obesity and GERD. Gastroenterol Clin N Am. 2014;43:161–73.
Vaishnav B, Bamanikar A, Maske P, Reddy A, Dasgupta S. Gastroesophageal reflux disease and its association with body mass index: clinical and endoscopic study. J Clin Diagn Res. 2017;11:OC01–4.
National Nutrition Monitoring Bureau, NNMB Technical Report No. 26, Diet and nutritional status of rural population, prevalence of hypertension & diabetes among adults and infant & young child feeding practices, Report of Third Repeat Survey National Institute of Nutrition, Indian Council of Medical Research, Hyderabad, India – 2012. Available at: http://nnmbindia.org. Accessed 08 May 2019.
Corley DA, Kubo A. Body mass index and gastroesophageal reflux disease: a systematic review and meta-analysis. Am J Gastroenterol. 2006;101:2619–28.
Këlliçi I, Kraja B. Smoking, alcohol, physical activity and gastroesophageal reflux disease: a literature review and the Albanian experience. Albanian Medical Journal. 2014;4:91–8.
Sethi S, Richter JE. Diet and gastroesophageal reflux disease: role in pathogenesis and management. Curr Opin Gastroenterol. 2017;33:107–11.
Arivan R, Deepanjali S. Prevalence and risk factors of gastro-esophageal reflux disease among undergraduate medical students from a southern Indian medical school: a cross-sectional study. BMC Res Notes. 2018;11:448.
Kim J, Oh SW, Myung SK, et al. Association between coffee intake and gastroesophageal reflux disease: a meta-analysis. Dis Esophagus. 2014;27:311–7.
Ghoshal UC, Chourasia D. Gastroesophageal reflux disease and Helicobacter pylori: what may be the relationship? J Neurogastroenterol Motil. 2010;16:243–50.
Goh KL. Gastroesophageal reflux disease in Asia: a historical perspective and present challenges. J Gastroenterol Hepatol. 2011;26 Suppl 1:2–10.
Peng S, Cui Y, Xiao YL, et al. Prevalence of erosive esophagitis and Barrett’s esophagus in the adult Chinese population. Endoscopy. 2009;41:1011–7.
Nam SY, Choi IJ, Ryu KH, Kim BC, Kim CG, Nam BH. Effect of Helicobacter pylori infection and its eradication on reflux esophagitis and reflux symptoms. Am J Gastroenterol. 2010;105:2153–62.
Gerson LB, Kahrilas PJ, Fass R. Insights into gastroesophageal reflux disease-associated dyspeptic symptoms. Clin Gastroenterol Hepatol. 2011;9:824–33.
Ghoshal UC, Abraham P, Bhatt C, et al. Epidemiological and clinical profile of irritable bowel syndrome in India: report of the Indian Society of Gastroenterology Task Force. Indian J Gastroenterol. 2008;27:22–8.
Lovell RM, Ford AC. Prevalence of gastro-esophageal reflux-type symptoms in individuals with irritable bowel syndrome in the community: a meta-analysis. Am J Gastroenterol. 2012;107:1793–801.
Fock KM, Talley N, Goh KL, et al. Asia-Pacific consensus on the management of gastro-oesophageal reflux disease: an update focusing on refractory reflux disease and Barrett’s oesophagus. Gut. 2016;65:1402–15.
Richter JE, Rubenstein JH. Presentation and epidemiology of gastroesophageal reflux disease. Gastroenterology. 2018;154:267–76.
Baruah B, Kumar T, Das P, et al. Prevalence of eosinophilic esophagitis in patients with gastroesophageal reflux symptoms: a cross-sectional study from a tertiary care hospital in North India. Indian J Gastroenterol. 2017;36:353–60.
Irvine EJ. Quality of life assessment in gastro-oesophageal reflux disease. Gut. 2004;53 Suppl 4:iv35–9.
Quigley EM, Hungin AP. Review article: quality-of-life issues in gastro-oesophageal reflux disease. Aliment Pharmacol Ther. 2005;22 Suppl 1:41–7.
Becher A, El-Serag H. Systematic review: The association between symptomatic response to proton pump inhibitors and health-related quality of life in patients with gastro-oesophageal reflux disease. Aliment Pharmacol Ther. 2011;34:618–27.
Bitnar P, Stovicek J, Andel R, et al. Leg raise increases pressure in lower and upper esophageal sphincter among patients with gastroesophageal reflux disease. J Bodyw Mov Ther. 2016;20:518–24.
Sodhi JS, Zargar SA, Javid G, et al. Effect of bending exercise on gastroesophageal reflux in symptomatic patients. Indian J Gastroenterol. 2008;27:227–31.
Khan BA, Sodhi JS, Zargar SA, et al. Effect of bed head elevation during sleep in symptomatic patients of nocturnal gastroesophageal reflux. J Gastroenterol Hepatol. 2012;27:1078–82.
Allampati S, Lopez R, Thota PN, Ray M, Birgisson S, Gabbard SL. Use of a positional therapy device significantly improves nocturnal gastroesophageal reflux symptoms. Dis Esophagus. 2017;30:1–7.
Hamilton JW, Boisen RJ, Yamamoto DT, Wagner JL, Reichelderfer M. Sleeping on a wedge diminishes exposure of the esophagus to refluxed acid. Dig Dis Sci. 1988;33:518–22.
Pollmann H, Zillessen E, Pohl J, et al. Effect of elevated head position in bed in therapy of gastroesophageal reflux. Z Gastroenterol. 1996;34 Suppl 2:93–9.
van Herwaarden MA, Katzka DA, Smout AJ, Samsom M, Gideon M, Castell DO. Effect of different recumbent positions on postprandial gastroesophageal reflux in normal subjects. Am J Gastroenterol. 2000;95:2731–6.
Khoury RM, Camacho-Lobato L, Katz PO, Mohiuddin MA, Castell DO. Influence of spontaneous sleep positions on nighttime recumbent reflux in patients with gastroesophageal reflux disease. Am J Gastroenterol. 1999;94:2069–73.
Orr WC. Sleep and gastroesophageal reflux: what are the risks? Am J Med. 2003;115:109–3S.
Shoenut JP, Yamashiro Y, Orr WC, Kerr P, Micflikier AB, Kryger MH. Effect of severe gastroesophageal reflux on sleep stage in patients with a peristaltic esophagus. Dig Dis Sci. 1996;41:372–6.
Freidin N, Fisher MJ, Taylor W, et al. Sleep and nocturnal acid reflux in normal subjects and patients with reflux oesophagitis. Gut. 1991;32:1275–9.
Ramu B, Mohan P, Rajasekaran MS, Jayanthi V. Prevalence and risk factors for gastroesophageal reflux in pregnancy. Indian J Gastroenterol. 2011;30:144–7.
Gaddam S, Maddur H, Wani S, et al. Risk factors for nocturnal reflux in a large GERD cohort. J Clin Gastroenterol. 2011;45:764–8.
