Abstract
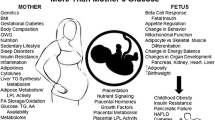
The intrauterine environment can have a significant impact on fetal and maternal well-being, both during pregnancy and in later life. We aimed to identify how fetal sex and maternal body mass index (BMI) influence insulin resistance and metabolic function during pregnancy with maternal BMI > 25 kg/m2. This secondary analysis assessed data from the PEARS–randomized controlled trial that recruited pregnant women with body mass indexes 25–39.9 kg/m2. Longitudinal measurements of maternal and fetal insulin resistance and metabolic function were recorded throughout pregnancy. Regression models tested the effects of fetal sex and maternal BMI on markers of metabolic function and insulin regulation. A total of 484 women and their newborns (252 (52%) males vs. 232 (48%) females) were included in the analysis. A total of 333 (69%) women were overweight and 151 (31%) were obese. Male newborns were heavier and larger than females, and had a higher rate of instrumental delivery. Males had a lower LDL, but no other markers of insulin resistance or metabolic function were affected by fetal sex. Women with obesity had elevated markers of insulin resistance and metabolic dysfunction compared with women that were overweight, but maternal BMI did not impact these variables in the fetus. Fetal sex did not impact maternal and fetal metabolic parameters in women with BMI > 25 kg/m2. However, a higher BMI caused increasingly deranged maternal blood lipid concentrations and markers of insulin resistance as pregnancy progressed. Lipid monitoring and interventions to reduce lipids during pregnancy therefore require further evaluation.
Similar content being viewed by others
References
Heindel J, Vandenberg L. Developmental origins of health and disease: a paradigm for understanding disease etiology and prevention. Current Opinions in Pediatrics. 2015;27(2):248–53.
Barker D. Fetal origins of coronary heart disease. BMJ. 1995;311:171–4.
Eriksson J, Forsen T, Tuomilehto J, Jaddoe V, Osmond C, Barker D. Effect of size at birth and childhood growth on the insulin resistance syndrome in elderly individuals. Diabetologia. 2002;45:342–8.
Harder T, Rodekamp E, Schellong K, Dudenhausen JW, Plagemann A. Birth weight and subsequent risk of type 2 diabetes: a meta-analysis. Am J Epidemiol. 2007;165(8):849–57.
Schaefer-Graf UM, Pawliczak J, Passow D, Hartmann R, Rossi R, Buhrer C, et al. Birth weight and parental BMI predict overweight in children from mothers with gestational diabetes. Diabetes Care. 2005;28(7):1745–50.
Sonagra AD, Biradar SM, Dattatreya K, Jayaprakash Murtha DS. Normal pregnancy - a state of insulin resistance. Journal of Clinical & Diagnostic Research. 2014;8(11):CC01–C3.
Reis FM, Florio P, Cobellis L, Luisi S, Severi FM, Bocchi C, et al. Human placenta as a source of neuroendocrine factors. Biol Neonate. 2001;79(3–4):150–60.
Shields BM, Knight B, Hopper H, Hill A, Powell RJ, Hattersley AT, et al. Measurement of cord insulin and insulin-related peptides suggests that girls are more insulin resistant than boys at birth. Diabetes Care. 2007;30(10):2661–6.
Ibanez L, Sebastiani G, Lopez-Bermejo A, Diaz M, Gomez-Roig MD, de Zegher F. Gender specificity of body adiposity and circulating adiponectin, visfatin, insulin, and insulin growth factor-I at term birth: relation to prenatal growth. J Clin Endocrinol Metab. 2008;93(7):2774–8.
Walsh JM, Segurado R, Mahony RM, Foley ME, McAuliffe FM. The effects of fetal gender on maternal and fetal insulin resistance. PLoS One. 2015;10(9):e0137215.
Xiao L, Zhao JP, Nuyt AM, Fraser WD, Luo ZC. Female fetus is associated with greater maternal insulin resistance in pregnancy Diabetic Medicine. 2014;31(12):1696–1701.
Retnakaran R, Kramer CK, Ye C, Kew S, Hanley AJ, Connelly PW, et al. Fetal sex and maternal risk of gestational diabetes mellitus: the impact of having a boy. Diabetes Care. 2015;38(5):844–51.
Montelongo A, Lasuncion MA, Pallardo LF, Herrera E. Longitudinal study of plasma lipoproteins and hormones during pregnancy in normal and diabetic women. Diabetes. 1992;41(12):1651–9.
Vrijkotte TG, Krukziener N, Hutten BA, Vollebregt KC, van Eijsden M, Twickler MB. Maternal lipid profile during early pregnancy and pregnancy complications and outcomes: the ABCD study. J Clin Endocrinol Metab. 2012;97(11):3917–25.
Wang C, Zhu W, Wei Y, Su R, Feng H, Lin L, et al. The predictive effects of early pregnancy lipid profiles and fasting glucose on the risk of gestational diabetes mellitus stratified by body mass index. J Diabetes Res. 2016;2016:3013567.
Geraghty AA, Alberdi G, O'Sullivan EJ, O'Brien EC, Crosbie B, Twomey PJ, et al. Maternal and fetal blood lipid concentrations during pregnancy differ by maternal body mass index: findings from the ROLO study. BMC Pregnancy Childbirth. 2017;17(1):360.
Scifres CM, Catov JM, Simhan HN. The impact of maternal obesity and gestational weight gain on early and mid-pregnancy lipid profiles. Obesity (Silver Spring). 2014;22(3):932–8.
