Abstract
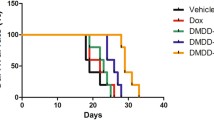
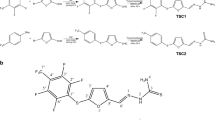
This paper describes a new method for the preparation of sodium 4-[5-(4-hydroxy-3-methoxyphenyl)-3-oxo-penta-1,4-dienyl]-2-methoxy-phenolate, DM-1, and 3-oxo-penta-1,4-dienyl-bis (2-methoxy-phenolate), DM-2. The aim of this work was to evaluate the antitumor effects of DM-1 in adjuvant chemotherapy for breast cancer treatment. Mice bearing mammary adenocarcinomas (Ehrlich ascites tumors) were treated with paclitaxel alone, DM-1 alone, and paclitaxel + DM-1. Tumor samples were used to perform cytological analysis by the Papanicolaou method and apoptosis analysis by annexin V and phosphorylated caspase 3. The paclitaxel + DM-1 group had decreased tumor areas and tumor volumes, and the frequency of metastasis was significantly reduced. This caused a decrease in cachexia, which is usually caused by the tumor. Furthermore, treatment with paclitaxel + DM-1 and DM-1 alone increased the occurrence of apoptosis up to 40% in tumor cells, which is 35% more than in the group treated with paclitaxel alone. This cell death was mainly caused through phosphorylated caspase 3 (11% increase in paclitaxel + DM-1 compared to the paclitaxel group), as confirmed by reduced malignancy criteria in the ascitic fluid. DM-1 emerges as a potential treatment for breast cancer and may act as an adjuvant in chemotherapy, enhancing antitumor drug activity with reduced side effects.








Similar content being viewed by others
References
Porter PL. Global trends in breast cancer incidence and mortality. Salud Publica Mex. 2009;51 Suppl 2:s141–6.
O'Shaughnessy J. Global trends in breast cancer incidence and mortality. Oncologist. 2005;10 Suppl 3:20–9.
Foster TS, Miller JD, Boye ME, Blieden MB, Gidwani R, Russell MW. The economic burden of metastatic breast cancer: a systematic review of literature from developed countries. Cancer Treat Rev. 2011;37:405–15.
Mareel M, Oliveira MJ, Madani I. Cancer invasion and metastasis: interacting ecosystems. Virchows Arch. 2009;454:599–622.
Micalizzi DS, Farabaugh SM, Ford HL. Epithelial-mesenchymal transition in cancer: parallels between normal development and tumor progression. J Mammary Gland Biol Neoplasia. 2010;15:117–34.
Mareel M, Leroy A. Clinical, cellular, and molecular aspects of cancer invasion. Physiol Rev. 2003;83:337–76.
Ehrlich P. Experimentelle carcinomstudien an Mäusen. Arb Inst Exp Ther. 1906;1:78–80.
von Minckwitz G. Evidence-based treatment of metastatic breast cancer—2006 recommendations by the AGO Breast Commission. Eur J Cancer. 2006;42:2897–908.
Seyhan AA, Varadarajan U, Choe S, Liu Y, McGraw J, Woods M, et al. A genome-wide RNAi screen identifies novel targets of neratinib sensitivity leading to neratinib and paclitaxel combination drug treatments. Mol Biosyst. 2011;7:1974–89.
Rivera E, Gomez H. Chemotherapy resistance in metastatic breast cancer: the evolving role of ixabepilone. Breast Cancer Res. 2010;12(2):S2.
Burstein HJ, Calrson RW, Kiel KD (2007) NCCN Clinical Practice Guidelines in Oncology. Breast Cancer. http://www.nccn.org. Accessed on 07 Oct 2011.
Cortes J, Baselga J. Targeting the microtubules in breast cancer beyond taxanes: the epothilones. Oncologist. 2007;12:271–80.
Smith I. Goals of treatment for patients with metastatic breast cancer. Semin Oncol. 2006;33:S2–5.
Discher DE, Eisenberg A. Polymer vesicles. Science. 2002;297:967–73.
Torchilin VP. PEG-based micelles as carriers of contrast agents for different imaging modalities. Adv Drug Deliv Rev. 2002;54:235–52.
