Abstract
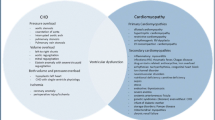
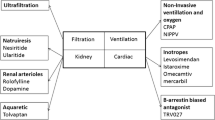
The International Society of Heart and Lung Transplantation (ISHLT) recently updated consensus pediatric heart failure guidelines from those published in 2004 with an aim to provide a practical evidence-based resource whilst recognizing the influence of adult heart failure practice. The new guidelines were formed from published evidence for heart failure management and used parallels with adult literature where pediatric evidence was lacking. This is a summary of the pharmacological therapies discussed in the new 2014 guidelines, emphasizing changes from the previous recommendations with regards to treatment of chronic heart failure with reduced ejection fraction, chronic heart failure with preserved ejection fraction, and acute decompensated heart failure. Each recommendation is classified according to strength and level of evidence. We also discuss future perspectives in the pharmacological treatment of heart failure. The 2014 ISHLT guidelines have evolved considerably from those published in 2004 with extensive information surrounding the underlying pathophysiology, investigations and recommended treatment. The new guidelines contain a modest amount of new pediatric data on pharmacological therapies and extrapolate adult data when appropriate. It is likely that most new recommendations for pediatric heart failure will continue to be based on therapies of proven benefit in adult heart failure studies.
Similar content being viewed by others
References
Kirk R, Dipchand AI, Rosenthal DN, editors. ISHLT Guidelines for the Management of Pediatric Heart Failure. Birmingham: University of Alabama at Birmingham; 2014.
Rosenthal D, Chrisant MRK, Edens E, et al. International Society for Heart and Lung Transplantation: practice guidelines for management of heart failure in children. J Heart Lung Transplant. 2004;23(12):1313–33.
Garg R, Yusuf S. Overview of randomized trials of angiotensin-converting enzyme inhibitors on mortality and morbidity in patients with heart failure. Collaborative Group on ACE Inhibitor Trials. JAMA. 1995;274(6):1450–6.
Duboc D, et al. Effect of perindopril on the onset and progression of left ventricular dysfunction in Duchenne muscular dystrophy. JACC. 2005;45(6):855–7.
Hsu DT, et al. Enalapril in infants with single ventricle: results of a multicenter randomized trial. Circulation. 2010;122(4):333–40.
Shaddy RE, et al. (For the Pediatric Carvedilol Study Group). Carvedilol for children and adolescents with heart failure. A randomized controlled trial. JAMA. 2007;298(10):1171–9.
Pitt B, et al. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study Investigators. NEJM. 1999;341(10):709–17.
Pitt B, et al. Effect of losartan compared with captopril on mortality in patients with symptomatic heart failure: randomised trial—the Losartan Heart Failure Survival Study ELITE II. Lancet. 2000;355(9215):1582–7.
Digitalis Investigation Group. The effect of digoxin on mortality and morbidity in patients with heart failure. NEJM. 1997;336(8):525–33.
Cohn J. N. Lessons from V-HeFT: questions for V-HeFT II and the future therapy of heart failure. Herz. 1991;16(Spec No 1):267–71.
Carson P, Ziesche S, Johnson G, Cohn JN. Racial differences in response to therapy for heart failure: analysis of the vasodilator-heart failure trials. Vasodilator-Heart Failure Trial Study Group. J Card Fail. 1999;5(3):178–87.
Taylor AL, et al. Combination of isosorbide dinitrate and hydralazine in blacks with heart failure. NEJM. 2004;351(20):2049–57.
Mark DB, et al. Cost-effectiveness of defibrillator therapy or amiodarone in chronic stable heart failure: results from the Sudden Cardiac Death in Heart Failure Trial (SCD-HeFT). Circulation. 2006;114(2):135–42.
Pratt CM, et al. Mortality in the Survival With ORal D-sotalol (SWORD) trial: why did patients die? Am J Cardiol. 1998;81(7):869–76.
Zhang S, et al. Efficacy of statin therapy in chronic systolic cardiac insufficiency: a meta-analysis. Eur J Intern Med. 2011;22(5):478–84.
Flynn JT. Not ready for prime time: aliskiren for treatment of hypertension or proteinuria in children. Pediatr Nephrol. 2011;26(3):491–2.
Sackner-Bernstein JD, Kowalski M, Fox M, Aaronson K. Short-term risk of death after treatment with nesiritide for decompensated heart failure: a pooled analysis of randomized controlled trials. JAMA. 2005;293(15):1900–5.
López-Candales A, et al. Symptomatic improvement in patients treated with intermittent infusion of inotropes: a double-blind placebo controlled pilot study. J Med. 2002;33(1–4):129–46.
Freimark D, Feinberg MS, Matezky S, Hochberg N, Shechter M. Impact of short-term intermittent intravenous dobutamine therapy on endothelial function in patients with severe chronic heart failure. Am Heart J. 2004;148(5):878–82.
Hatzizacharias A, et al. Intermittent milrinone effect on long-term hemodynamic profile in patients with severe congestive heart failure. Am Heart J. 1999;138(2 Pt 1):241–6.
Parle NM, Thomas MD, Dembo L, Best M, Driscoll GO. Repeated infusions of levosimendan: well tolerated and improves functional capacity in decompensated heart failure—a single-centre experience. Heart Lung Circ. 2008;17(3):206–10.