Kennelly MA, Ainscough K, Lindsay KL, O'Sullivan E, Gibney ER, McCarthy M, et al. Pregnancy exercise and nutrition with smartphone application support: a randomized controlled trial. Obstet Gynecol. 2018;131(5):818–26.
Institute of Medicine and National Research Council Committee to Reexamine IOMPWG. The National Academies Collection: Reports funded by National Institutes of Health. In: Rasmussen KM, Yaktine AL, editors. Weight gain during pregnancy: reexamining the guidelines. Washington (DC): National Academies Press (US) National Academy of Sciences; 2009.
International Association of Diabetes Pregnancy Study Groups Consensus Panel, Metzger BE, Gabbe SG, Persson B, Buchanan TA, Catalano PA, et al. International association of diabetes and pregnancy study groups recommendations on the diagnosis and classification of hyperglycemia in pregnancy. Diabetes Care. 2010;33(3):676–82.
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28(7):412–9.
Friedewald WT, Levy RI, Fredrickson DS. Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem. 1972;18(6):499–502.
Leys C, Ley C, Klein O, Bernard P, Licata L. Detecting outliers: do not use standard deviation around the mean, use absolute deviation around the median. J Exp Soc Psychol. 2013;49(4):764–6.
Ye K, Li L, Zhang D, Li Y, Wang HQ, Lai HL, et al. Effect of maternal obesity on fetal growth and expression of placental fatty acid transporters. J Clin Res Pediatr Endocrinol. 2017;9(4):300–7.
Schaffer-Graf UM, Graf K, Kulbacka I, Kjos SL, Dudenhausen JW, Vetter K, et al. Maternal lipids as strong determinants of fetal environment and growth in pregnancies with gestational diabetes mellitus. Diabetes Care. 2008;31(9):1858–63.
Horan MK, Donnelly JM, McGowan CA, Gibney ER, McAuliffe FM. The association between maternal nutrition and lifestyle during pregnancy and 2-year-old offspring adiposity: analysis from the ROLO study. J Public Health. 2016;24(5):427–36.
Eogan MA, Geary MP, O'Connell MP, Keane DP. Effect of fetal sex on labour and delivery: retrospective review. BMJ. 2003;326(7381):137.
Hindmarsh PC, Geary MP, Rodeck CH, Kingdom JC, Cole TJ. Intrauterine growth and its relationship to size and shape at birth. Pediatr Res. 2002;52(2):263–8.
Lipschuetz M, Cohen SM, Ein-Mor E, Sapir H, Hochner-Celnikier D, Porat S, et al. A large head circumference is more strongly associated with unplanned cesarean or instrumental delivery and neonatal complications than high birthweight. Am J Obstet Gynecol. 2015;213(6):833 e1- e12.
Enquobahrie DA, Williams MA, Qiu C, Luthy DA. Early pregnancy lipid concentrations and the risk of gestational diabetes mellitus. Diabetes Res Clin Pract. 2005;70(2):134–42.
Chiang AN, Yang ML, Hung JH, Chou P, Shyn SK, Ng HT. Alterations of serum lipid levels and their biological relevances during and after pregnancy. Life Sci. 1995;56(26):2367–75.
Ziaei S, Bonab KM, Kazemnejad A. Serum lipid levels at 28-32 weeks gestation and hypertensive disorders. Hypertens Pregnancy. 2006;25(1):3–10.
Kitajima M, Oka S, Yasuhi I, Fukuda M, Rii Y, Ishimaru T. Maternal serum triglyceride at 24--32 weeks’ gestation and newborn weight in nondiabetic women with positive diabetic screens. Obstet Gynecol. 2001;97(5 Pt 1):776–80.
Vahratian A, Misra VK, Trudeau S, Misra DP. Prepregnancy body mass index and gestational age-dependent changes in lipid levels during pregnancy. Obstet Gynecol. 2010;116(1):107–13.
Sulaiman WN, Caslake MJ, Delles C, Karlsson H, Mulder MT, Graham D, et al. Does high-density lipoprotein protect vascular function in healthy pregnancy? Clin Sci (Lond). 2016;130(7):491–7.
Barrett HL, Dekker Nitert M, McIntyre HD, Callaway LK. Maternal lipids in pre-eclampsia: innocent bystander or culprit? Hypertens Pregnancy. 2014;33(4):508–23.
Catalano PM. Obesity, insulin resistance, and pregnancy outcome. Reproduction. 2010;140(3):365–71.
Herrera E, Ortega-Senovilla H. Lipid metabolism during pregnancy and its implications for fetal growth. Curr Pharm Biotechnol. 2014;15(1):24–31.
Appold K. Determining laboratory reference intervals: CLSI guideline makes the task manageable. Lab Med. 2009;40(2):75–6.
Acknowledgements
The authors wish to acknowledge and thank the mothers who participated in the PEARS study in the National Maternity Hospital.
Funding
This research was supported by the National Maternity Hospital medical fund.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
This study presents a secondary analysis of the PEARS database, which was a single-centred–randomised controlled trial conducted at the National Maternity Hospital, Dublin, with institutional ethical approval. The trial was registered as ISRCTN29316280.
Statement of Informed Consent
Full written, informed consent was obtained from all participants.
Rights and permissions
About this article
Cite this article
Rafferty, A.R., Geraghty, A.A., Kennelly, M.A. et al. Limited Impact of Fetal Sex and Maternal Body Mass Index on Fetal and Maternal Insulin Resistance and Lipid Metabolism: Findings from the PEARs Study. Reprod. Sci. 27, 513–522 (2020). https://doi.org/10.1007/s43032-019-00045-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43032-019-00045-0