Adams LS, Phung S, Yee N, Seeram NP, Li L, Chen S. Blueberry phytochemicals inhibit growth and metastatic potential of MDA-MB-231 breast cancer cells through modulation of the phosphatidylinositol 3-kinase pathway. Cancer Res. 2010;70:3594–605.
Henning SM, Seeram NP, Zhang Y, Li L, Gao K, Lee RP, et al. Strawberry consumption is associated with increased antioxidant capacity in serum. J Med Food. 2010;13:116–22.
Ray RB, Raychoudhuri A, Steele R, Nerurkar P. Bitter melon (Momordica charantia) extract inhibits breast cancer cell proliferation by modulating cell cycle regulatory genes and promotes apoptosis. Cancer Res. 2010;70:1925–31.
Aggarwal S, Ndinguri MW, Solipuram R, Wakamatsu N, Hammer RP, Ingram D, et al. [DLys(6) ]-LHRH-curcumin conjugate inhibits pancreatic cancer cell growth in vitro and in vivo. Int J Cancer. 2011;129:1611–23.
Aggarwal S, Takada Y, Singh S, Myers JN, Aggarwal BB. Inhibition of growth and survival of human head and neck squamous cell carcinoma cells by curcumin via modulation of nuclear factor kappa B signaling. Int J Cancer. 2004;111:679–92.
Huang MT, Lou YR, Xie JG, Ma W, Lu YP, Yen P, et al. Effect of dietary curcumin and dibenzoylmethane on formation of 7,12-dimethylbenz[a]anthracene-induced mammary tumors and lymphomas/leukemias in Sencar mice. Carcinogenesis. 1998;19:1697–700.
Aggarwal S, Ichikawa H, Takada Y, Sandur SK, Shishodia S, Aggarwal BB. Curcumin (diferuloylmethane) down-regulates expression of cell proliferation and antiapoptotic and metastatic gene products through suppression of IkappaBalpha kinase and Akt activation. Mol Pharmacol. 2006;69:195–206.
Carvalho FR, Vassão RC, Nicoletti MA, Maria DA. Effect of Curcuma zedoaria crude extract against tumor progression and immunomodulation. J Venom Anim Toxins Incl Trop Dis. 2010;16:324–41.
Anand P, Thomas SG, Kunnumakkara AB, Sundaram C, Harikumar KB, Sung B, et al. Biological activities of curcumin and its analogues (Congeners) made by man and Mother Nature. Biochem Pharmacol. 2008;76:1590–611.
Schaaf C, Shan B, Buchfelder M, Losa M, Kreutzer J, Rachinger W, et al. Curcumin acts as anti-tumorigenic and hormone-suppressive agent in murine and human pituitary tumour cells in vitro and in vivo. Endocr Relat Cancer. 2009;16:1339–50.
Somers-Edgar TJ, Scandlyn MJ, Stuart EC, Le Nedelec MJ, Valentine SP, Rosengren RJ. The combination of epigallocatechin gallate and curcumin suppresses ER alpha-breast cancer cell growth in vitro and in vivo. Int J Cancer. 2008;122:1966–71.
Rivera-Espinoza Y, Muriel P. Pharmacological actions of curcumin in liver diseases or damage. Liver Int. 2009;29:1457–66.
Bisht S, Maitra A. Systemic delivery of curcumin: 21st century solutions for an ancient conundrum. Curr Drug Discov Technol. 2009;6:192–9.
Shoba G, Joy D, Joseph T, Majeed M, Rajendran R, Srinivas PS. Influence of piperine on the pharmacokinetics of curcumin in animals and human volunteers. Planta Med. 1998;64:353–6.
Safavy A, Raisch KP, Mantena S, Sanford LL, Sham SW, Krishna NR, et al. Design and development of water-soluble curcumin conjugates as potential anticancer agents. J Med Chem. 2007;50:6284–8.
Cheng AL, Hsu CH, Lin JK, Hsu MM, Ho YF, Shen TS, et al. Phase I clinical trial of curcumin, a chemopreventive agent, in patients with high-risk or pre-malignant lesions. Anticancer Res. 2001;21:2895–900.
Adams BK, Ferstl EM, Davis MC, Herold M, Kurtkaya S, Camalier RF, et al. Synthesis and biological evaluation of novel curcumin analogs as anti-cancer and anti-angiogenesis agents. Bioorg Med Chem. 2004;12:3871–83.