Ghoshal UC, Chourasia D, Tripathi S, Misra A, Singh K. Relationship of severity of gastroesophageal reflux disease with gastric acid secretory profile and esophageal acid exposure during nocturnal acid breakthrough: a study using 24-h dual-channel pH-metry. Scand J Gastroenterol. 2008;43:654–61.
Katz PO, Gerson LB, Vela MF. Guidelines for the diagnosis and management of gastroesophageal reflux disease. Am J Gastroenterol. 2013;108:308–28.
Niu XP, Yu BP, Wang YD, et al. Risk factors for proton pump inhibitor refractoriness in Chinese patients with non-erosive reflux disease. World J Gastroenterol. 2013;19:3124–9.
Lee ES, Kim N, Lee SH, et al. Comparison of risk factors and clinical responses to proton pump inhibitors in patients with erosive oesophagitis and non-erosive reflux disease. Aliment Pharmacol Ther. 2009;30:154–64.
Bytzer P, van Zanten SV, Mattsson H, et al. Partial symptom-response to proton pump inhibitors in patients with non-erosive reflux disease or reflux oesophagitis—a post hoc analysis of 5796 patients. Aliment Pharmacol Ther. 2012;36:635–43.
Amarasiri DL, Pathmeswaran A, de Silva HJ, Ranasinha CD. Response of the airways and autonomic nervous system to acid perfusion of the esophagus in patients with asthma: a laboratory study. BMC Pulm Med. 2013;13:33.
Stein MR. Possible mechanisms of influence of esophageal acid on airway hyperresponsiveness. Am J Med. 2003;115 Suppl 3A:55S–9S.
Schan CA, Harding SM, Haile JM, Bradley LA, Richter JE. Gastroesophageal reflux-induced bronchoconstriction. An intraesophageal acid infusion study using state-of-the-art technology. Chest. 1994;106:731–7.
Ates F, Vaezi MF. Insight into the relationship between gastroesophageal reflux disease and asthma. Gastroenterol Hepatol. 2014;10:729–36.
Sandur V, Murugesh M, Banait V, et al. Prevalence of gastro-esophageal reflux disease in patients with difficult to control asthma and effect of proton pump inhibitor therapy on asthma symptoms, reflux symptoms, pulmonary function and requirement for asthma medications. J Postgrad Med. 2014;60:282–6.
Charles S, Johnson P, Padmavathi R, Rajagopalan, Subhashini AS, Kumar AP. The prevalence of the gastro oesophageal reflux disease in asthmatics. J Clin Diagn Res. 2011;5:711–3.
Rameschandra S, Acharya V, Kunal VT, Ramkrishna A, Acharya P. Prevalence and spectrum of gastro esophageal reflux disease in bronchial asthma. J Clin Diagn Res. 2015;9:OC11–4.
Smith J, Woodcock A, Houghton L. New developments in reflux-associated cough. Lung. 2010;188 Suppl 1:S81–6.
Woodcock A, Young EC, Smith JA. New insights in cough. Br Med Bull. 2010;96:61–73.
Smith J, Decalmer S, Kelsall A, et al. Acoustic cough-reflux associations in chronic cough: potential triggers and mechanisms. Gastroenterology. 2010;139:754–62.
Pore R, Biswas S, Das S. Prevailing practices for the management of dry cough in India: a questionnaire based survey. J Assoc Physicians India. 2016;64:48–54.
Kahrilas PJ, Smith JA, Dicpinigaitis PV. A causal relationship between cough and gastroesophageal reflux disease (GERD) has been established: a pro/con debate. Lung. 2014;192:39–46.
Ford CN. Evaluation and management of laryngopharyngeal reflux. JAMA. 2005;294:1534–40.
Maldhure S, Chandrasekharan R, Dutta AK, Chacko A, Kurien M. Role of pH monitoring in laryngopharyngeal reflux patients with voice disorders. Iran J Otorhinolaryngol. 2016;28:377–83.
Belafsky PC, Postma GN, Koufman JA. The validity and reliability of the reflux finding score (RFS). Laryngoscope. 2001;111:1313–7.
Hicks DM, Ours TM, Abelson TI, Vaezi MF, Richter JE. The prevalence of hypopharynx findings associated with gastroesophageal reflux in normal volunteers. J Voice. 2002;16:564–79.
Campagnolo AM, Priston J, Thoen RH, Medeiros T, Assunção AR. Laryngopharyngeal reflux: diagnosis, treatment, and latest research. Int Arch Otorhinolaryngol. 2014;18:184–91.
Fass R, Achem SR. Noncardiac chest pain: epidemiology, natural course and pathogenesis. J Neurogastroenterol Motil. 2011;17:110–23.
Stahl WG, Beton RR, Johnson CS, Brown CL, Waring JP. Diagnosis and treatment of patients with gastroesophageal reflux and non cardiac chest pain. South Med J. 1994;87:739–42.
Jain M. Evaluation of noncardiac chest pain in Indian setting—can we reduce the investigation burden? Indian J Gastroenterol. 2015;34:266–7.
Kaltenbach T, Crockett S, Gerson LB. Are lifestyle measures effective in patients with gastroesophageal reflux disease? An evidence-based approach. Arch Intern Med. 2006;166:965–71.
Fan W, Hou Y, Sun X, et al. Effects of high-fat, standard, and functional food meals on esophageal and gastric pH in patients with gastroesophageal reflux disease and healthy subjects. J Dig Dis. 2018;19:664–73.
Wu KL, Kuo CM, Yao CC, et al. The effect of dietary carbohydrate on gastroesophageal reflux disease. J Formos Med Assoc. 2018;117:973–8.
Shapiro M, Green C, Bautista JM, et al. Assessment of dietary nutrients that influence perception of intra-oesophageal acid reflux events in patients with gastro-oesophageal reflux disease. Aliment Pharmacol Ther. 2007;25:93–101.
Dent J, Vakil N, Jones R, et al. Accuracy of the diagnosis of GORD by questionnaire, physicians and a trial of proton pump inhibitor treatment: the Diamond Study. Gut. 2010;59:714–21.
Hunt R, Armstrong D, Katelaris P, et al. World Gastroenterology Organisation global guidelines: GERD global perspective on gastroesophageal reflux disease. J Clin Gastroenterol. 2017;51:467–78.
Gasiorowska A, Fass R. The proton pump inhibitor (PPI) test in GERD: does it still have a role? J Clin Gastroenterol. 2008;42:867–74.
Lundell LR, Dent J, Bennett JR, et al. Endoscopic assessment of oesophagitis: clinical and functional correlates and further validation of the Los Angeles classification. Gut. 1999;45:172–80.
Dent J. Endoscopic grading of reflux oesophagitis: the past, present and future. Best Pract Res Clin Gastroenterol. 2008;22:585–99.
Rosaida MS, Goh KL. Gastro-oesophageal reflux disease, reflux oesophagitis and non-erosive reflux disease in a multiracial Asian population: a prospective, endoscopy based study. Eur J Gastroenterol Hepatol. 2004;16:495–501.
