Abstract
Background
Polypharmacy and fall-risk increasing drugs (FRIDS) have been associated with injurious falls. We aimed to estimate the prevalence of polypharmacy and FRIDS in older patients discharged from an Orthogeriatric Unit after a hip fracture surgery.
Methods
This study describes the baseline findings of a 2-year retrospective cohort study. We included patients older than 80 years discharged from an Orthogeriatric Unit who were able to walk before surgery. Patient’s baseline variables, total number of drugs, and FRIDS at hospital discharge were collected.
Results
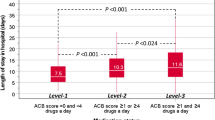
We included 228 patients. The mean number of drugs and FRIDS prescribed at discharge was 11.6 ± 3.0 and 2.9 ± 1.6, respectively. Polypharmacy was prevalent in all patients except in three: 23.3% (5–9 drugs) and 75.9% (≥ 10 drugs). Only 11 patients had no FRIDS and 35.5% were on > 3 FRIDS. The most prevalent FRIDS were: agents acting on the renin-angiotensin system (43.9%) and anxiolytics (39.9%). The number of FRIDS was higher in patients with extreme polypharmacy (3.4 ± 1.5) than in those on 5–9 drugs (1.5 ± 1.0, p < 0.05). Independent people in performing instrumental activities had lower risk of extreme polypharmacy (≥ 10 drugs) or > 3 FRIDS: OR 0.39 (95% CI 0.18–0.83) and OR 0.41 (95% CI 0.20–0.84), respectively. People living in a nursing home had higher risk of > 3 FRIDS: OR 4.03 (95% CI 1.12–14.53).
Conclusions
Polypharmacy and fall-risk increasing drugs are prevalent in patients discharged from orthogeriatric care after surgery for a hip fracture. Interventions on drug use at hospital discharge could have a potential impact on falls in this high-risk population.
Similar content being viewed by others
References
Tinetti ME, Doucette J, Claus E et al (1995) Risk factors for serious injury during falls by older persons in the community. J Am Geriatr Soc 43:1214–1221
Peel NM (2011) Epidemiology of falls in older age. Can J Aging 30:7–19. https://doi.org/10.1017/S071498081000070X
Shumway-Cook A, Ciol MA, Gruber W et al (2005) Incidence of and risk factors for falls following hip fracture in community-dwelling older adults. Phys Ther 85:648–655
Sjöberg C, Wallerstedt SM (2013) Effects of medication reviews performed by a physician on treatment with fracture-preventing and fall-risk-increasing drugs in older adults with hip fracture-a randomized controlled study. J Am Geriatr Soc 61:1464–1472. https://doi.org/10.1111/jgs.12412
Ikutomo H, Nagai K, Nakagawa N et al (2015) Falls in patients after total hip arthroplasty in Japan. J Orthop Sci 20:663–668. https://doi.org/10.1007/s00776-015-0715-7
Lloyd BD, Williamson DA, Singh NA et al (2009) Recurrent and Injurious Falls in the Year Following Hip Fracture: A Prospective Study of Incidence and Risk Factors From the Sarcopenia and Hip Fracture Study. J Gerontol Ser A Biol Sci Med Sci 64A:599–609. https://doi.org/10.1093/gerona/glp003
Sjöberg C, Bladh L, Klintberg L et al (2010) Treatment with fall-risk-increasing and fracture-preventing drugs before and after a hip fracture: an observational study. Drugs Aging 27:653–661. https://doi.org/10.2165/11538200-000000000-00000
Chen Y, Zhu LL, Zhou Q (2014) Effects of drug pharmacokinetic/pharmacodynamic properties, characteristics of medication use, and relevant pharmacological interventions on fall risk in elderly patients. Ther Clin Risk Manag 10:437–448. https://doi.org/10.2147/TCRM.S63756
Leipzig RM, Cumming RG, Tinetti ME (1999) Drugs and falls in older people: a systematic review and meta-analysis: I. Psychotropic drugs. J Am Geriatr Soc 47:30–39. https://doi.org/10.1111/j.1532-5415.1999.tb01898.x
Woolcott JC, Richardson KJ, Wiens MO et al (2009) Meta-analysis of the impact of 9 medication classes on falls in elderly persons. Arch Intern Med 169:1952–1960. https://doi.org/10.1001/archinternmed.2009.357
Ziere G, Dieleman JP, Hofman A et al (2006) Polypharmacy and falls in the middle age and elderly population. Br J Clin Pharmacol 61:218–223. https://doi.org/10.1111/j.1365-2125.2005.02543.x
Helgadóttir B, Laflamme L, Monárrez-Espino J et al (2014) Medication and fall injury in the elderly population; do individual demographics, health status and lifestyle matter? BMC Geriatr 14:92. https://doi.org/10.1186/1471-2318-14-92
van der Velde N, Stricker BHC, Pols HAP et al (2007) Risk of falls after withdrawal of fall-risk-increasing drugs: a prospective cohort study. Br J Clin Pharmacol 63:232–237. https://doi.org/10.1111/j.1365-2125.2006.02736.x
Leipzig RM, Cumming RG, Tinetti ME (1999) Drugs and falls in older people: a systematic review and meta-analysis: II. Cardiac and analgesic drugs. J Am Geriatr Soc 47:40–50
The Swedish National Board of Health and Welfare (2010) Indikatorer för god läkemedelsterapi hos äldre. [Indicators for appropriate drug therapy in the elderly]. https://www.socialstyrelsen.se/publikationer2010/2010-6-29. https://www.socialstyrelsen.se/Lists/Artikelkatalog/Attachments/18085/2010-6-29.pdf
Milos V, Bondesson Å, Magnusson M et al (2014) Fall risk-increasing drugs and falls: a cross-sectional study among elderly patients in primary care. BMC Geriatr 14:40. https://doi.org/10.1186/1471-2318-14-40