Fuchs JR, Pandit B, Bhasin D, Etter JP, Regan N, Abdelhamid D, et al. Structure-activity relationship studies of curcumin analogues. Bioorg Med Chem Lett. 2009;19:2065–9.
Liang G, Shao L, Wang Y, Zhao C, Chu Y, Xiao J, et al. Exploration and synthesis of curcumin analogues with improved structural stability both in vitro and in vivo as cytotoxic agents. Bioorg Med Chem. 2009;17:2623–31.
Hour TC, Chen J, Huang CY, Guan JY, Lu SH, Pu YS. Curcumin enhances cytotoxicity of chemotherapeutic agents in prostate cancer cells by inducing p21(WAF1/CIP1) and C/EBPbeta expressions and suppressing NF-kappaB activation. Prostate. 2002;51:211–8.
Bava SV, Puliappadamba VT, Deepti A, Nair A, Karunagaran D, Anto RJ. Sensitization of taxol-induced apoptosis by curcumin involves down-regulation of nuclear factor-kappaB and the serine/threonine kinase Akt and is independent of tubulin polymerization. J Biol Chem. 2005;280:6301–8.
Aggarwal BB, Shishodia S, Takada Y, Banerjee S, Newman RA, Bueso-Ramos CE, et al. Curcumin suppresses the paclitaxel-induced nuclear factor-kappaB pathway in breast cancer cells and inhibits lung metastasis of human breast cancer in nude mice. Clin Cancer Res. 2005;11:7490–8.
Quincoces Suarez J, Rando DG, Santos RP, Gonçalves CP, Ferreira E, Carvalho J, et al. New antitumoral agents I: In vitro anticancer activity and in vivo acute toxicity of synthetic 1,5-bis(4-hydroxy-3-methoxyphenyl)-1,4-pentadien-3-one and derivatives. Bioorg Med Chem. 2010;18:6275–81.
Quincoces Suarez J, Rando DG, Maria DA, Pardi P, Martins C, De Souza P. Brazilian Patent PI 0602640-0 (06.07.2006); PCT/BR2007/000175 (06.07.2007); WO 2008/003155.
Ji Z. Targeting DNA damage and repair by curcumin. Breast Cancer (Auckl). 2010;4:1–3.
Li J, Wang Y, Yang C, Wang P, Oelschlager DK, Zheng Y, et al. Polyethylene glycosylated curcumin conjugate inhibits pancreatic cancer cell growth through inactivation of Jab1. Mol Pharmacol. 2009;76:81–90.
Mosmann TJ. Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods. 1983;65:55–63.
Montgomery CA. Oncological and toxicological research: alleviation and control of pain and distress in laboratory animals. Cancer Bull. 1990;42:230–7.
Prasad CP, Rath G, Mathur S, Bhatnagar D, Ralhan R. Expression analysis of maspin in invasive ductal carcinoma of breast and modulation of its expression by curcumin in breast cancer cell lines. Chem Biol Interact. 2010;183:455–61.
Chatterjee SJ, Pandey S. Chemo-resistant melanoma sensitized by tamoxifen to low dose curcumin treatment through induction of apoptosis and autophagy. Cancer Biol Ther. 2011;11:216–28.
Anand P, Sundaram C, Jhurani S, Kunnumakkara AB, Aggarwal BB. Curcumin and cancer: an “old-age” disease with an “age-old” solution. Cancer Lett. 2008;267:133–64.
Kunnumakkara AB, Anand P, Aggarwal BB. Curcumin inhibits proliferation, invasion, angiogenesis and metastasis of different cancers through interaction with multiple cell signaling proteins. Cancer Lett. 2008;269:199–225.
Gururaj AE, Belakavadi M, Venkatesh DA, Marmé D, Salimath BP. Molecular mechanisms of anti-angiogenic effect of curcumin. Biochem Biophys Res Commun. 2002;297:934–42.
Ozcan Arican G, Ozalpan A. Evaluation of the effect of paclitaxel, epirubicin and tamoxifen by cell kinetics parameters in estrogen-receptor-positive ehrlich ascites tumor (eat) cells growing in vitro. Acta Biol Hung. 2007;58:49–59.
Oliveira MJ, Van Damme J, Lauwaet T, De Corte V, De Bruyne G, Verschraegen G, et al. β-casein-derived peptides, produced by bacteria, stimulate cancer cell invasion and motility. EMBO J. 2003;22:6161–73.