Dutta AK, Chacko A, Balekuduru A, Sahu MK, Gangadharan SK. High prevalence of significant endoscopic findings in patients with uninvestigated typical reflux symptoms. Am J Gastroenterol. 2011;106:1172–3.
Savarino E, Gemignani L, Pohl D, Zentilin P, Dulbecco P, Assandri L. Oesophageal motility and bolus transit abnormalities increase in parallel with the severity of gastro-oesophageal reflux disease. Aliment Pharmacol Ther. 2011;34:476–86.
Kahrilas PJ, McColl K, Fox M, et al. The acid pocket: a target for treatment in reflux disease? Am J Gastroenterol. 2013;108:1058–64.
Vaezi MF, Sifrim D. Assessing old and new diagnostic tests for gastroesophageal reflux disease. Gastroenterology. 2018;154:289–301.
Dhawan PS, Alvares JF, Vora IM, et al. Prevalence of short segments of specialized columnar epithelium in distal esophagus: association with gastroesophageal reflux. Indian J Gastroenterol. 2001;20:144–7.
Mathew P, Joshi AS, Shukla A, Bhatia SJ. Risk factors for Barrett's esophagus in Indian patients with gastroesophageal reflux disease. J Gastroenterol Hepatol. 2011;26:1151-6.
Kao SS, Chen WC, Hsu PI, et al. The frequencies of gastroesophageal and extragastroesophageal symptoms in patients with mild erosive esophagitis, severe erosive esophagitis, and Barrett’s esophagus in Taiwan. Gastroenterol Res Pract. 2013;2013:480325.
Johnsson F, Joelsson B, Gudmundsson K, Greiff L. Symptoms and endoscopic findings in the diagnosis of gastroesophageal reflux disease. Scand J Gastroenterol. 1987;22:714–8.
Gyawali CP, Kahrilas PJ, Savarino E, et al. Modern diagnosis of GERD: the Lyon consensus. Gut. 2018;67:1351–62.
Roman S, Gyawali CP, Savarino E, et al. GERD consensus group. Ambulatory reflux monitoring for diagnosis of gastro-esophageal reflux disease: update of the Porto consensus and recommendations from an international consensus group. Neurogastroenterol Motil. 2017;29:1–15.
Madan K, Ahuja V, Gupta SD, Bal C, Kapoor A, Sharma MP. Impact of 24-h esophageal pH monitoring on the diagnosis of gastroesophageal reflux disease: defining the gold standard. J Gastroenterol Hepatol. 2005;20:30–7.
Prakash C, Clouse RE. Value of extended recording time with wireless pH monitoring in evaluating gastroesophageal reflux disease. Clin Gastroenterol Hepatol. 2005;3:329–34.
Wong WM, Bautista J, Dekel R, et al. Feasibility and tolerability of transnasal/per-oral placement of the wireless pH capsule vs. traditional 24-h oesophageal pH monitoring—a randomized trial. Aliment Pharmacol Ther. 2005;21:155–63.
Karyampudi A, Ghoshal UC, Singh R, Verma A, Misra A, Saraswat VA. Esophageal acidification during nocturnal acid-breakthrough with ilaprazole versus omeprazole in gastroesophageal reflux disease. J Neurogastroenterol Motil. 2017;23:208–17.
Weigt J, Kandulski A, Büsch F, Malfertheiner P. Nocturnal gastric acid breakthrough is not associated with night-time gastroesophageal reflux in GERD patients. Dig Dis. 2009;27:68–73.
Jain M, Srinivas M, Bawane P, Venkataraman J. Basal lower esophageal sphincter pressure in gastroesophageal reflux disease: an ignored metric in high-resolution esophageal manometry. Indian J Gastroenterol. 2018;37:446–51.
Patti MG, Diener U, Tamburini A, Molena D, Way LW. Role of esophageal function tests in diagnosis of gastroesophageal reflux disease. Dig Dis Sci. 2001;46:597–602.
Spechler SJ, Souza RF, Rosenberg SJ, Ruben RA, Goyal RK. Heartburn in patients with achalasia. Gut. 1995;37:305–8.
Chourasia D, Misra A, Tripathi S, Krishnani N, Ghoshal UC. Patients with Helicobacter pylori infection have less severe gastroesophageal reflux disease: a study using endoscopy, 24-hour gastric and esophageal pH metry. Indian J Gastroenterol. 2011;30:12–21.
Pandit BB, Lahoti M, Amarapurkar AD, Kamath R, Naik AS, Bhatia SJ. Relationship between Helicobacter pylori and gastro-esophageal reflux disease. Indian J Gastroenterol. 2003;22 Suppl 1:A11.
Saleh CM, Smout AJ, Bredenoord AJ. The diagnosis of gastro-esophageal reflux disease cannot be made with barium esophagograms. Neurogastroenterol Motil. 2015;27:195–200.
Rey JW, Deris N, Marquardt JU, et al. High-definition endoscopy with iScan and Lugol's solution for the detection of inflammation in patients with nonerosive reflux disease: histologic evaluation in comparison with a control group. Dis Esophagus. 2016;29:185-91.
Miyasaka M, Hirakawa M, Nakamura K, et al. The endoscopic diagnosis of nonerosive reflux disease using flexible spectral imaging color enhancement image: a feasibility trial. Dis Esophagus. 2011;24:395-400.
Fock KM, Teo EK, Ang TL, et al. The utility of narrow band imaging in improving the endoscopic diagnosis of gastroesophageal reflux disease. Clin Gastroenterol Hepatol. 2009;7:54–9.
Sharma P, Wani S, Bansal A, et al. A feasibility trial of narrow band imaging endoscopy in patients with gastroesophageal reflux disease. Gastroenterology. 2007;133:454–64.
Chu CL, Zhen YB, Lv GP, et al. Microalterations of esophagus in patients with non-erosive reflux disease: in-vivo diagnosis by confocal laser endomicroscopy and its relationship with gastroesophageal reflux. Am J Gastroenterol. 2012;107:864–74.
Smeets FG, Keszthelyi D, Bouvy ND, Masclee AA, Conchillo JM. Does measurement of esophagogastric junction distensibility by EndoFLIP predict therapy-responsiveness to endoluminal fundoplication in patients with gastroesophageal reflux disease? J Neurogastroenterol Motil. 2015;21:255–64.
Chen JW, Rubenstein JH. Esophagogastric junction distensibility assessed using the functional lumen imaging probe. World J Gastroenterol. 2017;23:1289–97.
Price SF, Smithson KW, Castell DO. Food sensitivity in reflux esophagitis. Gastroenterology. 1978;75:240–3.
Boekema PJ, Samsom M, Smout AJ. Effect of coffee on gastro-oesophageal reflux in patients with reflux disease and healthy controls. Eur J Gastroenterol Hepatol. 1999;11:1271–6.
Wang J-H, Luo J-Y, Dong L, Gong J, Tong M. Epidemiology of gastroesophageal reflux disease: a general population-based study in Xi’an of northwest China. World J Gastroenterol. 2004;10:1647–51.