Saltvedt I, Prestmo A, Einarsen E et al (2012) Development and delivery of patient treatment in the trondheim hip fracture trial. A new geriatric in-hospital pathway for elderly patients with hip fracture. BMC Res Notes 5:355. https://doi.org/10.1186/1756-0500-5-355
Grigoryan KV, Javedan H, Rudolph JL (2014) Orthogeriatric care models and outcomes in hip fracture patients: a systematic review and meta-analysis. J Orthop Trauma 28:e49–e55. https://doi.org/10.1097/BOT.0b013e3182a5a045
Sanford AM, Morley JE, McKee A (2018) Editorial: orthogeriatrics and hip fractures. J Nutr Health Aging 22:457–462. https://doi.org/10.1007/s12603-018-1007-7
Holden MK, Gill KM, Magliozzi MR et al (1984) Clinical gait assessment in the neurologically impaired reliability and meaningfulness. Phys Ther 64:35–40. https://doi.org/10.1093/ptj/64.1.35
Scotland N (2015) Polypharmacy Guidance for the safe and effective use of multiple medicines to manage long term conditions. http://www.jitscotland.org.uk/resource/polypharmacy-guidance-march-2015/. Accessed 1 May 2016
Heckenbach K, Ostermann T, Schad F et al (2014) Medication and falls in elderly outpatients: an epidemiological study from a german pharmacovigilance network. Springerplus 3:483. https://doi.org/10.1186/2193-1801-3-483
O’mahony D, O’sullivan D, Byrne S et al (2015) STOPP/START criteria for potentially inappropriate prescribing in older people: version 2. Age Ageing 44:213–218. https://doi.org/10.1093/ageing/afu145
Boyé NDA, van der Velde N, de Vries OJ et al (2017) Effectiveness of medication withdrawal in older fallers: Results from the improving medication prescribing to reduce risk of falls (IMPROveFALL) trial. Age Ageing 46:142–146. https://doi.org/10.1093/ageing/afw161
Bennett A, Gnjidic D, Gillett M et al (2014) Prevalence and impact of fall-risk-increasing drugs, polypharmacy, and drug–drug interactions in robust versus frail hospitalised falls patients: a prospective cohort study. Drugs Aging 31:225–232. https://doi.org/10.1007/s40266-013-0151-3
Kragh A, Elmståhl S, Atroshi I (2011) Older adults’ medication use 6 months before and after hip fracture: a population-based cohort study. J Am Geriatr Soc 59:863–868. https://doi.org/10.1111/j.1532-5415.2011.03372.x
Munson JC, Bynum JPW, Bell J et al (2016) Patterns of prescription drug use before and after fragility fracture. JAMA Intern Med 176:1531–1538. https://doi.org/10.1001/jamainternmed.2016.4814
Rossini M, Viapiana O, Adami S et al (2014) Medication use before and after hip fracture: a population-based cohort and case-control study. Drugs Aging 31:547–553. https://doi.org/10.1007/s40266-014-0184-2
Beunza-Sola M, Hidalgo-Ovejero ÁM, Martí-Ayerdi J et al (2018) Study of fall risk-increasing drugs in elderly patients before and after a bone fracture. Postgrad Med J 94:76–80. https://doi.org/10.1136/postgradmedj-2017-135129
Turner JP, Tervonen HE, Shakib S et al (2017) Factors associated with use of falls risk-increasing drugs among patients of a geriatric oncology outpatient clinic in Australia: a cross-sectional study. J Eval Clin Pract 23:361–368. https://doi.org/10.1111/jep.12624
Rieckert A, Trampisch US, Klaaßen-Mielke R et al (2018) Polypharmacy in older patients with chronic diseases: a cross-sectional analysis of factors associated with excessive polypharmacy. BMC Fam Pract 19:113. https://doi.org/10.1186/s12875-018-0795-5
Belfrage B, Koldestam A, Sjöberg C et al (2015) Number of drugs in the medication list as an indicator of prescribing quality: a validation study of polypharmacy indicators in older hip fracture patients. Eur J Clin Pharmacol 71:363–368. https://doi.org/10.1007/s00228-014-1792-9
American Geriatrics Society, British Geriatrics Society and AA of OSP on FP (2001) Guideline for the Prevention of Falls in Older Persons. J Am Geriatr Soc 49:664–672. https://doi.org/10.1046/j.1532-5415.2001.49115.x
Funding
Authors did not receive any governmental or private grants.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare no competing interests. All authors have completed the Conflict of Interest Disclosure form and declare: no support from any organisation for the submitted work; no financial relationships with any organisations that might have an interest in the submitted work in the previous 3 years; no other relationships or activities that could appear to have influenced the submitted work.
Statement of human and animal rights
The study was approved by the Ethics Committee on Clinical Research of the Hospital Universitario Ramón y Cajal (Madrid) on May 2016.
Informed consent
No consent forms from patients were requested, as this is a retrospective study and hospital-collected data were analysed. Patients accept such kind of use of data when they are admitted to the hospital.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Correa-Pérez, A., Delgado-Silveira, E., Martín-Aragón, S. et al. Fall-risk increasing drugs and prevalence of polypharmacy in older patients discharged from an Orthogeriatric Unit after a hip fracture. Aging Clin Exp Res 31, 969–975 (2019). https://doi.org/10.1007/s40520-018-1046-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-018-1046-2