Leask A, Abraham DJ. TGF-β signaling and the fibrotic response. FASEB J. 2004;18:816–27.
Togni V, Ota CC, Folador A, Junior OT, Aikawa J, Yamazaki RK, et al. Cancer cachexia and tumor growth reduction in walker 256 tumor-bearing rats supplemented with N-3 polyunsaturated fatty acids for one generation. Nutr Cancer. 2003;46:52–8.
Huang MT, Newmark HL, Frenkel KJ. Inhibitory effects of curcumin on tumorigenesis in mice. J Cell Biochem Suppl. 1997;27:26–34.
Faião-Flores F, Pardi PC, Santos RP, Rando DG, Quincoces Suarez JAP, Maria DA. Antiproliferative and antimetastatic activity of DM-1, sodium 4-[5-(4-hydroxy-3-methoxyphenyl)-3-oxo-penta-1,4-dienyl]-2-methoxy-phenolate, in B16F10 melanoma. Applied Cancer Res. 2008;28:72–9.
Fischer AH, Zhao C, Li QK, Gustafson KS, Eltoum IE, Tambouret R, et al. The cytologic criteria of malignancy. J Cell Biochem. 2010;110:795–811.
Schulte EK, Fink DK. Hematoxylin staining in quantitative DNA cytometry: an image analysis study. Anal Cell Pathol. 1995;9:257–68.
Prasad CP, Rath G, Mathur S, Bhatnagar D, Ralhan R. Potent growth suppressive activity of curcumin in human breast cancer cells: modulation of Wnt/-catenin signaling. Chem Biol Interact. 2009;181:263–71.
Fecher LA, Amaravadi RK, Schuchter LM, Flaherty KT. Drug targeting of oncogenic pathways in melanoma. Hematol Oncol Clin North Am. 2009;23:599–618.
Philchenkov AJ. Caspases: potential targets for regulating cell death. J Cell Mol Med. 2004;8:432–44.
Kunnumakkara AB, Guha S, Krishnan S, Diagaradjane P, Gelovani J, Aggarwal BB. Curcumin potentiates antitumor activity of gemcitabine in an orthotopic model of pancreatic cancer through suppression of proliferation, angiogenesis, and inhibition of nuclear factor-kappaB-regulated gene products. Cancer Res. 2007;67:3853–61.
Chauhan DP. Chemotherapeutic potential of curcumin for colorectal cancer. Curr Pharm Des. 2002;8:1695–706.
Ali S, Ahmad A, Banerjee S, Padhye S, Dominiak K, Schaffert JM, et al. Gemcitabine sensitivity can be induced in pancreatic cancer cells through modulation of miR-200 and miR-21 expression by curcumin or its analogue CDF. Cancer Res. 2010;70:3606–17.
Subramaniam D, May R, Sureban SM, Lee KB, George R, Kuppusamy P, et al. Diphenyl difluoroketone: a curcumin derivative with potent in vivo anticancer activity. Cancer Res. 2008;68:1962–9.
Yadav B, Taurin S, Rosengren RJ, Schumacher M, Diederich M, Somers-Edgar TJ, et al. Synthesis and cytotoxic potential of heterocyclic cyclohexanone analogues of curcumin. Bioorg Med Chem. 2010;18:6701–7.
Tang H, Murphy CJ, Zhang B, Shen Y, Van Kirk EA, Murdoch WJ, et al. Curcumin polymers as anticancer conjugates. Biomaterials. 2010;31:7139–49.
Friedman L, Lin L, Ball S, Bekaii-Saab T, Fuchs J, Li PK, et al. Curcumin analogues exhibit enhanced growth suppressive activity in human pancreatic cancer cells. Anticancer Drugs. 2009;20:444–9.
Acknowledgments
The authors are grateful to the São Paulo Research Foundation, FAPESP (2006/59450-1 and 2004/11351-0) for financial support.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Faião-Flores, F., Suarez, J.A.Q., Pardi, P.C. et al. DM-1, sodium 4-[5-(4-hydroxy-3-methoxyphenyl)-3-oxo-penta-1,4-dienyl]-2-methoxy-phenolate: a curcumin analog with a synergic effect in combination with paclitaxel in breast cancer treatment. Tumor Biol. 33, 775–785 (2012). https://doi.org/10.1007/s13277-011-0293-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-011-0293-z