Stanghellini V. Relationship between upper gastrointestinal symptoms and lifestyle, psychosocial factors and comorbidity in the general population: results from the Domestic/International Gastroenterology Surveillance Study (DIGEST). Scand J Gastroenterol Suppl. 1999;231:29–37.
Cohen S, Booth GH. Gastric acid secretion and lower-esophageal-sphincter pressure in response to coffee and caffeine. N Engl J Med. 1975;293:897–9.
Kahrilas PJ, Gupta RR. The effect of cigarette smoking on salivation and esophageal acid clearance. J Lab Clin Med. 1989;114:431–8.
Watanabe Y, Fujiwara Y, Shiba M, et al. Cigarette smoking and alcohol consumption associated with gastro-oesophageal reflux disease in Japanese men. Scand J Gastroenterol. 2003;38:807–11.
Nilsson M, Johnsen R, Ye W, Hveem K, Lagergren J. Lifestyle related risk factors in the aetiology of gastro-oesophageal reflux. Gut. 2004;53:1730–5.
Schindlbeck NE, Heinrich C, Dendorfer A, Pace F, Müller-Lissner SA. Influence of smoking and esophageal intubation on esophageal pH-metry. Gastroenterology. 1987;92:1994–7.
Waring JP, Eastwood TF, Austin JM, Sanowski RA. The immediate effects of cessation of cigarette smoking on gastroesophageal reflux. Am J Gastroenterol. 1989;84:1076–8.
Kadakia SC, Kikendall JW, Maydonovitch C, Johnson LF. Effect of cigarette smoking on gastroesophageal reflux measured by 24-h ambulatory esophageal pH monitoring. Am J Gastroenterol. 1995;90:1785–90.
Ness-Jensen E, Lindam A, Lagergren J, Hveem K. Tobacco smoking cessation and improved gastroesophageal reflux: a prospective population-based cohort study: the HUNT study. Am J Gastroenterol. 2014;109:171–7.
Bujanda L. The effects of alcohol consumption upon the gastrointestinal tract. Am J Gastroenterol. 2000;95:3374–82.
Kaufman SE, Kaye MD. Induction of gastro-oesophageal reflux by alcohol. Gut. 1978;19:336–8.
Ness-Jensen E, Hveem K, El-Serag H, Lagergren J. Lifestyle intervention in gastroesophageal reflux disease. Clin Gastroenterol Hepatol. 2016;14:175–82.
Jacobson BC, Somers SC, Fuchs CS, Kelly CP, Camargo CA. Body-mass index and symptoms of gastroesophageal reflux in women. N Engl J Med. 2006;354:2340–8.
Ness-Jensen E, Lindam A, Lagergren J, Hveem K. Weight loss and reduction in gastroesophageal reflux. A prospective population-based cohort study: the HUNT study. Am J Gastroenterol. 2013;108:376–82.
Austin GL, Thiny MT, Westman EC, Yancy WS, Shaheen NJ. A very low-carbohydrate diet improves gastroesophageal reflux and its symptoms. Dig Dis Sci. 2006;51:1307–12.
Fraser-Moodie CA, Norton B, Gornall C, Magnago S, Weale AR, Holmes GK. Weight loss has an independent beneficial effect on symptoms of gastro-oesophageal reflux in patients who are overweight. Scand J Gastroenterol. 1999;34:337–40.
Mathus-Vliegen EM, Tygat GN. Gastro-oesophageal reflux in obese subjects: influence of overweight, weight loss and chronic gastric balloon distension. Scand J Gastroenterol. 2002;37:1246–52.
Mathus-Vliegen LM, Tytgat GN. Twenty-four-hour pH measurements in morbid obesity: effects of massive overweight, weight loss and gastric distension. Eur J Gastroenterol Hepatol. 1996;8:635–40.
Mathus-Vliegen EM, van Weeren M, van Eerten PV. Los function and obesity: the impact of untreated obesity, weight loss, and chronic gastric balloon distension. Digestion. 2003;68:161–8.
Singh M, Lee J, Gupta N, et al. Weight loss can lead to resolution of gastroesophageal reflux disease symptoms: a prospective intervention trial. Obesity (Silver Spring). 2013;21:284–90.
Sharma A, Aggarwal S, Ahuja V, Bal C. Evaluation of gastroesophageal reflux before and after sleeve gastrectomy using symptom scoring, scintigraphy, and endoscopy. Surg Obes Relat Dis. 2014;10:600–5.
Stanciu C, Bennett JR. Effects of posture on gastro-oesophageal reflux. Digestion. 1977;15:104–9.
Piesman M, Hwang I, Maydonovitch C, Wong RK. Nocturnal reflux episodes following the administration of a standardized meal. Does timing matter? Am J Gastroenterol. 2007;102:2128–34.
Lanzon-Miller S, Pounder RE, McIsaac RL, Wood JR. The timing of the evening meal affects the pattern of 24-hour intragastric acidity. Aliment Pharmacol Ther. 1990;4:547–53.
Duroux P, Bauerfeind P, Emde C, Koelz HR, Blum AL. Early dinner reduces nocturnal gastric acidity. Gut. 1989;30:1063–7.
Orr WC, Harnish MJ. Sleep-related gastro-oesophageal reflux: provocation with a late evening meal and treatment with acid suppression. Aliment Pharmacol Ther. 1998;12:1033–8.
Tran T, Lowry AM, El-Serag HB. Meta-analysis: the efficacy of over-the-counter gastro-oesophageal reflux disease therapies. Aliment Pharmacol Ther. 2007;25:143–53.
Surdea-Blaga T, Băncilă I, Dobru D, et al. Mucosal protective compounds in the treatment of gastroesophageal reflux disease. A position paper based on evidence of the Romanian Society of Neurogastroenterology. J Gastrointestin Liver Dis. 2016;25:537–46.
Savarino E, Zentilin P, Marabotto E, et al. A review of pharmacotherapy for treating gastroesophageal reflux disease (GERD). Expert Opin Pharmacother. 2017;18:1333–43.
Simon B, Ravelli GP, Goffin H. Sucralfate gel versus placebo in patients with non-erosive gastro-oesophageal reflux disease. Aliment Pharmacol Ther. 1996;10:441–6.
Wolfe MM, Sachs G. Acid suppression: optimizing therapy for gastroduodenal ulcer healing, gastroesophageal reflux disease, and stress-related erosive syndrome. Gastroenterology. 2000;118 2 Suppl 1:S9–31.
Sigterman KE, van Pinxteren B, Bonis PA, Lau J, Numans ME. Short-term treatment with proton pump inhibitors, H2-receptor antagonists and prokinetics for gastro-oesophageal reflux disease-like symptoms and endoscopy negative reflux disease. Cochrane Database Syst Rev. 2013;5:CD002095.
Gyawali CP, Fass R. Management of gastroesophageal reflux disease. Gastroenterology. 2018;154:302–18.