Bonios MJ, et al. Comparison of three different regimens of intermittent inotrope infusions for end stage heart failure. Int J Cardiol. 2012;159(3):225–9.
Valania G, Singh M, Slawsky MT. Targeting hyponatremia and hemodynamics in acute decompensated heart failure: is there a role for vasopressin antagonists? Curr Heart Fail Rep. 2011;8(3):198–205.
Borlaug BA, Paulus WJ. Heart failure with preserved ejection fraction: pathophysiology, diagnosis, and treatment. Eur Heart J. 2011;32(6):670–9.
Meune C, Wahbi K, Duboc D, Weber S. Meta-analysis of Renin–angiotensin–aldosterone blockade for heart failure in presence of preserved left ventricular function. J Cardiovasc Pharmacol Ther. 2011;16(3–4):368–75.
Edelmann F, et al. Effect of spironolactone on diastolic function and exercise capacity in patients with heart failure with preserved ejection fraction: the Aldo-DHF randomized controlled trial. JAMA. 2013;309(8):781–91.
Guiha NH, Cohn JN, Mikulic E, Franciosa JA, Limas CJ. Treatment of refractory heart failure with infusion of nitroprusside. NEJM. 1974;291(12):587–92.
Hoffman TM, Wernovsky G, Atz AM, et al. Efficacy and safety of milrinone in preventing low cardiac output syndrome in infants and children after corrective surgery for congenital heart disease. Circulation. 2003;107(7):996–1002.
Delaney A, Bradford C, McCaffrey J, Bagshaw SM, Lee R. Levosimendan for the treatment of acute severe heart failure: a meta-analysis of randomised controlled trials. Int J Cardiol. 2010;138(3):281–9.
Suominen PK, et al. Hemodynamic effects of rescue protocol hydrocortisone in neonates with low cardiac output syndrome after cardiac surgery. Pediatr Crit Care Med. 2005;6(6):655–9.
Dellinger RP, et al. Surviving Sepsis Campaign: international guidelines for management of sever sepsis and septic shock, 2012. Intensive Care Med. 2013;39(2):165–228.
Hamilton MA, Stevenson LW, Luu M, Walden JA. Altered thyroid hormone metabolism in advanced heart failure. JACC. 1990;16(1):91–5.
Opasich C, Pacini F, Ambrosino N, et al. Sick euthyroid syndrome in patients with moderate-to-severe chronic heart failure. Eur Heart J. 1996;17(12):1860–6.
Portman MA, et al. Triiodothyronine Supplementation in Infants and Children Undergoing Cardiopulmonary Bypass (TRICC): a multicenter placebo-controlled randomized trial: age analysis. Circulation. 2010;122:S224–33.
Liu C, Chen J, Liu K. Immunosuppressive treatment for inflammatory cardiomyopathy: meta-analysis of randomized controlled trials. Int Heart J. 2005;46(1):113–22.
Robinson J, Hartling L, Vandermeer B, Crumley E, Klassen TP. Intravenous immunoglobulin for presumed viral myocarditis in children and adults. Cochrane database Syst Rev. 2005;1:CD004370.
Drucker NA, et al. γ-Globulin treatment of acute myocarditis in the pediatric population. Circulation. 1994;89(1):252–7.
Raynolds MV, et al. Angiotensin-converting enzyme DD genotype in patients with ischaemic or idiopathic dilated cardiomyopathy. Lancet. 1993;342(8879):1073–5.
Andersson B, Sylvén C. The DD genotype of the angiotensin-converting enzyme gene is associated with increased mortality in idiopathic heart failure. JACC. 1996;28(1):162–7.
Candy GP, et al. Association of left ventricular systolic performance and cavity size with angiotensin-converting enzyme genotype in idiopathic dilated cardiomyopathy. Am J Cardiol. 1999;83(5):740–4.
Mestroni L, Begay R, Graw SL, Taylor MRG. Pharmacogenetics of Heart Failure. Curr Opin Cardiol. 2014;29(3):227–34.
Clifford DM et al. Stem cell treatment for acute myocardial infarction. Cochrane database Syst Rev. 2012;2:CD006536.
Strauer B-E, Yousef M, Schannwell CM. The acute and long-term effects of intracoronary Stem cell Transplantation in 191 patients with chronic heARt failure: the STAR-heart study. Eur J Heart Fail. 2010;12(7):721–9.
Seth S, et al. The ABCD (Autologous Bone Marrow Cells in Dilated Cardiomyopathy) trial a long-term follow-up study. JACC. 2010;55(15):1643–4.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No external funding was used in the preparation of this manuscript.
Conflict of interest
Dr Weintraub serves on an advisory board for Actelion Pharmaceuticals. Dr Hussey has no conflicts of interest to declare.
Rights and permissions
About this article
Cite this article
Hussey, A.D., Weintraub, R.G. Drug Treatment of Heart Failure in Children: Focus on Recent Recommendations from the ISHLT Guidelines for the Management of Pediatric Heart Failure. Pediatr Drugs 18, 89–99 (2016). https://doi.org/10.1007/s40272-016-0166-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40272-016-0166-4