Kahrilas PJ, Howden CW, Hughes N. Response of regurgitation to proton pump inhibitor therapy in clinical trials of gastroesophageal reflux disease. Am J Gastroenterol. 2011;106:1419–25.
Numans ME, Lau J, de Wit NJ, Bonis PA. Short-term treatment with proton-pump inhibitors as a test for gastroesophageal reflux disease: a meta-analysis of diagnostic test characteristics. Ann Intern Med. 2004;140:518–27.
Weijenborg PW, Cremonini F, Smout AJ, Bredenoord AJ. PPI therapy is equally effective in well-defined non-erosive reflux disease and in reflux esophagitis: a meta-analysis. Neurogastroenterol Motil. 2012;24:747–57.
Bhatia S, Shukla A, Johnson D. An expert review and recommendations on the rational use of proton pump inhibitors: Indian perspective. J Assoc Physicians India. 2019;67:88-96.
Zhang J-X, Ji M-Y, Song J, et al. Proton pump inhibitor for non-erosive reflux disease: a meta-analysis. World J Gastroenterol. 2013;19:8408–19.
Zhang H, Yang Z, Ni Z, Shi Y. A meta-analysis and systematic review of the efficacy of twice daily PPIs versus once daily for treatment of gastroesophageal reflux disease. Gastroenterol Res Pract. 2017;2017:9865963.
Chiba N, De Gara CJ, Wilkinson JM, Hunt RH. Speed of healing and symptom relief in grade II to IV gastroesophageal reflux disease: a meta-analysis. Gastroenterology. 1997;112:1798–810.
McDonagh MS, Carson S, Thakurta S. Drug class review: proton pump inhibitors: final report update 5 [internet]. Portland (OR): Oregon Health & Science University; 2009. (Drug Class Reviews). Available from: http://www.ncbi.nlm.nih.gov/books/NBK47260/
Delchier JC, Cohen G, Humphries TJ. Rabeprazole, 20 mg once daily or 10 mg twice daily, is equivalent to omeprazole, 20 mg once daily, in the healing of erosive gastrooesophageal reflux disease. Scand J Gastroenterol. 2000;35:1245–50.
Kinoshita Y, Hongo M, Japan TWICE Study Group. Efficacy of twice-daily rabeprazole for reflux esophagitis patients refractory to standard once-daily administration of PPI: the Japan-based TWICE study. Am J Gastroenterol. 2012;107:522–30.
Schindlbeck NE, Klauser AG, Berghammer G, Londong W, Müller-Lissner SA. Three year follow up of patients with gastrooesophageal reflux disease. Gut. 1992;33:1016–9.
Inadomi JM, Jamal R, Murata GH, et al. Step-down management of gastroesophageal reflux disease. Gastroenterology. 2001;121:1095–100.
Lind T, Havelund T, Lundell L, et al. On demand therapy with omeprazole for the long-term management of patients with heartburn without oesophagitis—a placebo-controlled randomized trial. Aliment Pharmacol Ther. 1999;13:907–14.
Zacny J, Zamakhshary M, Sketris I, Veldhuyzen van Zanten S. Systematic review: The efficacy of intermittent and on-demand therapy with histamine H2-receptor antagonists or proton pump inhibitors for gastro-oesophageal reflux disease patients. Aliment Pharmacol Ther. 2005;21:1299–312.
Pace F, Tonini M, Pallotta S, Molteni P, Porro GB. Systematic review: Maintenance treatment of gastro-oesophageal reflux disease with proton pump inhibitors taken “on-demand.”. Aliment Pharmacol Ther. 2007;26:195–204.
Donnellan C, Sharma N, Preston C, Moayyedi P. Medical treatments for the maintenance therapy of reflux oesophagitis and endoscopic negative reflux disease. Cochrane Database Syst Rev. 2005 Apr 18;2:CD003245.
Inadomi JM, McIntyre L, Bernard L, Fendrick AM. Step-down from multiple- to single-dose proton pump inhibitors (PPIs): a prospective study of patients with heartburn or acid regurgitation completely relieved with PPIs. Am J Gastroenterol. 2003;98:1940–4.
Vigneri S, Termini R, Leandro G, et al. A comparison of five maintenance therapies for reflux esophagitis. N Engl J Med. 1995;333:1106–10.
Gough AL, Long RG, Cooper BT, Fosters CS, Garrett AD, Langworthy CH. Lansoprazole versus ranitidine in the maintenance treatment of reflux oesophagitis. Aliment Pharmacol Ther. 1996;10:529–39.
Mine S, Iida T, Tabata T, Kishikawa H, Tanaka Y. Management of symptoms in step-down therapy of gastroesophageal reflux disease. J Gastroenterol Hepatol. 2005;20:1365–70.
Boghossian TA, Rashid FJ, Thompson W, et al. Deprescribing versus continuation of chronic proton pump inhibitor use in adults. Cochrane Database Syst Rev. 2017;3:CD011969.
Jaspersen D, Schwacha H, Schorr W, Brennenstuhl M, Raschka C, Hammar CH. Omeprazole in the treatment of patients with complicated gastro-oesophageal reflux disease. J Gastroenterol Hepatol. 1996;11:900–2.
Swarbrick ET, Gough AL, Foster CS, Christian J, Garrett AD, Langworthy CH. Prevention of recurrence of oesophageal stricture, a comparison of lansoprazole and high-dose ranitidine. Eur J Gastroenterol Hepatol. 1996;8:431–8.
Smith PM, Kerr GD, Cockel R, et al. A comparison of omeprazole and ranitidine in the prevention of recurrence of benign esophageal stricture. Restore Invest Group. Gastroenterology. 1994;107:1312–8.
Kuo B, Castell DO. Optimal dosing of omeprazole 40 mg daily: effects on gastric and esophageal pH and serum gastrin in healthy controls. Am J Gastroenterol. 1996;91:1532–8.
Xue S, Katz PO, Banerjee P, Tutuian R, Castell DO. Bedtime H2 blockers improve nocturnal gastric acid control in GERD patients on proton pump inhibitors. Aliment Pharmacol Ther. 2001;15:1351–6.
Peghini PL, Katz PO, Bracy NA, Castell DO. Nocturnal recovery of gastric acid secretion with twice-daily dosing of proton pump inhibitors. Am J Gastroenterol. 1998;93:763–7.
Peghini PL, Katz PO, Castell DO. Ranitidine controls nocturnal gastric acid breakthrough on omeprazole: a controlled study in normal subjects. Gastroenterology. 1998;115:1335–9.
Mainie I, Tutuian R, Castell DO. Addition of a H2 receptor antagonist to PPI improves acid control and decreases nocturnal acid breakthrough. J Clin Gastroenterol. 2008;42:676–9.
Fackler WK, Ours TM, Vaezi MF, Richter JE. Long-term effect of H2RA therapy on nocturnal gastric acid breakthrough. Gastroenterology. 2002;122:625–32.
Ours TM, Fackler WK, Richter JE, Vaezi MF. Nocturnal acid breakthrough: clinical significance and correlation with esophageal acid exposure. Am J Gastroenterol. 2003;98:545–50.
Dean BB, Gano AD, Knight K, Ofman JJ, Fass R. Effectiveness of proton pump inhibitors in nonerosive reflux disease. Clin Gastroenterol Hepatol. 2004;2:656–64.
Gunaratnam NT, Jessup TP, Inadomi J, Lascewski DP. Sub-optimal proton pump inhibitor dosing is prevalent in patients with poorly controlled gastro-oesophageal reflux disease. Aliment Pharmacol Ther. 2006;23:1473–7.
Fass R, Sontag SJ, Traxler B, Sostek M. Treatment of patients with persistent heartburn symptoms: a double-blind, randomized trial. Clin Gastroenterol Hepatol. 2006;4:50–6.
Khan M, Santana J, Donnellan C, Preston C, Moayyedi P. Medical treatments in the short term management of reflux oesophagitis. Cochrane Database Syst Rev. 2007;(2):CD003244.
Madan K, Ahuja V, Kashyap PC, Sharma MP. Comparison of efficacy of pantoprazole alone versus pantoprazole plus mosapride in therapy of gastroesophageal reflux disease: a randomized trial. Dis Esophagus. 2004;17:274–8.
Ren L-H, Chen W-X, Qian L-J, Li S, Gu M, Shi R-H. Addition of prokinetics to PPI therapy in gastroesophageal reflux disease: a meta-analysis. World J Gastroenterol. 2014;20:2412–9.
Kessing BF, Smout AJ, Bennink RJ, Kraaijpoel N, Oors JM, Bredenoord AJ. Prucalopride decreases esophageal acid exposure and accelerates gastric emptying in healthy subjects. Neurogastroenterol Motil. 2014;26:1079–86.
Futagami S, Iwakiri K, Shindo T, et al. The prokinetic effect of mosapride citrate combined with omeprazole therapy improves clinical symptoms and gastric emptying in PPI-resistant NERD patients with delayed gastric emptying. J Gastroenterol. 2010;45:413–21.
Kamiya T, Adachi H, Hirako M, et al. Impaired gastric motility and its relationship to reflux symptoms in patients with nonerosive gastroesophageal reflux disease. J Gastroenterol. 2009;44:183–9.
Giudicessi JR, Ackerman MJ, Camilleri M. Cardiovascular safety of prokinetic agents: a focus on drug-induced arrhythmias. Neurogastroenterol Motil. 2018;30:e13302.
Li S, Shi S, Chen F, Lin J. The effects of baclofen for the treatment of gastroesophageal reflux disease: a meta-analysis of randomized controlled trials. Gastroenterol Res Pract. 2014;2014:307805.
Kahrilas PJ, Boeckxstaens G, Smout AJ. Management of the patient with incomplete response to PPI therapy. Best Pract Res Clin Gastroenterol. 2013;27:401–14.
Vashani K, Murugesh M, Hattiangadi G, et al. Effectiveness of voice therapy in reflux-related voice disorders. Dis Esophagus. 2010;23:27-32.
Gopal B, Singhal P, Gaur SN. Gastroesophageal reflux disease in bronchial asthma and the response to omeprazole. Asian Pac J Allergy Immunol. 2005;23:29–34.
Kahrilas PJ, Hughes N, Howden CW. Response of unexplained chest pain to proton pump inhibitor treatment in patients with and without objective evidence of gastro-oesophageal reflux disease. Gut. 2011;60:1473–8.
Irwin RS, Zawacki JK, Wilson MM, French CT, Callery MP. Chronic cough due to gastroesophageal reflux disease: failure to resolve despite total/near-total elimination of esophageal acid. Chest. 2002;121:1132–40.
Chang AB, Lasserson TJ, Gaffney J, Connor FL, Garske LA. Gastro-oesophageal reflux treatment for prolonged non-specific cough in children and adults. Cochrane Database Syst Rev. 2011;1:CD004823.
Gopal B, Singhal P, Gaur SN. Gastroesophageal reflux disease in bronchial asthma and the response to omeprazole. Asian Pac J Allergy Immunol. 2005;23:29–34.
Harding SM, Richter JE, Guzzo MR, Schan CA, Alexander RW, Bradley LA. Asthma and gastroesophageal reflux: acid suppressive therapy improves asthma outcome. Am J Med. 1996;100:395–405.
Kiljander TO, Salomaa ER, Hietanen EK, Terho EO. Gastroesophageal reflux in asthmatics: a double-blind, placebo-controlled crossover study with omeprazole. Chest. 1999;116:1257–64.
Meier JH, McNally PR, Punja M, et al. Does omeprazole (Prilosec) improve respiratory function in asthmatics with gastroesophageal reflux? A double-blind, placebo-controlled crossover study. Dig Dis Sci. 1994;39:2127–33.
American Lung Association Asthma Clinical Research Centers, Mastronarde JG, Anthonisen NR, et al. Efficacy of esomeprazole for treatment of poorly controlled asthma. N Engl J Med. 2009;360:1487–99.
Littner MR, Leung FW, Ballard ED, Huang B, Samra NK, Lansoprazole Asthma Study Group. Effects of 24 weeks of lansoprazole therapy on asthma symptoms, exacerbations, quality of life, and pulmonary function in adult asthmatic patients with acid reflux symptoms. Chest. 2005;128:1128–35.
Gralnek IM, Dulai GS, Fennerty MB, Spiegel BM. Esomeprazole versus other proton pump inhibitors in erosive esophagitis: a meta-analysis of randomized clinical trials. Clin Gastroenterol Hepatol. 2006;4:1452–8.
Chen L, Chen Y, Li B. The efficacy and safety of proton-pump inhibitors in treating patients with non-erosive reflux disease: a network meta-analysis. Sci Rep. 2016;6:321–26.
derp-ppi.pdf [Internet]. [cited 2019 Jan 23]. Available from: https://www2.gov.bc.ca/assets/gov/health/health-drug-coverage/pharmacare/derp-ppi.pdf
Spechler SJ, Sharma P, Souza RF, et al. American Gastroenterological Association technical review on the management of Barrett’s esophagus. Gastroenterology. 2011;140:e18–52.
Johnson DA, Katz PO, Armstrong D, et al. The safety of appropriate use of over-the-counter proton pump inhibitors: an evidence-based review and Delphi consensus. Drugs. 2017;77:547–61.
Scarpignato C, Gatta L, Zullo A, Blandizzi C, SIF-AIGO-FIMMG Group, Italian Society of Pharmacology, et al. Effective and safe proton pump inhibitor therapy in acid-related diseases—a position paper addressing benefits and potential harms of acid suppression. BMC Med. 2016;14:179.
Kia L, Kahrilas PJ. Therapy: risks associated with chronic PPI use—signal or noise? Nat Rev Gastroenterol Hepatol. 2016;13:253–4.
Moayyedi P, Eikelboom J, Bosch J, Dyal L, Connolly S, Yusuf S. Adverse events related to proton pump inhibitor therapy. Results of a randomized trial of pantoprazole versus placebo with 53,152 patient years of follow-up. Gastroenterology. 2019;156:S173–4.
Sharma P, Dent J, Armstrong D, et al. The development and validation of an endoscopic grading system for Barrett’s esophagus: the Prague C & M criteria. Gastroenterology. 2006;131:1392–9.
Spechler SJ, Sharma P, Souza RF, et al. American Gastroenterological Association technical review on the management of Barrett’s esophagus. Gastroenterology. 2011;140:e18–52.
Wang KK, Sampliner RE, Practice Parameters Committee of the American College of Gastroenterology. Updated guidelines 2008 for the diagnosis, surveillance and therapy of Barrett’s esophagus. Am J Gastroenterol. 2008;103:788–97.
Fitzgerald RC, di Pietro M, Ragunath K, et al. British Society of Gastroenterology guidelines on the diagnosis and management of Barrett’s oesophagus. Gut. 2014;63:7–42.
Lee YC, Cook MB, Bhatia S, et al. Interobserver reliability in the endoscopic diagnosis and grading of Barrett’s esophagus: an Asian multi-national study. Endoscopy. 2010;42:699–704.
Ishimura N, Amano Y, Sollano JD, et al. Questionnaire-based survey conducted in 2011 concerning endoscopic management of Barrett’s esophagus in East Asian countries. Digestion. 2012;86:136–46.
Aida J, Vieth M, Ell C, et al. Palisade vessels as a new histologic marker of esophageal origin in ER specimens from columnar-lined esophagus. Am J Surg Pathol. 2011;35:1140–5.
Kandiah K, Chedgy FJQ, Subramaniam S, et al. International development and validation of a classification system for the identification of Barrett’s neoplasia using acetic acid chromoendoscopy: the Portsmouth Acetic Acid Classification (PREDICT). Gut. 2018;67:2085–91.
Sharma P, Bergman J, Goda K, et al. Development and validation of a classification system to identify high-grade dysplasia and esophageal adenocarcinoma in Barrett’s esophagus using narrow-band imaging. Gastroenterology. 2016;150:591–8.
Smith RR, Hamilton SR, Boitnott JK, et al. The spectrum of carcinoma arising in Barrett’s esophagus. A clinicopathologic study of 26 patients. Am J Surg Pathol. 1984;8:563–73.
Skinner DB, Walther BC, Riddell RH, et al. Barrett’s esophagus. Comparison of benign and malignant cases. Ann Surg. 1983;198:554–65.
Bhat S, Coleman HG, Yousef F, et al. Risk of malignant progression in Barrett’s esophagus patients: results from a large population-based study. J Natl Cancer Inst. 2011;103:1049–57.
Goda K, Singh R, Oda I, et al. Current status of endoscopic diagnosis and treatment of superficial Barrett’s adenocarcinoma in Asia-Pacific region. Dig Endosc. 2013;25 Suppl 2:146–50.
Fock KM, Talley NJ, Fass R, et al. Asia-Pacific consensus on the management of gastroesophageal reflux disease: update. J Gastroenterol Hepatol. 2008;23:8–22.
Harrison R, Perry I, Haddadin W, et al. Detection of intestinal metaplasia in Barrett’s esophagus: an observational comparator study suggests the need for a minimum of eight biopsies. Am J Gastroenterol. 2007;102:1154–61.
Kelty CJ, Gough MD, Van Wyk Q, et al. Barrett’s oesophagus: intestinal metaplasia is not essential for cancer risk. Scand J Gastroenterol. 2007;42:1271–4.
Gatenby PA, Ramus JR, Caygill CP, et al. Relevance of the detection of intestinal metaplasia in non-dysplastic columnar-lined oesophagus. Scand J Gastroenterol. 2008;43:524–30.
Montgomery E, Bronner MP, Goldblum JR, et al. Reproducibility of the diagnosis of dysplasia in Barrett esophagus: a reaffirmation. Hum Pathol. 2001;32:368–78.
Kerkhof M, van Dekken H, Steyerberg EW, et al. Grading of dysplasia in Barrett’s oesophagus: substantial interobserver variation between general and gastrointestinal pathologists. Histopathology. 2007;50:920–7.
Curvers WL, ten Kate FJ, Krishnadath KK, et al. Low-grade dysplasia in Barrett’s esophagus: overdiagnosed and underestimated. Am J Gastroenterol. 2010;105:1523–30.
Duits LC, Phoa KN, Curvers WL, et al. Barrett’s oesophagus patients with low-grade dysplasia can be accurately risk-stratified after histological review by an expert pathology panel. Gut. 2015;64:700–6.
Alikhan M, Rex D, Khan A, et al. Variable pathologic interpretation of columnar lined esophagus by general pathologists in community practice. Gastrointest Endosc. 1999;50:23–6.
Quante M, Graham TA, Jansen M. Insights into the pathophysiology of esophageal adenocarcinoma. Gastroenterology. 2018;154:406–20.
Epari K, Cade R. Oesophagectomy for tumours and dysplasia of the oesophagus and gastro-oesophageal junction. ANZ J Surg. 2009;79:251–7.
Qiao Y, Hyder A, Bae SJ, et al. Surveillance in patients with Barrett’s esophagus for early detection of esophageal adenocarcinoma: a systematic review and meta-analysis. Clin Transl Gastroenterol. 2015;6:e131.
Cherian JV, Sivaraman R, Muthusamy AK, Jayanthi V. Carcinoma of the esophagus in Tamil Nadu (South India): 16-year trends from a tertiary center. J Gastrointestin Liver Dis. 2007;16:245–9.
Streitz JM Jr, Andrews CW Jr, Ellis FH Jr. Endoscopic surveillance of Barrett’s esophagus. Does it help? J Thorac Cardiovasc Surg. 1993;105:383–7.
Peters JH, Clark GW, Ireland AP, et al. Outcome of adenocarcinoma arising in Barrett’s esophagus in endoscopically surveyed and nonsurveyed patients. J Thorac Cardiovasc Surg. 1994;108:813–21.
van Sandick JW, van Lanschot JJ, Kuiken BW, et al. Impact of endoscopic biopsy surveillance of Barrett’s oesophagus on pathological stage and clinical outcome of Barrett’s carcinoma. Gut. 1998;43:216–22.
Corley DA, Levin TR, Habel LA, et al. Surveillance and survival in Barrett’s adenocarcinomas: a population-based study. Gastroenterology. 2002;122:633–40.
Cooper GS, Yuan Z, Chak A, et al. Association of pre-diagnosis endoscopy with stage and survival in adenocarcinoma of the esophagus and gastric cardia. Cancer. 2002;95:32–8.
Fountoulakis A, Zafirellis KD, Dolan K, et al. Effect of surveillance of Barrett’s oesophagus on the clinical outcome of oesophageal cancer. Br J Surg. 2004;91:997–1003.
Rubenstein JH, Sonnenberg A, Davis J, et al. Effect of a prior endoscopy on outcomes of esophageal adenocarcinoma among United States veterans. Gastrointest Endosc. 2008;68:849–55.
Corley DA, Mehtani K, Quesenberry C, et al. Impact of endoscopic surveillance on mortality from Barrett’s esophagus-associated esophageal adenocarcinomas. Gastroenterology. 2013;145:312–9.
Gordon LG, Mayne GC, Hirst NG, et al. Cost-effectiveness of endoscopic surveillance of non-dysplastic Barrett’s esophagus. Gastrointest Endosc. 2014;79:242–56.
Visrodia K, Iyer PG, Schleck CD, Zinsmeister AR, Katzka DA. Yield of repeat endoscopy in Barrett’s esophagus with no dysplasia and low-grade dysplasia: a population-based study. Dig Dis Sci. 2016;61:158–67.
Rodriguez S, Mattek N, Lieberman D, Fennerty B, Eisen G. Barrett’s esophagus on repeat endoscopy: should we look more than once? Am J Gastroenterol. 2008;103:1892–7.
Hanna S, Rastogi A, Weston AP, et al. Detection of Barrett’s esophagus after endoscopic healing of erosive esophagitis. Am J Gastroenterol. 2006;101:1416–20.
Castell DO, Kahrilas PJ, Richter JE, et al. Esomeprazole (40 mg) compared with lansoprazole (30 mg) in the treatment of erosive esophagitis. Am J Gastroenterol. 2002;97:575–83.
Richter JE, Kahrilas PJ, Sontag SJ, Kovacs TO, Huang B, Pencyla JL. Comparing lansoprazole and omeprazole in onset of heartburn relief: results of a randomized, controlled trial in erosive esophagitis patients. Am J Gastroenterol. 2001;96:3089–98.
Palmer ED. The hiatus herniaesophagitis-esophageal stricture complex: twenty-year prospective study. Am J Med. 1968;44:566–79.
Rejeb BM, Bouche O, Zeitoun P. Study of 47 consecutive patients with peptic esophageal stricture compared with 3880 cases of reflux esophagitis. Dig Dis Sci. 1992;37:733–6.
Marks RD, Richter JE, Rizzo J, et al. Omeprazole versus H2-receptor antagonists in treating patients with peptic stricture and esophagitis. Gastroenterology. 1994;106:907–15.
Fass R, Cahn F, Scotti DJ, Gregory DA. Systematic review and meta-analysis of controlled and prospective cohort efficacy studies of endoscopic radiofrequency for treatment of gastroesophageal reflux disease. Surg Endos. 2017;31:4865–82.
Kalapala R, Shah H, Nabi Z, Darisetty S, Talukdar R, Nageshwar Reddy D. Treatment of gastroesophageal reflux disease using radiofrequency ablation (Stretta procedure): an interim analysis of a randomized trial. Indian J Gastroenterol. 2017;36:337–42.
Koch OO, Kaindlstorfer A, Antoniou SA, Spaun G, Pointner R, Swanstrom LL. Subjective and objective data on esophageal manometry and impedance pH monitoring 1 year after endoscopic full-thickness plication for the treatment of GERD by using multiple plication implants. Gastrointest Endosc. 2013;77:7–14.
Zaninotto G, Attwood SE. Surgical management of refractory gastro-oesophageal reflux. Br J Surg. 2010;97:139–40.
Jiang Y, Cui W-X, Wang Y, et al. Antireflux surgery vs medical treatment for gastroesophageal reflux disease: a meta-analysis. World J Meta-Anal. 2015;3:284–94.
The SAGES Guidelines Committee, Stefanidis D, Hope WW, Kohn GP, Reardon PR, Richardson WS, et al. Guidelines for surgical treatment of gastroesophageal reflux disease. Surg Endosc. 2010;24:2647–69.
Peters MJ, Mukhtar A, Yunus RM, et al. Meta-analysis of randomized clinical trials comparing open and laparoscopic anti-reflux surgery. Am J Gastroenterol. 2009;104:1548–61.
Singhal V, Khaitan L. Preoperative evaluation of gastroesophageal reflux disease. Surg Clin North Am. 2015;95:615–27.
Nagpal AP, Soni H, Haribhakti S. Is oesophageal manometry a must before laparoscopic fundoplication? Analysis of 46 consecutive patients treated without preoperative manometry. J Minim Access Surg. 2010;6:66–9.
Nagpal AP, Soni H, Haribhakti SP. Retrospective evaluation of patients of gastroesophageal reflux disease treated with laparoscopic Nissen’s fundoplication. J Minim Access Surg. 2010;6:42–5.
Herregods TV, Troelstra M, Weijenborg PW, et al. Patients with refractory reflux symptoms often do not have GERD. Neurogastroenterol Motil. 2015;27:1267–73.
Khajanchee YS, Dunst CM, Swanstrom LL. Outcomes of Nissen fundoplication in patients with gastroesophageal reflux disease and delayed gastric emptying. Arch Surg. 2009;144:823–8.
Noar MD, Noar E. Gastroparesis associated with gastroesophageal reflux disease and corresponding reflux symptoms may be corrected by radiofrequency ablation of the cardia and esophagogastric junction. Surg Endosc. 2008;22:2440–4.
Funding
The members of the ISG Task Force thank Emcure Pharmaceuticals for providing an unrestricted grant to conduct the face-to-face consensus meeting.
Author information
Authors and Affiliations
Contributions
AKD, SJB, UCG, VA, KD, and GVR generated the initial list of statements. AJ coordinated with the responders for the second round of voting. AKD, AJ, UCG, SK, KD, RD, and RK presented the evidence in seven parts at the final face-to-face meeting. Other members of the ISG Task Force voted in all the three rounds. All authors approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
SJB, GKM, PA, NB, AK, DNR, UCG, VA, GVR, KD, AKD, AJ, SK, RD, RK, JFA, SD, VKD, MKG, BDG, SKI, VL, MKM, PM, PM, SN, CGP, LP, AVSP, DS, JSS, RS, JV, VM, AB, UD, AKJ, RK, ASP, SPS, LS, AS, and RTW declare that they have no conflict of interest.
Ethical statement
The study was performed in a manner to conform with the Helsinki Declaration of 1975, as revised in 2000 and 2008 concerning human and animal rights, and the authors followed the policy concerning informed consent as shown on Springer.com.
Disclaimer
The authors are solely responsible for the data and the contents of the paper. In no way, the Honorary Editor-in-Chief, Editorial Board Members, or the printer/publishers are responsible for the results/findings and content of this article.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bhatia, S.J., Makharia, G.K., Abraham, P. et al. Indian consensus on gastroesophageal reflux disease in adults: A position statement of the Indian Society of Gastroenterology. Indian J Gastroenterol 38, 411–440 (2019). https://doi.org/10.1007/s12664-019-00979-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12664-019-00979-y